Abstract
Background
Recently, indocyanine green (ICG) fluorescence imaging has been increasingly used in laparoscopic anatomic liver resection. The aim of this study was to investigate the efficacy of ICG-guided laparoscopic anatomic liver resection in hepatocellular carcinoma (HCC) compared with traditional laparoscopic anatomic liver resection.
Methods
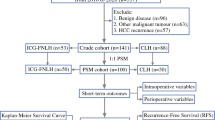
A retrospective study was performed on patients with pathologically diagnosed HCC who successfully underwent laparoscopic anatomical liver resection from January 2019 to December 2021. The outcomes were compared between the two groups before and after the propensity score matching (PSM).
Results
A total of 110 patients were included in this study, including 50 patients in the ICG-guided group and 60 patients in the traditional group. Compared with the traditional group, the ICG-guided group had a shorter operative duration (P = 0.040), less intraoperative blood loss (P = 0.044), a lower incidence of postoperative complications (P = 0.023), and a shorter postoperative hospitalisation (P < 0.001). After PSM, significant differences remained between the two groups for the duration of postoperative hospitalisation (P = 0.018) and postoperative complications (P = 0.042). There was no significant difference in the recurrence rate between the two groups before and after PSM.
Conclusion
Laparoscopic anatomic liver resection guided by ICG fluorescence imaging can reduce the duration of postoperative hospitalisation for patients and the incidence of postoperative complications. However, it has no impact on the long-term outcome of patients.



Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author, [JinLiang Ma], upon reasonable request.
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424
Makuuchi M, Takayama T, Kosuge T et al (1991) The value of ultrasonography for hepatic surgery. Hepatogastroenterology 38(1):64–70
Koffron AJ, Auffenberg G, Kung R, Abecassis M (2007) Evaluation of 300 minimally invasive liver resections at a single institution: less is more. Ann Surg. 246(3):385–392 (discussion 392-384)
Ishizawa T, Gumbs AA, Kokudo N, Gayet B (2012) Laparoscopic segmentectomy of the liver: from segment I to VIII. Ann Surg 256(6):959–964
Berardi G, Wakabayashi G, Igarashi K et al (2019) Full laparoscopic anatomical segment 8 resection for hepatocellular carcinoma using the Glissonian approach with indocyanine green dye fluorescence. Ann Surg Oncol 26(8):2577–2578
Nomi T, Hokuto D, Yoshikawa T, Matsuo Y, Sho M (2018) A novel navigation for laparoscopic anatomic liver resection using indocyanine green fluorescence. Ann Surg Oncol 25(13):3982
He JM, Zhen ZP, Ye Q, Mo JQ, Chen GH, Peng JX (2020) Laparoscopic anatomical segment VII resection for hepatocellular carcinoma using the glissonian approach with indocyanine green dye fluorescence. J Gastrointest Surg 24(5):1228–1229
Ishizawa T, Masuda K, Urano Y et al (2014) Mechanistic background and clinical applications of indocyanine green fluorescence imaging of hepatocellular carcinoma. Ann Surg Oncol 21(2):440–448
Inoue Y, Arita J, Sakamoto T et al (2015) Anatomical liver resections guided by 3-dimensional parenchymal staining using fusion indocyanine green fluorescence imaging. Ann Surg 262(1):105–111
Shindoh J, Mise Y, Satou S, Sugawara Y, Kokudo N (2010) The intersegmental plane of the liver is not always flat—tricks for anatomical liver resection. Ann Surg 251(5):917–922
Chana P, Burns EM, Arora S, Darzi AW, Faiz OD (2016) A systematic review of the impact of dedicated emergency surgical services on patient outcomes. Ann Surg 263(1):20–27
Xu Y, Chen M, Meng X et al (2020) Laparoscopic anatomical liver resection guided by real-time indocyanine green fluorescence imaging: experience and lessons learned from the initial series in a single center. Surg Endosc 34(10):4683–4691
Kawaguchi Y, Fuks D, Kokudo N, Gayet B (2018) Difficulty of laparoscopic liver resection: proposal for a new classification. Ann Surg 267(1):13–17
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196
Yao S, Zhang L, Ma J, Jia W, Chen H (2020) Precise right hemihepatectomy for the treatment of hepatocellular carcinoma guided by fusion ICG fluorescence imaging. J Cancer 11(9):2465–2475
Aoki T, Koizumi T, Mansour DA et al (2020) Ultrasound-guided preoperative positive percutaneous indocyanine green fluorescence staining for laparoscopic anatomical liver resection. J Am Coll Surg 230(3):e7–e12
Liu Y, Wang Q, Du B, Wang XZ, Xue Q, Gao WF (2021) Meta-analysis of indocyanine green fluorescence imaging-guided laparoscopic hepatectomy. Photodiagn Photodyn Ther 35:102354
Purich K, Dang JT, Poonja A et al (2020) Intraoperative fluorescence imaging with indocyanine green in hepatic resection for malignancy: a systematic review and meta-analysis of diagnostic test accuracy studies. Surg Endosc 34(7):2891–2903
Li J, Li X, Zhang X et al (2022) Indocyanine green fluorescence imaging-guided laparoscopic right posterior hepatectomy. Surg Endosc 36(2):1293–1301
Berardi G, Colasanti M, Meniconi RL et al (2021) The applications of 3D imaging and indocyanine green dye fluorescence in laparoscopic liver surgery. Diagnostics (Basel) 11(12):2169
Wang X, Teh CSC, Ishizawa T et al (2021) Consensus guidelines for the use of fluorescence imaging in hepatobiliary surgery. Ann Surg 274(1):97–106
Liang X, Zheng J, Xu J et al (2021) Laparoscopic anatomical portal territory hepatectomy using Glissonean pedicle approach (Takasaki approach) with indocyanine green fluorescence negative staining: how I do it. HPB (Oxford) 23(9):1392–1399
Ishizawa T, Zuker NB, Kokudo N, Gayet B (2012) Positive and negative staining of hepatic segments by use of fluorescent imaging techniques during laparoscopic hepatectomy. Arch Surg 147(4):393–394
Araki K, Conrad C, Ogiso S, Kuwano H, Gayet B (2014) Intraoperative ultrasonography of laparoscopic hepatectomy: key technique for safe liver transection. J Am Coll Surg 218(2):e37-41
Acknowledgements
We would like to acknowledge AJE Digital Editing for its linguistic assistance during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Study conception and design: Yi Zhou, Chuanhai Zhang, Yifan Wang, Jihai Yu, Di Wang, and Jinliang Ma. Analysis and interpretation of data: Yi Zhou, Chuanhai Zhang, Yifan Wang, and Jinliang Ma. Drafting of manuscript: Yi Zhou. Critical revision of manuscript: Yi Zhou, Chuanhai Zhang, Yifan Wang, Jihai Yu, Di Wang, and Jinliang Ma. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All of the experimental procedures were performed under a project license (No.: 2022-RE-008) granted by the institutional ethics board of The First Affiliated Hospital of USTC (Hefei, China).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhou, Y., Zhang, C., Wang, Y. et al. Effects of indocyanine green fluorescence imaging of laparoscopic anatomic liver resection for HCC: a propensity score-matched study. Langenbecks Arch Surg 408, 51 (2023). https://doi.org/10.1007/s00423-023-02781-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-02781-z