Abstract
Purpose
The aim of this study was to evaluate the effectiveness of an exercise protocol designed to induce delayed-onset muscle soreness (DOMS) in paraspinal muscles and its effects on low back functional capacities.
Methods
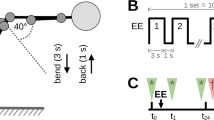
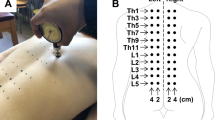
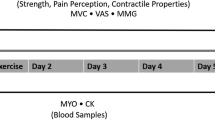
Twenty-four healthy participants were asked to perform four series of 25 trunk flexion–extension in a prone position (45° inclined Roman chair). The protocol was performed using loads corresponding to participant’s trunk weight plus 10% of their trunk extension maximal voluntary contraction. Perceived soreness and pain were assessed using an 11-point numerical analogue scale three times a day during 5 day post-DOMS protocol. Pressure-pain thresholds (PPT) in paraspinal muscles (L2 and L4 bilaterally) and the vastus medialis (control site), and trunk extension maximal voluntary contraction were assessed 24–36 h post-protocol and compared to baseline (t tests).
Results
Muscle soreness (3.8/10) and pain (2.1/10) peak scores were observed 24–36 h post-protocol (mean of 28 h). A significant reduction in trunk extension maximal voluntary contraction was observed post-protocol (p = 0.005). Significant reductions in PPT were observed post-protocol for all trunk extensor sites (ps < 0.01), but not for the control site (p = 0.40).
Conclusions
The exercise protocol efficiently led to low back muscle DOMS, reduced functional capacities, and increased pain sensitivity locally. Such protocol could be used as an efficient and safe experimental low back pain model.



Similar content being viewed by others
Abbreviations
- DOMS:
-
Delayed-onset muscle soreness
- MVC:
-
Maximal voluntary contraction
- PPT:
-
Pressure-pain threshold
References
Bishop MD, Horn ME, George SZ (2011a) Exercise-induced pain intensity predicted by pre-exercise fear of pain and pain sensitivity. Clin J Pain 27:398–404. https://doi.org/10.1097/AJP.0b013e31820d9bbf
Bishop MD, Horn ME, George SZ, Robinson ME (2011b) Self-reported pain and disability outcomes from an endogenous model of muscular back pain. BMC Musculoskelet Disord 12:35. https://doi.org/10.1186/1471-2474-12-35
Bishop MD, Horn ME, Lott DJ, Arpan I, George SZ (2011c) Magnitude of spinal muscle damage is not statistically associated with exercise-induced low back pain intensity. Spine J Off J N Am Spine Soc 11:1135–1142. https://doi.org/10.1016/j.spinee.2011.11.005
Cheung K, Hume P, Maxwell L (2003) Delayed onset muscle soreness: treatment strategies and performance factors. Sports Med 33:145–164
Chesterton LS, Sim J, Wright CC, Foster NE (2007) Interrater reliability of algometry in measuring pressure pain thresholds in healthy humans, using multiple raters. Clin J Pain 23:760–766. https://doi.org/10.1097/AJP.0b013e318154b6ae
Clarkson PM, Dedrick ME (1988) Exercise-induced muscle damage, repair, and adaptation in old and young subjects. J Gerontol 43:M91–M96
Clarkson PM, Hubal MJ (2002) Exercise-induced muscle damage in humans. Am J Phys Med Rehabil Assoc Acad Physiatr 81:S52–S69. https://doi.org/10.1097/01.PHM.0000029772.45258.43
Cleak MJ, Eston RG (1992) Delayed onset muscle soreness: mechanisms and management. J Sports Sci 10:325–341. https://doi.org/10.1080/02640419208729932
Crameri RM, Aagaard P, Qvortrup K, Langberg H, Olesen J, Kjaer M (2007) Myofibre damage in human skeletal muscle: effects of electrical stimulation versus voluntary contraction. J Physiol 583:365–380. https://doi.org/10.1113/jphysiol.2007.128827
de Leva P (1996) Adjustments to Zatsiorsky–Seluyanov’s segment inertia parameters. J Biomech 29:1223–1230
Dubois JD, Piche M, Cantin V, Descarreaux M (2011) Effect of experimental low back pain on neuromuscular control of the trunk in healthy volunteers and patients with chronic low back pain. J Electromyogr Kinesiol Off J Int Soc Electrophysiol Kinesiol 21:774–781. https://doi.org/10.1016/j.jelekin.2011.05.004
Falla D, Gizzi L, Tschapek M, Erlenwein J, Petzke F (2014) Reduced task-induced variations in the distribution of activity across back muscle regions in individuals with low back pain. Pain 155:944–953. https://doi.org/10.1016/j.pain.2014.01.027
Falla D, Gizzi L, Parsa H, Dieterich A, Petzke F (2017) People with chronic neck pain walk with a stiffer spine. J Orthop Sports Phys Ther 47:268–277. https://doi.org/10.2519/jospt.2017.6768
George SZ, Hirsh AT (2009) Psychologic influence on experimental pain sensitivity and clinical pain intensity for patients with shoulder pain. J Pain Off J Am Pain Soc 10:293–299. https://doi.org/10.1016/j.jpain.2008.09.004
Hjortskov N, Essendrop M, Skotte J, Fallentin N (2005) The effect of delayed-onset muscle soreness on stretch reflexes in human low back muscles. Scand J Med Sci Sports 15:409–415
Horn ME, Bishop MD (2013) Flexion relaxation ratio not responsive to acutely induced low back pain from a delayed onset muscle soreness protocol. ISRN Pain. https://doi.org/10.1155/2013/617698
Kumazawa T, Mizumura K (1977) Thin-fibre receptors responding to mechanical, chemical, and thermal stimulation in the skeletal muscle of the dog. J Physiol 273:179–194
Larsen LH, Hirata RP, Graven-Nielsen T (2017) Pain-evoked trunk muscle activity changes during fatigue and DOMS. Eur J Pain 21:907–917. https://doi.org/10.1002/ejp.993
Latremoliere A, Woolf CJ (2009) Central sensitization: a generator of pain hypersensitivity by central neural plasticity. J Pain Off J Am Pain Soc 10:895–926. https://doi.org/10.1016/j.jpain.2009.06.012
Lewis PB, Ruby D, Bush-Joseph CA (2012) Muscle soreness and delayed-onset muscle soreness. Clin Sports Med 31:255–262. https://doi.org/10.1016/j.csm.2011.09.009
Lo Vecchio S, Petersen LJ, Finocchietti S, Gazerani P, Arendt-Nielsen L, Graven-Nielsen T (2015) The effect of combined skin and deep tissue inflammatory pain models. Pain Med 16:2053–2064. https://doi.org/10.1111/pme.12826
Mayer JM, Mooney V, Matheson LN, Erasala GN, Verna JL, Udermann BE, Leggett S (2006) Continuous low-level heat wrap therapy for the prevention and early phase treatment of delayed-onset muscle soreness of the low back: a randomized controlled trial. Arch Phys Med Rehabil 87:1310–1317. https://doi.org/10.1016/j.apmr.2006.07.259
Newham DJ, Jones DA, Edwards RH (1983) Large delayed plasma creatine kinase changes after stepping exercise. Muscle Nerve 6:380–385. https://doi.org/10.1002/mus.880060507
Prasartwuth O, Taylor JL, Gandevia SC (2005) Maximal force, voluntary activation and muscle soreness after eccentric damage to human elbow flexor muscles. J Physiol 567:337–348. https://doi.org/10.1113/jphysiol.2005.087767
Proske U, Allen TJ (2005) Damage to skeletal muscle from eccentric exercise. Exerc Sport Sci Rev 33:98–104
Soer R, Groothoff JW, Geertzen JH, van der Schans CP, Reesink DD, Reneman MF (2008) Pain response of healthy workers following a functional capacity evaluation and implications for clinical interpretation. J Occup Rehabil 18:290–298. https://doi.org/10.1007/s10926-008-9132-5
Steele J, Bruce-Low S, Smith D (2014) A reappraisal of the deconditioning hypothesis in low back pain: review of evidence from a triumvirate of research methods on specific lumbar extensor deconditioning. Curr Med Res Opin 30:865–911. https://doi.org/10.1185/03007995.2013.875465
Trost Z, France CR, Thomas JS (2011) Pain-related fear and avoidance of physical exertion following delayed-onset muscle soreness. Pain 152:1540–1547. https://doi.org/10.1016/j.pain.2011.02.038
Tsao H, Tucker KJ, Coppieters MW, Hodges PW (2010) Experimentally induced low back pain from hypertonic saline injections into lumbar interspinous ligament and erector spinae muscle. Pain 150:167–172. https://doi.org/10.1016/j.pain.2010.04.023
Udermann BE, Mayer JM, Graves JE, Ploutz-Snyder LL (2002) Development of an exercise protocol to elicit delayed-onset muscle soreness in the lumbar extensors. Int Sports J 6:128–135
Vila-Cha C, Hassanlouei H, Farina D, Falla D (2012) Eccentric exercise and delayed onset muscle soreness of the quadriceps induce adjustments in agonist-antagonist activity, which are dependent on the motor task. Exp Brain Res Experimentelle Hirnforschung Experimentation Cerebrale 216:385–395. https://doi.org/10.1007/s00221-011-2942-2
Vlaeyen JW, Linton SJ (2000) Fear-avoidance and its consequences in chronic musculoskeletal pain: a state of the art. Pain 85:317–332
Weerakkody NS, Percival P, Hickey MW, Morgan DL, Gregory JE, Canny BJ, Proske U (2003) Effects of local pressure and vibration on muscle pain from eccentric exercise and hypertonic saline. Pain 105:425–435
Acknowledgements
The authors wish to acknowledge the contribution of Catherine Pauzé-Brodeur (undergraduate student) who assisted the authors during the experiment.
Author information
Authors and Affiliations
Contributions
All authors have contributed substantially to the manuscript. Study conception and design (JA and MD), acquisition of data (JA and AL), analysis and interpretation of data (all authors), drafting the manuscript (JA and AL), revising it critically for important intellectual content (all authors), and final approval of the version to be published (all authors).
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Communicated by Lori Ann Vallis.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Abboud, J., Lessard, A., Piché, M. et al. Paraspinal muscle function and pain sensitivity following exercise-induced delayed-onset muscle soreness. Eur J Appl Physiol 119, 1305–1311 (2019). https://doi.org/10.1007/s00421-019-04117-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-019-04117-6