Abstract
Introduction
Between 40 and 50 % of the population will have at least one thyroid nodule, although only 5–8 % will have a malignant one.
Objective
The objective of this study was to establish the ultrasonographic characteristics which allow us to distinguish benignity from malignancy in thyroid nodules.
Methods
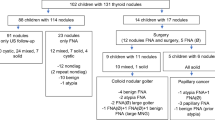
In the study population, inclusion criteria are (1) a single thyroid nodule and (2) multinodular goiter and exclusion criteria are (1) previous thyroid surgery and (2) fine needle aspiration (FNA) in the past month. This study is a double-blind prospective study. The study protocol is as follows: (1) clinical study; (2) ultrasound examination; (3) FNA; and (4) surgery—follow-up. The variables analysed are as follows: a multinodular nodule or goitre; colloid degeneration; morphology; margins; hyperechoic rim; rim thickness; rim morphology; size; angle between the major axis and the skin; echostructure; posterior acoustic findings; calcifications; thick colloid; localization of the intrathyroid nodular tissue; and characteristics in the Doppler scan.
Results
A total of 221 thyroid nodules were analysed. The following ultrasound findings were associated with malignancy (p < 0.05): a nodule with posterior acoustic shadowing; the echotexture of the nodule; intranodular colloid degeneration; nodule margins; nodular morphology; the presence of thick colloid; the angle between the major axis and the skin; characteristics of the intranodular vessels using color Doppler and Doppler energy; and calcifications. In the multivariate analysis, the following factors persisted as predictors of malignancy: the echotexture of the nodule (odds ratio 12.81), microcalcifications (OR 9.05), and chaotic vascularisation in the Doppler energy (OR 43.47).
Conclusions
The high-resolution ultrasound allowed for a more reliable diagnosis of malignancy. The main findings of malignancy were the hypoechogenicity echotexture, microcalcifications, and chaotic intranodular vessels using Doppler energy.
Similar content being viewed by others
References
Gnarini VL, Brigante G, Della Valle E, Diazzi C, Madeo B, Carani C, Rochira V, Simoni M (2013) Very high prevalence of ultrasound thyroid scan abnormalities in healthy volunteers in Modena, Italy. J Endocrinol Investig 36:722–728
Cronan JJ (2008) Thyroid nodules: is it time to turn off the US machines? Radiology 247:602–604
Hoang JK, Lee WK, Lee M, Johnson D, Farell S (2007) US features of thyroid malignancy: pearls and pitfalls. RadioGraphics 27:847–865
Bonavita JA, Mayo J, Babb J, Bennett G, Oweity T, Macari M, Yee J (2009) Pattern recognition of benign nodules at ultrasound of the thyroid: which nodules can be left alone? AJR 193:207–213
Liebeskind A, Sikora AG, Komisar A, Slavit D, Fried K (2005) Rates of malignancy in incidentally discovered thyroid nodules evaluated with sonography and fine-needle aspiration. J Ultrasound Med 24:629–634
Wu LM, Gu HY, Qu XH, Zheng J, Zhang W, Yin Y, Xu JR (2012) The accuracy of ultrasonography in the preoperative diagnosis of cervical lymph node metastasis in patients with papillary thyroid carcinoma: a meta-analysis. Eur J Radiol 81:1798–1805
Khoncarly SM, Tamarkin SW, McHenry CR (2014) Can ultrasound be used to predict malignancy in patients with a thyroid nodule and an indeterminate fine-needle aspiration biopsy? Surgery 156:967–970
Brito JP, Gionfriddo MR, Al Nofal A, Boehmer KR, Leppin AL, Reading C, Callstrom M, Elraiyah TA, Prokop LJ, Stan MN, Murad MH, Morris JC, Montori VM (2014) The accuracy of thyroid nodule ultrasound to predict thyroid cancer: systematic review and meta-analysis. J Clin Endocrinol Metab 99:1253–1263
Bhatia KS, Lee YY, Yuen EH, Ahuja AT (2013) Ultrasound elastography in the head and neck. Part II Accuracy for malignancy. Cancer Imaging 13:260–276
Kim GR, Kim MH, Moon HJ, Chung WY, Kwak JY, Kim EK (2013) Sonographic characteristics suggesting papillary thyroid carcinoma according to nodule size. Ann Surg Oncol 20:906–913
Nicola HD, Szejnfeld J, Logullo AF, Wolosker AMB, Souza LRMF, Chiferi V Jr (2005) Flow pattern and vascular resistive index as predictors of malignancy risk in thyroid follicular neoplasms. J Ultrasound Med 24:897–904
Sultan LR, Xiong H, Zafar HM, Schultz SM, Langer JE, Sehgal CM (2015) Vascularity assessment of thyroid nodules by quantitative color doppler ultrasound. Ultrasound Med Biol 41:1287–1293
Papini E, Guglielmi R, Bianchini A, Crescenzi A, Taccogna S, Nardi F et al (2002) Risk of malignancy in non palpable thyroid nodules: predictive value of ultrasound and color-Doppler features. J Clin Endocrinol Metab 87:1941–1946
Frates MC, Benson CB, Doubilet PM, Cibas ES, Marqusee E (2003) Can color doppler sonography aid in the prediction of malignancy of thyroid nodules? J Ultrasound Med 22:127–131
Reading CC, Charboneau JW, Hay ID, Sebo TJ (2005) Sonography oh thyroid nodules a “classic pattern” diagnostic approach. Ultrasound Q 21:157–165
Udelsman R, Zhang Y (2014) The epidemic of thyroid cancer in the United States: the role of endocrinologists and ultrasounds. Thyroid 24:472–479
Rosario PW (2014) Thyroid nodules with atypia or follicular lesions of undetermined significance (Bethesda category III): importance of ultrasonography and cytological subcategory. Thyroid 24:1115–1120
Azar N, Lance C, Nakamoto D, Michael C, Wasman J (2013) Ultrasonographic thyroid findings suspicious for malignancy. Diagn Cytopathol 41:1107–1114
Moon HJ, Kwak JY, Kim MJ, Son EJ, Kim EK (2010) Can vascularity at power Doppler US help predict thyroid malignancy? Radiology 255:260–269
Sipos JA (2009) Advances in ultrasound for the diagnosis and management of thyroid cancer. Thyroid 19:1363–1372
Kim MJ, Kim EK, Park SI, Kim BM, Kwak JY, Kim SJ, Youk JH, Park SH (2008) US-guided fine-needle aspiration of thyroid nodules: indications, techniques, results. RadioGraphics 28:1869–1889
Salmaslioglu A, Erbil Y, Dural C, Issever H, Kapran Y, Özarmagan S, Tezelman S (2008) Predictive value of sonographic features in preoperative evaluation of malignant thyroid nodules in a multinodular goiter. World J Surg 32:1948–1954
Moon WJ, Jung SL, Lee JH, Na DG, Baek JH, Lee YH, Kim J, Kim HS, Byun JS, Lee DH (2008) Benign and malignant thyroid nodules: US differentiation-multicenter retrospective study. Radiology 247:762–770
Kim JY, Lee CH, Kim SY, Jeon WK, Kang JH, An SK, Jun WS (2008) Radiologic and pathologic findings of nonpalpable thyroid carcinomas detected by ultrasonography in a medical screening center. J Ultrasound Med 27:215–223
Kwak JY, Kim EK, Son EJ, Kim MJ, Oh KK, Kim JY, Kim KI (2007) Papillary thyroid carcinoma manifested solely as microcalcifications on sonography. AJR 189:227–231
Jones R, Spendiff R, Fareedi S, Richards PS (2007) The role of ultrasound in the management of nodular thyroid disease. Imaging 19:28–38
Yoon DY, Lee JW, Chang SK, Choi CS, Yun EJ, Seo YL, Kim KH, Hwang HS (2007) Peripheral calcification in thyroid nodules. J Ultrasound Med 26:1349–1355
Howlett DC, Speirs A (2007) The thyroid incidentaloma—ignore or investigate? J Ultrasound Med 26:1367–1371
Mitchell J, Parangi S (2005) The thyroid incidentaloma: an increasingly frequent consequence of radiologic imaging. Semin Ultrasound CT MRI 26:37–46
Nachiappan AC, Metwalli ZA, Hailey BS, Patel RA, Ostrowski ML, Wynne DM (2014) The thyroid: review of imaging features and biopsy techniques with radiologic-pathologic correlation. Radiographics 34:276–293
Ozel A, Erturk SM, Ercan A, Yılmaz B, Basak T, Cantisani V, Basak M, Karpat Z (2012) The diagnostic efficiency of ultrasound in characterization for thyroid nodules: how many criteria are required to predict malignancy? Med Ultrason 14:24–28
Seo H, Na DG, Kim JH, Kim KW, Yoon JW (2015) Ultrasound-based risk stratification for malignancy in thyroid nodules: a four-tier categorization system. Eur Radiol 25:2153–2162
Cordes M, Kondrat P, Uder M, Kuwert T, Sasiadek M (2014) Differential diagnostic ultrasound criteria of papillary and follicular carcinomas: a multivariate analysis. Fortschr Röntgenstr 186:489–495
Yoon JH, Kwon HJ, Kim EK, Moon HJ, Kwak JY (2016) The follicular variant of papillary thyroid carcinoma: characteristics of preoperative ultrasonography and cytology. Ultrasonography 35:47–54
Gu WJ, Yan HX, Lou YK, Wang FL, Yang GQ, Guo QH, Jin N, Zang L, Chen K, Du J, Wang XL, Yang LJ, Ba JM, Dou JT, Mu YM, Pan CY, Lv ZH (2015) Characterization of papillary thyroid microcarcinomas using sonographic features in malignant papillary thyroid cancer: a retrospective analysis. Medicine (Baltimore) 94:e841
Lee HS, Park HS, Kim SW, Choi G, Park HS, Hong JC, Lee SG, Baek SM, Lee KD (2013) Clinical characteristics of papillary thyroid microcarcinoma less than or equal to 5 mm on ultrasonography. Eur Arch Otorhinolaryngol 270:2969–2974
Lee YC, Eun YG, Sohn YM, Rhee SY, Hong IK, Chon S, Oh SJ, Kim DY (2015) Predictive factors for occult contralateral carcinoma in patients with unilateral papillary thyroid microcarcinoma by preoperative ultrasonographic and pathological features. World J Surg 39:1736–1741
Yoon SJ, Yoon DY, Chang SK, Seo YL, Yun EJ, Choi CS, Bae SH (2010) “Taller-than-wide sign” of thyroid malignancy: comparison between ultrasound and CT. AJR 194:W420–W424
Chan BK, Desser TS, McDougall I, Weigel RJ, Jeffrey RB Jr (2003) Common and uncommon sonographic features of papillary thyroid carcinoma. J Ultrasound Med 22:1083–1090
Wang Z, Zhang H, Zhang P, He L, Dong W (2014) Diagnostic value of ultrasound-detected calcification in thyroid nodules. Ann Acad Med Singapore 43:102–106
Lee SH, Baek JS, Lee JY, Lim JA, Cho SY, Lee TH, Ku YH, Kim HI, Kim MJ (2013) Predictive factors of malignancy in thyroid nodules with a cytological diagnosis of follicular neoplasm. Endocr Pathol 24:177–183
Ma JJ, Ding H, Xu BH, Xu C, Song LJ, Huang BJ, Wang WP (2014) Diagnostic performances of various gray-scale, color Doppler, and contrast-enhanced ultrasonography findings in predicting malignant thyroid nodules. Thyroid 24:355–363
Tai JD, Yang JL, Wu SC, Wang BW, Chang CJ (2012) Risk factors for malignancy in patients with solitary thyroid nodules and their impact on the management. J Cancer Res Ther 8:379–383
Wang Y, Li L, Wang YX, Feng XL, Zhao F, Zou SM, Hao YZ, Ying JM, Zhou CW (2012) Ultrasound findings of papillary thyroid microcarcinoma: a review of 113 consecutive cases with histopathologic correlation. Ultrasound Med Biol 38:1681–1688
Iannuccilli JD, Cronan JJ, Monchik JM (2004) Risk for malignancy of thyroid nodules as assessed by sonographic criteria. J Ultrasound Med 23:1455–1464
Zambudio AR, Rodríguez JM, Riquelme J, Soria T, Canteras M, Parrilla P (2004) Prospective study of postoperative complications after total thyroidectomy for multinodular goitres by surgeons with experience in endocrine surgery. Ann Surg 240:18–25
Rios A, Rodríguez J, Ferri B, Martinez-Barba E, Febrero B, Parrilla P (2013) Are prognostic scoring systems of value in patients with Follicular Thyroid Carcinoma? Eur J Endocrinol 169:821–827
Ríos A, Rodríguez JM, Balsalobre MD, Tebar FJ, Parrilla P (2010) The value of various definitions of intrathoracic goiter for predicting intra-operative and postoperative complications. Surgery 147:233–238
Kwak JY, Koo H, Youk JH, Kim MJ, Moon HJ, Son EJ, Kim EK (2010) Value of US correlation of a thyroid nodule with initially benign cytologic results. Radiology 254:292–300
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Funding
This study was not funded by any company.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Disclosure statement
The authors have nothing to disclose.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Antonio Ríos Zambudio and B. Torregrosa contributed equally to this work.
Rights and permissions
About this article
Cite this article
Rios, A., Torregrosa, B., Rodríguez, J.M. et al. Ultrasonographic risk factors of malignancy in thyroid nodules. Langenbecks Arch Surg 401, 839–849 (2016). https://doi.org/10.1007/s00423-016-1451-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-016-1451-y