Abstract
Purpose
The aim of this study was to determine serum and aqueous xanthine oxidase (XO) levels, and mRNA expression in anterior lens epithelial cells in pseudoexfoliation (PEX).
Methods
In this prospective study, serum, aqueous and anterior lens capsules were taken from 21 patients with PEX and 23 normal subjects who had undergone routine cataract surgery. Serum and aqueous XO levels were analyzed using the colorimetric method. mRNA expression of XO in anterior lens epithelial cells was evaluated using reverse transcription polymerase chain reaction analysis.
Results
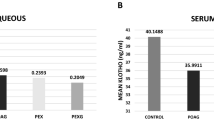
Serum XO levels (means ± standard deviations) were 207.0 ± 86.1 IU/mL and 240.6 ± 114.1 IU/mL in the normal and PEX groups, respectively (p = 0.310). Aqueous XO levels (means ± standard deviations) were 65.5 ± 54.3 IU/mL in the normal group and 130.5 ± 117.4 IU/mL in the PEX group (p = 0.028). There was a 2.9 fold decrease in mRNA expression in anterior lens epithelial cells of PEX, which is significantly lower than the normal group (p = 0.01).
Conclusions
Higher aqueous XO levels lacking associated different serum XO suggests higher oxidative stress in the aqueous. Higher aqueous XO levels in PEX with decreased mRNA expression in anterior lens epithelial cells indicate possible overexpression of XO in other structures related to the aqueous.


Similar content being viewed by others
References
Lindberg J (1917) Kliniska undersokningar over depigmentering av pupillarranden odr genomlysbarhet av iris vid fall av alderstarr samt i normala ogon hos gamla personer. Inaug Diss Helsingfors 18:87–89
Streeten BW, Li ZY, Wallace RN, Eagle RC Jr, Keshgegian AA (1992) Pseudoexfoliative fibrillopathy in visceral organs of a patient with pseudoexfoliation syndrome. Arch Ophthalmol 110(12):1757–1762
Yagci R, Ersoz I, Erdurmus M, Gurel A, Duman S (2008) Protein carbonyl levels in the aqueous humour and serum of patients with pseudoexfoliation syndrome. Eye (London) 22(1):128–131. doi:10.1038/sj.eye.6702751
Yagci R, Gurel A, Ersoz I, Karadag R, Hepsen IF, Duman S (2009) The activities of paraoxonase, xanthine oxidase, adenosine deaminase and the level of nitrite in pseudoexfoliation syndrome. Ophthalmic Res 42(3):155–159. doi:10.1159/000229306
Tosun M, Erdurmus M, Bugdayci G, Celebi S, Alcelik A (2012) Aqueous humour and serum concentration of asymmetric dimethyl arginine in pseudoexfoliation syndrome. Br J Ophthalmol 96(8):1137–1140. doi:10.1136/bjophthalmol-2012-301901
Selin JZ, Lindblad BE, Rautiainen S, Michaelsson K, Morgenstern R, Bottai M, Basu S, Wolk A (2014) Are increased levels of systemic oxidative stress and inflammation associated with age-related cataract? Antioxid Redox Signal 21(5):700–704. doi:10.1089/ars.2014.5853
Ugurlu N, Asik MD, Yulek F, Neselioglu S, Cagil N (2013) Oxidative stress and anti-oxidative defence in patients with age-related macular degeneration. Curr Eye Res 38(4):497–502. doi:10.3109/02713683.2013.774023
Harman D (1993) Free radical involvement in aging. Pathophysiology and therapeutic implications. Drugs Aging 3(1):60–80
Goyal A, Srivastava A, Sihota R, Kaur J (2014) Evaluation of oxidative stress markers in aqueous humor of primary open angle glaucoma and primary angle closure glaucoma patients. Curr Eye Res 39(8):823–829. doi:10.3109/02713683.2011.556299
Turk A, Aykut M, Akyol N, Kola M, Mentese A, Sumer A, Alver A, Erdol H (2014) Serum anti-carbonic anhydrase antibodies and oxidant-antioxidant balance in patients with acute anterior uveitis. Ocul Immunol Inflamm 22(2):127–132. doi:10.3109/09273948.2013.830753
Parks DA, Granger DN (1986) Xanthine oxidase: biochemistry, distribution and physiology. Acta Physiol Scand Suppl 548:87–99
Malik UZ, Hundley NJ, Romero G, Radi R, Freeman BA, Tarpey MM, Kelley EE (2011) Febuxostat inhibition of endothelial-bound XO: implications for targeting vascular ROS production. Free Radic Biol Med 51(1):179–184. doi:10.1016/j.freeradbiomed.2011.04.004
George J, Struthers AD (2009) Role of urate, xanthine oxidase and the effects of allopurinol in vascular oxidative stress. Vasc Health Risk Manag 5(1):265–272
Helbig H, Schlotzer-Schrehardt U, Noske W, Kellner U, Foerster MH, Naumann GO (1994) Anterior-chamber hypoxia and iris vasculopathy in pseudoexfoliation syndrome. Ger J Ophthalmol 3(3):148–153
Newaz MA, Yousefipour Z, Oyekan A (2006) Oxidative stress-associated vascular aging is xanthine oxidase-dependent but not NAD(P)H oxidase-dependent. J Cardiovasc Pharmacol 48(3):88–94. doi:10.1097/01.fjc.0000245402.62864.0a
Naji M, Naji F, Suran D, Gracner T, Kanic V, Pahor D (2008) Systemic endothelial dysfunction in patients with pseudoexfoliation syndrome. Klin Monatsbl Augenheilkd 225(11):963–967. doi:10.1055/s-2008-1027633
Atalar PT, Atalar E, Kilic H, Abbasoglu OE, Ozer N, Aksoyek S, Ovunc K, Ozmen F, Gursel E (2006) Impaired systemic endothelial function in patients with pseudoexfoliation syndrome. Int Heart J 47(1):77–84
Berry CE, Hare JM (2004) Xanthine oxidoreductase and cardiovascular disease: molecular mechanisms and pathophysiological implications. J Physiol 555(Pt 3):589–606. doi:10.1113/jphysiol.2003.055913
Yildirim Z, Yildirim F, Ucgun NI, Sepici-Dincel A (2013) The role of the cytokines in the pathogenesis of pseudoexfoliation syndrome. Int J Ophthalmol 6(1):50–53. doi:10.3980/j.issn.2222-3959.2013.01.10
Uysal S, Unal ZN, Erdogan S, Akyol S, Ramazan Yigitoglu M, Hirohata S, Isik B, Demircan K (2013) Augmentation of ADAMTS9 gene expression by IL-1beta is reversed by NFkappaB and MAPK inhibitors, but not PI3 kinase inhibitors. Cell Biochem Funct 31(7):539–544. doi:10.1002/cbf.2932
Strzalka-Mrozik B, Prudlo L, Kimsa MW, Kimsa MC, Kapral M, Nita M, Mazurek U (2013) Quantitative analysis of SOD2, ALDH1A1 and MGST1 messenger ribonucleic acid in anterior lens epithelium of patients with pseudoexfoliation syndrome. Mol Vis 19:1341–1349
Zoric L, Miric D, Milenkovic S, Jovanovic P, Trajkovic G (2006) Pseudoexfoliation syndrome and its antioxidative protection deficiency as risk factors for age-related cataract. Eur J Ophthalmol 16(2):268–273
Tosun M, Yagci R, Erdurmus M (2014) Glaucoma and antioxidant status. In: Preedy VR (ed) Handbook of nutrition, diet and the eye, 1st edn. Elsevier, Whaltam, pp 87–96
Guerciolini R, Szumlanski C, Weinshilboum RM (1991) Human liver xanthine oxidase: nature and extent of individual variation. Clin Pharmacol Ther 50(6):663–672
Relling MV, Lin JS, Ayers GD, Evans WE (1992) Racial and gender differences in N-acetyltransferase, xanthine oxidase, and CYP1A2 activities. Clin Pharmacol Ther 52(6):643–658
Aklillu E, Carrillo JA, Makonnen E, Bertilsson L, Ingelman-Sundberg M (2003) Xanthine oxidase activity is influenced by environmental factors in Ethiopians. Eur J Clin Pharmacol 59(7):533–536. doi:10.1007/s00228-003-0653-8
Begas E, Kouvaras E, Tsakalof A, Papakosta S, Asprodini EK (2007) In vivo evaluation of CYP1A2, CYP2A6, NAT-2 and xanthine oxidase activities in a Greek population sample by the RP-HPLC monitoring of caffeine metabolic ratios. Biomed Chromatogr 21(2):190–200. doi:10.1002/bmc.736
Zimmermann N, Wunscher M, Schlotzer-Schrehardt U, Erb C (2014) Corneal endothelial cell density and its correlation with the severity of pseudoexfoliation. Klin Monatsbl Augenheilkd 231(2):158–163. doi:10.1055/s-0033-1360308
Koliakos GG, Schlotzer-Schrehardt U, Konstas AG, Bufidis T, Georgiadis N, Dimitriadou A (2001) Transforming and insulin-like growth factors in the aqueous humour of patients with exfoliation syndrome. Graefes Arch Clin Exp Ophthalmol 239(7):482–487
Schlotzer-Schrehardt U, Zenkel M, Kuchle M, Sakai LY, Naumann GO (2001) Role of transforming growth factor-beta1 and its latent form binding protein in pseudoexfoliation syndrome. Exp Eye Res 73(6):765–780. doi:10.1006/exer.2001.1084
Doehner W, Anker SD (2005) Uric acid in chronic heart failure. Semin Nephrol 25(1):61–66
Mancino R, Di Pierro D, Varesi C, Cerulli A, Feraco A, Cedrone C, Pinazo-Duran MD, Coletta M, Nucci C (2011) Lipid peroxidation and total antioxidant capacity in vitreous, aqueous humor, and blood samples from patients with diabetic retinopathy. Mol Vis 17:1298–1304
Kinsey VE (1947) Transfer of ascorbic acid and related compounds across the blood-aqueous barrier. Am J Ophthalmol 30(10):1262–1266
Diehn JJ, Diehn M, Marmor MF, Brown PO (2005) Differential gene expression in anatomical compartments of the human eye. Genome Biol 6(9):R74. doi:10.1186/gb-2005-6-9-r74
Zenkel M, Poschl E, von der Mark K, Hofmann-Rummelt C, Naumann GO, Kruse FE, Schlotzer-Schrehardt U (2005) Differential gene expression in pseudoexfoliation syndrome. Invest Ophthalmol Vis Sci 46(10):3742–3752. doi:10.1167/iovs.05-0249
Gonen T, Gonen KA, Guzel S (2014) What is the effect of pseudoexfoliation syndrome on renal function in patients without glaucoma? Curr Eye Res 39(2):188–193. doi:10.3109/02713683.2013.834940
Disclosures
None.
Conflict of interest
All authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Simavli, H., Tosun, M., Bucak, Y.Y. et al. Serum and aqueous xanthine oxidase levels, and mRNA expression in anterior lens epithelial cells in pseudoexfoliation. Graefes Arch Clin Exp Ophthalmol 253, 1161–1167 (2015). https://doi.org/10.1007/s00417-015-3043-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-015-3043-x