Abstract
Objective
A significant proportion of patients with behavioural variant frontotemporal dementia (bvFTD) show memory impairments similar to patients with Alzheimer’s disease (AD), making them prone to misdiagnosis in early disease stages. Our objective was to establish a rapid and efficient memory measure that enhances discrimination between patients with dementia due to Alzheimer’s disease and amnestic presentations of behavioural variant frontotemporal dementia.
Method
Word list learning data of patients with diagnoses of AD and both amnestic and non-amnestic presentations of bvFTD were analysed. The overall recall rate and the relative contributions of the first two (primacy items) and last two words (recency items) to recall performance were compared between groups.
Results
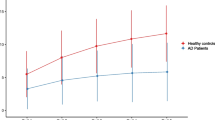
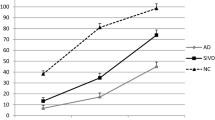
Overall recall rate was indistinguishable between patients with AD and amnestic bvFTD. However, AD patients’ recall was mostly driven by recency items, whereas amnestic bvFTD patients’ performance was mostly driven by primacy items.
Conclusion
We conclude that obtaining a simple recency dominance index from a single, 15-item word list memory trial can help discriminate patients with AD from patients with bvFTD, even if they present with similarly severe memory impairment.


Similar content being viewed by others
References
Hogan DB, Jetté N, Fiest KM et al (2016) The prevalence and incidence of frontotemporal dementia: a systematic review. Can J Neurol Sci 43:S96–S109. https://doi.org/10.1017/cjn.2016.25
Hornberger M, Piguet O (2012) Episodic memory in frontotemporal dementia : a critical review. Brain 135:678–692. https://doi.org/10.1093/brain/aws011
Reul S, Lohmann H, Wiendl H et al (2017) Can cognitive assessment really discriminate early stages of Alzheimer’s and behavioural variant frontotemporal dementia at initial clinical presentation? Alzheimer’s Res Ther 9:1–12. https://doi.org/10.1186/s13195-017-0287-1
Weiner MW, Veitch DP, Aisen PS et al (2015) 2014 Update of the Alzheimer’s Disease Neuroimaging Initiative: a review of papers published since its inception. Alzheimers Dement 11:e1–e120. https://doi.org/10.1016/j.jalz.2014.11.001
Rascovsky K, Hodges J, Knopman D et al (2011) Sensitivity of revised diagnostic criteria for the behavioural variant of frontotemporal dementia. Brain 134:2456–2477. https://doi.org/10.17925/ENR.2011.06.04.234
Johnen A, Bertoux M (2019) Psychological and cognitive markers of behavioral variant frontotemporal dementia—a Clinical Neuropsychologist’s view on diagnostic criteria and beyond. Front Neurol. https://doi.org/10.3389/fneur.2019.00594
Bertoux M, Cruz De Souza L, Corlier F et al (2014) Two distinct amnesic profiles in behavioral variant frontotemporal dementia. Biol Psychiatry 75:582–588. https://doi.org/http://dx.doi.org/10.1016/j.biopsych.2013.08.017
Fernández-Matarrubia M, Matías-Guiu JJL, Cabrera-Martín MN et al (2017) Episodic memory dysfunction in behavioral variant frontotemporal dementia: a clinical and FDG-PET study. J Alzheimer’s Dis 57:1251–1264. https://doi.org/10.3233/jad-160874
Hornberger M, Piguet O, Graham AJ et al (2010) How preserved is episodic memory in behavioral variant frontotemporal dementia? Neurology 74:472–479. https://doi.org/10.1212/WNL.0b013e3181cef85d
Mahoney CJ, Beck J, Rohrer JD et al (2012) Frontotemporal dementia with the C9ORF72 hexanucleotide repeat expansion: clinical, neuroanatomical and neuropathological features. Brain 135:736–750. https://doi.org/10.1093/brain/awr361
Ranasinghe KG, Rankin KP, Pressman PS et al (2016) Distinct subtypes of behavioral variant frontotemporal dementia based on patterns of network degeneration. JAMA Neurol 73:1078–1088. https://doi.org/10.1001/jamaneurol.2016.2016
Grober E, Buschke H, Crystal H et al (1988) Screening for dementia by memory testing. Neurology 38:900–903. https://doi.org/10.1212/wnl.38.6.900
Bertoux M, Ramanan S, Slachevsky A et al (2016) So close yet so far: executive contribution to memory processing in behavioral variant frontotemporal dementia. J Alzheimer’s Dis 54:1005–1014. https://doi.org/10.3233/JAD-160522
Ebbinghaus H (1885) Über das Gedächtnis: Untersuchungen zur Experimentellen Psycholotie. Verlag von Duncker & Humblot, Leipzig
Carlesimo GA, Sabbadini M, Fadda L, Caltagirone C (1995) Different components in word-list forgetting of pure amnesics, degenerative demented and healthy subjects. Cortex 31:735–745. https://doi.org/10.1016/S0010-9452(13)80024-X
Foldi NS, Brickman AM, Schaefer LA, Knutelska ME (2003) Distinct serial position profiles and neuropsychological measures differentiate late life depression from normal aging and Alzheimer’s disease. Psychiatry Res 120:71–84. https://doi.org/10.1016/S0165-1781(03)00163-X
McKhann GM, Knopman DS, Chertkow H et al (2011) The diagnosis of dementia due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement 7:263–269. https://doi.org/10.1016/j.jalz.2011.03.005
Kertesz A, Davidson W, Fox H (1997) Frontal Behavioral Inventory: Diagnostic Criteria for Frontal Lobe Dementi. Can J Neurol Sci / J Can des Sci Neurol 24:29–36. https://doi.org/10.1017/s0317167100021053
Helmstaedter C, Lendt M, Lux S (2001) Verbaler Lern- und Merkfähigkeitstest: Manual. Beltz Test
Rey A (1958) Memorisation d’une serie de 15 mots en 5 répétitions. In: Presses Universitaires de France (ed) Léxamen clinique en psychologie. Paris, pp 26–42
Strange BA, Otten LJ, Josephs O et al (2002) Dissociable human perirhinal, hippocampal, and parahippocampal roles during verbal encoding. J Neurosci 22:523–528. https://doi.org/10.1523/jneurosci.22-02-00523.2002
Talmi D, Grady CL, Goshen-Gottstein Y, Moscovitch M (2005) Neuroimaging the serial position curve. Psychol Sci 16:716–723
Youden WJ (1950) An index for rating diagnostic tests. Cancer 3:32–35
La Rue A, La HB, Jones JE et al (2008) Effect of parental family history of Alzheimer’s disease on serial position profiles. Alzheimers Dement 4:285–290. https://doi.org/10.1016/j.jalz.2008.03.009
Turchetta CS, Perri R, Fadda L et al (2018) Forgetting rate on the recency portion of a word list differentiates mild to moderate Alzheimer’s Disease from other forms of dementia. J Alzheimer’s Dis 66:461–470. https://doi.org/10.3233/JAD-180690
Atkinson, R. & Shiffrin R (1968) Human memory: a proposed system and its control processes. Psychol Learn Motiv 89–195
Baddeley A (2000) Short-term and working memory. In: Tulving E, Craik FIM (eds) The Oxford Handbook of Memory. Oxford University Press, New York, pp 77–92
Glanzer M, Cunitz AR (1966) Two storage mechanisms in free recall. J Verbal Learn Verbal Behav 5:351–368. https://doi.org/10.1016/S0079-7421(08)60441-7
Sarazin M, Chauviré V, Gerardin E et al (2010) The amnestic syndrome of hippocampal type in Alzheimer’s disease: an MRI study. J Alzheimer’s Dis 22:285–294. https://doi.org/10.3233/JAD-2010-091150
Frisch S, Dukart J, Vogt B et al (2013) Dissociating memory networks in early Alzheimer’s disease and frontotemporal lobar degeneration—a combined study of hypometabolism and atrophy. PLoS ONE 8:e55251. https://doi.org/10.1371/journal.pone.0055251
Graham A, Davies R, Xuereb J et al (2005) Pathologically proven frontotemporal dementia presenting with severe amnesia. Brain 128:597–605. https://doi.org/10.1093/brain/awh348
Irish M, Piguet O, Hodges JR, Hornberger M (2014) Common and unique gray matter correlates of episodic memory dysfunction in frontotemporal dementia and Alzheimer’s disease. Hum Brain Mapp 35:1422–1435. https://doi.org/10.1002/hbm.22263
Pennington C, Hodges JR, Hornberger M (2011) Neural correlates of episodic memory in behavioral variant frontotemporal dementia. J Alzheimers Dis 1:261–268. https://doi.org/10.3233/JHD-120029
De Souza LC, Chupin M, Bertoux M et al (2013) Is hippocampal volume a good marker to differentiate Alzheimer’s disease from frontotemporal dementia? J Alzheimers Dis 36:57–66. https://doi.org/10.3233/JAD-122293
Bertoux M, Flanagan EC, Hobbs M et al (2018) Structural anatomical investigation of long-term memory deficit in behavioral frontotemporal dementia. J Alzheimers Dis 62:1887–1900. https://doi.org/10.3233/JAD-170771
Wicklund AH, Johnson N, Rademaker A et al (2006) Word list versus story memory in Alzheimer disease and frontotemporal dementia. Alzheimer Dis Assoc Disord 20:86–92. https://doi.org/10.1097/01.wad.0000213811.97305.49
Hutchinson AD, Mathias JL (2007) Neuropsychological deficits in frontotemporal dementia and Alzheimer’s disease: a meta-analytic review. J Neurol Neurosurg Psychiatry 78:917–928. https://doi.org/10.1136/jnnp.2006.100669
Dodich A, Cerami C, Cappa SF et al (2018) Combined socio-behavioral evaluation improves the differential diagnosis between the behavioral variant of frontotemporal dementia and Alzheimer’s disease. in search of neuropsychological markers. J Alzheimers Dis 61:761–772. https://doi.org/10.3233/JAD-170650
Porto CS, Bahia VS, Brucki SMD et al (2008) Neuropsychological differences between frontotemporal lobar degeneration and Alzheimer’s disease. Dement Neuropsychol 2:223–227. https://doi.org/10.1590/s1980-57642009dn20300011
Johnen A, Frommeyer J, Modes F et al (2015) Dementia apraxia test (DATE): a brief tool to differentiate behavioral variant frontotemporal dementia from Alzheimer’s dementia based on apraxia profiles. J Alzheimers Dis 49:593–605. https://doi.org/10.3233/JAD-150447
Marczinski CA, Davidson W, Kertesz A (2004) A longitudinal study of behavior in frontotemporal dementia and primary progressive aphasia. Cogn Behav Neurol 17:185–90. https://doi.org/00146965-200412000-00001
Acknowledgements
We thank Angelina Höfig and Nils Kleine for their support with data acquisition. We are grateful to the patients and their carers who agreed to contribute data to this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Nadine Kloth reports no competing interests. Jolene Lemke reports no competing interests. Heinz Wiendl receives honoraria for acting as a member of Scientific Advisory Boards and as consultant for Biogen, Evgen, MedDay Pharmaceuticals, Merck Serono, Novartis, Roche Pharma AG, Sanofi-Genzyme, as well as speaker honoraria and travel support from Alexion, Biogen, Cognomed, F. Hoffmann-La Roche Ltd., Gemeinnützige Hertie-Stiftung, Merck Serono, Novartis, Roche Pharma AG, Sanofi-Genzyme, TEVA, and WebMD Global. Prof. Wiendl is acting as a paid consultant for Abbvie, Actelion, Biogen, IGES, Johnson & Johnson, Novartis, Roche, Sanofi-Genzyme, and the Swiss Multiple Sclerosis Society. His research is funded by the German Ministry for Education and Research (BMBF), Deutsche Forschungsgesellschaft (DFG), Else Kröner Fresenius Foundation, Fresenius Foundation, Hertie Foundation, NRW Ministry of Education and Research, Interdisciplinary Center for Clinical Studies (IZKF) Muenster and RE Children’s Foundation, Biogen GmbH, GlaxoSmithKline GmbH, Roche Pharma AG, Sanofi-Genzyme. Sven G. Meuth receives honoraria for lecturing, and travel expenses for attending meetings from Almirall, Amicus Therapeutics Germany, Bayer Health Care, Biogen, Celgene, Diamed, Genzyme, MedDay Pharmaceuticals, Merck Serono, Novartis, Novo Nordisk, ONO Pharma, Roche, Sanofi-Aventis, Chugai Pharma, QuintilesIMS and Teva. His research is funded by the German Ministry for Education and Research (BMBF), Deutsche Forschungsgemeinschaft (DFG), Else Kröner Fresenius Foundation, German Academic Exchange Service, Hertie Foundation, Interdisciplinary Center for Clinical Studies (IZKF) Muenster, German Foundation Neurology and Almirall, Amicus Therapeutics Germany, Biogen, Diamed, Fresenius Medical Care, Genzyme, HERZ Burgdorf, Merck Serono, Novartis, ONO Pharma, Roche, and Teva. Thomas Duning received honoraria and travel expenses from Genzyme, Shire, Bristol-Myers Squibb, Boehringer-Ingelheim Pharma, Sanofi Aventis, Eisai, Novartis, Bayer Vital, Merz Pharma, Actelion, Amicus for serving as a speaker and consultant. He received research support from Genzyme, Shire, Amicus and Actelion. For conducting of studies on dementia, he received grants from Novartis, Merz Pharma, Roche and Biogen. Andreas Johnen received honoraria and travel expenses for acting as a speaker for Actelion Pharmaceuticals and Biogen unrelated to the content of this study.
Ethical standards
The study was conducted at the Department of Neurology of the University Hospital Muenster and was approved by the ethics committee of the regional Medical Association (Ärztekammer Westfalen-Lippe, 2012-365-f-S).
Informed consent
All participants gave written informed consent.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kloth, N., Lemke, J., Wiendl, H. et al. Serial position effects rapidly distinguish Alzheimer’s from frontotemporal dementia. J Neurol 267, 975–983 (2020). https://doi.org/10.1007/s00415-019-09662-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-019-09662-w