Abstract
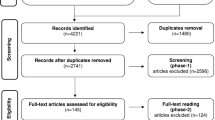
The aim of the present study was to perform a critical reflection about intervention options for bruxism reduction in children and adolescents. Search was conducted based on the PICO-structured question: “What are the intervention options to reduce bruxism in children/adolescents?”. No language, year, or study design restrictions were imposed. Studies reporting interventions to reduce bruxism in children (< 10) and adolescents (10 to 19 years old) were included. Reviews and letters to editors were not included. From 2723 records, 17 papers were included. Included studies were primarily randomized clinical trials performed in Brazil (35.3%) and using different criteria for the diagnosis of bruxism. Reduction in self-reported bruxism and headaches associated with bruxism were observed in studies that used medications (hydroxyzine/trazodone/flurazepam), occlusal splints, orthodontic interventions, and psychological and physical therapy interventions. Reduction in Rhythmic Masticatory Muscle Activity was observed with the use of the occlusal splint and in orthodontic interventions. Alternative treatments (medicinal extracts such as Melissa officinalis-L) have shown inconclusive results.
Conclusions: Several intervention options are available to inhibit or reduce bruxism activity. The respective indication, contraindications, and side effects of each treatment option must be assessed individually and carefully, taking into account that bruxism is not considered a disorder in otherwise healthy individuals.
What is known • Biological and psychological factors have been strongly correlated to the development of bruxism • Bruxism prevalence ranging from 6 to 50% in children | |
What is new • Reduction in self-reported bruxism and headaches associated with bruxism were observed in studies that used medication (Hydroxyzine/ Trazodone/ Flurazepam), occlusal splints, orthodontic interventions, psychological, and physical therapy interventions • A reduction in Rhythmic Masticatory Muscle Activity was observed with the use of the occlusal splint and orthodontic interventions. Alternative treatments (medicinal extracts such as Melissa officinalis L) show inconclusive results in respect of the reduction in bruxism |

Similar content being viewed by others
Abbreviations
- CC:
-
Clinical case
- CS:
-
Cross-sectional
- CT:
-
Clinical trial
- F:
-
Feminine
- GABA:
-
Gamma-aminobutyric acid
- IADR:
-
International Association for Dental Research
- ICSD:
-
International Classification of Sleep Disorders for bruxism
- M:
-
Masculine
- Mg:
-
Milligram
- N:
-
Number of individual in bruxism treatment
- NR:
-
Not reported
- NS:
-
Not specified (NS)
- RCT:
-
Randomized clinical trial
- RDC:
-
Research Diagnostic Criteria
- REM:
-
Rapid eye movement sleep
- RMMA:
-
Rhythmic masticatory muscle activity
- SB:
-
Sleep bruxism
- TMD:
-
Temporomandibular disorders
- Vs:
-
Versus
References
Lobbezoo F, Ahlberg J, Glaros AG, Kato T, Koyano K, Lavigne GJ, de Leeuw R, Manfredini D, Svensson P, Winocur E (2013) Bruxism defined and graded: an international consensus. J Oral Rehabil 40:2–4. https://doi.org/10.1111/joor.12011
Lobbezoo F, Ahlberg J, Raphael KG, Wetselaar P, Glaros AG, Kato T, Santiago V, Winocur E, De Laat A, De Leeuw R, Koyano K, Lavigne GJ, Svensson P, Manfredini D (2018) International consensus on the assessment of bruxism: report of a work in progress. J Oral Rehabil 45:837–844 https://doi.org/10.1111/joor.12663
Ophoff D, Slaats MA, Boudewyns A, Glazemakers I, Van Hoorenbeeck K, Verhulst SL (2018) Sleep disorders during childhood: a practical review. Eur J Pediatr 177:641–648. https://doi.org/10.1007/s00431-018-3116-z
Barbosa TS, Miyakoda LS, Pocztaruk RL, Rocha CP, Gavião MB (2008) Temporomandibular disorders and bruxism in childhood and adolescence: review of the literature. Int J Pediatr Otorhinolaryngol 72:299–314 https://doi.org/10.1016/j.ijporl.2007.11.006
Antonio AG, Pierro VS, Maia LC (2006) Bruxism in children: a warning sign for psychological problems. J Can Dent Assoc 72:155–159
Restrepo CC, Vásquez LM, Alvarez M, Valencia I (2008) Personality traits and temporomandibular disorders in a group of children with bruxing behaviour. J Oral Rehabil 35:585–593 https://doi.org/10.1111/j.1365-2842.2007.01838.x
Cheifetz AT, Osganian SK, Allred EN, Needleman HL (2005) Prevalence of bruxism and associated correlates in children as reported by parents. J Dent Child (Chic) 72:67–73
Manfredini D, Serra-Negra J, Carboncini F, Lobbezoo F (2017) Current concepts of bruxism. Int J Prosthodont 30:437–438. https://doi.org/10.11607/ijp.5210
Katsaros C (2001) Masticatory muscle function and transverse dentofacial growth. Swed Dent J Suppl:1–47
Manfredini D, Winocur E, Guarda-Nardini L, Paesani D, Lobbezoo F (2013) Epidemiology of bruxism in adults: a systematic review of the literature. J Orofac Pain 27:99–110. https://doi.org/10.11607/jop.921
Machado E, Dal-Fabbro C, Cunali PA, Kaizer OB (2014) Prevalence of sleep bruxism in children: a systematic review. Dental Press J Orthod 19:54–61 https://doi.org/10.1590/2176-9451.19.6.054-061.oar
Manfredini D, Restrepo C, Diaz-Serrano K, Winocur E, Lobbezoo F (2013) Prevalence of sleep bruxism in children: a systematic review of the literature. J Oral Rehabil 40:631–642. https://doi.org/10.1111/joor.12069
Restrepo C, Gómez S, Manrique R (2009) Treatment of bruxism in children: a systematic review. Quintessence Int 40:849–855
Arksey H, O’Malley L (2005) Scoping studies: towards a methodological framework. Int J Soc Res Methodol 8:19–32
Conde MC, Chisini LA, Sarkis-Onofre R, Schuch HS, Nor JE, Demarco FF (2017) A scoping review of root canal revascularization: relevant aspects for clinical success and tissue formation. Int Endod J 50:860–874. https://doi.org/10.1111/iej.12711
Rizk M, Aziz J, Shorr R, Allan DS (2017) Cell-based therapy using umbilical cord blood for novel indications in regenerative therapy and immune modulation: an updated systematic scoping review of the literature. Biol Blood Marrow Transplant 23:1607–1613. https://doi.org/10.1016/j.bbmt.2017.05.032
Chisini LA, Conde MCM, Grazioli G, Martin ASS, Carvalho RV, Nor JE, Demarco FF (2017) Venous blood derivatives as FBS-substitutes for mesenchymal stem cells: a systematic scoping review. Braz Dent J 28:657–668. https://doi.org/10.1590/0103-6440201701646
Chisini LA, Conde MCM, Grazioli G, Martin ASS, Carvalho RV, Sartori LRM, Demarco FF (2019) Bone, periodontal and dental pulp regeneration in dentistry: a systematic scoping review. Braz Dent J 30:77–95. https://doi.org/10.1590/0103-6440201902053
Carra MC, Huynh N, Fleury B, Lavigne G (2015) Overview on sleep bruxism for sleep medicine clinicians. Sleep Med Clin 10:375–384. https://doi.org/10.1016/j.jsmc.2015.05.005
Carra MC, Huynh N, Morton P, Rompré PH, Papadakis A, Remise C, Lavigne GJ (2011) Prevalence and risk factors of sleep bruxism and wake-time tooth clenching in a 7- to 17-yr-old population. Eur J Oral Sci 119:386–394. https://doi.org/10.1111/j.1600-0722.2011.00846.x
de Oliveira MT, Bittencourt ST, Marcon K, Destro S, Pereira JR (2015) Sleep bruxism and anxiety level in children. Braz Oral Res 29:1–5. https://doi.org/10.1590/1807-3107BOR-2015.vol29.0024
Murad MH, Sultan S, Haffar S, Bazerbachi F (2018) Methodological quality and synthesis of case series and case reports. BMJ Evid Based Med 23:60–63 https://doi.org/10.1136/bmjebm-2017-110853
Bortoletto CC, Cordeiro da Silva F, Silva PFC, Leal de Godoy CH, Albertini R, Motta LJ, Mesquita-Ferrari RA, Fernandes KP, Romano R, Bussadori SK (2014) Evaluation of cranio-cervical posture in children with bruxism before and after bite plate therapy: a pilot project. J Phys Ther Sci 26:1125–1128. https://doi.org/10.1589/jpts.26.1125
Meltzer LJ, Plaufcan MR, Thomas JH, Mindell JA (2014) Sleep problems and sleep disorders in pediatric primary care: treatment recommendations, persistence, and health care utilization. J Clin Sleep Med 10:421–426. https://doi.org/10.5664/jcsm.3620
Stuhr SH, Earnshaw DH, Duncombe AM (2014) Use of orthopedic manual physical therapy to manage chronic orofacial pain and tensiontype headache in an adolescent. J Man Manip Ther 22:51–58. https://doi.org/10.1179/2042618613Y.0000000054
Karibe H, Shimazu K, Okamoto A, Kawakami T, Kato Y, Warita-Naoi S (2015) Prevalence and association of self-reported anxiety, pain, and oral parafunctional habits with temporomandibular disorders in Japanese children and adolescents: a cross-sectional survey BMC Oral Health 15-8 https://doi.org/10.1186/1472-6831-15-8
Barão VA, Gallo AK, Zuim PR, Garcia AR, Assunção WG (2011) Effect of occlusal splint treatment on the temperature of different muscles in patients with TMD. J Prosthodont Res 55:19–23 https://doi.org/10.1016/j.jpor.2010.06.001
Kurt H, Alioğlu C, Karayazgan B, Tuncer N, Kılıçoğlu H (2011) The effects of two methods of class III malocclusion treatment on temporomandibular disorders. Eur J Orthod 33:636–641. https://doi.org/10.1093/ejo/cjq114
Soares AS, Medeiros de Oliveira M, Burlamarqui Klautau E, Alves BP, da Silva Gomes CEV (2015) Analysis of the effectiveness of the type of equipment occlusive plan and soft in relief of pain in temporomandibular disorder. Oral Pathol Oral Med:389–398
Wahlund K, Nilsson IM, Larsson B (2015) Treating temporomandibular disorders in adolescents: a randomized, controlled, sequential comparison of relaxation training and occlusal appliance therapy. J Oral Facial Pain Headache 29:41–50. https://doi.org/10.11607/ofph.1285
Wahlund K, List T, Larsson B (2003) Treatment of temporomandibular disorders among adolescents: a comparison between occlusal appliance, relaxation training, and brief information. Acta Odontol Scand 61:203–211
Reimão R, Lefévre AB (1982) Evaluation of flurazepam and placebo on sleep disorders in childhood. Arq Neuropsiquiatr 40:1–13
Oliveira M, Bressan T, Pamato S, Niehues A, Niehues N, Netto J, Bittencourt S (2013) Bruxism in children - effectiveness of bite splints. Acoust Speech Signal Process Newslett 2:22–29
Restrepo CC, Medina I, Patiño I (2011) Effect of occlusal splints on the temporomandibular disorders, dental wear and anxiety of bruxist children. Eur J Dent 5:441–450
Jones CM (1993) Chronic headache and nocturnal bruxism in a 5-year-old child treated with an occlusal splint. Int J Paediatr Dent 3:95–97
Carra M, Huynh N, El-Khatib H, Remise C, Lavigne G (2013) Sleep bruxism, snoring, and headaches in adolescents: short-term effects of a mandibular advancement appliance. Sleep Med 14:656–661. https://doi.org/10.1016/j.sleep.2013.03.009
Egermark I, Rönnerman A (1995) Temporomandibular disorders in the active phase of orthodontic treatment. J Oral Rehabil 22:613–618
Giannasi LC, Santos IR, Alfaya TA, Bussadori SK, Leitão-Filho FS, de Oliveira LV (2015) Effect of a rapid maxillary expansion on snoring and sleep in children: a pilot study. Cranio 33:169–173. https://doi.org/10.1179/2151090314Y.0000000029
Bellerive A, Montpetit A, El-Khatib H, Carra MC, Remise C, Desplats E, Huynh N (2015) The effect of rapid palatal expansion on sleep bruxism in children. Sleep Breath 19:1265–1271 https://doi.org/10.1007/s11325-015-1156-4
Restrepo CC, Alvarez E, Jaramillo C, Vélez C, Valencia I (2001) Effects of psychological techniques on bruxism in children with primary teeth. J Oral Rehabil 28:354–360
Ghanizadeh A, Zare S (2013) A preliminary randomised double-blind placebo-controlled clinical trial of hydroxyzine for treating sleep bruxism in children. J Oral Rehabil 40:413–417 https://doi.org/10.1111/joor.12049
Ghanizadeh A (2013) Treatment of bruxism with hydroxyzine. Eur Rev Med Pharmacol Sci 17:839–841
Shakibaei F, Gholamrezaei A, Heidari S (2008) Effect of trazodone on sleep bruxism in children and adolescents 6-18 years of age, a pilot study. J Res Med Sci 13:29–33
Mostafavi SN, Jafari A, Hoseini SG, Khademian M, Kelishadi R (2019) The efficacy of low and moderate dosage of diazepam on sleep bruxism in children: a randomized placebo-controlled clinical trial. J Res Med Sci 24:8. https://doi.org/10.4103/jrms.JRMS_131_18
Quintero Y, Restrepo CC, Tamayo V, Tamayo M, Vélez AL, Gallego G, Peláez-Vargas A (2009) Effect of awareness through movement on the head posture of bruxist children. J Oral Rehabil 36:18–25. https://doi.org/10.1111/j.1365-2842.2008.01906.x
Bortoletto CC, Cordeiro da Silva F, Salgueiro MCC, Motta LJ, Curiki LM, Mesquita-Ferarri RA, Fernandes KPS, Bussadori SK (2016) Evaluation of electromyographic signals in children with bruxism before and after therapy with Melissa Officinalis L-a randomized controlled clinical trial. J Phys Ther Sci 28:738–742
Silva CT, Primo LG, Mangabeira A, Maia LC, Fonseca-Goncalves A (2017) Homeopathic therapy for sleep bruxism in a child: findings of a 2-year case report. J Indian Soc Pedod Prev Dent 35:381–383. https://doi.org/10.4103/JISPPD.JISPPD_49_17
Tavares-Silva C, Holandino C, Homsani F, Luiz RR, Prodestino J, Farah A, Lima JP, Simas RC, Castilho CVV, Leitão SG, Maia LC, Fonseca-Gonçalves A (2019) Homeopathic medicine of Melissa officinalis combined or not with Phytolacca decandra in the treatment of possible sleep bruxism in children: a crossover randomized triple-blinded controlled clinical trial. Phytomedicine 58:152869. https://doi.org/10.1016/j.phymed.2019.152869
Buysse DJ, Young T, Edinger JD, Carroll J, Kotagal S (2003) Clinicians' use of the International Classification of Sleep Disorders: results of a national survey. Sleep 26:48–51
Manfredini D, Ahlberg J, Winocur E, Lobbezoo F (2015) Management of sleep bruxism in adults: a qualitative systematic literature review. J Oral Rehabil 42:862–874 https://doi.org/10.1111/joor.12322
Raphael KG, Marbach JJ, Klausner JJ, Teaford MF, Fischoff DK (2003) Is bruxism severity a predictor of oral splint efficacy in patients with myofascial face pain? J Oral Rehabil 30:17–29
Restrepo CC, Medina I, Patiño I (2011) Effect of occlusal splints on the temporomandibular disorders, dental wear and anxiety of bruxist children. Eur J Dent 5:441–450
Restrepo C, Manfredini D, Castrillon E, Svensson P, Santamaria A, Alvarez C, Manrique R, Lobbezoo F (2017) Diagnostic accuracy of the use of parental-reported sleep bruxism in a polysomnographic study in children. Int J Paediatr Dent 27:318–325
Manfredini D, Ahlberg J, Castroflorio T, Poggio CE, Guarda-Nardini L, Lobbezoo F (2014) Diagnostic accuracy of portable instrumental devices to measure sleep bruxism: a systematic literature review of polysomnographic studies. J Oral Rehabil 41:836–842. https://doi.org/10.1111/joor.12207
Restrepo C, Lobbezoo F, Castrillon E, Svensson P, Santamaria A, Alvarez C, Manrique R, Manfredini D (2017) Agreement between jaw-muscle activity measurement with portable single-channel electromyography and polysomnography in children. Int J Paediatr Dent. https://doi.org/10.1111/ipd.12308
Sommer I, Lavigne G, Ettlin DA (2015) Review of self-reported instruments that measure sleep dysfunction in patients suffering from temporomandibular disorders and/or orofacial pain. Sleep Med 16:27–38. https://doi.org/10.1016/j.sleep.2014.07.023
Guaita M, Hogl B (2016) Current treatments of bruxism. Curr Treat Options Neurol 18:10. https://doi.org/10.1007/s11940-016-0396-3
Guo H, Wang T, Li X, Ma Q, Niu X, Qiu J (2017) What sleep behaviors are associated with bruxism in children? A systematic review and meta-analysis. Sleep Breath 21:1013–1023. https://doi.org/10.1007/s11325-017-1496-3
Castroflorio T, Bargellini A, Rossini G, Cugliari G, Deregibus A (2017) Sleep bruxism in adolescents: a systematic literature review of related risk factors. Eur J Orthod 39:61–68. https://doi.org/10.1093/ejo/cjw012
Lavigne GJ, Khoury S, Abe S, Yamaguchi T, Raphael K (2008) Bruxism physiology and pathology: an overview for clinicians. J Oral Rehabil 35:476–494. https://doi.org/10.1111/j.1365-2842.2008.01881.x
Khoury S, Rouleau GA, Rompré PH, Mayer P, Montplaisir JY, Lavigne GJ (2008) A significant increase in breathing amplitude precedes sleep bruxism. Chest 134:332–337. https://doi.org/10.1378/chest.08-0115
Castrillon EE, Exposto FG (2018) Sleep bruxism and pain. Dent Clin N Am 62:657–663
Muzalev K, Visscher CM, Koutris M, Lobbezoo F (2018) Long-term variability of sleep bruxism and psychological stress in patients with jaw-muscle pain: report of two longitudinal clinical cases. J Oral Rehabil 45:104–109. https://doi.org/10.1111/joor.12594
Author information
Authors and Affiliations
Contributions
Luiz Alexandre Chisini: Conception of the design, write the paper, participate of data collection, perform the literature review and data analysis. Alissa Schmidt San Martin: Participate of data collection, perform the literature review Mariana Cademartori: Review of paper Noeli Boscato: Review of paper Marcos Correa: Review of paper Marilia Goettems: Conception of the design and review of paper.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chisini, L.A., San Martin, A.S., Cademartori, M.G. et al. Interventions to reduce bruxism in children and adolescents: a systematic scoping review and critical reflection. Eur J Pediatr 179, 177–189 (2020). https://doi.org/10.1007/s00431-019-03549-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-019-03549-8