Abstract
Background
Bacterial endophthalmitis is a serious complication of penetrating ocular trauma and cataract surgery. The purpose of this study is to assess the ability of an anterior chamber air bubble to prevent experimental Staphylococcus epidermidis endophthalmitis.
Methods
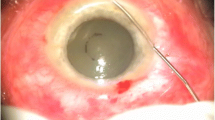
The anterior chamber was opened with a clear corneal incision to drain the aqueous humor in one eye of 24 rabbits. S. epidermidis was injected into the anterior chamber. The infected rabbits were randomly divided into two groups. Animals in group 1 (n = 12) received an air bubble to reconstruct the anterior chamber, and animals in Group 2 (n = 12) received Balanced Salt Solution (BSS) for reconstruction. Clinical examination in each group was performed 2, 3 and 7 days after inoculation of the bacteria. Clinical examination scores were recorded. All eyes were enucleated for histophatological examination.
Results
Clinical endophthalmitis was seen in 7/12 (58.3%) in group 2, but in only 1/12 (8.3%) in group 1 (p = 0.027). Mean clinical scores of groups 1and 2 on the 3rd day were 2.6 ± 1.4 and 7.2 ± 1.7 respectively. (p < 0.001). The mean clinical scores of groups 1and 2 on the 7th day were 2.3 ± 1.2 and 6.8 ± 1.5 respectively (p < 0.001). Histopathological examination confirmed clinical findings.
Conclusion
An air bubble in the anterior chamber may have protective effects against the development of experimental S. epidermidis endophthalmitis.


Similar content being viewed by others
References
Ellis MF (2003) Topical anaesthesia: a risk factor for postcataract-extraction endophthalmitis? Clin Experiment Ophthalmol 31:125–128
Lemley CA, Han DP (2007) Endophthalmitis: a review of current evaluation and management. Retina 27:662–680
Clark A, Ng JQ, Morlet N, Tropiano E, Mahendran P, Spilsbury K, Preen D, Semmens JB (2008) Quality of life after postoperative endophthalmitis. Clin Experiment Ophthalmol 36(6):526–531
Morlet N, Li J, Semmens J, Ng J, teamEPSWA (2003) The Endophthalmitis Population Study of Western Australia (EPSWA): first report. Br J Ophthalmol 87:574–576
Ng JQ, Morlet N, Bremner AP, Bulsara MK, Morton AP, Semmens JB (2008) Techniques to monitor for endophthalmitis and other cataract surgery complications. Ophthalmology 115(1):3–10
Yu-Wai-Man P, Morgan SJ, Hildreth AJ, Steel DH, Allen D (2008) Efficacy of intracameral and subconjunctival cefuroxime in preventing endophthalmitis after cataract surgery. J Cataract Refract Surg 34(3):447–451
Buzard K, Liapis S (2004) Prevention of endophthalmitis. J Cataract Refract Surg 30(9):1953–1959
Sim DA, Wong R, Griffiths MF (2007) Injecting an air bubble at the end of sutureless cataract surgery to prevent inflow of ocular surface fluid. Eye 21(11):1444–1445
Peyman GA, Paque JT, Meisels HI, Bennett TO (1975) Postoperative endophthalmitis: A comparison of methods for treatment and prophylaxis with gentamicin. Ophthalm Surg 6:45–55
Liu SM, Way T, Rodrigues M, Steidl SM (2000) Effects of intravitreal corticosteroids in the treatment of Bacillus cereus endophthalmitis. Arch Ophthalmol 118:803–806
Lalwani GA, Flynn HW Jr, Scott IU, Quinn CM, Berrocal AM, Davis JL, Murray TG, Smiddy WE, Miller D (2008) Acute-onset endophthalmitis after clear corneal cataract surgery (1996–2005). Clinical features, causative organisms, and visual acuity outcomes. Ophthalmology 115(3):473–476
Schein OD (2007) Prevention of endophthalmitis after cataract surgery: making the most of the evidence. Ophthalmology 114(5):831–832
Wejde G, Samolov B, Seregard S, Koranyi G, Montan PG (2005) Risk factors for endophthalmitis following cataract surgery: a retrospective case-control study. J Hosp Infect 61(3):251–256
Pleyer U, Mondino BJ, Adamu SA, Pitchekian-Halabi H, Engstrom RE, Glasgow BJ (1992) Immune response to Staphylococcus epidermidis-induced endophthalmitis in a rabbit model. Invest Ophthalmol Vis Sci 33(9):2650–2663
Callegan MC, Gilmore MS, Gregory M, Ramadan RT, Wiskur BJ, Moyer AL, Hunt JJ, Novosad BD (2007) Bacterial endophthalmitis: therapeutic challenges and host-pathogen interactions. Prog Retin Eye Res 26(2):189–203
Giese MJ, Shum DC, Rayner SA, Mondino BJ, Berliner JA (2000) Adhesion molecule expression in a rat model of Staphylococcus aureus dophthalmitis. Invest Ophthalmol Vis Sci 41(1):145–153
Persson M, Svenarud P, Flock JI, van der Linden J (2005) Carbon dioxide inhibits the growth rate of Staphylococcus aureus at body temperature. Surg Endosc 19(1):91–94
Baker RC, Qureshi RA, Hotchkiss JH (1986) Effect of an elevated level of carbon dioxide containing atmosphere on the growth of spoilage and pathogenic bacteria at 2, 7, and 13 C. Poult Sci 65(4):729–737
Muhvich KH, Park MK, Myers RA, Marzella L (1989) Hyperoxia and the antimicrobial susceptibility of Escherichia coli and Pseudomonas aeruginosa. Antimicrob Agents Chemother 33(9):1526–1530
Keck PE, Gottlieb SF, Conley J (1980) Interaction of increased pressures of oxygen and sulfonamides on the in vitro and in vivo growth of pathogenic bacteria. Undersea Biomed Res 7(2):95–106
Liesegang TJ, Skuta GL, Cantor LB (2007) American Academy of Ophthalmology Basic and Clinical Science Course: Section 9, Intraocular Inflammation and Uveitis. Saunders, Philadelphia, pp 80–85
Olson RJ (1980) Air and the corneal endothelium: an in vivo specular microscopy study in cats. Arch Ophthalmol 98(7):1283–1284
Van Horn DL, Edelhauser HF, Aaberg TM, Pederson HJ (1972) In vivo effects of air and sulfur hexafluoride gas on rabbit corneal endothelium. Invest Ophthalmol 11(12):1028–1036
Norn MS (1975) Corneal thickness after cataract extraction with air in the anterior chamber. Acta Ophthalmol (Copenh) 53(5):747–750
Acknowledgment
Appreciation is expressed to the staff of the Animal Laboratory of the Shiraz University of Medical Sciences for their generous assistance, and to K. Shashok (AuthorAID in the Eastern Mediterranean) for improving the use of English in the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
No authors have any financial/conflicting interests to disclose. The authors alone are responsible for the content and writing of the paper.
Rights and permissions
About this article
Cite this article
Mehdizadeh, M., Rahat, F., Khalili, M.R. et al. Effect of anterior chamber air bubble on prevention of experimental Staphylococcus epidermidis endophthalmitis. Graefes Arch Clin Exp Ophthalmol 248, 277–281 (2010). https://doi.org/10.1007/s00417-009-1173-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-009-1173-8