Abstract
The Cook Partisan Voting Index (PVI) determines how strongly a state leans toward the Democratic or Republican Party in US presidential elections compared to the nation. We set out to determine the correlation between childhood health outcomes and state-level partisanship using PVI. Sixteen measures of childhood health were obtained from several US governmental agencies for 2003–2017. The median PVI for every state was calculated for the same time period. Pearson’s rho determined the correlation between PVI and each health outcome. Multiple regression was also conducted, adjusting for educational attainment and percentage of non-White residents. We also compared childhood health in moderately Democratic and Republican states (5–9.9% more Democratic/Republican than the national mean) and, similarly, for extremely Democratic and Republican states (10% or more Democratic/Republican than the national mean), using Wilcoxon tests. For all 16 health measures, the median values in Democratic-leaning states represented better outcomes than Republican-leaning states (9/16 had a beta value for linear regression associated with P < 0.05). When compared to Republican states, the median values in moderately Democratic states represented better outcomes for 14 of 16 health measures (9/14 associated with P < 0.05). Similarly, the median values for extremely Democratic states represented better outcomes with regard to all 16 health measures, when compared to Republican-leaning states (8/16 associated with P < 0.05).
Conclusions: Democratic-leaning states displayed superior outcomes for multiple childhood health measures when compared to Republican counterpart states. Future research should investigate the significance of these findings and attempt to determine which state-level policies may have contributed to such disparate health outcomes.
What is Known: • In the United States, many health disparities exist among children along racial, economic and geographic lines. • Many US states lean strongly towards either the Democratic or Republican political parties in federal elections. | |
What is New: • Trends for multiple measures of childhood health vary in association with the political partisanship of the state being examined. • Multiple barometers of childhood health are superior in Democratic-leaning states, while no measures are better in Republican-leaning states. |

Similar content being viewed by others
Availability of data and materials
All material is publicly available online, as outlined in the methods section.
Code availability
All code is available in R Studio.
References
Nagle GA, Usry LR (2016) Using public health strategies to shape early childhood policy. Am J Orthopsychiatry 86:171–178. https://doi.org/10.1037/ort0000088
Ben-Shlomo Y, Kuh D (2002) A life course approach to chronic disease epidemiology: conceptual models, empirical challenges and interdisciplinary perspectives. Int J Epidemiol 31:285–293
Kalmakis KA, Chandler GE (2015) Health consequences of adverse childhood experiences: a systematic review. J Am Assoc Nurse Pract 27:457–465. https://doi.org/10.1002/2327-6924.12215
Chehade H, Simeoni U, Guignard JP, Boubred F (2018) Preterm birth: long term cardiovascular and renal consequences. Curr Pediatr Rev 14:219–226. https://doi.org/10.2174/1573396314666180813121652
Laditka JN, Laditka SB (2018) Lifetime disadvantages after childhood adversity: health problems limiting work and shorter life. Ann Am Acad Pol Soc Sci 680:259–277. https://doi.org/10.1177/0002716218795436
Wu XY, Kirk S, Ohinmaa A, Veugelers PJ (2017) The importance of health behaviours in childhood for the development of internalizing disorders during adolescence. BMC Psychol 5:38. https://doi.org/10.1186/s40359-017-0208-x
Maciosek MV, Coffield AB, Flottemesch TJ, Edwards NM, Solberg LI (2010) Greater use of preventive services in U.S. health care could save lives at little or no cost. Health Aff (Millwood) 29:1656–1660. https://doi.org/10.1377/hlthaff.2008.0701
Bjur KA, Wi CI, Ryu E, Derauf C, Crow S, King K, Juhn Y (2019) Socioeconomic status, race/ethnicity, and health disparities in children and adolescents in a mixed rural-urban community-Olmsted County. Minnesota Mayo Clin Proc 94:44–53. https://doi.org/10.1016/j.mayocp.2018.06.030
Subramania SV, Kawachi I, Kennedy BP (2001) Does the state you live in make a difference? Multilevel analysis of self-rated health in the US. Soc Sci Med 53:9–19. https://doi.org/10.1016/s0277-9536(00)00309-9
Hughes DC, Ng S (2003) Reducing health disparities among children. Future Child 13:153–167
Cheng TC, Lo CC (2016) Racial disparities in children’s health: a longitudinal analysis of mothers based on the multiple disadvantage model. J Community Health 41:753–760. https://doi.org/10.1007/s10900-016-0149-y
Kannan VD, Veazie PJ (2018) Political orientation, political environment, and health behaviors in the United States. Prev Med 114:95–101. https://doi.org/10.1016/j.ypmed.2018.06.011
Montez JK (2017) Deregulation, devolution, and state preemption laws’ impact on US mortality trends. Am J Public Health 107:1749–1750. https://doi.org/10.2105/AJPH.2017.304080
Wasserman D, Flinn A (2017) Introducing the 2017 Cook Political Report Partisan Voter Index. Cook Partisan Voter Index for the 115th Congress. https://cookpolitical.com/introducing-2017-cook-political-report-partisan-voter-index (Accessed 15 July 2020)
Wasserman D, Flinn A (2021) Introducing the 2021 Cook Political Report Partisan Voter Index. Cook Partisan Voter Index for the 117th Congress. https://cookpolitical.com/analysis/national/pvi/introducing-2021-cook-political-report-partisan-voter-index (Accessed 21 June 2021)
Leamon E, Bucelato J (2013) Federal Elections 2012: Election Results for the U.S. President, the U.S. Senate and the U.S. House of Representatives. ed: Federal Election Commission, Washinton, DC, pp. 6–8. https://www.fec.gov/resources/cms-content/documents/federalelections2012.pdf (Accessed 15 July 2020)
Leamon E, Bucelato J (2017) Federal Elections 2016: Election Results for the U.S. President, the U.S. Senate and the U.S. House of Representatives. ed: Federal Election Commission, Washinton, DC, pp. 6–8. https://www.fec.gov/resources/cms-content/documents/federalelections2016.pdf (Accessed 15 July 2020)
Leamon E, Bucelato J (2005) Federal Elections 2004: Election Results for the U.S. President, the U.S. Senate and the U.S. House of Representatives. ed: Federal Election Commission, Washinton, DC, pp. 6–8. https://www.fec.gov/resources/cms-content/documents/federalelections2004.pdf (Accessed 15 July 2020)
Leamon E, Bucelato J (2009) Federal Elections 2008: Election Results for the U.S. President, the U.S. Senate and the U.S. House of Representatives. ed: Federal Election Commission, Washinton, DC, pp. 6–8. https://www.fec.gov/resources/cms-content/documents/federalelections2008.pdf (Accessed 15 July 2020)
Meyer PA, Yoon PW, Kaufmann RB (2013) Introduction: CDC Health Disparities and Inequalities Report - United States, 2013. MMWR Suppl 62:3–5
"State Population by Characteristics," ed: US Census Bureau, 2010–2019 (2021) ed: Washington, D.C.: United States Census Bureau
Public high school 4-year adjusted cohort graduation rate (ACGR), by selected student characteristics and state: 2010–2018 (2020) ed: Washington, D.C.: National Center for Education Statistics, 2010–2018. https://nces.ed.gov/programs/digest/d19/tables/dt19_219.46.asp (Accessed 1 April 2021)
Shi Y, Hunter Guevara L, Dykhoff H, Sangaralingham L, Phelan S, Zaccariello M, Warner D (2021) Racial disparities in diagnosis of attention-deficit/hyperactivity disorder in a US national birth cohort. JAMA Netw Open 4:e210321. https://doi.org/10.1001/jamanetworkopen.2021.0321
Testa A, Jackson DB (2021) Race, ethnicity, WIC participation, and infant health disparities in the United States. Ann Epidemiol 58:22–28. https://doi.org/10.1016/j.annepidem.2021.02.005
Zahnd WE et al (2021) The intersection of rural residence and minority race/ethnicity in cancer disparities in the United States. Int J Environ Res Public Health 18:1384. https://doi.org/10.3390/ijerph18041384
Marin JR et al (2020) Racial and ethnic differences in emergency department diagnostic imaging at US children’s hospitals, 2016–2019. JAMA Netw Open 4:e2033710. https://doi.org/10.1001/jamanetworkopen.2020.33710
Mitchell HK, Reddy A, Montoya-Williams D, Harhay M, Fowler JC, Yehya N (2021) Hospital outcomes for children with severe sepsis in the USA by race or ethnicity and insurance status: a population-based, retrospective cohort study. Lancet Child Adolesc Health 5:103–112. https://doi.org/10.1016/s2352-4642(20)30341-2
Prickett KC, Augustine JM (2016) Maternal education and investments in children’s health. J Marriage Fam 78:7–25. https://doi.org/10.1111/jomf.12253
Torvik FA et al (2020) Mechanisms linking parental educational attainment with child ADHD, depression, and academic problems: a study of extended families in The Norwegian Mother, Father and Child Cohort Study. J Child Psychol Psychiatry 61:1009–1018. https://doi.org/10.1111/jcpp.13197
Bycoffe A, Koeze E, Wasserman D, Silver N (2018) We drew 2,568 congressional districts by hand. Here’s How. FiveThirtyEight. https://fivethirtyeight.com/features/we-drew-2568-congressional-districts-by-hand-heres-how/ (accessed 8 May 2020)
Population, Population Change, and Estimated Components of Population Change: April 1, 2010 to July 1, 2019 (2020) Census.gov, Ed., ed. Washington, D.C.: United States Census Bureau. https://www.census.gov/data/tables/time-series/demo/popest/2010s-national-total.html (Accessed 1 Feb 2021)
Gilbert SM, Pow-Sang JM, Xiao H (2016) Geographical factors associated with health disparities in prostate cancer. Cancer Control 23:401–408. https://doi.org/10.1177/107327481602300411
Graham-Garcia J, Raines TL, Andrews JO, Mensah GA (2001) Race, ethnicity, and geography: disparities in heart disease in women of color. J Transcult Nurs 12:56–67. https://doi.org/10.1177/104365960101200108
Zhan FB, Lin Y (2014) Racial/Ethnic, socioeconomic, and geographic disparities of cervical cancer advanced-stage diagnosis in Texas. Womens Health Issues 24:519–527. https://doi.org/10.1016/j.whi.2014.06.009
Holt JB, Zhang X, Presley-Cantrell L, Croft JB (2011) Geographic disparities in chronic obstructive pulmonary disease (COPD) hospitalization among Medicare beneficiaries in the United States. Int J Chron Obstruct Pulmon Dis 6:321–328. https://doi.org/10.2147/COPD.S19945
Navarro V, Muntaner C, Borrell C, Benach J, Quiroga A, Rodriguez-Sanz M, Verges N, Pasarin NI (2006) Politics and health outcomes. Lancet 368:1033–1037. https://doi.org/10.1016/s0140-6736(06)69341-0
Status of State Action on the Medicaid Expansion Decision (2014) ed: Kaiser Family Foundation. https://www.kff.org/health-reform/state-indicator/state-activity-around-expanding-medicaid-under-the-affordable-care-act/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D (Accessed 16 Oct 2020)
A. Prokop (2015) The battle over Medicaid expansion in 2013 and 2014, explained. ed: Vox. https://www.vox.com/2015/1/27/18088994/medicaid-expansion-explained (Accessed 1 Dec 2020)
Bhatt CB, Beck-Sagué CM (2018) Medicaid expansion and infant mortality in the United States. Am J Public Health 108:565–567. https://doi.org/10.2105/AJPH.2017.304218
Rushovich T, Boulicault M, Chen JT, Danielsen AC, Tarrant A, Richardson SS, Shattuck-Heidorn, H (2021) Sex disparities in COVID-19 mortality vary across US racial groups. J Gen Intern Med 36:1696–1701. https://doi.org/10.1007/s11606-021-06699-4
Campbell O, Bann D, Patalay P (2021) The gender gap in adolescent mental health: a cross-national investigation of 566,829 adolescents across 73 countries. SSM Popul Health 13:100742. https://doi.org/10.1016/j.ssmph.2021.100742
Hollingshead NA, Vrany EA, Hsueh L, Stewart JC, Hirsh AT (2021) Language use and generation status are associated with chronic pain differences in Mexican Americans. J Immigr Minor Health. 2021 Mar 16. https://doi.org/10.1007/s10903-021-01160-4
Huebinger R et al (2021) "Community disparities in out of hospital cardiac arrest care and outcomes in Texas," (in eng), Resuscitation, Mar 30 2021. https://doi.org/10.1016/j.resuscitation.2021.03.021
Holmen JE et al (2021) Relationship between neighborhood census-tract level socioeconomic status and respiratory syncytial virus-associated hospitalizations in U.S. adults, 2015–2017. BMC Infect Dis. 21:293. https://doi.org/10.1186/s12879-021-05989-w
Huang C, Liu H, Jia L, Lu M, Hu S (2021) Survival disparities in multiple myeloma by health insurance status among US non-elderly adults: a SEER-based comparative analysis. Acta Haematol 30:1–9. https://doi.org/10.1159/000514671
Shi T, Jiang C, Zhu C, Wu F, Fotjhadi I, Zarich S (2021) Insurance disparity in cardiovascular mortality among non-elderly cancer survivors. Cardiooncology 7:11. https://doi.org/10.1186/s40959-021-00098-8
Roy M, Purington N, Liu M, Blayney DW, Kurian AW, Schapira L (2021) Limited English proficiency and disparities in health care engagement among patients with breast cancer. JCO Oncol Pract 2021 Apr 12:OP2001093. https://doi.org/10.1200/op.20.01093.
Author information
Authors and Affiliations
Contributions
Megan Paul helped conceptualize and design the study, collected the data, carried out the initial analyses, drafted the initial manuscript, and reviewed and revised the manuscript. Dr. Brian A. Coakley conceptualized and designed the study, collected the data, and drafted, reviewed, and revised the manuscript. Dr. Bian Liu and Ruya Zhang reviewed the initial analyses and critically reviewed the manuscript for important intellectual content. Dr. Payam Saadai critically reviewed the manuscript for important intellectual content. All the authors approved the final manuscript as submitted and agreed to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Ethics approval
This study was exempt from IRB approval given that it used publicly available data.
Consent for publication
All the authors involved consent for the publication of this manuscript.
Conflict of interest
The authors declare no competing interests.
Additional information
Communicated by Gregorio Paolo Milani
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
431_2021_4203_MOESM1_ESM.pdf
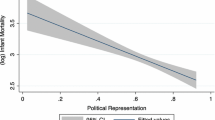
Supplementary file1 (PDF 500 KB) Supplementary Fig. 1 Unadjusted Bivariate Regression of PVI vs. 16 Childhood Health Outcomes. The median PVI and variable of interest from 2004 to 2016 are displayed for each state in the scatterplots above.
431_2021_4203_MOESM2_ESM.pdf
Supplementary file2 (PDF 209 KB) Supplementary Fig. 2 Childhood Health Outcomes in Democratic vs. Republican States (Top Right): All health outcomes that were percentages are graphed. (Top Left): Life expectancy at birth is graphed (Bottom Left): All health outcomes that were graphed as rate per 1000 children. (Bottom Right): All health outcomes that were graphed as rate per 1000 children For all graphs, note that the boxes represent the interquartile range while the bars represent the minimum and maximum.
Rights and permissions
About this article
Cite this article
Paul, M., Zhang, R., Liu, B. et al. State-level political partisanship strongly correlates with health outcomes for US children. Eur J Pediatr 181, 273–280 (2022). https://doi.org/10.1007/s00431-021-04203-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-021-04203-y