Abstract
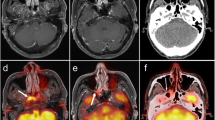
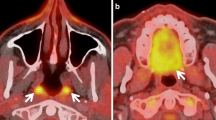
The aim of this study was to verify the effectiveness of positron emission tomography (PET) in detecting primary sites in carcinoma of unknown primary (CUP) patients. In this study, CUP represented a group of heterogeneous tumors that shared the clinical manifestation of metastatic carcinoma with no obvious primary site at the time of first diagnosis, which included clinical investigations, computed tomography, magnetic resonance imaging and panendoscopy. We reviewed the records of 24 patients with CUP between January 1995 and December 2009. The patients who demonstrated additional tracer uptake sites other than previously known metastatic lesions by PET scan were done direct biopsies for the sites of accumulation. Patients who had a negative PET scan or for whom the primary site could not be identified by direct biopsies underwent examination under anesthesia of the at-risk occult tumor sites. PET scan demonstrated focal accumulation suspicious for primary tumor in 12 (50.0%) of 24 patients: tonsil 5, nasopharynx 3, hypopharynx 1, tongue 1, larynx 1, and maxillary sinus 1. A subsequent biopsy of these sites revealed primary cancer in 9 (37.5%) of 24 patients: tonsil 5, nasopharynx 1, hypopharynx 1, tongue 1, and maxillary sinus 1. In the remaining three patients, no malignant cells were found by the biopsy of the accumulated area: nasopharynx 2, larynx 1. PET scans increase the yield of primary tumor by 37.5%. The sensitivity, specificity for PET scan were 80.8, 76.9%, respectively. PET scanning is useful in detecting primary cancer of CUP patients.


Similar content being viewed by others
References
Johansen J, Eigtved A, Buchwald C, Theilgaard SA, Hansen HS (2002) Implication of 18F-fluoro-2-deoxy-d-glucose positron emission tomography on management of carcinoma of unknown primary in the head and neck: a Danish cohort study. Laryngoscope 112:2009–2014
Calabrese L, Jereczek-Fossa BA, Jassem J et al (2005) Diagnosis and management of neck metastases from an unknown primary. Acta Otorhinolaryngol Ital 25:2–12
Miller FR, Karnad AB, Eng T, Hussey DH, Stan McGuff H, Otto RA (2008) Management of the unknown primary carcinoma: long-term follow-up on a negative PET scan and negative panendoscopy. Head Neck 30:28–34
Fletcher JW, Djulbegovic B, Soares HP et al (2008) Recommendations on the use of 18F-FDG PET in oncology. J Nucl Med 49:480–508
AAssar OS, Fischbein NJ, Caputo GR et al (1999) Metastatic head and neck cancer: role and usefulness of FDG PET in locating occult primary tumors. Radiology 210:177–181
Braams JW, Pruim J, Kole AC et al (1997) Detection of unknown primary head and neck tumors by positron emission tomography. Int J Oral Maxillofac Surg 26:112–115
Greven KM, Keyes JW Jr, Williams DW 3rd, McGuirt WF, Joyce WT 3rd (1999) Occult primary tumors of the head and neck: lack of benefit from positron emission tomography imaging with 2-[F-18]fluoro-2-deoxy-d-glucose. Cancer 86:114–118
Hanasono MM, Kunda LD, Segall GM, Ku GH, Terris DJ (1999) Uses and limitations of FDG positron emission tomography in patients with head and neck cancer. Laryngoscope 109:880–885
Kole AC, Nieweg OE, Pruim J et al (1998) Detection of unknown occult primary tumors using positron emission tomography. Cancer 82:1160–1166
Lassen U, Daugaard G, Eigtved A, Damgaard K, Friberg L (1999) 18F-FDG whole body positron emission tomography (PET) in patients with unknown primary tumours (UPT). Eur J Cancer 35:1076–1082
Safa AA, Tran LM, Rege S et al (1999) The role of positron emission tomography in occult primary head and neck cancers. Cancer J Sci Am 5:214–218
Stokkel MP, Terhaard CH, Hordijk GJ, van Rijk PP (1999) The detection of unknown primary tumors in patients with cervical metastases by dual-head positron emission tomography. Oral Oncol 35:390–394
Bohuslavizki KH, Klutmann S, Kröger S et al (2000) FDG PET detection of unknown primary tumors. J Nucl Med 41:816–822
Jungehülsing M, Scheidhauer K, Damm M et al (2000) 2[F]-fluoro-2-deoxy-d-glucose positron emission tomography is a sensitive tool for the detection of occult primary cancer (carcinoma of unknown primary syndrome) with head and neck lymph node manifestation. Otolaryngol Head Neck Surg 123:294–301
Wong WL, Saunders M (2003) The impact of FDG PET on the management of occult primary head and neck tumours. Clin Oncol (R Coll Radiol) 15:461–466
Gutzeit A, Antoch G, Kühl H et al (2005) Unknown primary tumors: detection with dual-modality PET/CT—initial experience. Radiology 34:227–234
Nanni C, Rubello D, Castellucci P et al (2005) Role of 18F-FDG PET-CT imaging for the detection of an unknown primary tumour: preliminary results in 21 patients. Eur J Nucl Med Mol Imaging 32:589–592
Wartski M, Le Stanc E, Gontier E et al (2007) In search of an unknown primary tumour presenting with cervical metastases: performance of hybrid FDG-PET-CT. Nucl Med Commun 28:365–371
Johansen J, Buus S, Loft A et al (2008) Prospective study of 18FDG-PET in the detection and management of patients with lymph node metastases to the neck from an unknown primary tumor. Results from the DAHANCA-13 study. Head Neck 30:471–478
Rusthoven KE, Koshy M, Paulino AC (2004) The role of fluorodeoxyglucose positron emission tomography in cervical lymph node metastases from an unknown primary tumor. Cancer 101:2641–2649
Waltonen JD, Ozer E, Schuller DE, Agrawal A (2009) Tonsillectomy vs. deep tonsil biopsies in detecting occult tonsil tumors. Laryngoscope 119:102–106
Dong MJ, Zhao K, Lin XT, Zhao J, Ruan LX, Liu ZF (2008) Role of fluorodeoxyglucose-PET versus fluorodeoxyglucose-PET/computed tomography in detection of unknown primary tumor: a meta-analysis of the literature. Nucl Med Commun 29:791–802
Taguchi T, Tsukuda M, Mikami Y et al (2009) Treatment results and prognostic factors for advanced squamous cell carcinoma of the head and neck treated with concurrent chemoradiotherapy. Auris Nasus Larynx 36:199–204
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yabuki, K., Tsukuda, M., Horiuchi, C. et al. Role of 18F-FDG PET in detecting primary site in the patient with primary unknown carcinoma. Eur Arch Otorhinolaryngol 267, 1785–1792 (2010). https://doi.org/10.1007/s00405-010-1371-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-010-1371-3