Abstract
Introduction
Functional alignment (FA) in total knee arthroplasty (TKA) has been introduced to restore the native joint line obliquity, respect the joint line height and minimize the need of soft tissue releases. The purpose of this study was to assess the intraoperative joint line alignment and compare it with the preoperative epiphyseal orientation of the femur and tibia in patients undergoing robotic-arm-assisted (RA)-TKA using FA.
Materials and Methods
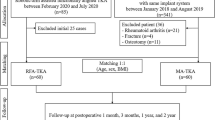
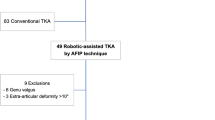
This retrospective study included a consecutive series of patients undergoing RA-TKA between February 2019 and February 2021. The joint line orientation of the femur and tibia in the three-dimensions was calculated and classified on preoperative CT-scans and compared with the intraoperative implant alignment. The tibial cut was performed according to the tibial preoperative anatomy. The femoral cuts were fine-tuned based on tensioned soft tissues, aiming for balanced medial and lateral gaps in flexion and extension.
Results
A total of 115 RA-TKAs were assessed. On average, the tibial component was placed at 1.8° varus (SD 1.3), while the femur was placed at 0.8° valgus (SD 2.2) and 0.6° external rotation (SD 2.6) relative to the surgical transepicondylar axis. Moderate to strong, statistically significant relationships were described between preoperative tibial coronal alignment and tibial cut orientation (r = 0.7, p < 0.0001), preoperative femoral orientation in the coronal and axial planes and intraoperative femoral cuts alignment (r = 0.7, p < 0.0001 and r = 0.5, p < 0.0001, respectively). One case (0.9%) of slight tibial component varus subsidence was reported 45-days post-operatively, but implant revision was not necessary.
Conclusions
The proposed robotic-assisted functional technique for TKA alignment, with a restricted tibial component coronal alignment, based on the preoperative phenotype and femoral component positioning as dictated by the soft tissues, provided joint line respecting resections. Further studies are needed to assess long-term implant survivorship, patient satisfaction and alignment-related failures.





Similar content being viewed by others
References
Hirschmann MT, Becker R, Tandogan R, Vendittoli PA, Howell S (2019) Alignment in TKA: what has been clear is not anymore! Knee Surg Sports Traumatol Arthrosc 27(7):2037–2039. https://doi.org/10.1007/s00167-019-05558-4
Insall JN, Binazzi R, Soudry M, Mestriner LA (1985) Total knee arthroplasty. Clin Orthop Relat Res 192:13–22. https://doi.org/10.1097/00003086-198501000-00003
Rivière C, Lazic S, Boughton O, Wiart Y, Vïllet L, Cobb J (2018) Current concepts for aligning knee implants: patient-specific or systematic? EFORT Open Rev 3(1):1–6. https://doi.org/10.1302/2058-5241.3.170021
Howell SM, Howell SJ, Kuznik KT, Cohen J, Hull ML (2013) Does a kinematically aligned total knee arthroplasty restore function without failure regardless of alignment category? Clin Orthop Relat Res 471(3):1000–1007. https://doi.org/10.1007/s11999-012-2613-z
Hess S, Moser LB, Amsler F, Behrend H, Hirschmann MT (2019) Highly variable coronal tibial and femoral alignment in osteoarthritic knees: a systematic review. Knee Surg Sports Traumatol Arthrosc 27(5):1368–1377. https://doi.org/10.1007/s00167-019-05506-2
Blakeney W, Beaulieu Y, Puliero B, Kiss MO, Vendittoli PA (2020) Bone resection for mechanically aligned total knee arthroplasty creates frequent gap modifications and imbalances. Knee Surg Sports Traumatol Arthrosc 28(5):1532–1541. https://doi.org/10.1007/s00167-019-05562-8
MacDessi SJ, Griffiths-Jones W, Chen DB, Griffiths-Jones S, Wood JA, Diwan AD, Harris IA (2020) Restoring the constitutional alignment with a restrictive kinematic protocol improves quantitative soft-tissue balance in total knee arthroplasty: a randomized controlled trial. Bone Joint J. 102-B(1):117–124. https://doi.org/10.1302/0301-620X.102B1.BJJ-2019-0674.R2
Klasan A, de Steiger R, Holland S, Hatton A, Vertullo CJ, Young SW (2020) Similar risk of revision after kinematically aligned, patient-specific instrumented total knee arthroplasty, and all other total knee arthroplasty: combined results from the Australian and New Zealand joint replacement registries. J Arthroplasty 35:2872–2877. https://doi.org/10.1016/j.arth.2020.05.065
Teeter MG, Naudie DD, McCalden RW, Yuan X, Holdsworth DW, MacDonald SJ, Lanting BA (2018) Varus tibial alignment is associated with greater tibial baseplate migration at 10 years following total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26(6):1610–1617. https://doi.org/10.1007/s00167-017-4765-6
Innocenti B, Bellemans J, Catani F (2016) Deviations from optimal alignment in TKA: is there a biomechanical difference between femoral or tibial component alignment? J Arthroplasty 31(1):295–301. https://doi.org/10.1016/j.arth.2015.07.038
Almaawi AM, Hutt JRB, Masse V, Lavigne M, Vendittoli PA (2017) The impact of mechanical and restricted kinematic alignment on knee anatomy in total knee arthroplasty. J Arthroplasty 32(7):2133–2140. https://doi.org/10.1016/j.arth.2017.02.028
Rivière C, Iranpour F, Auvinet E, Howell S, Vendittoli PA, Cobb J, Parratte S (2017) Alignment options for total knee arthroplasty: a systematic review. Orthop Traumatol Surg Res 103(7):1047–1056. https://doi.org/10.1016/j.otsr.2017.07.010
Zambianchi F, Giorgini A, Ensini A, Lombari V, Daffara V, Catani F (2021) Navigated, soft tissue-guided total knee arthroplasty restores the distal femoral joint line orientation in a modified mechanically aligned technique. Knee Surg Sports Traumatol Arthrosc 29(3):966–974. https://doi.org/10.1007/s00167-020-06056-8
Onggo JR, Onggo JD, de Steiger R, Hau R (2020) Robotic-assisted total knee arthroplasty is comparable to conventional total knee arthroplasty: a meta-analysis and systematic review. Arch Orthop Trauma Surg 140(10):1533–1549. https://doi.org/10.1007/s00402-020-03512-5
Oussedik S, Abdel MP, Victor J, Pagnano MW, Haddad FS (2020) Alignment in total knee arthroplasty. Bone Joint J 102-B(3):276–279. https://doi.org/10.1302/0301-620X.102B3.BJJ-2019-1729
Kayani B, Konan S, Tahmassebi J, Oussedik S, Moriarty PD, Haddad FS (2020) A prospective double-blinded randomised control trial comparing robotic arm-assisted functionally aligned total knee arthroplasty versus robotic arm-assisted mechanically aligned total knee arthroplasty. Trials 21(1):194. https://doi.org/10.1186/s13063-020-4123-8
Chang JS, Kayani B, Wallace C, Haddad FS (2021) Functional alignment achieves soft-tissue balance in total knee arthroplasty as measured with quantitative sensor-guided technology. Bone Joint J. 103-B(3):507–514. https://doi.org/10.1302/0301-620X.103B.BJJ-2020-0940.R1
Hirschmann MT, Hess S, Behrend H, Amsler F, Leclercq V, Moser LB (2019) Phenotyping of hip-knee-ankle angle in young non-osteoarthritic knees provides better understanding of native alignment variability. Knee Surg Sports Traumatol Arthrosc 27(5):1378–1384. https://doi.org/10.1007/s00167-019-05507-1
Meier M, Janssen D, Koeck FX, Thienpont E, Beckmann J, Best R (2021) Variations in medial and lateral slope and medial proximal tibial angle. Knee Surg Sports Traumatol Arthrosc 29(3):939–946. https://doi.org/10.1007/s00167-020-06052-y
Kayani B, Konan S, Pietrzak JRT, Haddad FS (2018) Iatrogenic bone and soft tissue trauma in robotic-arm assisted total knee arthroplasty compared with conventional jig-based total knee arthroplasty: a prospective cohort study and validation of a new classification system. J Arthroplasty 33(8):2496–2501. https://doi.org/10.1016/j.arth.2018.03.042
Kayani B, Konan S, Horriat S, Ibrahim MS, Haddad FS (2019) Posterior cruciate ligament resection in total knee arthroplasty: the effect on flexion-extension gaps, mediolateral laxity, and fixed flexion deformity. Bone Joint J. 101-B(10):1230–1237. https://doi.org/10.1302/0301-620X.101B10.BJJ-2018-1428.R2
Winnock de Grave P, Luyckx T, Claeys K, Tampere T, Kellens J, Müller J, Gunst P (2020) Higher satisfaction after total knee arthroplasty using restricted inverse kinematic alignment compared to adjusted mechanical alignment. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06165-4
Ritter MA, Davis KE, Meding JB, Pierson JL, Berend ME, Malinzak RA (2011) The effect of alignment and BMI on failure of total knee replacement. J Bone Joint Surg Am 93(17):1588–1596. https://doi.org/10.2106/JBJS.J.00772
Laende EK, Richardson CG, Dunbar MJ (2019) A randomized controlled trial of tibial component migration with kinematic alignment using patient-specific instrumentation versus mechanical alignment using computer-assisted surgery in total knee arthroplasty. Bone Joint J 101(8):929–940. https://doi.org/10.1302/0301-620X.101B8.BJJ-2018-0755.R3
Laforest G, Kostretzis L, Kiss MO, Vendittoli PA (2021) Restricted kinematic alignment leads to uncompromised osseointegration of cementless total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06427-1
Liow MH, Xia Z, Wong MK, Tay KJ, Yeo SJ, Chin PL (2014) Robot-assisted total knee arthroplasty accurately restores the joint line and mechanical axis. A prospective randomised study. J Arthroplasty 29(12):2373–2377. https://doi.org/10.1016/j.arth.2013.12.010
Luyckx T, Vandenneucker H, Ing LS, Vereecke E, Ing AV, Victor J (2018) Raising the joint line in TKA is associated with mid-flexion laxity: a study in cadaver knees. Clin Orthop Relat Res 476(3):601–611. https://doi.org/10.1007/s11999.0000000000000067
Gu Y, Roth JD, Howell SM, Hull ML (2014) How frequently do four methods for mechanically aligning a total knee arthroplasty cause collateral ligament imbalance and change alignment from normal in white patients? AAOS exhibit selection. J Bone Joint Surg Am 96(12):101. https://doi.org/10.2106/JBJS.M.00306
Batailler C, Fernandez A, Swan J, Servien E, Haddad FS, Catani F, Lustig S (2020) MAKO CT-based robotic arm-assisted system is a reliable procedure for total knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06283-z
Kayani B, Konan S, Huq SS, Tahmassebi J, Haddad FS (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sports Traumatol Arthrosc 27(4):1132–1141. https://doi.org/10.1007/s00167-018-5138-5
Acknowledgements
The authors would like to thank Laura Scholl, MSc for English language editing.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
FZ—developed the study protocol, performed data interpretation and wrote the manuscript. GB—collected primary data. AM—performed data analysis and interpretation. MP—collected primary data. AI—performed data analysis. AE—revised the manuscript critically. FC—generated the study hypothesis, performed data interpretation and critically appraised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors Francesco Zambianchi, Gabriele Bazzan, Andrea Marcovigi, Andrea Illuminati and Andrea Ensini or any member of their immediate family, have no funding or commercial associations (e.g. consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article. The author Marco Pavesi is a paid employee of Ab Medica S.p.A. The author Fabio Catani reports consultancy and speaking fees, royalties, and fees for participation in review activities from Stryker and consultancy fees from Adler.
Ethics approval
Given the retrospective nature of the study, which was conducted on already available data and without involving subjects, Ethics Approval was not necessary.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zambianchi, F., Bazzan, G., Marcovigi, A. et al. Joint line is restored in robotic-arm-assisted total knee arthroplasty performed with a tibia-based functional alignment. Arch Orthop Trauma Surg 141, 2175–2184 (2021). https://doi.org/10.1007/s00402-021-04039-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-04039-z