Abstract
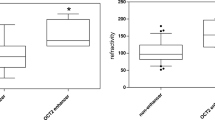
Several organic cations, such as guanidino compounds and polyamines, have been found to accumulate in plasma of patients with kidney failure due to inadequate renal clearance. Here, we studied the interaction of cationic uremic toxins with renal organic cation transport in a conditionally immortalized human proximal tubule epithelial cell line (ciPTEC). Transporter activity was measured and validated in cell suspensions by studying uptake of the fluorescent substrate 4-(4-(dimethylamino)styryl)-N-methylpyridinium-iodide (ASP+). Subsequently, the inhibitory potencies of the cationic uremic toxins, cadaverine, putrescine, spermine and spermidine (polyamines), acrolein (polyamine breakdown product), guanidine, and methylguanidine (guanidino compounds) were determined. Concentration-dependent inhibition of ASP+ uptake by TPA, cimetidine, quinidine, and metformin confirmed functional endogenous organic cation transporter 2 (OCT2) expression in ciPTEC. All uremic toxins tested inhibited ASP+ uptake, of which acrolein required the lowest concentration to provoke a half-maximal inhibition (IC50 = 44 ± 2 μM). A Dixon plot was constructed for acrolein using three independent inhibition curves with 10, 20, or 30 μM ASP+, which demonstrated competitive or mixed type of interaction (K i = 93 ± 16 μM). Exposing the cells to a mixture of cationic uremic toxins resulted in a more potent and biphasic inhibitory response curve, indicating complex interactions between the toxins and ASP+ uptake. In conclusion, ciPTEC proves a suitable model to study cationic xenobiotic interactions. Inhibition of cellular uptake transport was demonstrated for several uremic toxins, which might indicate a possible role in kidney disease progression during uremia.








Similar content being viewed by others
Abbreviations
- ASP+ :
-
4-(4-(Dimethylamino)styryl)-N-methylpyridinium-iodide
- ciPTEC:
-
Conditionally immortalized proximal tubule epithelial cells
- CKD:
-
Chronic kidney disease
- DMEM:
-
Dulbecco's modified eagle medium
- ESRD:
-
End-stage renal disease
- FCS:
-
Fetal calf serum
- IC50 :
-
Half-maximal inhibitory concentration
- MATE:
-
Multidrug and toxic compound extrusion protein
- MTT:
-
(3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide
- OCT:
-
Organic cation transporter
- RLU:
-
Relative light units
- TPA:
-
Tetrapentylammonium
References
Ahlin G, Hilgendorf C, Karlsson J, Szigyarto CA, Uhlen M, Artursson P (2009) Endogenous gene and protein expression of drug-transporting proteins in cell lines routinely used in drug discovery programs. Drug Metab Dispos 37:2275–2283. doi:10.1124/dmd.109.028654
Astorga B, Ekins S, Morales M, Wright SH (2012) Molecular determinants of ligand selectivity for the human multidrug and toxin extruder proteins mate1 and mate2-k. J Pharmacol Exp Ther 341:743–755. doi:10.1124/jpet.112.191577
Ciarimboli G, Ludwig T, Lang D, Pavenstadt H, Koepsell H, Piechota HJ, Haier J, Jaehde U, Zisowsky J, Schlatter E (2005) Cisplatin nephrotoxicity is critically mediated via the human organic cation transporter 2. Am J Pathol 167:1477–1484. doi:10.1016/S0002-9440(10)61234-5
D'Hooge R, De Deyn PP, Van de Vijver G, Antoons G, Raes A, Van Bogaert PP (1999) Uraemic guanidino compounds inhibit gamma-aminobutyric acid-evoked whole cell currents in mouse spinal cord neurones. Neurosci Lett 265:83–86. doi:10.1016/S0304-3940(99)00190-1
De Deyn PP, Robitaille P, Vanasse M, Qureshi IA, Marescau B (1995) Serum guanidino compound levels in uremic pediatric patients treated with hemodialysis or continuous cycle peritoneal dialysis. Correlations between nerve conduction velocities and altered guanidino compound concentrations. Nephrol 69:411–417. doi:10.1159/000188511
Dhondt A, Vanholder R, Van Biesen W, Lameire N (2000) The removal of uremic toxins. Kidney Int Suppl 76:S47–S59. doi:10.1046/j.1523-1755.2000.07606.x
Duranton F, Cohen G, De Smet R, Rodriguez M, Jankowski J, Vanholder R, Argiles A (2012) Normal and pathologic concentrations of uremic toxins. J Am Soc Nephrol 23:1258–1270. doi:10.1681/ASN.2011121175
Eloot S, van Biesen W, Dhondt A, de Smet R, Marescau B, De Deyn PP, Verdonck P, Vanholder R (2009) Impact of increasing haemodialysis frequency versus haemodialysis duration on removal of urea and guanidino compounds: a kinetic analysis. Nephrol Dial Transplant 24:2225–2232. doi:10.1093/ndt/gfp059
Fujita T, Urban TJ, Leabman MK, Fujita K, Giacomini KM (2006) Transport of drugs in the kidney by the human organic cation transporter, oct2 and its genetic variants. J Pharm Sci 95:25–36. doi:10.1002/jps.20536
Giovannetti S, Cioni L, Balestri PL, Biagnini M (1968) Evidence that guanidines and some related compounds cause haemolysis in chronic uraemia. Clin Sci 34:141–148http://www.ncbi.nlm.nih.gov/pubmed/5640680
Glorieux GL, Dhondt AW, Jacobs P, Van Langeraert J, Lameire NH, De Deyn PP, Vanholder RC (2004) In vitro study of the potential role of guanidines in leukocyte functions related to atherogenesis and infection. Kidney Int 65:2184–2192. doi:10.1111/j.1523-1755.2004.00631.x
Gorboulev V, Ulzheimer JC, Akhoundova A, Ulzheimer-Teuber I, Karbach U, Quester S, Baumann C, Lang F, Busch AE, Koepsell H (1997) Cloning and characterization of two human polyspecific organic cation transporters. DNA Cell Biol 16:871–881. doi:10.1089/dna.1997.16.871
Hosoya K, Tachikawa M (2011) Roles of organic anion/cation transporters at the blood–brain and blood–cerebrospinal fluid barriers involving uremic toxins. Clin Exp Nephrol 15:478–485. doi:10.1007/s10157-011-0460-y
Igarashi K, Kashiwagi K (2010) Modulation of cellular function by polyamines. Int J Biochem Cell Biol 42:39–51. doi:10.1016/j.biocel.2009.07.009
Igarashi K, Ueda S, Yoshida K, Kashiwagi K (2006) Polyamines in renal failure. Amino Acids 31:477–483. doi:10.1007/s00726-006-0264-7
Jenkinson SE, Chung GW, van Loon E, Bakar NS, Dalzell AM, Brown CD (2012) The limitations of renal epithelial cell line hk-2 as a model of drug transporter expression and function in the proximal tubule. Pflugers Arch 464:601–611. doi:10.1007/s00424-012-1163-2
Kimura N, Masuda S, Katsura T, Inui K (2009) Transport of guanidine compounds by human organic cation transporters, hoct1 and hoct2. Biochem Pharmacol 77:1429–1436. doi:10.1016/j.bcp.2009.01.010
Kimura N, Okuda M, Inui K (2005) Metformin transport by renal basolateral organic cation transporter hoct2. Pharm Res 22:255–259. doi:10.1007/s11095-004-1193-3
Krieter DH, Hackl A, Rodriguez A, Chenine L, Moragues HL, Lemke HD, Wanner C, Canaud B (2010) Protein-bound uraemic toxin removal in haemodialysis and post-dilution haemodiafiltration. Nephrol Dial Transplant 25:212–218. doi:10.1093/ndt/gfp437
Kushner D, Beckman B, Nguyen L, Chen S, Della Santina C, Husserl F, Rice J, Fisher JW (1991) Polyamines in the anemia of end-stage renal disease. Kidney Int 39:725–732. doi:10.1038/ki.1991.88
Lumen AA, Acharya P, Polli JW, Ayrton A, Ellens H, Bentz J (2010) If the KI is defined by the free energy of binding to P-glycoprotein, which kinetic parameters define the IC50 for the Madin–Darby canine kidney II cell line overexpressing human multidrug resistance 1 confluent cell monolayer? Drug Metab Dispos 38:260–269. doi:10.1124/dmd.109.029843
MacAllister RJ, Whitley GS, Vallance P (1994) Effects of guanidino and uremic compounds on nitric oxide pathways. Kidney Int 45:737–742. doi:10.1038/ki.1994.98
Meyer TW, Hostetter TH (2007) Uremia. N Engl J Med 357:1316–1325. doi:10.1056/NEJMra071313
Meyer TW, Walther JL, Pagtalunan ME, Martinez AW, Torkamani A, Fong PD, Recht NS, Robertson CR, Hostetter TH (2005) The clearance of protein-bound solutes by hemofiltration and hemodiafiltration. Kidney Int 68:867–877. doi:10.1111/j.1523-1755.2005.00469.x
Momper JD, Venkataramanan R, Nolin TD (2010) Nonrenal drug clearance in CKD: searching for the path less traveled. Adv Chronic Kidney Dis 17:384–391. doi:10.1053/j.ackd.2010.05.009
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65:55–63http://www.ncbi.nlm.nih.gov/pubmed/6606682
Motohashi H, Uwai Y, Hiramoto K, Okuda M, Inui K (2004) Different transport properties between famotidine and cimetidine by human renal organic ion transporters (slc22a). Eur J Pharmacol 503:25–30. doi:10.1016/j.ejphar.2004.09.032
Nies AT, Koepsell H, Damme K, Schwab M (2011) Organic cation transporters (OCTs, MATEs), in vitro and in vivo evidence for the importance in drug therapy. Handb Exp Pharmacol:105–167. doi:10.1007/978-3-642-14541-4_3
Niwa T (2010) Uremic toxicity of indoxyl sulfate. Nagoya J Med Sci 72:1–11. doi:10.1159/000057433
Nolin TD (2008) Altered nonrenal drug clearance in ESRD. Curr Opin Nephrol Hypertens 17:555–559. doi:10.1097/MNH.0b013e3283136732
Radtke HW, Rege AB, LaMarche MB, Bartos D, Bartos F, Campbell RA, Fisher JW (1981) Identification of spermine as an inhibitor of erythropoiesis in patients with chronic renal failure. J Clin Invest 67:1623–1629. doi:10.1172/JCI110197
Reidenberg MM, Drayer DE (1984) Alteration of drug–protein binding in renal disease. Clin Pharmacokinet 9(Suppl 1):18–26. doi:10.2165/00003088-198400091-00003
Rowland Yeo K, Aarabi M, Jamei M, Rostami-Hodjegan A (2011) Modeling and predicting drug pharmacokinetics in patients with renal impairment. Expert Rev Clin Pharmacol 4:261–274. doi:10.1586/ecp.10.143
Sakata K, Kashiwagi K, Sharmin S, Ueda S, Igarashi K (2003) Acrolein produced from polyamines as one of the uraemic toxins. Biochem Soc Trans 31:371–374. doi:10.1042/BST0310371
Sakata K, Kashiwagi K, Sharmin S, Ueda S, Irie Y, Murotani N, Igarashi K (2003) Increase in putrescine, amine oxidase, and acrolein in plasma of renal failure patients. Biochem Biophys Res Commun 305:143–149. doi:10.1016/S0006-291x(03)00716-2
Schlatter E, Monnich V, Cetinkaya I, Mehrens T, Ciarimboli G, Hirsch JR, Popp C, Koepsell H (2002) The organic cation transporters rOCT1 and hOCT2 are inhibited by cGMP. J Membr Biol 189:237–244. doi:10.1007/s00232-002-1023-7
Sharmin S, Sakata K, Kashiwagi K, Ueda S, Iwasaki S, Shirahata A, Igarashi K (2001) Polyamine cytotoxicity in the presence of bovine serum amine oxidase. Biochem Biophys Res Commun 282:228–235. doi:10.1006/bbrc.2001.4569
Stabellini G, Mariani G, Pezzetti F, Calastrini C (1997) Direct inhibitory effect of uremic toxins and polyamines on proliferation of VERO culture cells. Exp Mol Pathol 64:147–155. doi:10.1006/exmp.1997.2215
Sun H, Frassetto L, Benet LZ (2006) Effects of renal failure on drug transport and metabolism. Pharmacol Ther 109:1–11. doi:10.1016/j.pharmthera.2005.05.010
Tadolini B, Hakim G, Orlandini G, Casti A (1986) Intracellular location of polyamines associated to red blood cells. Biochem Biophys Res Commun 134:1365–1371. doi:10.1016/0006-291X(86)90400-6
Takagi T, Chung TG, Saito A (1983) Determination of polyamines in hydrolysates of uremic plasma by high-performance cation-exchange column chromatography. J Chromatogr 272:279–285, <Go to ISI>://A1983QE07100007
Vanholder R, De Smet R (1999) Pathophysiologic effects of uremic retention solutes. J Am Soc Nephrol 10:1815–1823
Vanholder R, Van Landschoot N, De Smet R, Schoots A, Ringoir S (1988) Drug protein binding in chronic renal failure: evaluation of nine drugs. Kidney Int 33:996–1004. doi:10.1038/ki.1988.99
Volk C, Gorboulev V, Budiman T, Nagel G, Koepsell H (2003) Different affinities of inhibitors to the outwardly and inwardly directed substrate binding site of organic cation transporter 2. Mol Pharmacol 64:1037–1047. doi:10.1124/mol.64.5.1037
Wilde S, Schlatter E, Koepsell H, Edemir B, Reuter S, Pavenstadt H, Neugebauer U, Schroter R, Brast S, Ciarimboli G (2009) Calmodulin-associated post-translational regulation of rat organic cation transporter 2 in the kidney is gender dependent. Cell Mol Life Sci 66:1729–1740. doi:10.1007/s00018-009-9145-z
Wilmer MJ, Saleem MA, Masereeuw R, Ni L, van der Velden TJ, Russel FG, Mathieson PW, Monnens LA, van den Heuvel LP, Levtchenko EN (2010) Novel conditionally immortalized human proximal tubule cell line expressing functional influx and efflux transporters. Cell Tissue Res 339:449–457. doi:10.1007/s00441-009-0882-y
Winter TN, Elmquist WF, Fairbanks CA (2011) Oct2 and mate1 provide bidirectional agmatine transport. Mol Pharm 8:133–142. doi:10.1021/mp100180a
Zolk O, Solbach TF, Konig J, Fromm MF (2009) Structural determinants of inhibitor interaction with the human organic cation transporter oct2 (slc22a2). Naunyn Schmiedebergs Arch Pharmacol 379:337–348. doi:10.1007/s00210-008-0369-5
Acknowledgment
This work was supported by the BioMedical Materials Institute (BMM, Project P3.01 BioKid); the Dutch Ministry of Economic Affairs, Agriculture and Innovation; the Nierstichting Nederland; and the Netherlands Institute for Regenerative Medicine (NIRM, grant no. FES0908). M.J.G. Wilmer and R. Masereeuw were supported by a collaboration research grant from AstraZeneca (grant no. A10-0324). J. Hoenderop was supported by an EURYI award.
Ethical standards
The experiments described in this article comply with the current laws of the country in which they were performed (the Netherlands).
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
The manuscript was written through contributions of all authors. All authors have given approval to the final version of the manuscript.
Carolien M.S. Schophuizen, Martijn J. Wilmer, Lambert P. van den Heuvel, and Rosalinde Masereeuw contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Fig9
Online Resource 1 OCT-mediated ASP+ uptake by mature ciPTEC analyzed by measuring the fluorescence of transported ASP+ in the absence (white bar) or presence (gray bar) of OCT2 inhibitor tetrapentylammonium (TPA). Additionally, uptake was performed at 4 °C (black bar). Uptake was significantly decreased in ciPTEC in the presence of TPA or at 4 °C (**P < 0.001). Results are shown as mean values ± SEM of three experiments (GIF 7 kb)
Fig10
Online Resource 2 Time dependence of ASP+ uptake. OCT-mediated ASP+ uptake by ciPTEC analyzed by measuring the fluorescence of transported ASP+ for 60 min. Uptake was found to be linear for at least 60 min. Results are shown as mean values ± SEM of three experiments (GIF 10 kb)
Rights and permissions
About this article
Cite this article
Schophuizen, C.M.S., Wilmer, M.J., Jansen, J. et al. Cationic uremic toxins affect human renal proximal tubule cell functioning through interaction with the organic cation transporter. Pflugers Arch - Eur J Physiol 465, 1701–1714 (2013). https://doi.org/10.1007/s00424-013-1307-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-013-1307-z