Abstract
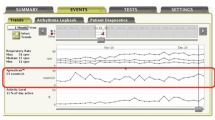
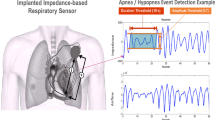
Pacemaker apnea scan algorithms are able to screen for sleep apnea. We investigated whether these systems were able to accurately detect sleep-disordered breathing (SDB) in two patients from an outpatient clinic. The first patient suffered from ischemic heart failure and severe central sleep apnea (CSA) and underwent adaptive servoventilation therapy (ASV). The second patient suffered from dilated cardiomyopathy and moderate obstructive sleep apnea (OSA). Pacemaker read-outs did not match polysomnography (PSG) recordings well and overestimated the apnea–hypopnea index. However, ASV therapy-induced SDB improvements were adequately recognized by the apnea scan of the Boston Scientific INVIVE® cardiac resynchronization therapy pacemaker. Detection of obstructive respiratory events using impedance-based technology may underestimate the number of events, as frustrane breathing efforts induce impedance changes without significant airflow. By contrast, in the second case, apnea scan overestimated the number of total events and of obstructive events, perhaps owing to a very sensitive but less specific hypopnea definition and detection within the diagnostic algorithm of the device. These two cases show that a pacemaker apnea scan is able to reflect SDB, but PSG precision is not met by far. The device scan revealed the decline of SDB through ASV therapy for CSA in one patient, but not for OSA in the second case. To achieve reliable monitoring of SDB, further technical developments and clinical studies are necessary.
Zusammenfassung
Schrittmacher-Apnoescan-Algorithmen können zum Apnoe-Screening genutzt werden. Wir untersuchten, ob diese Systeme zuverlässig für die Erkennung schlafbezogener Atemstörungen sind bei 2 Patienten unserer Ambulanz. Der erste Patient hatte eine ischämische Kardiomyopathie, schwere zentrale Schlafapnoe (ZSA) und erhielt eine adaptive Servoventilationstherapie (ASV). Der zweite Patient hatte eine dilatative Kardiomyopathie und ein mittelgradiges obstruktives Schlafapnoe-Syndrom (OSAS). Die Schrittmacher-Ausdrucke korrelierten nicht gut mit der Polysomnographie (PSG) und überschätzten den Apnoe-Hypopnoe-Index (AHI). ASV-Therapie-induzierte Verbesserungen der Schlafapnoe wurden jedoch adäquat durch den Apnoe-Scan des CRT-Schrittmachers erkannt. Die Anzahl obstruktiver Atemereignisse kann durch Impedanz-messende Algorithmen unterschätzt werden, da frustrane Atemmanöver Impedanzänderungen verursachen ohne signifikanten Luftstrom. Auf der anderen Seite zeigt der 2. Fall, dass der Apnoe-Scan die Anzahl aller Ereignisse und aller obstruktiven Ereignisse überschätzen kann, am ehesten aufgrund einer zu sensitiven und zu unspezifischen Definition der Hypopnoe und -Detektion in diesem diagnostischen Device-Algorithmus. Diese 2 Fälle zeigen, dass Schrittmacher Apnoe-Scans in der Lage sind, schlafbezogene Atemstörungen zu erkennen, jedoch mit einer Präzision weit unter der Polysomnographie. Der Device-Scan erkannte die Abnahme der Schlafapnoe durch ASV-Therapie bei ZSA bei einem Patienten, jedoch nicht für OSAS im zweiten Fall. Um Schlafapnoe zuverlässig monitoren zu können, sind weitere technische Verbesserungen und klinische Studien notwendig.
Similar content being viewed by others
References
Jilek C, Krenn M, Sebah D, Obermeier R, Braune A, Kehl V, Schroll S, Montalvan S, Riegger GA, Pfeifer M, Arzt M (2011) Prognostic impact of sleep disordered breathing and its treatment in heart failure: an observational study. Eur J Heart Fail 13:68–75
Oldenburg O, Lamp B, Faber L, Teschler H, Horstkotte D, Töpfer V (2007) Sleep-disordered breathing in patients with symptomatic heart failure: a contemporary study of prevalence in and characteristics of 700 patients. Eur J Heart Fail 9:251–257
Javaheri S, Shukla R, Zeigler H, Wexler L (2007) Central sleep apnea, right ventricular dysfunction, and low diastolic blood pressure are predictors of mortality in systolic heart failure. J Am Coll Cardiol 49:2028–2034
Jelic S, Le Jemtel TH (2009) Sleep-disordered breathing in acute decompensated heart failure. Curr Heart Fail Rep 6:169–175
Defaye P, Pepin JL, Poezevara Y, Mabo P, Murgatroyd F, Lévy P, Garrigue S (2004) Automatic recognition of abnormal respiratory events during sleep by a pacemaker transthoracic impedance sensor. J Cardiovasc Electrophysiol 15:1034–1040
Shalaby A, Atwood C, Hansen C, Konermann M, Jamnadas P, Lee K, Willems R, Hartley J, Stahmann J, Kwok J, Ni Q, Neuzner J (2006) Feasibility of automated detection of advanced sleep disordered breathing utilizing an implantable pacemaker ventilation sensor. Pacing Clin Electrophysiol 29:1036–1043
Meoli AL, Casey KR, Clark RW, Coleman JA Jr, Fayle RW, Troell RJ, Iber C, Clinical Practice Review Committee (2001) Hypopnea in sleep-disordered breathing in adults. Sleep 24:469–470
Efken C, Bitter T, Prib N, Horstkotte D, Oldenburg O (2013) Obstructive sleep apnoea: longer respiratory event lengths in patients with heart failure. Eur Resp J 41:1340–1346
Wedewardt J, Bitter T, Prinz C, Faber L, Horstkotte D, Oldenburg O (2010) Cheyne-Stokes respiration in heart failure: cycle length is dependent on left ventricular ejection fraction. Sleep Med 11:137–142
Berry RB, Budhiraja R, Gottlieb DJ, Gozal D, Iber C, Kapur VK, Marcus CL, Mehra R, Parthasarathy S, Quan SF, Redline S, Strohl KP, Davidson Ward SL, Tangredi MM, American Academy of Sleep Medicine (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM Manual for the Scoring of Sleep and Associated Events. Deliberations of the sleep apnea definitions task force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
Conflict of interest
H. Fox, G. Nölker, K-J. Gutleben, T. Bitter, D. Horstkotte, and O. Oldenburg state that there are no conflicts of interest.
This article does not contain any studies with human or animal subjects.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fox, H., Nölker, G., Gutleben, KJ. et al. Reliability and accuracy of sleep apnea scans in novel cardiac resynchronization therapy devices: an independent report of two cases. Herzschr Elektrophys 25, 53–55 (2014). https://doi.org/10.1007/s00399-014-0298-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00399-014-0298-6