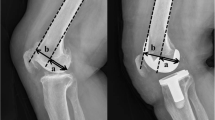
Abstract
Introduction
There is no algorithm for the management of joint stability in midflexion up to now. Change in the joint line (JL) is considered to be the primary cause, although it only determines the extension gap. The purpose of this study was to determine the influence of the posterior condylar offsets (PCO), which defines the flexion gap, on midflexion instability.
Materials and methods
Forty-two knee joints (38 patients) were included in this study, patients undergoing navigated total knee arthroplasty due to primary osteoarthritis of the knee. Changes in the JL and the PCO were determined from the navigation data. A gap tensioning device was used to determine the width of the joint gap at −5°, 0°, 30° and 60° intraoperatively.
Results
Within a range between 5 mm proximalization and 2 mm distalization, the JL had no influence on stability in midflexion. In contrast to this, both an increase and a decrease in PCO led to midflexion instability (R = 0.361, p = 0.019). In 16 cases (38%), the PCO was changed by more than 2 mm. This led to a midflexion instability of more than 2 mm in seven of these cases (44%).
Conclusions
Whereas the joint line can be displaced by up to 5 mm without measurable changes in joint stability, reconstruction of the posterior offset within a tight range of 2 mm is necessary to avoid midflexion instability.



Similar content being viewed by others
References
Thiele K, Perka C, Matziolis G et al (2015) Current failure mechanisms after knee arthroplasty have changed: polyethylene wear is less common in revision surgery. J Bone Jt Surg Am 97:715–720. doi:10.2106/JBJS.M.01534
Sharkey PF, Lichstein PM, Shen C et al (2014) Why are total knee arthroplasties failing today–has anything changed after 10 years? J Arthroplasty 29:1774–1778. doi:10.1016/j.arth.2013.07.024
Pang H-N, Yeo S-J, Chong H-C et al (2013) Joint line changes and outcomes in constrained versus unconstrained total knee arthroplasty for the type II valgus knee. Knee Surg Sports Traumatol Arthrosc 21:2363–2369. doi:10.1007/s00167-013-2390-6
Kazemi SM, Daftari Besheli L, Eajazi A et al (2011) Pseudo-patella baja after total knee arthroplasty. Med Sci Monit 17:CR292–C6
Hofmann AA, Kurtin SM, Lyons S et al (2006) Clinical and radiographic analysis of accurate restoration of the joint line in revision total knee arthroplasty. J Arthroplasty 21:1154–1162. doi:10.1016/j.arth.2005.10.026
Cross MB, Nam D, Plaskos C et al (2012) Recutting the distal femur to increase maximal knee extension during TKA causes coronal plane laxity in mid-flexion. Knee 19:875–879. doi:10.1016/j.knee.2012.05.007
Martin JW, Whiteside LA (1990) The influence of joint line position on knee stability after condylar knee arthroplasty. Clin Orthop Relat Res 146–156
König C, Matziolis G, Sharenkov A et al (2011) Collateral ligament length change patterns after joint line elevation may not explain midflexion instability following TKA. Med Eng Phys 33:1303–1308. doi:10.1016/j.medengphy.2011.06.008
König C, Sharenkov A, Matziolis G et al (2010) Joint line elevation in revision TKA leads to increased patellofemoral contact forces. J Orthop Res 28:1–5. doi:10.1002/jor.20952
Fornalski S, McGarry MH, Bui CNH et al (2012) Biomechanical effects of joint line elevation in total knee arthroplasty. Clin Biomech (Bristol Avon) 27:824–829. doi:10.1016/j.clinbiomech.2012.05.009
Yoon J-R, Jeong H-I, Oh K-J, Yang J-H (2013) In vivo gap analysis in various knee flexion angles during navigation-assisted total knee arthroplasty. J Arthroplasty 28:1796–1800. doi:10.1016/j.arth.2013.04.043
Bellemans J, Banks S, Victor J et al (2002) Fluoroscopic analysis of the kinematics of deep flexion in total knee arthroplasty. Influence of posterior condylar offset. J Bone Jt Surg Br 84:50–53
Kim J-H (2013) Effect of posterior femoral condylar offset and posterior tibial slope on maximal flexion angle of the knee in posterior cruciate ligament sacrificing total knee arthroplasty. Knee Surg Relat Res 25:54–59. doi:10.5792/ksrr.2013.25.2.54
Ishii Y, Noguchi H, Takeda M et al (2013) Posterior condylar offset does not correlate with knee flexion after TKA. Clin Orthop Relat Res 471:2995–3001. doi:10.1007/s11999-013-2999-2
Bauer T, Biau D, Colmar M et al (2010) Influence of posterior condylar offset on knee flexion after cruciate-sacrificing mobile-bearing total knee replacement: a prospective analysis of 410 consecutive cases. Knee 17:375–380. doi:10.1016/j.knee.2009.11.001
Hanratty BM, Thompson NW, Wilson RK, Beverland DE (2007) The influence of posterior condylar offset on knee flexion after total knee replacement using a cruciate-sacrificing mobile-bearing implant. J Bone Jt Surg Br 89:915–918. doi:10.1302/0301-620X.89B7.18920
Lo C-S, Wang S-J, Wu S-S (2003) Knee stiffness on extension caused by an oversized femoral component after total knee arthroplasty: a report of two cases and a review of the literature. J Arthroplasty 18:804–808
Mizu-Uchi H, Colwell CW, Fukagawa S et al (2012) The importance of bony impingement in restricting flexion after total knee arthroplasty: computer simulation model with clinical correlation. J Arthroplasty 27:1710–1716. doi:10.1016/j.arth.2012.03.041
Servien E, Viskontas D, Giuffrè BM et al (2008) Reliability of bony landmarks for restoration of the joint line in revision knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 16:263–269. doi:10.1007/s00167-007-0449-y
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflict of interest.
There is no funding source.
All included data were from patients that where untreated controls from a previous randomized controlled trial (clinicaltrials.gov registration number NCT02450409), so that a separate ethical approval was not necessary for this study. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Matziolis, G., Brodt, S., Windisch, C. et al. Changes of posterior condylar offset results in midflexion instability in single-radius total knee arthroplasty. Arch Orthop Trauma Surg 137, 713–717 (2017). https://doi.org/10.1007/s00402-017-2671-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-017-2671-5