Abstract
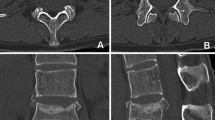
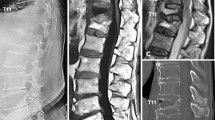
We report on a 43-year-old male who sustained an isolated distraction injury of the thoracic spine Th7/Th8 (AO/ASIF B 2.3) with wedge compression Th8 and sagittal split Th10 without neurological injury. A bisegmental posterior stabilisation and a monosegmental interlaminar fusion was the treatment of choice. A synthetic bone substitute, β-tricalcium phosphate (β-TCP, Chronos™) without additional autogenous bone was used to achieve the monosegmental posterior fusion. The clinical course was favourable and 10 months postoperatively the implant was removed. On implant removal the CT scan showed a fused segment and intraoperatively it was found that the fusion was solidly healed. A biopsy was taken from the fusion mass and histology showed vital bone that was rich with osteocytes. Noncalcified osteoid surrounding the bone marrow cavity could be identified. Several studies and the reported case might indicate that osteoconductive material alone can be sufficient for achieving a solid fusion.





Similar content being viewed by others
Notes
Synthes, Oberdorf, Switzerland
References
Banwart JC, Asher MA, Hassanein RS (1995) Iliac crest bone graft harvest donor site morbidity. A statistical evaluation. Spine 20(9):1055–1060
Delecrin J, Takahashi S, Gouin F, Passuti N (2000) A synthetic porous ceramic as a bone graft substitute in the surgical management of scoliosis - A prospective, randomized study. Spine 25(5):563–569
Erbe EM, Marx JG, Clineff TD, Bellincampi LD (2001) Potential of an ultra porous b-tricalcium phosphate synthetic cancellous bone void filler and bone marrow aspirate composite graft In: Gunzburg R, Szpalski M, Passuti N, Aebi M (Hrsg.) The use of Bone Substitutes in Spine Surgery - a state of the art review, 1. Aufl., Springer, Berlin Heidelberg New York Barcelona Hong Kong London Milan Paris Tokyo:57–62
Goulet JA, Senunas LE, De Silva GL, Greenfield ML (1997) Autogenous iliac crest bone graft. Complications and functional assessment. Clin Orthop 339:76–81
Kai T, Shao-qing G, Geng-ting D (2003) In vivo evaluation of bone marrow stromal-derived osteoblasts-porous calcium phosphate ceramic composites as bone graft substitute for lumbar intervertebral spinal fusion. Spine 28(15):1653–1658
Kurz LT, Garfin SR, Booth RE Jr (1989) Harvesting autogenous iliac bone grafts. A review of complications and techniques. Spine 14(12):1324–1331
Li HS, Zou XN, Xue QY, Egund N, Lind M, Bunger C (2004) Anterior lumbar interbody fusion with carbon fiber cage loaded with bioceramics and platelet-rich plasma. An experimental study on pigs. Eur Spine J 13(4):354–358
Magerl F, Aebi M, Gertzbein SD, Harms J, Nazarian S (1994) A comprehensive classification of thoracic and lumbar injuries. Eur Spine J 3(4):184–201
Muschik M, Ludwig R, Halbhübner S, Bursche K, Stoll T (2001) b-tricalcium phosphate as a bone substitute for dorsal spinal fusion in adolescent idiopathic scoliosis: preliminary results of a prospective clinical study. Eur Spine J 10(Suppl. 2):S178–S184
Passuti N, Daculsi G, Rogez JM, Martin S, Bainvel JV (1989) Macro porous calcium phosphate ceramic performance in human spine fusion. Clin Orthop 248:169–176
Ransford AO, Morley T, Edgar MA, Webb P et al (1998) Synthetic porous ceramic compared with auto graft in scoliosis surgery. A prospective, randomized study of 341 patients. J Bone Joint Surg Br 80(1):13–18
Sasso RC, Williams JI, Dimasi N, Meyer-PR J (1998) Postoperative drains at the donor sites of iliac-crest bone grafts. A prospective, randomized study of morbidity at the donor site in patients who had a traumatic injury of the spine. J Bone Joint Surg Am 80(5):631–635
Sawin PD, Traynelis VC, Menezes AH (1998) A comparative analysis of fusion rates and donor-site morbidity for autogeneic rib and iliac crest bone grafts in posterior cervical fusions. J Neurosurg 88(2):255–265
Schnee CL, Freese A, Weil RJ, Marcotte PJ (1997) Analysis of harvest morbidity and radiographic outcome using auto graft for anterior cervical fusion. Spine 22(19):2222–2227
Steffen T, Stoll T, Arvinte T, Schenk RK (2001) Porous tricalcium phosphate and transforming growth factor used for anterior spine surgery. Eur Spine J 10(Suppl. 2):S132–S140
Suh DY, Boden SD, Louis-Ugbo J, Mayr M et al (2002) Delivery of recombinant human bone morphogenetic protein-2 using a compression-resistant matrix in posterolateral spine fusion in the rabbit and in the non-human primate. Spine 27(4):353–360
Walsh WR, Harrison J, Loefler A, Martin T et al (2000) Mechanical and histologic evaluation of Collagraft (R) in an ovine lumbar fusion model. Clin Orthop Relat Res (375):258–266
Younger EM, Chapman MW (1989) Morbidity at bone graft donor sites. J Orthop Trauma 3(3):192–195
Zerwek J, Kourosh S, Scheinberg R (1992) Fibrillar collagen: biphasic calcium phosphate composite as a bone graft substitute for spinal fusion. J Orthop Res 10:562–572
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Knop, C., Sitte, I., Canto, F. et al. Successful posterior interlaminar fusion at the thoracic spine by sole use of β-tricalcium phosphate. Arch Orthop Trauma Surg 126, 204–210 (2006). https://doi.org/10.1007/s00402-006-0107-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-006-0107-8