Abstract
Purpose
In the east countries, patients with hepatocellular carcinoma (HCC) are usually associated with varied degrees of liver cirrhosis, and anatomic resection is therefore limited to use, especially in those with severe liver cirrhosis. This study aims to evaluate the clinical value of non-anatomic resection in HCC patients with cirrhosis.
Methods
Seventy-seven consecutive HCC patients with cirrhosis underwent non-anatomic liver resection in Tongji Hospital from January 2003 to December 2006. The clinical data, severity of liver cirrhosis, and survival rates of these patients were retrospectively evaluated, and the prognostic factors were analyzed.
Results
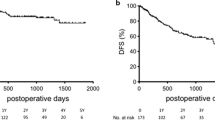
One-, 2-, and 3-year overall and disease-free survival rates of this cohort of patients were 78%, 68%, 56%, and 66%, 58%, 55%, respectively. The hospital mortality and morbidity were 0% and 24.7%, respectively. The 1-, 2-, and 3-year overall survival rates were 85.7%, 77.1%, and 74.3% in the patients with mild cirrhosis, 81.5%, 63%, and 48.1% in the patients with moderate cirrhosis, and 60.0%, 53.3%, and 26.7% in the patients with severe cirrhosis, respectively. There was a significant difference among the patients with different grades of cirrhosis (P = 0.001). Multivariate and univariate analyses revealed that severity of cirrhosis, tumor diameter larger than 5 cm, and vascular invasion were independent prognostic factors.
Conclusions
Non-anatomic liver resection for HCC could yield comparable outcomes with anatomic resection in the patients with mild cirrhosis or tumors diameter smaller than 5 cm. Severity of cirrhosis is an independent factor worsening long-time survival. Non-anatomic resection is a safe and effective surgical modality in the treatment of HCC patients with cirrhosis.



Similar content being viewed by others
References
Chen XP, Huang ZY (2005) Surgical treatment of hepatocellular carcinoma in China: surgical techniques, indications, and outcomes. Langenbecks Arch Surg 390:259–265
Chen XP, Qiu FZ, Wu ZD, Zhang ZW, Huang ZY, Chen YF (2006) Long-term outcome of resection of large hepatocellular carcinoma. Br J Surg 93:600–606
Rutkauskas S, Gedrimas V, Pundzius J, Barauskas G, Basevicius A (2006) Clinical and anatomical basis for the classification of the structural parts of liver. Medicina (Kaunas) 42:98–106
El-Serag HB, Mason AC (1999) Rising incidence of hepatocellular carcinoma in the United States. N Engl J Med 340:745–750
Toyosaka A, Okamoto E, Mitsunobu M, Oriyama T, Nakao N, Miura K (1996) Intrahepatic metastases in hepatocellular carcinoma: evidence for spread via the portal vein as an efferent messel. Am J Gastroenterol 91:1610–1615
Tanaka K, Shimada H, Matsumoto C, Matsuo K, Nagano Y, Endo I et al (2008) Anatomic versus limited nonanatomic resection for solitary hepatocellular carcinoma. Surgery 143:607–615
Zhou XD, Tang ZY, Yang BH, Lin ZY, Ma ZC, Ye SL et al (2001) Experience of 1000 patients who underwent hepatectomy for small hepatocellular carcinoma. Cancer 91:1479–1486
Makuuchi M, Hasegawa H, Yamazaki S (1985) Ultrasonically guided subsegmentectomy. Surg Gynecol Obstet 161:346–350
Cho YB, Lee KU, Lee HW, Cho EH, Yang SH, Cho JY (2007) Anatomic versus non-anatomic resection for small single hepatocellular carcinomas. Hepatogastroenterology 54(78):1766–1769
Makuuchi M, Imamura H, Sugawara Y, Takayama T (2002) Progress in surgical treatment of hepatocellular carcinoma. Oncology 62(suppl 1):74–81
Imamura H, Matsuyama Y, Miyagawa Y, Ishida K, Shimada R, Miyagawa S et al (1999) Prognostic significance of anatomical resection and des-gamma-carboxy prothrombin in patients with hepatocellular carcinoma. Br J Surg 86(1–2):1032–1038
Yamamoto M, Takasaki K, Ohtsubo T, Katsuragawa H, Fukuda C, Katagiri S (2001) Effectiveness of systematized hepatectomy with Glisson’s pedicle transaction at the hepatic hilus for small nodular hepatocellular carcinoma: retrospective analysis. Surgery 130(1–3):443–448
Yuki K, Hirohashi S, Sakamoto M, Kanai T, Shimosato Y (1990) Growth and spread of hepatocellular carcinoma. A review of 240 consecutive autopsy cases. Cancer 66:2174–2179
Hasegawa K, Kokudo N, Imamura H, Matsuyama Y, Aoki T, Minagawa M et al (2005) Prognostic impact of anatomic resection for hepatocellular carcinoma. Ann Surg 242:252–259
Kaibori M, Matsui Y, Hijikawa T, Uchida Y, Kwon AH, Kamiyama Y (2006) Comparison of limited and anatomic hepatic resection for hepatocellular carcinoma with hepatitis C. Surgery 139:385–394
Yamashita Y, Taketomi A, Itoh S, Kitagawa D, Kayashima H, Harimoto N et al (2007) Longterm favorable results of limited hepatic resections for patients with hepatocellular carcinoma: 20 years of experience. J Am Coll Surg 205:19–26
Rigimbeau JM, Kianmanesh R, Farges O, Dondero F, Sauvanet A, Beighiti J (2002) Extent of liver resection influences the outcome in patients with cirrhosis and small hepatocellular carcinoma. Surgery 131:311–317
Cherqui D, Laurent A, Mocellin N, Tayar C, Luciani A, Van Nhieu JT et al (2009) Liver resection for transplantable hepatocellular carcinoma: long-term survival and role of secondary liver transplantation. Ann Surg 250:738–746
de Villa V, Lo CM (2007) Liver transplantation for hepatocellular carcinoma in Asia. Oncologist 12:1321–1331
Chen XP, Wu ZD, Huang ZY, Qiu FZ (2005) Use of hepatectomy and splenectomy to treat hepatocellular carcinoma with cirrhosis hypersplenism. Br J Surg 92:334–339
Eguchi S, Kanematsu T, Arii S, Okazaki M, Okita K, Omata M et al (2008) Comparison of the outcomes between an anatomical subsegmentectomy and a non-anatomical minor hepatectomy for single hepatocellular carcinomas based on a Japanese nationwide survey. Surgery 143:469–475
Kosuge T, Makuuchi M, Takayama T, Yamamoto J, Shimada K, Yamasaki S (1993) Long-term results after resection of hepatocellular carcinoma: experience of 480 cases. Hepatogastroenterology 40:328–332
Suh KS (2005) Systematic hepatectomy for small hepatocelular carcinoma in Korea. J Hepatobiliary Pancreat Surg 12:365–370
Ercolani G, Grazi GL, Ravaioli M, Del Gaudio M, Gardini A, Cescon M et al (2003) Liver resection for hepatocellular carcinoma on cirrhosis: univariate and multivariate analysis of risk factors for intrahepatic recurrence. Ann Surg 237:536–543
Wakai T, Shirai Y, Yokoyama N, Nagakura S, Hatakeyama K (2003) Hepatitis viral status affects the pattern of intrahepatic recurrence after resection for hepatocellular carcinoma. Eur J Surg Oncol 29:266–271
Poon RT, Fan ST, Ng IO, Wong J (2000) Significance of resection margin in hepatectomy for hepatocellular carcinoma. Ann Surg 231(4):544–551
Shimada K, Sakamoto Y, Esaki M, Kosuge T (2008) Role of the width of the surgical margin in a hepatectomy for small hepatocellular carcinomas eligible for percutaneous local ablative therapy. Am J Surg 195:775–781
Shi M, Guo RP, Lin XJ, Zhang YQ, Chen MS, Zhang CQ et al (2007) Partial hepatectomy with wide versus narrow resection margin for solitary hepatocellular carcinoma. Ann Surg 245:36–43
Acknowledgments
This work was supported by funding from the National Natural Science Foundation of China (No. 30772126) and the New Centaury Excellent Talent Foundation of China Ministry of Education (No. NCET-04-0701) to Dr. Zhi-Yong Huang, and by grants from the Chinese Ministry of Public Health for Key Clinical Projects (No. 353, 2007) and the Health Department, the Science & Technology Department of Hubei Province for the Clinical Medicine Research Centre of Hepatic Surgery (2007) to Prof Xiao-ping Chen.
Conflicts of interest
None.
Authors' contributions
Study conception and design, Zhi-yong Huang and Xiao-ping Chen
Acquisition of data, Gen Chen and Rong-yao Cai
Analysis and interpretation of data, Zhi-yong Huang and Xiao-yi Hao
Drafting of manuscript, Zhi-yong Huang, Gen Chen and Yin-feng Zhao
Critical revision of manuscript, Xiao-ping Chen
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huang, Zy., Chen, G., Hao, Xy. et al. Outcomes of non-anatomic liver resection for hepatocellular carcinoma in the patients with liver cirrhosis and analysis of prognostic factors. Langenbecks Arch Surg 396, 193–199 (2011). https://doi.org/10.1007/s00423-010-0700-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-010-0700-8