Abstract
Introduction
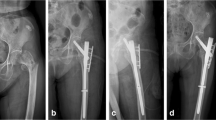
Intramedullary nail fixation is a useful treatment option for A3 intertrochanteric fractures. Occasionally, we have encountered displaced lateral femoral wall (LFW) fragment during surgery with intramedullary nail system. We investigated the postoperative spontaneous reduction of displaced LFW fragments without further fixation and the factors that affected the spontaneous reduction of displaced LFW fragments.
Materials and methods
Forty-four patients with A3.3 intertrochanteric fracture were treated by surgery using intramedullary nails (PFNA; Synthes, Paoli) between March 2007 and December 2012. All patients had a minimum follow-up period of 12 months. We calculated the amount of spontaneous reduction of the displaced LFW fragments from immediate postoperative and last follow-up anteroposterior radiographs. We measured the tilting angle of the LFW fragment, tip–apex distance (TAD), and telescoping of the blade, and evaluated the quality of postoperative reduction.
Results
Twenty-five of the 44 patients had displaced LFW fragments, and the average amount of spontaneous reduction of the displaced LFW fragment was 4.8 mm with statistical significance (p = 0.005). The average tilting angle of all patients was −4.97°, telescoping was 6.83 mm, and TAD was 19.77 mm. Twenty-one patients had good quality of reduction, 21 had acceptable quality, and 2 had poor quality. Multivariate logistic regression analysis for these factors indicated that tilting angle was the only significant factor related to spontaneous reduction of a displaced LFW fragment (p = 0.007, odds ratio = 1.336).
Conclusions
In intramedullary nailing of A3.3 intertrochanteric fractures, the displaced LFW fragments tend to reduce spontaneously without any additional fixation during the postoperative period. We conclude that no additional fixation is needed for the displaced LFW fragment after surgery with intramedullary nail.







Similar content being viewed by others
References
Desjardins AL, Roy A, Paiement G, Newman N, Pedlow F, Desloges D, Turcotte RE (1993) Unstable intertrochanteric fracture of the femur. A prospective randomised study comparing anatomical reduction and medial displacement osteotomy. J Bone Joint Surg Br 75:445–447
Adams CI, Robinson CM, Court-Brown CM, McQueen MM (2001) Prospective randomized controlled trial of an intramedullary nail versus dynamic screw and plate for intertrochanteric fractures of the femur. J Orthop Trauma 15:394–400
Bartonicek I, Dousa P (2002) Prospective randomized controlled trial of an intramedullary nail versus dynamic screw and plate of intertrochanteric fractures of the femur. J Orthop Trauma 16:363–364 (author reply 364)
Gotfried Y (2004) The lateral trochanteric wall: a key element in the reconstruction of unstable pertrochanteric hip fractures. Clin Orthop Relat Res 425:82–86
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, Prokuski L, Sirkin M, Ziran B, Henley B, Audigé L (2007) Fracture and dislocation classification compendium—2007: orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma 21:S1–133
Baixauli F, Vicent V, Baixauli E, Serra V, Sánchez-Alepuz E, Gómez V, Martos F (1999) A reinforced rigid fixation device for unstable intertrochanteric fractures. Clin Orthop Relat Res 361:205–215
Müller-Färber J, Wittner B, Reichel R (1988) Late results in the management of pertrochanteric femoral fractures in the elderly with the dynamic hip screw. Unfallchirurg 91:341–350
Babst R, Renner N, Biedermann M, Rosso R, Heberer M, Harder F, Regazzoni P (1998) Clinical results using the trochanter stabilizing plate (TSP): the modular extension of the dynamic hip screw (DHS) for internal fixation of selected unstable intertrochanteric fractures. J Orthop Trauma 12:392–399
Gupta RK, Sangwan K, Kamboj P, Punia SS, Walecha P (2010) Unstable trochanteric fractures: the role of lateral wall reconstruction. Int Orthop 34:125–129. doi:10.1007/s00264-009-0744-y
Haidukewych GJ, Israel TA, Berry DJ (2001) Reverse obliquity fractures of the intertrochanteric region of the femur. J Bone Joint Surg Am 83-A:643–650
Ruecker AH, Rupprecht M, Gruber M, Gebauer M, Barvencik F, Briem D, Rueger JM (2009) The treatment of intertrochanteric fractures: results using an intramedullary nail with integrated cephalocervical screws and linear compression. J Orthop Trauma 23:22–30. doi:10.1097/BOT.0b013e31819211b2
Sadowski C, Lübbeke A, Saudan M, Riand N, Stern R, Hoffmeyer P (2002) Treatment of reverse oblique and transverse intertrochanteric fractures with use of an intramedullary nail or a 95 degrees screw-plate: a prospective, randomized study. J Bone Joint Surg Am 84-A:372–381
Hardy DC, Descamps PY, Krallis P, Fabeck L, Smets P, Bertens CL, Delince PE (1998) Use of an intramedullary hip-screw compared with a compression hip-screw with a plate for intertrochanteric femoral fractures. A prospective, randomized study of one hundred patients. J Bone Joint Surg Am 80:618–630
Baumgaertner MR, Curtin SL, Lindskog DM, Keggi JM (1995) The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip. J Bone Joint Surg Am 77:1058–1064
Gardner MJ, Bhandari M, Lawrence BD, Helfet DL, Lorich DG (2005) Treatment of intertrochanteric hip fractures with the AO trochanteric fixation nail. Orthopedics 28:117–122
Baumgaertner MR, Curtin SL, Lindskog DM (1998) Intramedullary versus extramedullary fixation for the treatment of intertrochanteric hip fractures. Clin Orthop Relat Res 348:87–94
Kim Y, Dheep K, Lee J, Yoon Y-C, Shon W-Y, Oh C-W, Oh J-K (2014) Hook leverage technique for reduction of intertrochanteric fracture. Injury 45:1006–1010. doi:10.1016/j.injury.2014.02.007
Streubel PN, Moustoukas MJ, Obremskey WT (2013) Mechanical failure after locking plate fixation of unstable intertrochanteric femur fractures. J Orthop Trauma 27:22–28. doi:10.1097/BOT.0b013e318251930d
Wirtz C, Abbassi F, Evangelopoulos DS, Kohl S, Siebenrock KA, Krüger A (2013) High failure rate of trochanteric fracture osteosynthesis with proximal femoral locking compression plate. Injury 44:751–756. doi:10.1016/j.injury.2013.02.020
Palm H, Jacobsen S, Sonne-Holm S, Gebuhr P (2007) Integrity of the lateral femoral wall in intertrochanteric hip fractures: an important predictor of a reoperation. J Bone Joint Surg Am 89:470–475. doi:10.2106/JBJS.F.00679
Boopalan PRJVC, Oh J-K, Kim T-Y, Oh C-W, Cho J-W, Shon W-Y (2012) Incidence and radiologic outcome of intraoperative lateral wall fractures in OTA 31A1 and A2 fractures treated with cephalomedullary nailing. J Orthop Trauma 26:638–642. doi:10.1097/BOT.0b013e318244e5ad
Gardner MJ, Briggs SM, Kopjar B, Helfet DL, Lorich DG (2007) Radiographic outcomes of intertrochanteric hip fractures treated with the trochanteric fixation nail. Injury 38:1189–1196. doi:10.1016/j.injury.2007.03.014
Haidukewych GJ (2009) Intertrochanteric fractures: ten tips to improve results. J Bone Joint Surg Am 91:712–719
Baumgaertner MR, Solberg BD (1997) Awareness of tip-apex distance reduces failure of fixation of trochanteric fractures of the hip. J Bone Joint Surg Br 79:969–971
Guerra Pinto F, Dantas P, Moreira R, Mamede R, Amaral LB (2010) Complications relating to accuracy of reduction of intertrochanteric fractures treated with a compressive hip screw. Hip Int 20:221–228
Schindeler A, McDonald MM, Bokko P, Little DG (2008) Bone remodeling during fracture repair: the cellular picture. Semin Cell Dev Biol 19:459–466. doi:10.1016/j.semcdb.2008.07.004
Acknowledgments
This study was presented and nominated for the award of Young Investigator at the Second AO Trauma Asia Pacific Scientific Congress and TK Experts’ Symposium 2014, Seoul, Republic of Korea.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kim, Y., Bahk, W.J., Yoon, YC. et al. Radiologic healing of lateral femoral wall fragments after intramedullary nail fixation for A3.3 intertrochanteric fractures. Arch Orthop Trauma Surg 135, 1349–1356 (2015). https://doi.org/10.1007/s00402-015-2284-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-015-2284-9