Abstract
Purpose
To evaluate and compare the efficacy of prostate volume (PV), transitional zone volume (TZV), and prostate volume index (PVI, the ratio of TZV to peripheral zone volume) in the identification of men at risk of prostate cancer (PCa) and high-progression PCa (HPPCa) at the initial biopsy (IBX) in a real-world population.
Methods
From Jul 2014 to Aug 2016, data on 1144 patients who had undergone the initial prostate biopsies were prospectively collected and analyzed. Univariate and multivariate logistic regression analyses were performed to identify the independent predictors for PCa and HPPCa. Based on independent predictors, nomogram models were developed and internally validated to assess a man’s risk of harboring PCa and HPPCa.
Results
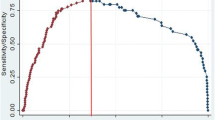
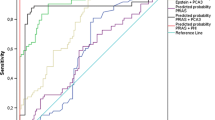
The detection rates of PCa and HPPCa were 43.09% (493/1144) and 39.16% (448/1144), respectively. In the multivariate analyses, age, PSA, TZV, DRE, and TRUS instead of PV or PVI were independent predictors for PCa and HPPCa, percent free PSA was independent predictor for PCa not for HPPCa. Such independent predictors were finally included in the nomogram models. The AUCs of TZV-based nomogram models were 87.0% for PCa and 87.7% for HPPCa, which were higher than that of PSA alone or other predictive models.
Conclusions
TZV is a better predictive biomarker than PV or PVI for PCa and HPPCa, we recommend adding TZV but not PV or PVI to the nomogram models to improve the predictive accuracy of PCa and HPPCa at IBX.




Similar content being viewed by others
References
Ahn JH, Lee JZ, Chung MK, Ha HK (2014) Nomogram for prediction of prostate cancer with serum prostate specific antigen less than 10 ng/mL. J Korean Med Sci 29: 338–342
Boorjian SA, Karnes RJ, Rangel LJ et al (2008) Mayo Clinic validation of the D’amico risk group classification for predicting survival following radical prostatectomy. J Urol 179:1354–1360
Chen W, Zheng R, Baade PD et al (2016) Cancer statistics in China, 2015. CA Cancer J Clin 66:115–132
Djavan B, Zlotta AR, Byttebier G et al (1998) Prostate specific antigen density of the transition zone for early detection of prostate cancer. J Urol 160:411–418
Elshafei A, Chevli KK, Moussa AS et al (2015) PCA3-based nomogram for predicting prostate cancer and high grade cancer on initial transrectal guided biopsy. Prostate 75:1951–1957
Hansen J, Auprich M, Ahyai SA et al (2013) Initial prostate biopsy: development and internal validation of a biopsy-specific nomogram based on the prostate cancer antigen 3 assay. Eur Urol 63:201–209
Hayes JH, Barry MJ (2014) Screening for prostate cancer with the prostate-specific antigen test: a review of current evidence. JAMA 311:1143–1149
Heijnsdijk EA, Wever EM, Auvinen A et al (2012) Quality-of-life effects of prostate-specific antigen screening. N Engl J Med 367:595–605
Heijnsdijk EA, de Carvalho TM, Auvinen A et al (2014) Cost-effectiveness of prostate cancer screening: a simulation study based on ERSPC data. J Natl Cancer Inst 107:366
Ilic D, Neuberger MM, Djulbegovic M, Dahm P (2013) Screening for prostate cancer. Cochrane Database Syst Rev 1:CD004720
Kang SH, Bae JH, Park HS et al (2006) Prostate-specific antigen adjusted for the transition zone volume as a second screening test: a prospective study of 248 cases. Int J Urol 13:910–914
Kawamura K, Suzuki H, Kamiya N et al (2008) Development of a new nomogram for predicting the probability of a positive initial prostate biopsy in Japanese patients with serum PSA levels less than 10 ng/mL. Int J Urol 15:598–603
Kuo SC, Hung SH, Wang HY et al (2013) Chinese nomogram to predict probability of positive initial prostate biopsy: a study in Taiwan region. Asian J Androl 15:780–784
Lazzeri M, Haese A, de la Taille A et al (2013) Serum isoform [-2]proPSA derivatives significantly improve prediction of prostate cancer at initial biopsy in a total PSA range of 2–10 ng/ml: a multicentric European study. Eur Urol 63:986–994
Lin YR, Wei XH, Uhlman M et al (2015) PSA density improves the rate of prostate cancer detection in Chinese men with a PSA between 2.5–10.0 ng ml (−1) and 10.1–20.0 ng ml (−1): a multicenter study. Asian J Androl 17:503–507
Nam RK, Toi A, Klotz LH et al (2007) Assessing individual risk for prostate cancer. J Clin Oncol 25:3582–3588
Porcaro AB, Novella G, Molinari A et al (2015) Prostate volume index and chronic inflammation of the prostate type IV with respect to the risk of prostate cancer. Urol Int 94:270–285
Porcaro AB, Novella G, Cacciamani G et al (2017) Prostate volume index associates with a decreased risk of prostate cancer: results of a large cohort of patients elected to a first biopsy set. Urol Int 98:22–27
Shariat SF, Karakiewicz PI, Suardi N, Kattan MW (2008) Comparison of nomograms with other methods for predicting outcomes in prostate cancer: a critical analysis of the literature. Clin Cancer Res 14:4400–4407
Siegel R, Miller KD, Jemal A (2016) Cancer statistics, 2016. CA Cancer J Clin 66:7–30
Tang P, Chen H, Uhlman M et al (2013) A nomogram based on age, prostate-specific antigen level, prostate volume and digital rectal examination for predicting risk of prostate cancer. Asian J Androl 15:129–133
Vaiciūnas K, Auskalnis S, Matjosaitis A, Trumbeckas D, Jievaltas M (2007) Importance of prostate volume for detection of prostate cancer by first sextant biopsy in high-risk patients. Medicina (Kaunas) 43:285–290
Acknowledgements
This study was supported by the National Natural Science Foundation of China (81572536, 81672850), Science and Technology Commission of Shanghai Municipality (14140901700, 16411969800), the Joint Research Foundation for Innovative Medical Technology of Shanghai Shenkang Hospital Development Center (SHDC12015125), Shanghai Municipal Education Commission (15ZZ058), Shanghai Municipal Commission of Health and Family Planning (201640247), Shanghai Municipal Education Commission-Gaofeng Clinical Medicine Grant Support (20152215), Key Disciplines Group Construction Project of Pudong Health Bureau of Shanghai (PWZxq2014-05), the Shanghai Jiao Tong University School of Medicine Translational Research Innovation Fund (15ZH4002), and Incubating Program for clinical Research and Innovation of Renji Hospital Shanghai Jiao Tong University School of Medicine (PYZY16-008, PYXJS16-015).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Human rights
This study was approved by the Ethics Committee at the Renji Hospital, Shanghai Jiao Tong University School of Medicine. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Y. Wang and S. Xie contributed equally to the manuscript.
Rights and permissions
About this article
Cite this article
Wang, Y., Xie, S., Shangguan, X. et al. Prostate transitional zone volume-based nomogram for predicting prostate cancer and high progression prostate cancer in a real-world population. J Cancer Res Clin Oncol 143, 1157–1166 (2017). https://doi.org/10.1007/s00432-017-2389-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-017-2389-3