Abstract
Purpose
To assess treatment effects following intravitreal injection of ocriplasmin for vitreomacular traction (VMT), with or without full-thickness macular hole (FTMH), in real-life setting.
Methods
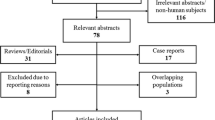
This is a monocentric, retrospective, consecutive series of 82 eyes from 82 patients who underwent ocriplasmin treatment between July 2013 and December 2016. We included 57 eyes with pure VMT, 17 eyes with small FTMHs, and eight eyes with medium FTMHs. Primary outcome measures were VMT release and MH closure rates. Secondary outcomes were visual acuity (VA), morphological changes, and subjective visual impairment after 1, 3, and 6 months and at last follow-up.
Results
After a median follow-up of 10 months, VMT release was achieved by pharmacologic vitreolysis in 57% of all eyes, whereas the macular hole closure rate was 32%. In those presenting with five or more positive prognostic factors (PPF), eyes with pure VMT showed nonsurgical traction release in 88%, and FTMHs were released in 93%, with a closure rate of 20%. Small FTMHs closed in 41% and medium FTMHs in 13%. The mean change in VA (LogMAR) was −0.07 ± 0.24 (median − 0.10) in all eyes. Subretinal fluid accumulation and ellipsoid zone changes were seen in 31% and 37% of all eyes, respectively. They were more frequent in eyes with traction release, but were self-limited.
Conclusions
In a real-life setting, release of VMT by ocriplasmin injection can be achieved in the majority of eyes, relying on a strict patient selection. Closure of FTMHs rather correlates with hole diameter than with presence of PPF, and remains a rare finding in medium FTMHs.


Similar content being viewed by others
References
Duker JS, Kaiser PK, Binder S et al (2013) The international Vitreomacular traction study group classification of vitreomacular adhesion, traction, and macular hole. Ophthalmology 120:2611–2619
Gandorfer A, Rohleder M, Sethi C et al (2004) Posterior vitreous detachment induced by microplasmin. Invest Ophthalmol Vis Sci 45:641–647
de Smet MD, Valmaggia C, Zarranz-Ventura J, Willekens B (2009) Microplasmin: ex vivo characterization of its activity in porcine vitreous. Invest Ophthalmol Vis Sci 50:814–819
de Smet MD, Gandorfer A, Stalmans P et al (2009) Microplasmin intravitreal administration in patients with vitreomacular traction scheduled for vitrectomy: the MIVI I trial. Ophthalmology 116:1349–1355
Stalmans P, Benz MS, Gandorfer A et al (2012) MIVI-TRUST study group. Enzymatic vitreolysis with ocriplasmin for vitreomacular traction and macular holes. N Engl J Med 367:606–615
Haller JA, Stalmans P, Benz MS et al (2015) Efficacy of intravitreal ocriplasmin for treatment of vitreomacular adhesion. Subgroup analyses from two randomized trials. Ophthalmology 122:117–122
Gandorfer A, Benz MS, Haller JA et al (2015) MIVI-TRUST study group. Association between anatomical resolution and functional outcomes in the MIVI-Trust studies using ocriplasmin to treat symptomatic vitreomacular adhesion/vitreomacular traction, including when associated with macular hole. Retina 35:1151–1157
Kim BT, Schwartz SG, Smiddy WE et al (2013) Initial outcomes following intravitreal ocriplasmin for treatment of symptomatic vitreomacular adhesion. Ophthalmic Surg Lasers Imaging Retina 44:334–343
Singh RP, Li A, Bedi R et al (2014) Anatomical and visual outcomes following ocriplasmin treatment for symptomatic vitreomacular traction syndrome. Br J Ophthalmol 98:356–360
Sharma P, Juhn A, Houston SK et al (2015) Efficacy of intravitreal ocriplasmin on vitreomacular traction and full-thickness macular holes. Am J Ophthalmol 159:861.e2–867.e2
Dugel PU, Tolentino M, Feiner L et al (2016) Results of the 2-year ocriplasmin for treatment for symptomatic vitreomacular adhesion including macular hole (OASIS) randomized trial. Ophthalmology 123:2232–2247
Warrow DJ, Lai MM, Patel A et al (2015) Treatment outcomes and spectral-domain optical coherence tomography findings of eyes with symptomatic vitreomacular adhesion treated with intravitreal ocriplasmin. Am J Ophthalmol 159:20–30
Maier M, Abraham S, Frank C et al (2016) Pharmakologische Vitreolyse mit Ocriplasmin als Behandlungsoption bei symptomatischer fokaler vitreomakulärer Traktion mit oder ohne Makulaforamen (≤400 μm) im Vergleich zur transkonjunktivalen Vitrektomie. Ophthalmologe 114:148–154 German
Stalmans P, Duker JS, Kaiser PK et al (2013) OCT-based interpretation of the vitreomacular interface and indications for pharmacologic vitreolysis. Retina 33:2003–2011
Hahn P, Chung MM, Flynn HW et al (2015) Safety profile of ocriplasmin for symptomatic vitreomacular adhesion: a comprehensive analysis of premarketing and postmarketing experiences. Retina 35:1128–1134
Shah SP, Jeng-Miller KW, Fine HF et al (2016) Post-marketing survey of adverse events following ocriplasmin. Ophthalmic Sug Lasers Imaging Retina 47:156–160
Beebe DC (2015) Understanding the adverse effects of ocriplasmin. JAMA Ophthalmol 133:229
Nudleman E, Franklin MS, Wolfe JD et al (2016) Resolution of subretinal fluid and outer retinal changes in patients treated with ocriplasmin. Retina 36:738–743
Quezada-Ruiz C, Pieramici DJ, Nasir M et al (2015) Outer retina reflectivity changes on SD-OCT after intravitreal ocriplasmin for vitreomacular traction and macular hole. Retina 35:1144–1150
Itoh Y, Ehlers JP (2016) Ellipsoid zone mapping and outer retinal characterization after intravitreal ocriplasmin. Retina 36:2290–2296
Itoh Y, Kaiser PK, Singh RP et al (2014) Assessment of retinal alterations after intravitreal ocriplasmin with spectral-domain optical coherence tomography. Ophthalmology 121:2506.e2-2507.e2
Figueira J, Martins D, Pessoa B et al (2016) The Portuguese experience with ocriplasmin in clinical practice. Opthalmic Res 56:186–192
Greven MA, Garg S, Chiu B et al (2016) Vitrectomy after ocriplasmin for VitreOmacular adhesion or macular hole (VAVOOM) study. Br J Ophthalmol 100:1211–1215
Schumann RG, Wolf A, Hoerauf H et al (2017) Vitrectomy for persistent macular holes following ocriplasmin injection: a comparative multicenter study. Retina. doi:10.1097/IAE.0000000000001473
Khan MA, Haller JA (2016) Ocriplasmin for treatment of vitreomacular traction: an update. Ophthalmol Ther 5:147–159
Chatziralli I, Theodossiadis G, Xanthopoulou P, Miligkos M, Siviprasad S, Theodossiadis P (2016) Ocriplasmin use for vitreomacular traction and macular hole: a meta-analysis and comprehensive review on predictive factors for vitreous release and potential complications. Graefes Arch Clin Exp Ophthalmol 254:1247–1256
Chen W, Mo W, Sun K et al (2009) Microplasmin degrades fibronectin and laminin at the vitreoretinal interface and outer retina during enzymatic vitrectomy. Curr Eye Res 34:1057–1064
Libby RT, Lavallee CR, Balkema GW et al (1999) Disruption of laminin beta2 chain production causes alterations in morphology and function in the CNS. J Neurosci 19:9399–9411
Schumann RG, Wolf A, Mayer WJ et al (2015) Pathology of internal limiting membrane specimens following invtravitreal injection of ocriplasmin. Am J Ophthalmol 160:767–778
Vielmuth F, Schumann RG, Spindler V et al (2016) Biomechanical properties of the internal limiting membrane after intravitreal Ocriplasmin treatment. Ophthalmologica 235:233–240
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licencing arrangements) or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Schumann, R.G., Langer, J., Compera, D. et al. Assessment of intravitreal ocriplasmin treatment for vitreomacular traction in clinical practice. Graefes Arch Clin Exp Ophthalmol 255, 2081–2089 (2017). https://doi.org/10.1007/s00417-017-3747-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-017-3747-1