Abstract
Background
To report the incidence, clinical presentation, and surgical outcomes of retinal detachment in highly myopic patients corrected by implantation of phakic intraocular lenses (PIOLs).
Methods
This is a retrospective interventional non-comparative case series. A total of 530 highly myopic eyes that underwent PIOLs implantation were included in the study. All patients completed at least a 2-year follow-up after PIOL implantation. The incidence of retinal detachment (RD) and subsequent treatments were reviewed. The refractive errors, axial lengths, time between refractive surgery and RD detection, vitreoretinal findings, rate of retinal reattachment, and the pre- and postoperative best-corrected visual acuity (BCVA) were analyzed.
Results
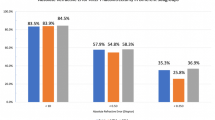
The overall incidence of RD was 1.5 % (eight eyes of seven patients) with a mean time between PIOL implantation and detachment of 23.63 ± 18.12 months (range, 2 days–51 months). Mean spherical equivalent (SE) before PIOL implantation was −17.53 ± 3.86 diopters (D) (range, −11.5D to −23.5D). Six patients underwent bilateral PIOL implantation. Five eyes were implanted with anterior chamber PIOLs and the other three received posterior chamber PIOLs. A traumatic history was presented before RD detection in four cases. Horseshoe tears, atrophic holes, or giant retinal tears were found in four (50 %), two (25 %), and two (25 %) eyes, respectively. Two eyes (25 %) underwent scleral buckling surgery, five eyes (62.5 %) underwent pars plana vitrectomy surgery, and one eye (12.5 %) underwent both procedures. Anatomical retinal attachment was achieved after first RD surgery in seven eyes. Mean BCVA after PIOL implantation and before RD was 20/40 (decimal refraction, 0.51 ± 0.31) compared to that of 20/80 (decimal refraction, 0.26 ± 0.12) after the RD surgery. Mean follow-up after RD surgery was 20.63 ± 12.93 months (range, 8–42 months).
Conclusions
The incidence of RD after PIOLs implantation is low. Its characteristics do not differ significantly from the natural history of RD in high myopic eyes. PIOL implantation for surgical correction of severe myopia does not seem to increase the risk of RD. Good visual prognosis can be obtained with early surgical intervention.
Similar content being viewed by others
References
Lackner B, Pieh S, Schmidinger G, Hanselmayer G, Dejaco-Ruhswurm I, Funovics MA, Skorpik C (2003) Outcome after treatment of ametropia with implantable contact lenses. Ophthalmology 110:2153–2161
Sanders DR, Vukich JA, Doney K, Gaston M, Implantable Contact Lens in Treatment of Myopia Study Group (2003) U.S. Food and Drug Administration clinical trial of the Implantable Contact Lens for moderate to high myopia. Ophthalmology 110:255–266
Petternel V, Köppl CM, Dejaco-Ruhswurm I, Findl O, Skorpik C, Drexler W (2004) Effect of accommodation and pupil size on the movement of a posterior chamber lens in the phakic eye. Ophthalmology 111:325–331
Sanders DR (2003) Postoperative inflammation after implantation of the implantable contact lens. Ophthalmology 110:2335–2341
García-Feijoó J, Hernández-Matamoros JL, Méndez-Hernández C, Castillo-Gómez A, Lázaro C, Martín T, Cuiña-Sardiña R, García-Sánchez J (2003) Ultrasound biomicroscopy of silicone posterior chamber phakic intraocular lens for myopia. J Cataract Refract Surg 29:1932–1939
Brauweiler PH, Wehler T, Busin M (1999) High incidence of cataract formation after implantation of a silicone posterior chamber lens in phakic, highly myopic eyes. Ophthalmology 106:1651–1655
Brandt JD, Mockovak ME, Chayet A (2001) Pigmentary dispersion syndrome induced by a posterior chamber phakic refractive lens. Am J Ophthalmol 131:260–263
Jiménez-Alfaro I, Benítez del Castillo JM, García-Feijoó J, Gil de Bernabé JG, Serrano de La Iglesia JM (2001) Safety of posterior chamber phakic intraocular lenses for the correction of high myopia: anterior segment changes after posterior chamber phakic intraocular lens implantation. Ophthalmology 108:90–99
Arne JL, Lesueur LC (2000) Phakic posterior chamber lenses for high myopia: functional and anatomical outcome. J Cataract Refr Surg 26:369–374
Qasem Q, Kirwan C, O’Keefe M (2010) 5-Year prospective follow-up of artisan phakic intraocular lenses for the correction of myopia, hyperopia and astigmatism. Ophthalmologica 224:283–290
Daniel HC, Elizabeth AD (2006) Phakic intraocular lenses. Curr Opin Ophthalmol 17:99–104
Baikoff G (1991) Phakic anterior chamber intraocular lenses. Int Ophthalmology Clin 31:75–86
Ruiz-Moreno JM, Alió JL, Pérez-Santonja JJ, de la Hoz F (1999) Retinal detachment in phakic eyes with anterior chamber lenses to correct severe myopia. Am J Ophthalmol 127:270–275
Ruiz-Moreno JM, Montero JA, de la Vega C, Alió JL, Zapater P (2006) Retinal detachment in myopic eyes after phakic intraocular lens implantation. J Refract Surg 22:247–252
Martínez-Castillo V, Boixadera A, Verdugo A, Elíes D, Coret A, García-Arumí J (2005) Rhegmatogenous retinal detachment in phakic eyes after posterior chamber phakic intraocular lens implantation for severe myopia. Ophthalmology 112:580–585
Rizzo S, Belting C, Genovesi-Ebert F (2003) Two cases of giant retinal tear after implantation of a phakic intraocular lens. Retina 23:411–413
Freeman HM (2001) Fellow eye of non-traumatic giant retinal breaks. In: Ryan SJ (ed) Retina. St. Louis, Mo, Mosby, pp 2366–2370
Melberg NS, Thomas MA (1995) Nuclear sclerotic cataract after vitrectomy in patients younger than 50years of age. Ophthalmology 102:1466–1471
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jiang, T., Chang, Q., Wang, X. et al. Retinal detachment after phakic intraocular lens implantation in severe myopic eyes. Graefes Arch Clin Exp Ophthalmol 250, 1725–1730 (2012). https://doi.org/10.1007/s00417-012-2002-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-012-2002-z