Abstract
Purpose
To investigate whether the presence of micropapillary and solid patterns are associated with nodal upstaging and survival patterns in patients with cT1N0M0 lung adenocarcinoma.
Method
We retrospectively analyzed the clinicopathologic data of 2571 patients undergoing lobectomy and lymph node dissection or sampling. Logistic and Cox regression analysis were applied to determine the association between histological patterns and nodal upstaging and survival.
Results
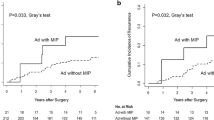
Nodal upstaging was detected in 115 patients (4.5%) through postoperative pathologic examination. Tumors absent of lepidic pattern, and present with acinar, micropapillary and solid patterns had significantly higher nodal upstaging rate (all P < 0.001). Presence of micropapillary [odds ratios (ORs) = 3.51; 95% confidence intervals (CI) = 2.09–5.89; P < 0.001] and solid (OR 2.28; 95% CI 1.42–3.64; P = 0.001) patterns were independent predictors for nodal upstaging. Presence of micropapillary and solid patterns also significantly deteriorated the recurrence-free survival (RFS) (both log-rank P < 0.001), and were independently associated with unfavorable RFS in multivariable Cox analysis RFS [micropapillary: hazard ratios (HR) = 1.41; 95% CI 1.04–1.99; P = 0.041; solid: HR 2.05; 95% CI 1.56–2.70; P < 0.001].
Conclusion
The analysis of a large-scale cohort demonstrated that the presence of micropapillary and solid patterns significantly increase the risk of nodal upstaging and are independently associated with unfavorable prognosis.

Similar content being viewed by others
References
Aberle DR et al (2011) Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med 365:395–409. https://doi.org/10.1056/NEJMoa1102873
Altorki NK et al (2014) Sublobar resection is equivalent to lobectomy for clinical stage 1A lung cancer in solid nodules. J Thorac Cardiovasc Surg 147:754–762. https://doi.org/10.1016/j.jtcvs.2013.09.065 (Discussion 762–754)
Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT (2017) The eighth edition lung cancer. Stage Classif Chest 151:193–203. https://doi.org/10.1016/j.chest.2016.10.010
Ferlay J et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136:E359–E386. https://doi.org/10.1002/ijc.29210
Goldstraw P et al (2016) The IASLC lung cancer staging project: proposals for revision of the TNM stage groupings in the forthcoming (Eighth) edition of the TNM classification for lung cancer. J Thorac Oncol 11:39–51. https://doi.org/10.1016/j.jtho.2015.09.009
Huang KY, Ko PZ, Yao CW, Hsu CN, Fang HY, Tu CY, Chen HJ (2017) Inaccuracy of lung adenocarcinoma subtyping using preoperative biopsy specimens. J Thorac Cardiovasc Surg 154:332–339 e331. https://doi.org/10.1016/j.jtcvs.2017.02.059
Hung JJ, Jeng WJ, Chou TY, Hsu WH, Wu KJ, Huang BS, Wu YC (2013) Prognostic value of the new International Association for the Study of Lung Cancer/American Thoracic Society/European Respiratory Society lung adenocarcinoma classification on death and recurrence in completely resected stage I lung adenocarcinoma. Ann Surg 258:1079–1086. https://doi.org/10.1097/SLA.0b013e31828920c0
Landreneau RJ et al (2014) Recurrence and survival outcomes after anatomic segmentectomy versus lobectomy for clinical stage I non-small-cell lung cancer: a propensity-matched analysis. J Clin Oncol: Off J Am Soc Clin Oncol 32:2449–2455. https://doi.org/10.1200/JCO.2013.50.8762
Luo J et al (2016) Prognostic and predictive value of the novel classification of lung adenocarcinoma in patients with stage. IB J Cancer Res Clin Oncol 142:2031–2040. https://doi.org/10.1007/s00432-016-2192-6
Lv YL et al (2011) Diagnostic performance of integrated positron emission tomography/computed tomography for mediastinal lymph node staging in non-small cell lung cancer: a bivariate systematic review and meta-analysis. J Thorac Oncol: Off Publ Int Assoc Study Lung Cancer 6:1350–1358. https://doi.org/10.1097/JTO.0b013e31821d4384
Nitadori J et al (2013) Impact of micropapillary histologic subtype in selecting limited resection vs lobectomy for lung adenocarcinoma of 2 cm or smaller. J Natl Cancer Inst 105:1212–1220. https://doi.org/10.1093/jnci/djt166
Rice D et al (2016) The IASLC mesothelioma staging project: proposals for revisions of the N descriptors in the forthcoming eighth edition of the TNM classification for pleural mesothelioma J Thorac Oncol: Off Publ Int Assoc Study Lung Cancer 11:2100–2111. https://doi.org/10.1016/j.jtho.2016.09.121
Travis WD et al (2011) International association for the study of lung cancer/american thoracic society/european respiratory society international multidisciplinary classification of lung adenocarcinoma J Thorac Oncol: Off Publ Int Assoc Study Lung Cancer 6:244–285. https://doi.org/10.1097/JTO.0b013e318206a221
Travis WD, Brambilla E, Riely GJ (2013) New pathologic classification of lung cancer: relevance for clinical practice and clinical trials. J Clin Oncol: Off J Am Soc Clin Oncol 31:992–1001. https://doi.org/10.1200/jco.2012.46.9270
Travis WD et al (2015) The 2015 world health organization classification of lung tumors: impact of genetic, clinical and radiologic advances since the 2004 Classif J Thorac Oncol: Off Publ Int Assoc Study Lung Cancer 10:1243–1260. https://doi.org/10.1097/JTO.0000000000000630
Trejo Bittar HE, Incharoen P, Althouse AD, Dacic S (2015) Accuracy of the IASLC/ATS/ERS histological subtyping of stage I lung adenocarcinoma on intraoperative frozen sections Mod Pathol 28:1058–1063. https://doi.org/10.1038/modpathol.2015.71
Tsao MS et al (2015) Subtype classification of lung adenocarcinoma predicts benefit from adjuvant chemotherapy in patients undergoing complete resection. J Clin Oncol 33:3439–3446. https://doi.org/10.1200/JCO.2014.58.8335
Tsuta K et al (2013) The utility of the proposed IASLC/ATS/ERS lung adenocarcinoma subtypes for disease prognosis and correlation of driver gene alterations. Lung Cancer 81:371–376. https://doi.org/10.1016/j.lungcan.2013.06.012
Tsutani Y, Miyata Y, Nakayama H, Okumura S, Adachi S, Yoshimura M, Okada M (2014) Sublobar resection for lung adenocarcinoma meeting node-negative criteria on preoperative imaging Ann Thorac Surg 97:1701–1707. https://doi.org/10.1016/j.athoracsur.2014.02.024
Ujiie H et al (2015) Solid predominant histologic subtype in resected stage I lung adenocarcinoma is an independent predictor of early, extrathoracic, multisite recurrence and of poor. Postrecurrence Surviv J Clin oncol 33:2877–2884. https://doi.org/10.1200/JCO.2015.60.9818
Yoshizawa A et al (2011) Impact of proposed IASLC/ATS/ERS classification of lung adenocarcinoma: prognostic subgroups and implications for further revision of staging based on analysis of 514 stage I cases Mod Pathol 24:653–664. https://doi.org/10.1038/modpathol.2010.232
Yoshizawa A et al (2013) Validation of the IASLC/ATS/ERS lung adenocarcinoma classification for prognosis and association with EGFR and KRAS gene mutations: analysis of 440 Japanese patients J Thorac Oncol 8:52–61. https://doi.org/10.1097/JTO.0b013e3182769aa8
Zhao Z-R, To KF, Mok TSK, Ng CSH (2017) Is there significance in identification of non-predominant micropapillary or solid components in early-stage lung adenocarcinoma? Interact CardioVasc Thorac Surg 24:121–125. https://doi.org/10.1093/icvts/ivw283
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Yuan, Y., Ma, G., Zhang, Y. et al. Presence of micropapillary and solid patterns are associated with nodal upstaging and unfavorable prognosis among patient with cT1N0M0 lung adenocarcinoma: a large-scale analysis. J Cancer Res Clin Oncol 144, 743–749 (2018). https://doi.org/10.1007/s00432-017-2571-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-017-2571-7