Abstract
Purpose
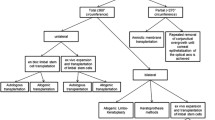
To evaluate the long-term results of keratolimbal allograft (KLAL) and elucidate the prognostic factors of KLAL survival.
Methods
Twenty-four eyes of 22 patients underwent KLAL one or more times, and were followed up more than 1 year postoperatively. Their medical records were reviewed. The success of KLAL and penetrating keratoplasty (PKP) was evaluated. KLAL success was defined as absence of persistent corneal epithelial defect, corneal conjunctivalization, or neovascularization on the corneal edge of the graft. Prognostic factors for survival of KLAL were analyzed, including preoperative diagnosis, history of graft rejection, symblepharon, concurrent surgery, immunosuppressant dose, and interval for full epithelialization time. The prognostic factors were evaluated by univariate survival analysis or multivariate Cox proportional hazards survival regression.
Results
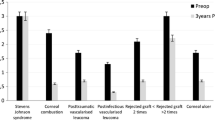
KLAL had been successful in 33.3% of the eyes over an average of 47.9 months. Fifteen episodes of KLAL rejection developed in ten eyes (41.7%), but 13 cases (86.7%) were reversible. Of 45 KLAL procedures, eyelid deformity, symblepharon, and the interval of full epithelialization were significantly associated with KLAL success by univariate analysis, and the presence of symblepharon was identified by multivariate Cox regression analysis as the most important prognostic factor to affect KLAL outcome (p = 0.010).
Conclusions
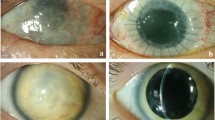
KLAL has been partly successful for reconstruction of limbal stem cell deficiency, and symblepharon has been identified as a significant prognostic factor for KLAL survival. Surgical correction of symblepharon is important before KLAL and PKP.



Similar content being viewed by others
References
Thoft RA (1989) The role of the limbus in ocular surface maintenance and repair. Acta Ophthalmol Suppl 192:91–94
Tsai RJ, Tseng SC (1994) Human allograft limbal transplantation for corneal surface reconstruction. Cornea 13:389–400
Tan DT, Ficker LA, Buckley RJ (1996) Limbal transplantation. Ophthalmology 103:29–36
Tsubota K, Toda I, Saito H, Shinozaki N, Shimazaki J (1995) Reconstruction of the corneal epithelium by limbal allograft transplantation for severe ocular surface disorders. Ophthalmology 102:1486–1496
Tsubota K, Satake Y, Ohyama M, Toda I, Takano Y, Ono M, Shinozaki N, Shimazaki J (1996) Surgical reconstruction of the ocular surface in advanced ocular cicatricial pemphigoid and Stevens–Johnson syndrome. Am J Ophthalmol 122:38–52
Solomon A, Ellies P, Anderson DF, Touhami A, Grueterich M, Espana EM, Ti SE, Goto E, Feuer WJ, Tseng SC (2002) Long-term outcome of keratolimbal allograft with or without penetrating keratoplasty for total limbal stem cell deficiency. Ophthalmology 109:1159–1166
Ilari L, Daya SM (2002) Long-term outcomes of keratolimbal allograft for the treatment of severe ocular surface disorders. Ophthalmology 109:1278–1284
Maruyama-Hosoi F, Shimazaki J, Shimmura S, Tsubota K (2006) Changes observed in keratolimbal allograft. Cornea 25:377–382
Samson CM, Nduaguba C, Baltatzis S, Foster CS (2002) Limbal stem cell transplantation in chronic inflammatory eye disease. Ophthalmology 109:862–868
Liang L, Sheha H, Tseng SC (2009) Long-term outcomes of keratolimbal allograft for total limbal stem cell deficiency using combined immunosuppressive agents and correction of ocular surface deficits. Arch Ophthalmol 127:1428–1434
Shimazaki J, Shimmura S, Fujishima H, Tsubota K (2000) Association of preoperative tear function with surgical outcome in severe Stevens–Johnson syndrome. Ophthalmology 107:1518–1523
Han ES, Wee WR, Lee JH, Kim MK (2007) The long-term safety of donor eye for 180 degrees limbal transplantation. Graefes Arch Clin Exp Ophthalmol 245:745–748
Kenyon KR, Tseng SC (1989) Limbal autograft transplantation for ocular surface disorders. Ophthalmology 96:709–722, discussion 722–703
Tsubota K, Satake Y, Kaido M, Shinozaki N, Shimmura S, Bissen-Miyajima H, Shimazaki J (1999) Treatment of severe ocular-surface disorders with corneal epithelial stem-cell transplantation. N Engl J Med 340:1697–1703
Ukponmwan CU, Njinaka I, Ehimiyen ET (2010) Ocular complications of Stevens–Johnson syndrome and toxic epidermal necrolysis. Trop Doct 40:167–168
De Rojas MV, Dart JK, Saw VP (2007) The natural history of Stevens–Johnson syndrome: patterns of chronic ocular disease and the role of systemic immunosuppressive therapy. Br J Ophthalmol 91:1048–1053
Vajpayee RB, Sharma N, Sinha R, Agarwal T, Singhvi A (2007) Infectious keratitis following keratoplasty. Surv Ophthalmol 52:1–12
Hohage H, Welling U, Zeh M, Gerhardt U, Suwelack B (2005) Switching immunosuppression from cyclosporine to tacrolimus improves long-term kidney function: a 6-year study. Transplant Proc 37:1898–1899
Filler G, Webb NJ, Milford DV, Watson AR, Gellermann J, Tyden G, Grenda R, Vondrak K, Hughes D, Offner G, Griebel M, Brekke IB, McGraw M, Balzar E, Friman S, Trompeter R (2005) Four-year data after pediatric renal transplantation: a randomized trial of tacrolimus vs. cyclosporin microemulsion. Pediatr Transplant 9:498–503
Margreiter R (2002) Efficacy and safety of tacrolimus compared with ciclosporin microemulsion in renal transplantation: a randomised multicentre study. Lancet 359:741–746
Briggs D, Dudley C, Pattison J, Pfeffer P, Salmela K, Rowe P, Tyden G (2003) Effects of immediate switch from cyclosporine microemulsion to tacrolimus at first acute rejection in renal allograft recipients. Transplantation 75:2058–2063
Holland EJ (1996) Epithelial transplantation for the management of severe ocular surface disease. Trans Am Ophthalmol Soc 94:677–743
Holland EJ, Schwartz GS (1996) The evolution of epithelial transplantation for severe ocular surface disease and a proposed classification system. Cornea 15:549–556
DeSousa JL, Daya S, Malhotra R (2009) Adnexal surgery in patients undergoing ocular surface stem cell transplantation. Ophthalmology 116:235–242
Kheirkhah A, Blanco G, Casas V, Hayashida Y, Raju VK, Tseng SC (2008) Surgical strategies for fornix reconstruction based on symblepharon severity. Am J Ophthalmol 146:266–275
Acknowledgement
There was no government and non-government support. The authors have no financial or other proprietary interest in any material or method mentioned in this article.
Author information
Authors and Affiliations
Corresponding author
Additional information
Commercial interest or financial relationship: none
We have full control of all primary data, and we agree to allow Graefe's Archive for Clinical and Experimental Ophthalmology to review our data upon request.
Institutional review board (H-1006-143-322).
Rights and permissions
About this article
Cite this article
Han, E.S., Wee, W.R., Lee, J.H. et al. Long-term outcome and prognostic factor analysis for keratolimbal allografts. Graefes Arch Clin Exp Ophthalmol 249, 1697–1704 (2011). https://doi.org/10.1007/s00417-011-1760-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-011-1760-3