Abstract
Introduction
This retrospective study was undertaken to define cut-off values for synovial fluid (SF) leukocyte count and neutrophil percentage for differentiating aseptic failure and periprosthetic joint infection (PJI) and to evaluate the diagnostic accuracy of blood inflammatory markers, and microbiological testing according to the criteria proposed by the International Consensus Meeting (ICM) of Philadelphia.
Methods
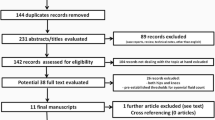
All patients who underwent revision total knee arthroplasty from January 2010 to July 2015 were included: we identified and classified 31 PJIs and 136 aseptic joints. The diagnostic performance of single test was assessed by receiver operating characteristic curve analyses. The sensitivity and specificity were calculated for each of the cut-off values and the area under the curve (AUC) was calculated.
Results
The median SF leukocyte count as well as the neutrophil percentage and inflammatory markers were significantly higher in patients with PJI than in those with aseptic failure (p < 0.001). A leukocyte count of > 2.8 × 103/μL had a sensitivity of 83.8% and a specificity of 89.7% whereas a neutrophil percentage of > 72% yielded a marginally higher sensitivity of 84% and a specificity of 91%. Applying the ICM criteria we found a significant correlation between all these diagnostic measures and PJI (p < 0.001) except for a single positive culture. The most accurate criterion of the ICM was the synovial neutrophil differential (AUC = 0.89; 95% CI 0.81–0.97), followed by SF leukocyte count (AUC = 0.86; 95% CI 0.78–0.94), increased inflammatory markers (AUC = 0.85; 95% CI 0.76–0.93), and two positive periprosthetic cultures (AUC = 0.84; 95% CI 0.73–0.94). The presence of sinus tract communicating with the joint and a single positive culture showed unfavourable diagnostic accuracy (AUC = 0.60, 95% CI 0.47–0.72; AUC = 0.49, 95% CI 0.38–0.61, respectively)
Conclusions
The present study highlights the adequate ability of fluid cell count and neutrophil differential to distinguish between PJI and aseptic loosening. The clinical utility of fluid analysis in diagnosing infection can be improved by evaluation of other diagnostic criteria.
Level of evidence
Level I Diagnostic Study.


Similar content being viewed by others
References
Lavernia C, Lee DJ, Hernandez VH (2006) The increasing financial burden of knee revision surgery in the United States. Clin Orthop Relat Res 446:221–226
Zmistowski B, Karam JA, Durinka JB, Casper DS, Parvizi J (2013) Periprosthetic joint infection increases the risk of one-year mortality. J Bone Joint Surg Am 95:2177–2184
Springer BD (2015) The diagnosis of periprosthetic joint infection. J Arthroplast 30:908–911
Bozic KJ, Kurtz SM, Lau E, Ong K, Chiu V, Vail TP, Rubash HE, Berry DJ (2010) The epidemiology of revision total knee arthroplasty in the United States. Clin Orthop Relat Res 468:45–51
Bozic KJ, Kurtz SM, Lau E, Ong K, Vail TP, Berry DJ (2009) The epidemiology of revision total hip arthroplasty in the United States. J Bone Joint Surg Am 91:128–133
Murgier J, Laffosse JM, Cailliez J, Cavaignac E, Murgier P, Bayle-Iniguez X, Chiron P, Bonnevialle P (2016) Is the prognosis the same for periprosthetic joint infections due to Staphylococcus aureus versus coagulase-negative staphylococci? A retrospective study of 101 patients with 2-year minimum follow-up. Arch Orthop Trauma Surg 136:1357–1361
Di Benedetto P, Di Benedetto ED, Buttironi MM, De Franceschi D, Beltrame A, Gissoni R, Cainero V, Causero A (2017) Two-stage revision after total knee arthroplasty. Acta Biomed 88:92–97
Hossain F, Patel S, Haddad FS (2010) Midterm assessment of causes and results of revision total knee arthroplasty. Clin Orthop Relat Res 468:1221–1228
Kim YH, Park JW, Kim JS, Kim DJ (2015) The outcome of infected total knee arthroplasty: culture-positive versus culture-negative. Arch Orthop Trauma Surg 135:1459–1467
Windisch C, Brodt S, Roehner E, Matziolis G (2017) C-reactive protein course during the first 5 days after total knee arthroplasty cannot predict early prosthetic joint infection. Arch Orthop Trauma Surg 137:1115–1119
Janz V, Wassilew GI, Kribus M, Trampuz A, Perka C (2015) Improved identification of polymicrobial infection in total knee arthroplasty through sonicate fluid cultures. Arch Orthop Trauma Surg 135:1453–1457
Parvizi J, Zmistowski B, Berbari EF, Bauer TW, Springer BD, Della Valle CJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG (2011) New definition for periprosthetic joint infection: from the Workgroup of the Musculoskeletal Infection Society. Clin Orthop Relat Res 469:2992–2994
Parvizi J, Gehrke T (2014) International Consensus Group on Periprosthetic Joint Infection Definition of periprosthetic joint infection. J Arthroplast 29:1331
Trampuz A, Hanssen AD, Osmon DR, Mandrekar J, Steckelberg JM, Patel R (2014) Synovial fluid leukocyte count and differential for the diagnosis of prosthetic knee infection. Am J Med 117:556–562
Ghanem E, Parvizi J, Burnett RS, Sharkey PF, Keshavarzi N, Aggarwal A, Barrack RL (2008) Cell count and differential of aspirated fluid in the diagnosis of infection at the site of total knee arthroplasty. J Bone Joint Surg Am 90:1637–1643
Schinsky MF, Della Valle CJ, Sporer SM, Paprosky WG (2008) Perioperative testing for joint infection in patients undergoing revision total hip arthroplasty. J Bone Joint Surg Am 90:1869–1875
Dinneen A, Guyot A, Clements J, Bradley N (2013) Synovial fluid white cell and differential count in the diagnosis or exclusion of prosthetic joint infection. Bone Joint J 95-B:554–557
Shukla SK, Ward JP, Jacofsky MC, Sporer SM, Paprosky WG, Della Valle CJ (2010) Perioperative testing for persistent sepsis following resection arthroplasty of the hip for periprosthetic infection. J Arthroplast 25:87–91
Zmistowski B, Restrepo C, Huang R, Hozack WJ, Parvizi J (2012) Periprosthetic joint infection diagnosis: a complete understanding of white blood cell count and differential. J Arthroplast 27:1589–1593
Nilsdotter-Augustinsson A, Briheim G, Herder A, Ljunghusen O, Wahlström O, Ohman L (2007) Inflammatory response in 85 patients with loosened hip prostheses: a prospective study comparing inflammatory markers in patients with aseptic and septic prosthetic loosening. Acta Orthop 78:629–639
Ahmad SS, Shaker A, Saffarini M, Chen AF, Hirschmann MT, Kohl S (2016) Accuracy of diagnostic tests for prosthetic joint infection: a systematic review. Knee Surg Sports Traumatol Arthrosc 24:3064–3074
Bauer TW, Parvizi J, Kobayashi N, Krebs V (2006) Diagnosis of periprosthetic infection. J Bone Joint Surg Am 88:869–882
Toms AD, Davidson D, Masri BA, Duncan CPP (2006) The management of peri-prosthetic infection in total joint arthroplasty. J Bone Joint Surg Br 88:149–155
Kersey R, Benjamin J, Marson B (2000) White blood cell counts and differential in synovial fluid of aseptically failed total knee arthroplasty. J Arthroplast 15:301–304
Spangehl MJ, Masri BA, O’Connell JX, Duncan CP (1999) Prospective analysis of preoperative and intraoperative investigations for the diagnosis of infection at the sites of two hundred and two revision total hip arthroplasties. J Bone Joint Surg Am 81:672–683
Cats-Baril W, Gehrke T, Huff K, Kendoff D, Maltenfort M, Parvizi J (2013) International consensus on periprosthetic joint infection: description of the consensus process. Clin Orthop Relat Res 471:4065–4075
Ascione T, Pagliano P, Balato G, Mariconda M, Rotondo R, Esposito S (2017) Oral therapy, microbiological findings, and comorbidity influence the outcome of prosthetic joint infections undergoing 2-stage exchange. J Arthroplast 32:2239–2243
Gomez E, Cazanave C, Cunningham SA, Greenwood-Quaintance KE, Steckelberg JM, Uhl JR, Hanssen AD, Karau MJ, Schmidt SM, Osmon DR, Berbari EF, Mandrekar J, Patel R (2015) Prosthetic joint infection diagnosis using broad-range PCR of biofilms dislodged from knee and hip arthroplasty surfaces using sonication. J Clin Microbiol 50:3501–3508
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors have no conflict of interest to declare.
Funding
Authors received no funding for this project.
Rights and permissions
About this article
Cite this article
Balato, G., Franceschini, V., Ascione, T. et al. Diagnostic accuracy of synovial fluid, blood markers, and microbiological testing in chronic knee prosthetic infections. Arch Orthop Trauma Surg 138, 165–171 (2018). https://doi.org/10.1007/s00402-017-2832-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-017-2832-6