Abstract
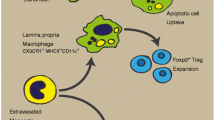
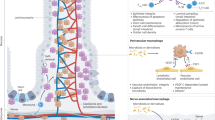
The resident macrophages of the gastrointestinal tract represent the largest population of macrophages in the human body and are usually located in the subepithelial lamina propria. This strategic location guarantees a first-line defense to the huge numbers of potentially harmful bacteria and antigenic stimuli that are present in the intestinal lumen. In non-inflamed mucosa, macrophages phagocytose and kill microbes in the absence of an inflammatory response. However, in the event of an epithelial breach and/or microbial invasion, new circulating monocytes and lymphocytes will be recruited to the damaged area of the gut, which will result in the secretion of proinflammatory mediators and engage a protective inflammatory response. Although macrophages are usually not conspicuous in normal mucosal samples of the gut, they can easily be detected when they accumulate exogenous particulate material or endogenous substances or when they become very numerous. These events will mostly occur in pathologic conditions, and this review presents an overview of the diseases which are either mediated by or affecting the resident macrophages of the gut.




Similar content being viewed by others
References
Valledor AF, Borras FE, Cullell-Young M, Celada A (1998) Transcription factors that regulate monocyte/macrophage differentiation. J Leukoc Biol 63:405–417
Gordon S, Clarke S, Greaves D, Doyle A (1995) Molecular immunobiology of macrophages—recent progress. Curr Opin Immunol 7:24–33
Smythies LE, Sellers M, Clements RH et al (2005) Human intestinal macrophages display profound inflammatory anergy despite avid phagocytic and bacteriocidal activity. J Clin Invest 115:66–75
Smythies LE, Shen RZ, Bimczok D et al (2010) Inflammation anergy in human intestinal macrophages is due to SMAD-induced I kappa B alpha expression and NF-kappa B inactivation. J Biol Chem 285:19593–19604
Smith PD, Smythies LE, Shen R, Greenwell-Wild T, Gliozzi M, Wahl SM (2011) Intestinal macrophages and response to microbial encroachment. Mucosal Immunol 4:31–42
Smythies LE, Maheshwari A, Clements R et al (2006) Mucosal IL-8 and TGF-beta recruit blood monocytes: evidence for cross-talk between the lamina propria stroma and myeloid cells. J Leukoc Biol 80:492–499
Eidelman S, Lagunoff D (1972) Morphology of normal human rectal biopsy. Hum Pathol 3:389–401
Kunisch E, Fuhrmann R, Roth A, Winter R, Lungershausen W, Kinne RW (2004) Macrophage specificity of three anti-CD68 monoclonal antibodies (KP1, EBM11, and PGM1) widely used for immunohistochemistry and flow cytometry. Ann Rheum Dis 63:774–784
Ramprasad MP, Terpstra V, Kondratenko N, Quehenberger O, Steinberg D (1996) Cell surface expression of mouse macrosialin and human CD68 and their role as macrophage receptors for oxidized low density lipoprotein. PNAS 93:14833–14838
Strobl H, Scheinecker C, Csmarits B, Majdic O, Knapp W (1995) Flow cytometric analysis of intracellular Cd68 molecule expression in normal and malignant hematopoiesis. Br J Haematol 90:774–782
Greaves DR, Gordon S (2002) Macrophage-specific gene expression: current paradigms and future challenges. Int J Hematol 76:6–15
Donato R (2003) Intracellular and extracellular roles of S100 proteins. Micros Res Technol 60:540–551
Selby WS, Poulter LW, Hobbs S, Jewell DP, Janossy G (1983) Heterogeneity of Hla-Dr-positive histiocytes in human intestinal lamina propria—a combined histochemical and immunohistological analysis. J Clin Pathol 36:379–384
Freeman HA (2008) “Melanosis” in the small and large intestine. World J Gastroenterol 14:4296–4299
Marginean EC, Bennick M, Cyczk J, Robert ME, Jain D (2006) Gastric siderosis—patterns and significance. Am J Surg Pathol 30:514–520
Yantiss RK, Goldman H, Odze RD (2001) Hyperplastic polyp with epithelial misplacement (inverted hyperplastic polyp): a clinicopathologic and immunohistochemical study of 19 cases. Mod Pathol 14:869–875
Parker RL, Dadmanesh F, Young RH, Clement PB (2004) Polypoid endometriosis—a clinicopathologic analysis of 24 cases and a review of the literature. Am J Surg Pathol 28:285–297
Kato S, Hashiguchi K, Yamamoto R et al (2006) Jumbo biopsy is useful for the diagnosis of colonic prolapsing mucosal polyps with diverticulosis. World J Gastroenterol 12:1634–1636
Shepherd NA, Crocker PR, Smith AP, Levison DA (1987) Exogenous pigment in Peyers-patches. Hum Pathol 18:50–54
Urbanski SJ, Arsenault AL, Green FHY, Haber G (1989) Pigment resembling atmospheric dust in Peyers patches. Mod Pathol 2:222–226
Powell JJ, Ainley CC, Harvey RSJ et al (1996) Characterisation of inorganic microparticles in pigment cells of human gut associated lymphoid tissue. Gut 38:390–395
Levine DS, Haggitt RC (1989) Normal histology of the colon. Am J Surg Pathol 13:966–984
Goldman H, Antonioli DA (1982) Mucosal biopsy of the rectum, colon, and distal ileum. Hum Pathol 13:981–1012
Lou TY, Teplitz C, Thayer WR (1971) Ultrastructural morphogenesis of colonic Pas-positive macrophages (colonic histiocytosis). Hum Pathol 2:421–439
Bejarano PA, Aranda-Michel J, Fenoglio-Preiser C (2000) Histochemical and immunohistochemical characterization of foamy histiocytes (muciphages and xanthelasma) of the rectum. Am J Surg Pathol 24:1009–1015
Coletta U, Sturgill BC (1985) Isolated xanthomatosis of the small bowel. Hum Pathol 16:422–424
Scheiman J, Elta G, Colturi T, Nostrant T (1988) Colonic xanthomatosis—relationship to disordered motility and review of the literature. Dig Dis Sci 33:1491–1494
Melling N, Bruder E, Dimmler A, Hohenberger W, Aigner T (2007) Localised massive tumourous xanthomatosis of the small intestine. Int J Colorectal Dis 22:1401–1404
Romeu J, Rybak B (1979) Lipid proctitis. N Engl J Med 301:1099–1100
Remmele W, Beck K, Kaiserling E (1988) Multiple lipid islands of the colonic mucosa—a light and electron-microscopic study. Pathol Res Pract 183:336–342
Schneider T, Moos V, Loddenkemper C, Marth T, Fenollar F, Raoult D (2008) Whipple's disease: new aspects of pathogenesis and treatment. Lancet Infect Dis 8:179–190
Desnues B, Al Moussawi K, Fenollar F (2010) New insights into Whipple's disease and Tropheryma whipplei infections. Microbes Infect 12:1102–1110
Marth T, Roux M, Vonherbay A, Meuer SC, Feurle GE (1994) Persistent reduction of complement receptor-3 alpha-chain expressing mononuclear blood-cells and transient inhibitory serum factors in Whipples-disease. Clin Immunol Immunopathol 72:217–226
Bai J, Sen L, Diez R et al (1996) Monocyte function in patients successfully treated for Whipple's disease. Acta Gastroenterologica Latinoam 26:85–89
Bjerknes R, Laerum OD, Odegaard S (1985) Impaired bacterial-degradation by monocytes and macrophages from a patient with treated Whipple's disease. Gastroenterology 89:1139–1146
Marth T, Kleen N, Stallmach A et al (2002) Dysregulated peripheral and mucosal Th1/Th2 response in Whipple's disease. Gastroenterology 123:1468–1477
Marth T, Neurath M, Cuccherini BA, Strober W (1997) Defects of monocyte interleukin 12 production and humoral immunity in Whipple's disease. Gastroenterology 113:442–448
Marcial MA, Villafana M (1997) Whipple's disease with esophageal and colonic involvement: endoscopic and histopathologic findings. Gastrointest Endosc 46:263–266
Fenollar F, Fournier PE, Robert C, Raoult D (2004) Use of genome selected repeated sequences increases the sensitivity of PCR detection of Tropheryma whipplei. J Clin Microbiol 42:401–403
Baisden BL, Lepidi H, Raoult D, Argani P, Yardley JH, Dumler JS (2002) Diagnosis of Whipple disease by immunohistochemical analysis—a sensitive and specific method for the detection of Tropheryma whipplei (the Whipple bacillus) in paraffin-embedded tissue. Am J Clin Pathol 118:742–748
Fenollar F, Raoult D (2010) How should classic Whipple disease be managed? Nat Rev Gastroenterol Hepatol 7:246–248
Feurle GE, Junga NS, Marth T (2010) Efficacy of ceftriaxone or meropenem as initial therapies in Whipple's disease. Gastroenterology 138:478–486
Mendoza JL, Lana R, Diaz-Rubio M (2009) Mycobacterium avium subspecies paratuberculosis and its relationship with Crohn's disease. World J Gastroenterol 15:417–422
Hamrock D, Azmi FH, O'Donnell E, Gunning WT, Philips ER, Zaher A (1999) Infection by Rhodococcus equi in a patient with AIDS: histological appearance mimicking Whipple's disease and Mycobacterium avium-intracellulare infection. J Clin Pathol 52:68–71
Ehrt S, Schnappinger D (2009) Mycobacterial survival strategies in the phagosome: defence against host stresses. Cell Microbiol 11:1170–1178
Almadi MA, Aljebreen AM, Sanai FM, Marcus V, AlMeghaiseeb ES, Ghosh S (2011) New insights into gastrointestinal and hepatic granulomatous disorders. Nat Rev Gastroenterol Hepatol 8:455–466
Radzi M, Rihan N, Vijayalakshmi N, Pani SP (2009) Diagnostic challenge of gastrointestinal tuberculosis: a report of 34 cases and an overview of the literature. Southeast Asian J Trop Med Public Health 40:505–510
Giouleme O, Paschos P, Katsaros M et al (2011) Intestinal tuberculosis: a diagnostic challenge—case report and review of the literature. Eur J Gastroenterol Hepatol 23:1074–1077
Yamshchikov AV, Schuetz A, Lyon GM (2010) Rhodococcus equi infection. Lancet Infect Dis 10:350–359
Kedlaya I, Ing MB, Wong SS (2001) Rhodococcus equi infections in immunocompetent hosts: case report and review. Clin Infect Dis 32:E39–E46
Toyooka K, Takai S, Kirikae T (2005) Rhodococcus equi can survive a phagolysosomal environment in macrophages by suppressing acidification of the phagolysosome. J Med Microbiol 54:1007–1015
Zink MC, Yager JA, Prescott JF, Wilkie BN (1985) In vitro phagocytosis and killing of Corynebacterium equi by alveolar macrophages of foals. Am J Vet Res 46:2171–2174
Nordmann P, Ronco E, Guenounou M (1993) Involvement of interferon-gamma and tumor-necrosis-factor-alpha in host defense against Rhodococcus equi. J Infect Dis 167:1456–1459
Nordmann P, Ronco E, Nauciel C (1992) Role of T-lymphocyte subsets in Rhodococcus equi infection. Infect Immun 60:2748–2752
Kanaly ST, Hines SA, Palmer GH (1993) Failure of pulmonary clearance of Rhodococcus equi infection in Cd4+ T-lymphocyte-deficient transgenic mice. Infect Immun 61:4929–4932
Kinchen K, Kinchen TH, Inglesby T (1998) Pneumocystis carinii infections of the small intestine. J Nat Med Assoc 90:625–627
Dieterich DT, Lew EA, Bacon DJ, Pearlman KI, Scholes JV (1992) Gastrointestinal pneumocystosis in HIV-infected patients on aerosolized pentamidine—report of 5 cases and literature-review. Am J Gastroenterol 87:1763–1770
Raviglione MC (1990) Extrapulmonary pneumocystosis—the 1st 50 cases. Rev Infect Dis 12:1127–1138
Alvarez-Nebreda ML, Alvarez-Fernandez E, Rada S et al (2005) Unusual duodenal presentation of leishmaniasis. J Clin Pathol 58:1321–1322
Salah MBH, Mekni A, Khanfir M et al (2006) Unusual presentation of visceral leishmaniasis in an immunocompetent patient. Med Mal Infect 36:167–169
Burns JM, Shreffler WG, Benson DR, Ghalib HW, Badaro R, Reed SG (1993) Molecular characterization of a kinesin-related antigen of Leishmania chagasi that detects specific antibody in African and American visceral leishmaniasis. PNAS 90:775–779
Reithinger R, Dujardin JC (2007) Molecular diagnosis of leishmaniasis: current status and future applications. J Clin Microbiol 45:21–25
Chappuis F, Sundar S, Hailu A et al (2007) Visceral leishmaniasis: what are the needs for diagnosis, treatment and control? Nat Rev Microbiol 5:873–882
Goodwin RA, Shapiro JL, Thurman GH, Thurman SS, Desprez RM (1980) Disseminated histoplasmosis—clinical and pathologic correlations. Medicine 59:1–33
Haggerty CM, Britton MC, Dorman JM, Marzoni FA (1985) Gastrointestinal histoplasmosis in suspected acquired immunodeficiency syndrome. West J Med 143:244–246
Goodwin RA, Desprez RM (1978) Histoplasmosis. Am Rev Respir Dis 117:929–956
Wheat LJ, Connollystringfield PA, Baker RL et al (1990) Disseminated histoplasmosis in the acquired-immune-deficiency-syndrome—clinical findings, diagnosis and treatment, and review of the literature. Medicine 69:361–374
Suh KN, Anekthananon T, Mariuz PR (2001) Gastrointestinal histoplasmosis in patients with AIDS: case report and review. Clin Infect Dis 32:483–491
Kahi CJ, Wheat LJ, Allen SD, Sarosi GA (2005) Gastrointestinal histoplasmosis. Am J Gastroenterol 100:220–231
Wheat J, Sarosi G, McKinsey D et al (2000) Practice guidelines for the management of patients with histoplasmosis. Clin Infect Dis 30:688–695
Rabsch W, Tschape H, Baumler AJ (2001) Non-typhoidal salmonellosis: emerging problems. Microbes Infect 3:237–247
Reuser AJJ, Drost MR (2006) Lysosomal dysfunction, cellular pathology and clinical symptoms: basic principles. Acta Paediatr 95:77–82
Parkinson-Lawrence EJ, Shandala T, Prodoehl M, Plew R, Borlace GN, Brooks DA (2010) Lysosomal storage disease: revealing lysosomal function and physiology. Physiology 25:102–115
Settembre C, Fraldi A, Rubinsztein DC, Ballabio A (2008) Lysosomal storage diseases as disorders of autophagy. Autophagy 4:113–114
Grabowski GA (2008) Lysosomal storage disease 1—phenotype, diagnosis, and treatment of Gaucher's disease. Lancet 372:1263–1271
Harmanci O, Bayraktar Y (2008) Gaucher disease: new developments in treatment and etiology. World J Gastroenterol 14:3968–3973
Charrow J, Andersson HC, Kaplan P et al (2000) The Gaucher registry—demographics and disease characteristics of 1698 patients with Gaucher disease. Arch Intern Med 160:2835–2843
Lim AKP, Vellodi A, McHugh K (2002) Mesenteric mass in a young girl—an unusual site for Gaucher's disease. Pediatr Radiol 32:674–676
Jones DR, Hoffman J, Downie R, Haqqani M (1991) Massive gastrointestinal hemorrhage associated with ileal lymphoid hyperplasia in Gauchers-disease. Postgrad Med J 67:479–481
Henderson JM, Gilinsky NH, Lee EY, Greenwood MF (1991) Gauchers-disease complicated by bleeding esophageal-varices and colonic infiltration by Gaucher cells. Am J Gastroenterol 86:346–348
Zarate YA, Hopkin RJ (2008) Lysosomal storage disease 3—Fabry's disease. Lancet 372:1427–1435
Mehta A, Ricci R, Widmer U et al (2004) Fabry disease defined: baseline clinical manifestations of 366 patients in the Fabry outcome survey. Eur J Clin Investig 34:236–242
O'Brien B, Shnitka T, McDougall R et al (1982) Pathophysiologic and ultrastructural basis for intestinal symptoms in Fabry's disease. Gastroenterology 82:957–962
Tumer L, Ezgu FS, Hasanoglu A et al (2004) The co-existence of Fabry and celiac diseases: a case report. Pediatr Nephrol 19:679–681
Kolodny EH (2000) Niemann–Pick disease. Curr Opin Hematol 7:48–52
Ory DS (2004) The Niemann–Pick disease genes—regulators of cellular cholesterol homeostasis. Trends Cardiovasc Med 14:66–72
Schuchman EH (2007) The pathogenesis and treatment of acid sphingomyelinase-deficient Niemann–Pick disease. J Inherit Metabol Dis 30:654–663
Horinouchi K, Erlich S, Perl DP et al (1995) Acid sphingomyelinase deficient mice—a model of type-A and type-B Niemann–Pick disease. Nat Genet 10:288–293
Galvis D, Nakazato Y, Wells T, Landing B (1987) Demonstration of myenteric plexus abnormalities in genetic diseases by a microdissection technique: preliminary studies. Am J Med Gen 3:329–342
Candoni A, Grimaz S, Doretto P, Fanin R, Falcomer F, Bembi B (2001) Sea-blue histiocytosis secondary to Niemann–Pick disease type B: a case report. Ann Hematol 80:620–622
van der Ploeg AT, Reuser AJJ (2008) Lysosomal storage disease 2—Pompe's disease. Lancet 372:1342–1353
Nofer JR, Remaley AT (2005) Tangier disease: still more questions than answers. Cell Mol Life Sci 62:2150–2160
Bale PM, Clifton-Bligh P, Benjamin BN, Whyte HM (1971) Pathology of Tangier disease. J Clin Pathol 24:609–616
Hoeg JM, Demosky SJ, Pescovitz OH, Brewer HB (1984) Cholesteryl ester storage disease and wolman disease—phenotypic variants of lysosomal acid cholesteryl ester hydrolase deficiency. Am J Hum Gen 36:1190–1203
Lambert I, Fransis S, Ectors N, Desreumaux P, Geboes K (2003) Macrophage collections in gastrointestinal biopsies and metabolic disorders: two unusual case reports. Histopathology 42:196–198
Boldrini R, Devito R, Biselli R, Filocamo M, Bosman C (2004) Wolman disease and cholesteryl ester storage disease diagnosed by histological and ultrastructural examination of intestinal and liver biopsy. Pathol Res Pract 200:231–240
Gahl WA, Thoene JG, Schneider JA (2002) Cystinosis. N Engl J Med 347:111–121
Dohil R, Newbury RO, Sellers ZM, Deutsch R, Schneider JA (2003) The evaluation and treatment of gastrointestinal disease in children with cystinosis receiving cysteamine. J Pediatr 143:224–230
Anderson CA, Massey DCO, Barrett JC et al (2009) Investigation of Crohn's disease risk loci in ulcerative colitis further defines their molecular relationship. Gastroenterology 136:523–529
Van Limbergen J, Wilson DC, Satsangi J (2009) The genetics of Crohn's disease. Annu Rev Genom Hum Genet 10:89–116
Xavier RJ, Podolsky DK (2007) Unravelling the pathogenesis of inflammatory bowel disease. Nature 448:427–434
Marks DJB, Harbord MWN, MacAllister R et al (2006) Defective acute inflammation in Crohn's disease: a clinical investigation. Lancet 367:668–678
Campos N, Magro F, Castro AR et al (2011) Macrophages from IBD patients exhibit defective tumour necrosis factor-alpha secretion but otherwise normal or augmented pro-inflammatory responses to infection. Immunobiology 216:961–970
Smith AM, Rahman FZ, Hayee B et al (2009) Disordered macrophage cytokine secretion underlies impaired acute inflammation and bacterial clearance in Crohn's disease. J Exp Med 206:1883–1897
Yousef GM, Naghibi B (2007) Malakoplakia outside the urinary tract—reply. Arch Pathol Lab Med 131:1512–1513
Boudny P, Kurrer MO, Stamm B, Laeng RH (2000) Malakoplakia of the colon in an infant with severe combined immunodeficiency (SCID) and CHARGE association. Pathol Res Pract 196:577–582
Jain M, Arora VK, Singh N, Bhatia A (2000) Malakoplakia of the appendix—an unusual association with eggs of Taenia species. Arch Pathol Lab Med 124:1828–1829
Guinaudeau E, Person B, Valo I, Tuech JJ, Rousselet MC (2002) Colonic malakoplakia and ulcerative colitis: report of a case. Gastroenterol Clin Biol 26:174–177
Kim PTW, Davis JE, Erb SR, Yoshida EM, Steinbrecher UP (2007) Colonic malakoplakia in a liver transplant recipient. Can J Gastroenterol 21:753–755
Cachia AR, Eshoo S, Kench J et al (2005) Synchronous malakoplakia and Whipple's disease. Pathology 37:315–317
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sagaert, X., Tousseyn, T., De Hertogh, G. et al. Macrophage-related diseases of the gut: a pathologist's perspective. Virchows Arch 460, 555–567 (2012). https://doi.org/10.1007/s00428-012-1244-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-012-1244-9