Abstract
Aim
The aim of this study was to evaluate microscopic nodal status in papillary thyroid carcinoma (PTC) with and without lymphadenopathy and its relation to outcomes.
Materials and methods
We retrospectively analyzed 134 patients with PTC who underwent initial thyroidectomy. Forty-two patients with lymphadenopathy underwent therapeutic modified neck dissection (MND) and 92 without lymphadenopathy underwent prophylactic MND. The frequencies, numbers, and percentages of lymph node metastasis (LNM) were determined to evaluate nodal status; then, whether each nodal status influence to outcomes was analyzed. Disease-free survival (DFS) and disease-specific survival (DSS) were assessed (Kaplan–Meier method and log-rank test).
Results
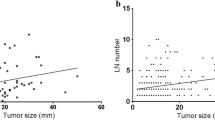
Lymphadenopathy was significantly related to local recurrence and DFS, but not DSS. The frequency (100 vs 67.4%), number (15.8 vs 2.7), and percentage (49.7 vs 17.8%) were significantly higher in patients with lymphadenopathy than in those without lymphadenopathy (p < 0.0001). Similarly, these were significantly higher in patients who developed recurrence than in those who did not. Recurrence was frequent in older patients with lymphadenopathy. The frequency, number, and percentage were also higher in older patients who developed local recurrence.
Conclusions
Lymphadenopathy and microscopic nodal status are significantly related to recurrence. Only a few nodes seem to be involved pathologically when no lymphadenopathy.

Similar content being viewed by others
References
Noguchi S, Murakami N, Yamashita H, Toda M, Kawamoto H (1998) Papillary thyroid carcinoma: modified radical neck dissection improves prognosis. Arch Surg 133:276–280
Chow SM, Law SC, Chan JK, Au SK, Yau S, Lau WH (2003) Papillary microcarcinoma of the thyroid: prognostic significance of lymph node metastasis and multifocality. Cancer 98:31–40
Lundgren CI, Hall P, Dickman PW, Zedenius J (2006) Clinically significant prognostic factors for differentiated thyroid carcinoma. Cancer 106:524–531
Machens A, Holzhausen HJ, Lautenschlager C, Thanh PN, Dralle H (2003) Enhancement of lymph node metastasis and distant metastasis of thyroid carcinoma. Cancer 98:712–719
Ducci M, Appetecchia M, Marzetti M (1997) Neck dissection for surgical treatment of lymphnode metastasis in papillary thyroid carcinoma. J Exp Clin Cancer Res 16:333–335
Musacchio MJ, Kim AW, Vijungco JD, Prinz RA (2003) Greater local recurrence occurs with “berry picking” than neck dissection in thyroid cancer. Am Surg 69:191–196
Beasley NJ, Lee J, Eski S, Walfish P, Witterick I, Freeman JL (2002) Impact of nodal metastases on prognosis in patients with well-differentiated thyroid cancer. Arch Otolaryngol Head Neck Surg 128:825–828
Mazzaferri EL, Young RL (1981) Papillary thyroid carcinoma: a 10 year follow-up report of the impact of therapy in 576 patients. Am J Med 70:511–518
Sivanandan R, Soo KC (2001) Pattern of cervical lymph node metastases from papillary carcinoma of the thyroid. Br J Surg 88:1241–1244
Kupferman ME, Patterson M, Mandel SJ, LiVolsi V, Weber RS (2004) Patterns of lateral neck metastasis in papillary thyroid carcinoma. Arch Otolaryngol Head Neck Surg 130:857–860
McHenry CR, Rosen IB, Walfish PG (1991) Prospective management of nodal metastases in differentiated thyroid cancer. Am J Surg 162:353–356
Wada N, Duh QY, Sugino K, Iwasaki H, Kameyama K, Mimura T, Ito K, Takami H, Takanashi Y (2003) Lymph node metastasis from 259 papillary thyroid microcarcinomas: frequency, pattern of occurrence and recurrence, and optimal strategy for neck dissection. Ann Surg 237:399–407
Borson-Chazot F, Causeret S, Lifante JC, Augros M, Berger N, Peix JL (2004) Predictive factors for recurrence from a series of 74 children and adolescents with differentiated thyroid cancer. World J Surg 28:1088–1092
Leboulleux S, Rubino C, Baudin E, Caillou B, Hartl DM, Bidart JM, Travagli JP, Schlumberger M (2005) Prognostic factors for persistent or recurrent disease of papillary thyroid carcinoma with neck lymph node metastases and/or tumor extension beyond the thyroid capsule at initial diagnosis. J Clin Endocrinol Metab 90:5723–5729
Scheumann GF, Gimm O, Wegener G, Hundeshagen H, Dralle H (1994) Prognostic significance and surgical management of locoregional lymph node metastases in papillary thyroid cancer. World J Surg 18:559–567
Sugitani I, Kasai N, Fujimoto Y, Yanagisawa A (2004) A novel classification system for patients with PTC: addition of the new variables of large (3 cm or greater) nodal metastases and reclassification during the follow-up period. Surgery 135:139–148
Sugino K, Kure Y, Iwasaki H, Ozaki O, Mimura T, Matsumoto A, Ito K (1995) Metastases to the regional lymph nodes, lymph node recurrence, and distant metastases in nonadvanced papillary thyroid carcinoma. Surg Today 25:324–328
Hughes CJ, Shaha AR, Shah JP, Loree TR (1996) Impact of lymph node metastasis in differentiated carcinoma of the thyroid: a matched-pair analysis. Head Neck 18:127–132
Hay ID, Bergstralh EJ, Grant CS, McIver B, Thompson GB, van Heerden JA, Goellner JR (1999) Impact of primary surgery on outcome in 300 patients with pathologic tumor-node-metastasis stage III papillary thyroid carcinoma treated at one institution from 1940 through 1989. Surgery 126:1173–1181
Gimm O, Rath FW, Dralle H (1998) Pattern of lymph node metastases in papillary thyroid carcinoma. Br J Surg 85:252–254
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wada, N., Suganuma, N., Nakayama, H. et al. Microscopic regional lymph node status in papillary thyroid carcinoma with and without lymphadenopathy and its relation to outcomes. Langenbecks Arch Surg 392, 417–422 (2007). https://doi.org/10.1007/s00423-007-0159-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-007-0159-4