Abstract
Introduction
PCT is used in the diagnosis of acute neurological syndromes, particularly stroke. We aimed to evaluate PCT abnormalities in patients with acute epileptic seizures or status epilepticus (SE).
Methods
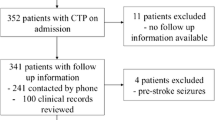
We collected patients undergoing acute PCT for the suspicion of acute ischemic stroke (AIS), who received a final diagnosis of focal seizures or generalised seizures with a post-ictal deficit, with or without concomitant AIS. PCTs were retrospectively analysed for the presence of hyper- and hypoperfusion, and results correlated with delay from seizure onset, aetiology, type of seizures and the presence of electrical SE.
Results
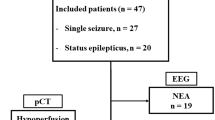
Half of the 43 consecutively identified patients had regional PCT abnormalities—hyperperfusion in 13 (30%) and hypoperfusion in 8 (19%)—and 4 (9%) had AIS. Among patients with hyperperfusion, six (46%) had a focal deficit during imaging acquisition (two a normal clinical status, one altered consciousness and four ongoing seizure); nine (69%) of these patients had a SE; none had a stroke. All patients with hypoperfusion had focal neurological deficit; three (37%) of them a simultaneous ischemic stroke (in the remaining five, hypoperfusion was considered to be related to the seizure post-ictal phase). In the 22 with normal perfusion, 9 had a focal deficit (10 a normal clinical status, 2 altered consciousness and 1 ongoing seizure); 3 had a SE, and 1 had a stroke. Patients with SE featured a higher prevalence of hyperperfusion (9/13 [69%] vs. 4/30 [13%] without SE, p = 0.00).
Conclusion
In patients with acute epileptic seizures, regional hyperperfusion on PCT may suggest an ongoing or recently resolved SE, whereas hypoperfusion may be due to post-ictal state or simultaneous AIS. These observations might help attributing focal deficits to epileptic seizures rather than stroke, allowing for targeted therapy.



Similar content being viewed by others
References
Nor AM, Davis J, Sen B et al (2005) The Recognition of Stroke in the Emergency Room (ROSIER) Scale: development and validation of a stroke recognition instrument. Lancet Neurol 4:727–734. https://doi.org/10.1016/S1474-4422(05)70201-5
Alvarez V, Rossetti AO, Papavasileiou V, Michel P (2013) Acute seizures in acute ischemic stroke: does thrombolysis have a role to play? J Neurol 260:55–61. https://doi.org/10.1007/s00415-012-6583-6
Richoz B, Hugli O, Dami F et al (2015) Acute stroke chameleons in a university hospital: risk factors, circumstances, and outcomes. Neurology 85:505–511. https://doi.org/10.1212/WNL.0000000000001830
Chernyshev OY, Martin-Schild S, Albright KC et al (2010) Safety of tPA in stroke mimics and neuroimaging-negative cerebral ischemia. Neurology 74:1340–1345. https://doi.org/10.1212/WNL.0b013e3181dad5a6
Leonhardt G, de Greiff A, Weber J et al (2005) Brain perfusion following single seizures. Epilepsia 46:1943–1949. https://doi.org/10.1111/j.1528-1167.2005.00336.x
Flacke S, Wüllner U, Keller E et al (2000) Reversible changes in echo planar perfusion- and diffusion-weighted MRI in status epilepticus. Neuroradiology 42:92–95
Bill O, Faouzi M, Meuli R et al (2016) Added value of multimodal computed tomography imaging: analysis of 1994 acute ischaemic strokes. Eur J Neurol. https://doi.org/10.1111/ene.13173
Campbell BCV, Mitchell PJ, Kleinig TJ et al (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372:1009–1018. https://doi.org/10.1056/NEJMoa1414792
Royter V, Paletz L, Waters MF (2008) Stroke vs. status epilepticus. A case report utilizing CT perfusion. J Neurol Sci 266:174–176. https://doi.org/10.1016/j.jns.2007.08.038
Gelfand JM, Wintermark M, Josephson SA (2010) Cerebral perfusion-CT patterns following seizure. Eur J Neurol 17:594–601. https://doi.org/10.1111/j.1468-1331.2009.02869.x
Hauf M, Slotboom J, Nirkko A et al (2009) Cortical regional hyperperfusion in nonconvulsive status epilepticus measured by dynamic brain perfusion CT. Am J Neuroradiol 30:693–698. https://doi.org/10.3174/ajnr.A1456
Austein F, Huhndorf M, Meyne J et al (2018) Advanced CT for diagnosis of seizure-related stroke mimics. Eur Radiol 28:1791–1800. https://doi.org/10.1007/s00330-017-5174-4
Michel P, Odier C, Rutgers M et al (2010) The Acute STroke Registry and Analysis of Lausanne (ASTRAL): design and baseline analysis of an ischemic stroke registry including acute multimodal imaging. Stroke 41:2491–2498. https://doi.org/10.1161/STROKEAHA.110.596189
Meier P, Zierler KL (1954) On the theory of the indicator-dilution method for measurement of blood flow and volume. J Appl Physiol 6:731–744
Knollmann F, Coakley F (2006) Multislice CT: principles and protocols. Saunders, Philadelphia
Mathews MS, Smith WS, Wintermark M et al (2008) Local cortical hypoperfusion imaged with CT perfusion during postictal Todd’s paresis. Neuroradiology 50:397–401. https://doi.org/10.1007/s00234-008-0362-1
Marchal G, Young AR, Baron JC (1999) Early postischemic hyperperfusion: pathophysiologic insights from positron emission tomography. J Cerebral Blood Flow Metab 19:467–482. https://doi.org/10.1097/00004647-199905000-00001
Trinka E, Cock H, Hesdorffer D et al (2015) A definition and classification of status epilepticus–Report of the ILAE Task Force on Classification of Status Epilepticus. Epilepsia 56:1515–1523. https://doi.org/10.1111/epi.13121
Guidelines for epidemiologic studies on epilepsy (1993) Commission on epidemiology and prognosis, international league against epilepsy. Epilepsia 34:592–596
Berg AT, Berkovic SF, Brodie MJ et al (2010) Revised terminology and concepts for organization of seizures and epilepsies: report of the ILAE Commission on Classification and Terminology, 2005–2009. Epilepsia 51:676–685. https://doi.org/10.1111/j.1528-1167.2010.02522.x
Payabvash S, Oswood MC, Truwit CL, McKinney AM (2015) Acute CT perfusion changes in seizure patients presenting to the emergency department with stroke-like symptoms: correlation with clinical and electroencephalography findings. Clin Radiol 70:1136–1143. https://doi.org/10.1016/j.crad.2015.06.078
Newton MR, Berkovic SF, Austin MC et al (1992) Postictal switch in blood flow distribution and temporal lobe seizures. J Neurol Neurosurg Psychiatry 55:891–894
Masterson K, Vargas MI, Delavelle J (2009) Postictal deficit mimicking stroke: role of perfusion CT. J Neuroradiol 36:48–51. https://doi.org/10.1016/j.neurad.2008.08.006
Salih MA, Kabiraj M, Al-Jarallah AS et al (1997) Hemiconvulsion-hemiplegia-epilepsy syndrome. A clinical, electroencephalographic and neuroradiological study. Childs Nerv Syst 13:257–263
Farrell JS, Colangeli R, Wolff MD et al (2017) Postictal hypoperfusion/hypoxia provides the foundation for a unified theory of seizure-induced brain abnormalities and behavioral dysfunction. Epilepsia 58:1493–1501. https://doi.org/10.1111/epi.13827
Best AC, Acosta NR, Fraser JE et al (2012) Recognizing false ischemic penumbras in CT brain perfusion studies. RadioGraphics 32:1179–1196. https://doi.org/10.1148/rg.324105742
Tsivgoulis G, Zand R, Katsanos AH et al (2015) Safety of intravenous thrombolysis in stroke mimics: prospective 5-year study and comprehensive meta-analysis. Stroke 46:1281–1287. https://doi.org/10.1161/STROKEAHA.115.009012
Meyer IA, Cereda CW, Correia PN et al (2017) Factors associated with focal computed tomographic perfusion abnormalities in supratentorial transient ischemic attacks. Stroke. https://doi.org/10.1161/STROKEAHA.117.018635
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Strambo, Dr. Rey, Dr. Rossetti, Dr. Maeder, Dr. Dunet and Dr. Browaeys have nothing to disclose. Dr. Michel received research grants from the Swiss Heart Foundation, and BMS; speaker fees from Bayer, Daiichi-Sankyo, Medtronic and Stryker; honoraria from scientific advisory boards from Boehringer-Ingelheim, Bayer, Pfizer and BMS; and consulting fees from Astra-Zeneca and Amgen. All this support is received by his institution (CHUV) and is used for stroke education and research.
Ethical standards
Data were obtained from routine care during hospitalisation and analysed after anonymization, which does not require formal ethical approval or patient consent under national law.
Rights and permissions
About this article
Cite this article
Strambo, D., Rey, V., Rossetti, A.O. et al. Perfusion-CT imaging in epileptic seizures. J Neurol 265, 2972–2979 (2018). https://doi.org/10.1007/s00415-018-9095-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-018-9095-1