Abstract
Purpose
Postoperative pancreatic fistula (POPF) is a major determinant of pancreatic surgery outcome, and prevention of POPF is a relevant clinical challenge. The aim of the present study is to compare the cost-effectiveness of octreotide and pasireotide for POPF prophylaxis.
Methods
A systematic literature review and meta-analysis and a retrospective patient cohort provided the data. Cost-effectiveness was calculated by the incremental cost-effectiveness ratio (ICER) and by decision tree modelling of hospital stay duration.
Results
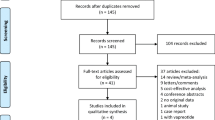
Six randomised trials on octreotide (1255 patients) and one trial on pasireotide (300 patients) were included. The median POPF incidence without prophylaxis was 19.6 %. The relative risks for POPF after octreotide or pasireotide prophylaxis were 0.54 or 0.45. Octreotide prophylaxis (21 × 0.1 mg) costs were 249.69 Euro, compared with 728.84 Euro for pasireotide (14 × 0.9 mg) resulting in an ICER of 266.19 Euro for an additional 1.8 % risk reduction with pasireotide. Decision tree modelling revealed no significant reduction of median hospital stay duration if pasireotide was used instead of octreotide.
Conclusion
Prophylactic octreotide is almost as effective as pasireotide but incurs significantly fewer drug costs per case. However, the data quality is limited, because the effect of octreotide on clinically relevant POPF is unclear. Together with the lack of multicentric data on pasireotide and its effectiveness, a current off-label use of pasireotide does not appear to be justified.


Similar content being viewed by others
References
Hartwig W, Hackert T, Hinz U, Gluth A, Bergmann F et al (2011) Pancreatic cancer surgery in the new millennium: better prediction of outcome. Ann Surg 254:311–319
Winter JM, Cameron JL, Campbell KA, Arnold MA, Chang DC et al (2006) 1423 pancreaticoduodenectomies for pancreatic cancer: a single-institution experience. J Gastrointest Surg 10:1199–1210, discussion 1210–1
Wente MN, Veit JA, Bassi C, Dervenis C, Fingerhut A et al (2007) Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery 142:20–25
Yekebas EF, Wolfram L, Cataldegirmen G, Habermann CR, Bogoevski D et al (2007) Postpancreatectomy hemorrhage: diagnosis and treatment: an analysis in 1669 consecutive pancreatic resections. Ann Surg 246:269–280
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C et al (2005) Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138:8–13
Harnoss JC, Ulrich AB, Harnoss JM, Diener MK, Büchler MW, Welsch T (2014) Use and results of consensus definitions in pancreatic surgery: a systematic review. Surgery 155:47–57
Malleo G, Pulvirenti A, Marchegiani G, Butturini G, Salvia R, Bassi C (2014) Diagnosis and management of postoperative pancreatic fistula. Langenbeck’s Arch Surg 399:801–810
Pratt WB, Maithel SK, Vanounou T, Huang ZS, Callery MP, Vollmer CM (2007) Clinical and economic validation of the International Study Group of Pancreatic Fistula (ISGPF) classification scheme. Ann Surg 245:443–451
Denbo JW, Orr WS, Zarzaur BL, Behrman SW (2012) Toward defining grade C pancreatic fistula following pancreaticoduodenectomy: incidence, risk factors, management and outcome. HPB (Oxford) 14:589–593
Gurusamy KS, Koti R, Fusai G, Davidson BR (2013) Somatostatin analogues for pancreatic surgery. Cochrane Database Syst Rev 4, CD008370
Haane C, Mardin WA, Schmitz B, Dhayat S, Hummel R et al (2013) Pancreatoduodenectomy—current status of surgical and perioperative techniques in Germany. Langenbeck’s Arch Surg 398:1097–1105
Allen PJ, Gönen M, Brennan MF, Bucknor AA, Robinson LM et al (2014) Pasireotide for postoperative pancreatic fistula. N Engl J Med 370:2014–2022
Gurusamy KS, Gluud C, Nikolova D, Davidson BR (2009) Assessment of risk of bias in randomized clinical trials in surgery. Br J Surg 96:342–349
Alghamdi AA, Jawas AM, Hart RS (2007) Use of octreotide for the prevention of pancreatic fistula after elective pancreatic surgery: a systematic review and meta-analysis. Can J Surg 50:459–466
Koti RS, Gurusamy KS, Fusai G, Davidson BR (2010) Meta-analysis of randomized controlled trials on the effectiveness of somatostatin analogues for pancreatic surgery: a Cochrane review. HPB (Oxford) 12:155–165
Li-Ling J, Irving M (2001) Somatostatin and octreotide in the prevention of postoperative pancreatic complications and the treatment of enterocutaneous pancreatic fistulas: a systematic review of randomized controlled trials. Br J Surg 88:190–199
Zeng Q, Zhang Q, Han S, Yu Z, Zheng M et al (2008) Efficacy of somatostatin and its analogues in prevention of postoperative complications after pancreaticoduodenectomy: a meta-analysis of randomized controlled trials. Pancreas 36:18–25
Büchler M, Friess H, Klempa I, Hermanek P, Sulkowski U et al (1992) Role of octreotide in the prevention of postoperative complications following pancreatic resection. Am J Surg 163:125–130, discussion 130–1
Fernández-Cruz L, Jiménez Chavarría E, Taurà P, Closa D, Boado MA, Ferrer J (2013) Prospective randomized trial of the effect of octreotide on pancreatic juice output after pancreaticoduodenectomy in relation to histological diagnosis, duct size and leakage. HPB (Oxford) 15:392–399
Friess H, Beger HG, Sulkowski U, Becker H, Hofbauer B et al (1995) Randomized controlled multicentre study of the prevention of complications by octreotide in patients undergoing surgery for chronic pancreatitis. Br J Surg 82:1270–1273
Montorsi M, Zago M, Mosca F, Capussotti L, Zotti E et al (1995) Efficacy of octreotide in the prevention of pancreatic fistula after elective pancreatic resections: a prospective, controlled, randomized clinical trial. Surgery 117:26–31
Pederzoli P, Bassi C, Falconi M, Camboni MG (1994) Efficacy of octreotide in the prevention of complications of elective pancreatic surgery. Italian Study Group. Br J Surg 81:265–269
Suc B, Msika S, Piccinini M, Fourtanier G, Hay JM et al (2004) Octreotide in the prevention of intra-abdominal complications following elective pancreatic resection: a prospective, multicenter randomized controlled trial. Arch Surg 139:288–294, discussion 295
Keck T, Wellner UF, Bahra M, Klein F, Sick O et al (2015) Pancreatogastrostomy Versus Pancreatojejunostomy for RECOnstruction After PANCreatoduodenectomy (RECOPANC, DRKS 00000767): perioperative and long-term results of a multicenter randomized controlled trial. Ann Surg 263:440–449
Gudjonsson B (1995) Carcinoma of the pancreas: critical analysis of costs, results of resections, and the need for standardized reporting. J Am Coll Surg 181:483–503
Ljungman D, Lundholm K, Hyltander A (2011) Cost-utility estimation of surgical treatment of pancreatic carcinoma aimed at cure. World J Surg 35:662–670
Morris S, Gurusamy KS, Sheringham J, Davidson BR (2015) Cost-effectiveness of preoperative biliary drainage for obstructive jaundice in pancreatic and periampullary cancer. J Surg Res 193:202–209
Morris S, Gurusamy KS, Sheringham J, Davidson BR (2015) Cost-effectiveness of diagnostic laparoscopy for assessing resectability in pancreatic and periampullary cancer. BMC Gastroenterol 15:44
Rosenberg L, MacNeil P, Turcotte L (1999) Economic evaluation of the use of octreotide for prevention of complications following pancreatic resection. J Gastrointest Surg 3:225–232
Lowy AM, Lee JE, Pisters PW, Davidson BS, Fenoglio CJ et al (1997) Prospective, randomized trial of octreotide to prevent pancreatic fistula after pancreaticoduodenectomy for malignant disease. Ann Surg 226:632–641
Yeo CJ, Cameron JL, Lillemoe KD, Sauter PK, Coleman J et al (2000) Does prophylactic octreotide decrease the rates of pancreatic fistula and other complications after pancreaticoduodenectomy? Results of a prospective randomized placebo-controlled trial. Ann Surg 232:419–429
Daskalaki D, Butturini G, Molinari E, Crippa S, Pederzoli P, Bassi C (2011) A grading system can predict clinical and economic outcomes of pancreatic fistula after pancreaticoduodenectomy: results in 755 consecutive patients. Langenbeck’s Arch Surg 396:91–98
Abbott DE, Sutton JM, Jernigan PL, Chang A, Frye P et al (2016) Prophylactic pasireotide administration following pancreatic resection reduces cost while improving outcomes. J Surg Oncol in press
Belyaev O, Herzog T, Chromik AM, Meurer K, Uhl W (2013) Early and late postoperative changes in the quality of life after pancreatic surgery. Langenbeck’s Arch Surg 398:547–555
Author contributions
T.W. designed the study, performed the analysis and drafted the manuscript. B.M. and M.D. contributed to the analysis and data collection. H.K. provided data and reviewed the manuscript. J.W. helped to set up the study and reviewed the manuscript. D.H. designed the study and reviewed the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
There was no third-party funding of the present project.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Informed consent was not obtained by all included participants, since it was a retrospective study with anonymised individuals, and many of the individuals were deceased by the time of analysis. The present study was approved by the local ethical committee of the TU Dresden (decision no. 247062015) as stated in the “Methods” section.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 1161 kb)
Rights and permissions
About this article
Cite this article
Welsch, T., Müssle, B., Distler, M. et al. Cost-effectiveness comparison of prophylactic octreotide and pasireotide for prevention of fistula after pancreatic surgery. Langenbecks Arch Surg 401, 1027–1035 (2016). https://doi.org/10.1007/s00423-016-1456-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-016-1456-6