Abstract
Introduction
An increasing number of patients sustaining a fragility hip fracture (FHF) have either an active diagnosis or a history of cancer. However, little is known about the outcomes of non-malignant related FHF in this group of patients. We aimed to evaluate the mortality and complications rates during hospitalization, as well as at 1-year follow-up within this population.
Methods
A retrospective cohort study of patients 65 years of age and above, who underwent surgery for the treatment of proximal femoral fractures between January 2012 and June 2016 was conducted. Patients diagnosed with malignancies, both solid (Carcinomas) and a hematological neoplasias (Lymphomas, Multiple Myeloma) were included, along with consecutive controls without a diagnosis of cancer in the 5 years prior to the study period. Demographic, clinical and radiographic parameters were recorded and analyzed.
Results
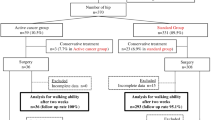
Seven hundred and fifty-two patients with FHF were included, of whom 51 had a malignancy diagnosis within the 5-year period preceding the fracture (18% metastatic disease). The mean time from malignancy diagnosis to FHF was 4.3 ± 4.8 years. Time to surgery did not differ between groups, and the vast majority of patients from both groups (over 87%) were operated within the desirable 48 h from admission. Patients with malignancy had a higher probability of being admitted to an internal medicine department both pre and post-surgically (p < 0.001), and were more susceptible to pre-operative anemia (p = 0.034). In-hospital mortality did not differ between groups, yet 1-year mortality was higher for the malignancy group (41.2% vs 19.5%, p < 0.001). At 1-year post-operatively, orthopedic complications were similar between groups.
Conclusion
Patients with a history of malignancy in the 5-years prior to a non-neoplastic FHF, showed similar mortality and complications rates during admission but increased 1 year mortality rate when compared to patients without cancer undergoing surgical treatment of a non-neoplastic proximal femoral fracture.


Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A (2016) Cancer statistics, 2016. CA Cancer J Clin 66:7–30. https://doi.org/10.3322/caac.21332
Ryerson AB, Eheman CR, Altekruse SF, Ward JW, Jemal A, Sherman RL et al (2016) Annual report to the nation on the status of cancer, 1975–2012, featuring the increasing incidence of liver cancer. Cancer 122:1312–1337. https://doi.org/10.1002/cncr.29936
Rosas S, Sabeh K, Kurowicki J, Buller L, Law TY, Roche M et al (2017) National use of total hip arthroplasty among patients with a history of breast, lung, prostate, colon or bladder cancer-an analysis of the Medicare population. Ann Transl Med 5:S34. https://doi.org/10.21037/atm.2017.11.18
Karam JA, Huang RC, Abraham JA, Parvizi J (2015) Total joint arthroplasty in cancer patients. J Arthroplasty 30:758–761. https://doi.org/10.1016/j.arth.2014.12.017
Ryan DJ, Yoshihara H, Yoneoka D, Egol KA, Zuckerman JD (2015) Delay in hip fracture surgery: an analysis of patient-specific and hospital-specific risk factors. J Orthop Trauma 29:343–348. https://doi.org/10.1097/BOT.0000000000000313
Shiga T, Wajima Z, Ohe Y (2008) Is operative delay associated with increased mortality of hip fracture patients? Systematic review, meta-analysis, and meta-regression. Can J Anaesth 55:146–154. https://doi.org/10.1007/BF03016088
Lawrence JE, Fountain DM, Cundall-Curry DJ, Carrothers AD (2017) Do patients taking warfarin experience delays to theatre, longer hospital stay, and poorer survival after hip fracture? Clin Orthop Relat Res 475:273–279. https://doi.org/10.1007/s11999-016-5056-0
White RH, Zhou H, Romano PS (2003) Incidence of symptomatic venous thromboembolism after different elective or urgent surgical procedures. Thromb Haemost 90:446–455. https://doi.org/10.1160/TH03-03-0152
Heit JA, O’Fallon WM, Petterson TM, Lohse CM, Silverstein MD, Mohr DN et al (2002) Relative impact of risk factors for deep vein thrombosis and pulmonary embolism: a population-based study. Arch Intern Med 162:1245–1248
Memtsoudis SG, Pumberger M, Ma Y, Chiu Y-L, Fritsch G, Gerner P et al (2012) Epidemiology and risk factors for perioperative mortality after total hip and knee arthroplasty. J Orthop Res 30:1811–1821. https://doi.org/10.1002/jor.22139
Mantilla CB, Wass CT, Goodrich KA, Johanns CJ, Kool ML, Zhu X et al (2011) Risk for perioperative myocardial infarction and mortality in patients undergoing hip or knee arthroplasty: the role of anemia. Transfusion 51:82–91. https://doi.org/10.1111/j.1537-2995.2010.02797.x
Bozic KJ, Lau E, Kurtz S, Ong K, Berry DJ (2012) Patient-related risk factors for postoperative mortality and periprosthetic joint infection in medicare patients undergoing TKA. Clin Orthop Relat Res 470:130–137. https://doi.org/10.1007/s11999-011-2043-3
Bozic KJ, Lau E, Kurtz S, Ong K, Rubash H, Vail TP et al (2012) Patient-related risk factors for periprosthetic joint infection and postoperative mortality following total hip arthroplasty in Medicare patients. J Bone Joint Surg Am 94:794–800. https://doi.org/10.2106/JBJS.K.00072
Leung F, Lau TW, Kwan K, Chow SP, Kung AW (2010) Does timing of surgery matter in fragility hip fractures? Osteoporos Int 21:S529–S534. https://doi.org/10.1007/s00198-010-1391-2
Eardley WG, Macleod KE, Freeman H, Tate A (2014) “Tiers of delay”: warfarin, hip fractures, and target-driven care. Geriatr Orthop Surg Rehabil 5:103–108. https://doi.org/10.1177/2151458514532469
Ftouh S, Morga A, Swift C, Group GD (2011) Management of hip fracture in adults: summary of NICE guidance. BMJ 342:d3304. https://doi.org/10.1136/bmj.d3304
Khan SK, Kalra S, Khanna A, Thiruvengada MM, Parker MJ (2009) Timing of surgery for hip fractures: a systematic review of 52 published studies involving 291,413 patients. Injury 40:692–697. https://doi.org/10.1016/j.injury.2009.01.010
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Quan H, Li B, Couris CM, Fushimi K, Graham P, Hider P et al (2011) Updating and validating the Charlson comorbidity index and score for risk adjustment in hospital discharge abstracts using data from 6 countries. Am J Epidemiol 173:676–682. https://doi.org/10.1093/aje/kwq433
Frenkel Rutenberg T, Aizer A, Levi A, Naftali N, Zeituni S, Velkes S et al (2020) Antibiotic prophylaxis as a quality of care indicator: does it help in the fight against surgical site infections following fragility hip fractures? Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-020-03682-2
Frenkel Rutenberg T, Vitenberg M, Haviv B, Velkes S (2018) Timing of physiotherapy following fragility hip fracture: delays cost lives. Arch Orthop Trauma Surg 138:1519–1524. https://doi.org/10.1007/s00402-018-3010-1
Ottanelli S (2015) Prevention and treatment of bone fragility in cancer patient. Clin Cases Miner Bone Metab Off J Ital Soc Osteoporos Miner Metab Skelet Dis 12:116–129. https://doi.org/10.11138/ccmbm/2015.12.2.116
Rachner TD, Coleman R, Hadji P, Hofbauer LC (2018) Bone health during endocrine therapy for cancer. Lancet Diabetes Endocrinol 6:901–910. https://doi.org/10.1016/S2213-8587(18)30047-0
Cianferotti L, Bertoldo F, Carini M, Kanis JA, Lapini A, Longo N et al (2017) The prevention of fragility fractures in patients with non-metastatic prostate cancer: a position statement by the international osteoporosis foundation. Oncotarget 8:75646–75663. https://doi.org/10.18632/oncotarget.17980
Peichl P, Holzer LA, Maier R, Holzer G (2011) Parathyroid hormone 1–84 accelerates fracture-healing in pubic bones of elderly osteoporotic women. J Bone Joint Surg Am 93:1583–1587. https://doi.org/10.2106/JBJS.J.01379
Suhm N, Egger A, Zech C, Eckhardt H, Morgenstern M, Gratza S (2020) Low acceptance of osteoanabolic therapy with parathyroid hormone in patients with fragility fracture of the pelvis in routine clinical practice: a retrospective observational cohort study. Arch Orthop Trauma Surg 140:321–329. https://doi.org/10.1007/s00402-019-03241-4
Leer-Salvesen S, Engesæter LB, Dybvik E, Furnes O, Kristensen TB, Gjertsen J-E (2019) Does time from fracture to surgery affect mortality and intraoperative medical complications for hip fracture patients? An observational study of 73 557 patients reported to the Norwegian hip fracture register. Bone Joint J 101:1129–1137
Dorotka R, Schoechtner H, Buchinger W (2003) The influence of immediate surgical treatment of proximal femoral fractures on mortality and quality of life. Operation within six hours of the fracture versus later than six hours. J Bone Joint Surg Br 85:1107–1113
Mitchell SM, Chung AS, Walker JB, Hustedt JW, Russell GV, Jones CB (2018) Delay in hip fracture surgery prolongs postoperative hospital length of stay but does not adversely affect outcomes at 30 days. J Orthop Trauma 32:629–633. https://doi.org/10.1097/BOT.0000000000001306
Frenkel Rutenberg T, Velkes S, Vitenberg M, Leader A, Halavy Y, Raanani P et al (2018) Morbidity and mortality after fragility hip fracture surgery in patients receiving vitamin K antagonists and direct oral anticoagulants. Thromb Res 166:106–112. https://doi.org/10.1016/j.thromres.2018.04.022
Yombi JC, Putineanu DC, Cornu O, Lavand’homme P, Cornette P, Castanares-Zapatero D (2019) Low haemoglobin at admission is associated with mortality after hip fractures in elderly patients. Bone Joint J 101:1122–1128. https://doi.org/10.1302/0301-620X.101B9.BJJ-2019-0526.R1
Sim YE, Sim SED, Seng C, Howe TS, Koh SB, Abdullah HR (2018) preoperative anemia, functional outcomes, and quality of life after hip fracture surgery. J Am Geriatr Soc 66:1524–1531. https://doi.org/10.1111/jgs.15428
Smith GH, Tsang J, Molyneux SG, White TO (2011) The hidden blood loss after hip fracture. Injury 42:133–135. https://doi.org/10.1016/j.injury.2010.02.015
Khan SK, Rushton SP, Courtney M, Gray AC, Deehan DJ (2013) Elderly men with renal dysfunction are most at risk for poor outcome after neck of femur fractures. Age Ageing 42:76–81. https://doi.org/10.1093/ageing/afs152
Porter CJ, Moppett IK, Juurlink I, Nightingale J, Moran CG, Devonald MAJ (2017) Acute and chronic kidney disease in elderly patients with hip fracture: prevalence, risk factors and outcome with development and validation of a risk prediction model for acute kidney injury. BMC Nephrol 18:20. https://doi.org/10.1186/s12882-017-0437-5
Donnellan E, Khorana AA (2017) Cancer and venous thromboembolic disease: a review. Oncologist 22:199–207. https://doi.org/10.1634/theoncologist.2016-0214
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rutenberg, T.F., Vitenberg, M., Daglan, E. et al. Do cancer patients undergoing surgery for a non-neoplastic related fragility hip fracture have worse outcomes? A retrospective study. Arch Orthop Trauma Surg 143, 9–17 (2023). https://doi.org/10.1007/s00402-021-03976-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-03976-z