Abstract
Purpose
To explore the prognostic factors and the optimal treatment modalities for patients with stage IVA laryngeal squamous cell carcinoma (LSCC), so as to improve the survival rate of patients.
Methods
Patients with stage IVA LSCC between 2004 and 2019 were selected from the Surveillance, Epidemiology, and End Results (SEER) database. We used competing risk models to build nomograms for predicting cancer-specific survival (CSS). The effectiveness of the model was assessed using the calibration curves and the concordance index (C-index). The above results were compared with the nomogram established by Cox regression analysis. The patients were grouped into low-risk and high-risk groups by competing risk nomogram formula. And the Kaplan–Meier (K–M) method and log-rank test were used to make sure that these groups had a survival difference.
Results
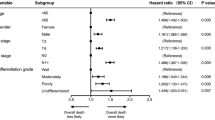
Overall, 3612 patients were included. Older age, black race, a higher N stage, a higher pathological grade, and a larger tumor size were independent risk factors for CSS; married marital status, total/radical laryngectomy, and radiotherapy were protective factors. The C-index was 0.663, 0.633, and 0.628 in the train set and 0.674, 0.639, and 0.629 in the test set of the competing risk model, and 0.672, 0.640, and 0.634 in the traditional Cox nomogram for 1, 3, and 5 years. In overall survival and CSS, the prognosis of the high-risk group was poorer than that of the low-risk group.
Conclusion
For patients with stage IVA LSCC, a competing risk nomogram was created to help screen risk population and guide clinical decision-making.





Similar content being viewed by others
Data availability
The raw data were derived from Surveillance, Epidemiology, and End Results (SEER) Program. SEER*Stat Software version 8.4.0.1. https://seer.cancer.gov/seerstat/download. Accessed June 11, 2022.
Abbreviations
- CIF:
-
Cumulative incidence function
- C-index:
-
Concordance index
- CRT:
-
Chemoradiotherapy
- CSS:
-
Cancer-specific survival
- K–M:
-
Kaplan–Meier
- LSCC:
-
Laryngeal squamous cell carcinoma
- NCCN:
-
National Comprehensive Cancer Network
- OS:
-
Overall survival
- SEER:
-
Surveillance, Epidemiology, and End Results
References
Sung H, Ferlay J, Siegel RL et al (2021) Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Bray F, Ferlay J, Soerjomataram I et al (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424. https://doi.org/10.3322/caac.21492
Torre LA, Bray F, Siegel RL et al (2015) Global cancer statistics, 2012. CA Cancer J Clin 65:87–108. https://doi.org/10.3322/caac.21262
Steuer CE, El-Deiry M, Parks JR et al (2017) An update on larynx cancer. CA Cancer J Clin 67:31–50. https://doi.org/10.3322/caac.21386
Cavalieri S, Orlandi E, Ivaldi E et al (2021) Management of loco-regionally advanced squamous laryngeal cancer in elderly patients. Eur Arch Otorhinolaryngol 278:771–779. https://doi.org/10.1007/s00405-020-06179-1
Ramsey T, Guo E, Svider PF et al (2018) Laryngeal cancer: global socioeconomic trends in disease burden and smoking habits. Laryngoscope 128:2039–2053. https://doi.org/10.1002/lary.27068
Zhu X, Zhao M, Zhou L et al (2020) Significance of examined lymph nodes number and metastatic lymph nodes ratio in overall survival and adjuvant treatment decision in resected laryngeal carcinoma. Cancer Med 9:3006–3014. https://doi.org/10.1002/cam4.2902
Forastiere AA, Goepfert H, Maor M et al (2003) Concurrent chemotherapy and radiotherapy for organ preservation in advanced laryngeal cancer. N Engl J Med 349:2091–2098. https://doi.org/10.1056/NEJMoa031317
Lin CC, Fedewa SA, Prickett KK et al (2016) Comparative effectiveness of surgical and nonsurgical therapy for advanced laryngeal cancer. Cancer 122:2845–2856. https://doi.org/10.1002/cncr.30122
Wushouer A, Li W, Zhang M et al (2022) Comparison of treatment modalities for selected advanced laryngeal squamous cell carcinoma. Eur Arch Otorhinolaryngol 279:361–371. https://doi.org/10.1007/s00405-021-06780-y
Ben Kridis W, Werda I, Mnejja W et al (2021) Therapeutic results of laryngeal preservation: a retrospective study. Exp Oncol 43:168–172. https://doi.org/10.32471/exp-oncology.2312-8852.vol-43-no-2.16273
Liao F, Wang W, Wang J (2022) A deep learning-based model predicts survival for patients with laryngeal squamous cell carcinoma: a large population-based study. Eur Arch Otorhinolaryngol. https://doi.org/10.1007/s00405-022-07627-w
Grover S, Swisher-McClure S, Mitra N et al (2015) Total laryngectomy versus larynx preservation for T4a larynx cancer: patterns of care and survival outcomes. Int J Radiat Oncol Biol Phys 92:594–601. https://doi.org/10.1016/j.ijrobp.2015.03.004
National Comprehensive Cancer Network NCCN Clinical Practice Guidelines in Oncology: Head and Neck Cancers version 2.2022. https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf. Accessed 25 Oct 2022
Fine JP, Gray RJ (1999) A Proportional hazards model for the subdistribution of a competing risk. J Am Stat Assoc 94:496–509. https://doi.org/10.1080/01621459.1999.10474144
Wu W, Yang J, Li D et al (2021) Competitive risk analysis of prognosis in patients with cecum cancer: a population-based study. Cancer Control 28:1073274821989316. https://doi.org/10.1177/1073274821989316
Abdel-Qadir H, Thavendiranathan P, Austin PC et al (2019) Development and validation of a multivariable prediction model for major adverse cardiovascular events after early stage breast cancer: a population-based cohort study. Eur Heart J 40:3913–3920. https://doi.org/10.1093/eurheartj/ehz460
Bian F, Li C, Han D et al (2020) Competing-risks model for predicting the postoperative prognosis of patients with papillary thyroid adenocarcinoma based on the surveillance, epidemiology, and end results (SEER) database. Med Sci Monit 26:e924045. https://doi.org/10.12659/MSM.924045
Di Wu, Yang Y, Jiang M et al (2022) Competing risk of the specific mortality among Asian-American patients with prostate cancer: a surveillance, epidemiology, and end results analysis. BMC Urol 22:42. https://doi.org/10.1186/s12894-022-00992-y
Camp RL, Dolled-Filhart M, Rimm DL (2004) X-tile: a new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization. Clin Cancer Res 10:7252–7259. https://doi.org/10.1158/1078-0432.CCR-04-0713
Wolf GT, Fisher SG, Hong WK et al (1991) Induction chemotherapy plus radiation compared with surgery plus radiation in patients with advanced laryngeal cancer. N Engl J Med 324:1685–1690. https://doi.org/10.1056/NEJM199106133242402
Chen N-X, Fan W-J, Ma L et al (2020) Efficacy of non-surgical larynx-preservation comprehensive treatment in advanced laryngeal carcinoma. Chin Med J (Engl) 133:615–617. https://doi.org/10.1097/CM9.0000000000000639
Hoffman HT, Porter K, Karnell LH et al (2006) Laryngeal cancer in the United States: changes in demographics, patterns of care, and survival. Laryngoscope 116:1–13. https://doi.org/10.1097/01.mlg.0000236095.97947.26
Li M, Zhang T, Tan B et al (2019) Role of postoperative adjuvant radiotherapy for locally advanced laryngeal cancer: a meta-analysis. Acta Otolaryngol 139:172–177. https://doi.org/10.1080/00016489.2018.1542159
Patel SA, Qureshi MM, Dyer MA et al (2019) Comparing surgical and nonsurgical larynx-preserving treatments with total laryngectomy for locally advanced laryngeal cancer. Cancer 125:3367–3377. https://doi.org/10.1002/cncr.32292
Wu Y, Zhang L, Tang T et al (2021) Postoperative radiotherapy omitting level IV for locally advanced supraglottic and glottic laryngeal carcinoma. Technol Cancer Res Treat 20:1533033820985876. https://doi.org/10.1177/1533033820985876
Forastiere AA, Ismaila N, Lewin JS et al (2018) Use of larynx-preservation strategies in the treatment of laryngeal cancer: American Society of Clinical Oncology Clinical Practice Guideline Update. J Clin Oncol 36:1143–1169. https://doi.org/10.1200/JCO.2017.75.7385
Stokes WA, Jones BL, Bhatia S et al (2017) A comparison of overall survival for patients with T4 larynx cancer treated with surgical versus organ-preservation approaches: a National Cancer Data Base analysis. Cancer 123:600–608. https://doi.org/10.1002/cncr.30382
Su X, He H-C, Ye Z-L et al (2020) A 10-year study on larynx preservation compared with surgical resection in patients with locally advanced laryngeal and hypopharyngeal cancers. Front Oncol 10:535893. https://doi.org/10.3389/fonc.2020.535893
Aslıer M, Uçurum BE, Kaya HC et al (2021) The prognostic value of thyroid gland invasion in locally advanced laryngeal cancers. Acta Otolaryngol 141:865–872. https://doi.org/10.1080/00016489.2021.1962013
Divi V, Worden FP, Prince ME et al (2010) Chemotherapy alone for organ preservation in advanced laryngeal cancer. Head Neck 32:1040–1047. https://doi.org/10.1002/hed.21285
Lin T-C, Huang C-H, Lien M-Y et al (2022) Tumor Volume Reduction Rate to Induction Chemotherapy is a Prognostic Factor for Locally Advanced Head and Neck Squamous Cell Carcinoma: A Retrospective Cohort Study. Technol Cancer Res Treat 21:15330338221107714. https://doi.org/10.1177/15330338221107714
Spector ME, Rosko AJ, Swiecicki PL et al (2018) From VA Larynx to the future of chemoselection: Defining the role of induction chemotherapy in larynx cancer. Oral Oncol 86:200–205. https://doi.org/10.1016/j.oraloncology.2018.09.026
Kowalski LP, Alcantara PS, Magrin J et al (1994) A case-control study on complications and survival in elderly patients undergoing major head and neck surgery. The American Journal of Surgery 168:485–490. https://doi.org/10.1016/s0002-9610(05)80107-2
Kang EJ, Lee Y-G, Keam B et al (2022) Characteristics and treatment patterns in older patients with locally advanced head and neck cancer (KCSG HN13-01). Korean J Intern Med 37:190–200. https://doi.org/10.3904/kjim.2020.636
Cui J, Wang L, Zhong W et al (2020) Development and validation of nomogram to predict risk of survival in patients with laryngeal squamous cell carcinoma. Biosci Rep. https://doi.org/10.1042/BSR20200228
Zhu X, Heng Y, Zhou L et al (2020) Survival prediction and treatment strategies for patients with advanced laryngeal carcinoma: a population-based study. Int J Clin Oncol 25:1483–1491. https://doi.org/10.1007/s10147-020-01688-9
Gong H, Zhou L, Hsueh C-Y et al (2021) Prognostic value of pathological tumor size in patients with supraglottic carcinoma. Am J Otolaryngol 42:102757. https://doi.org/10.1016/j.amjoto.2020.102757
Gong H, Zhou L, Wu H et al (2021) Pathologic tumor size as a predictor of the survival outcomes of patients with glottic carcinoma. Otolaryngol Head Neck Surg 164:353–358. https://doi.org/10.1177/0194599820937296
Wang Q, Tan Z, Zheng C et al (2022) Number of positive lymph nodes combined with the logarithmic ratio of positive lymph nodes predicts survival in patients with non-metastatic larynx squamous cell carcinoma. J Cancer 13:1773–1784. https://doi.org/10.7150/jca.67348
Dağdelen M, Şahin M, Çatal TK et al (2022) Selective local postoperative radiotherapy for T3–T4 N0 laryngeal cancer. Strahlenther Onkol 198:1025–1031. https://doi.org/10.1007/s00066-022-01999-y
Almadori G, Coli A, de Corso E et al (2022) Parathyroid hormone-related peptide and parathyroid hormone-related peptide receptor type 1 in locally advanced laryngeal cancer as prognostic indicators of relapse and survival. BMC Cancer 22:704. https://doi.org/10.1186/s12885-022-09748-1
Mesía R, Garcia-Saenz JA, Lozano A et al (2017) Could the addition of cetuximab to conventional radiation therapy improve organ preservation in those patients with locally advanced larynx cancer who respond to induction chemotherapy? An organ preservation Spanish Head and Neck Cancer Cooperative Group Phase 2 Study. Int J Radiat Oncol Biol Phys 97:473–480. https://doi.org/10.1016/j.ijrobp.2016.11.016
Frankart AJ, Sadraei NH, Huth B et al (2022) A phase I/II trial of concurrent immunotherapy with chemoradiation in locally advanced larynx cancer. Laryngosc Investig Otolaryngol 7:437–443. https://doi.org/10.1002/lio2.780
Acknowledgements
The authors are grateful to the open access SEER database and R software for providing us with the raw research data and for the data analysis, and to all the professors and friends who have helped us with the use of related software.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
Conceptualization: ZS, ZC, XS, and LZ; data curation: ZS and ZC; formal analysis: ZS and ZC; writing—original draft preparation: ZS and ZC; writing—review and editing: ZS, ZC, XS, and LZ. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Institutional review board statement
Ethical review and approval were waived for this study, due to the data being publicly available and anonymous.
Informed consent statement
Patient consent was waived due to the data being publicly available and anonymous.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
405_2023_7983_MOESM1_ESM.tif
Supplementary Figure 1. Traditional Cox nomogram to predict 1-, 3-, and 5-year cancer specific survival (CSS) in patients with primary stage IVA laryngeal squamous cell carcinoma
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, Z., Chen, Z., Sun, X. et al. Competing risk models versus traditional Cox models for prognostic factors’ prediction and care recommendation in patients with advanced laryngeal squamous carcinoma: a population-based study. Eur Arch Otorhinolaryngol 280, 3745–3756 (2023). https://doi.org/10.1007/s00405-023-07983-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-023-07983-1