Abstract
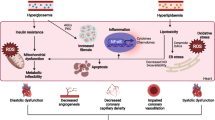
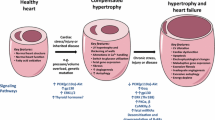
Coronary microvascular dysfunction is prevalent among people with diabetes and is correlated with cardiac mortality. Compromised endothelial-dependent dilation (EDD) is an early event in the progression of diabetes, but its mechanisms remain incompletely understood. Nitric oxide (NO) is the major endothelium-dependent vasodilatory metabolite in the healthy coronary circulation, but this switches to hydrogen peroxide (H2O2) in coronary artery disease (CAD) patients. Because diabetes is a significant risk factor for CAD, we hypothesized that a similar NO-to-H2O2 switch would occur in diabetes. Vasodilation was measured ex vivo in isolated coronary arteries from wild type (WT) and microRNA-21 (miR-21) null mice on a chow or high-fat/high-sugar diet, and B6.BKS(D)-Leprdb/J (db/db) mice using myography. Myocardial blood flow (MBF), blood pressure, and heart rate were measured in vivo using contrast echocardiography and a solid-state pressure sensor catheter. RNA from coronary arteries, endothelial cells, and cardiac tissues was analyzed via quantitative real-time PCR for gene expression, and cardiac protein expression was assessed via western blot analyses. Superoxide was detected via electron paramagnetic resonance. (1) Ex vivo coronary EDD and in vivo MBF were impaired in diabetic mice. (2) Nω-Nitro-L-arginine methyl ester, an NO synthase inhibitor (L-NAME), inhibited ex vivo coronary EDD and in vivo MBF in WT. In contrast, polyethylene glycol-catalase, an H2O2 scavenger (Peg-Cat), inhibited diabetic mouse EDD ex vivo and MBF in vivo. (3) miR-21 was upregulated in diabetic mouse endothelial cells, and the deficiency of miR-21 prevented the NO-to-H2O2 switch and ameliorated diabetic mouse vasodilation impairments. (4) Diabetic mice displayed increased serum NO and H2O2, upregulated mRNA expression of Sod1, Sod2, iNos, and Cav1, and downregulated Pgc-1α in coronary arteries, but the deficiency of miR-21 reversed these changes. (5) miR-21-deficient mice exhibited increased cardiac PGC-1α, PPARα and eNOS protein and reduced endothelial superoxide. (6) Inhibition of PGC-1α changed the mRNA expression of genes regulated by miR-21, and overexpression of PGC-1α decreased the expression of miR-21 in high (25.5 mM) glucose treated coronary endothelial cells. Diabetic mice exhibit a NO-to-H2O2 switch in the mediator of coronary EDD, which contributes to microvascular dysfunction and is mediated by miR-21. This study represents the first mouse model recapitulating the NO-to-H2O2 switch seen in CAD patients in diabetes.










Similar content being viewed by others
References
Allaqaband H, Gutterman DD, Kadlec AO (2018) Physiological consequences of coronary arteriolar dysfunction and its influence on cardiovascular disease. Physiology (Bethesda) 33:338–347. https://doi.org/10.1152/physiol.00019.2018
Andes LJ, Cheng YJ, Rolka DB, Gregg EW, Imperatore G (2020) Prevalence of prediabetes among adolescents and young adults in the United States, 2005–2016. JAMA Pediatr 174:e194498. https://doi.org/10.1001/jamapediatrics.2019.4498
Aronson D, Edelman ER (2014) Coronary artery disease and diabetes mellitus. Cardiol Clin 32:439–455. https://doi.org/10.1016/j.ccl.2014.04.001
Bagi Z, Koller A, Kaley G (2003) Superoxide-NO interaction decreases flow- and agonist-induced dilations of coronary arterioles in Type 2 diabetes mellitus. Am J Physiol Heart Circ Physiol 285:H1404-1410. https://doi.org/10.1152/ajpheart.00235.2003
Ben-Nun D, Buja LM, Fuentes F (2020) Prevention of heart failure with preserved ejection fraction (HFpEF): reexamining microRNA-21 inhibition in the era of oligonucleotide-based therapeutics. Cardiovasc Pathol 49:107243. https://doi.org/10.1016/j.carpath.2020.107243
Beyer AM, Freed JK, Durand MJ, Riedel M, Ait-Aissa K, Green P, Hockenberry JC, Morgan RG, Donato AJ, Peleg R, Gasparri M, Rokkas CK, Santos JH, Priel E, Gutterman DD (2016) Critical role for telomerase in the mechanism of flow-mediated dilation in the human microcirculation. Circ Res 118:856–866. https://doi.org/10.1161/circresaha.115.307918
Beyer AM, Zinkevich N, Miller B, Liu Y, Wittenburg AL, Mitchell M, Galdieri R, Sorokin A, Gutterman DD (2017) Transition in the mechanism of flow-mediated dilation with aging and development of coronary artery disease. Basic Res Cardiol 112:5. https://doi.org/10.1007/s00395-016-0594-x
Bijkerk R, Duijs JM, Khairoun M, Ter Horst CJ, van der Pol P, Mallat MJ, Rotmans JI, de Vries AP, de Koning EJ, de Fijter JW, Rabelink TJ, van Zonneveld AJ, Reinders ME (2015) Circulating microRNAs associate with diabetic nephropathy and systemic microvascular damage and normalize after simultaneous pancreas-kidney transplantation. Am J Transplant 15:1081–1090. https://doi.org/10.1111/ajt.13072
Calo N, Ramadori P, Sobolewski C, Romero Y, Maeder C, Fournier M, Rantakari P, Zhang FP, Poutanen M, Dufour JF, Humar B, Nef S, Foti M (2016) Stress-activated miR-21/miR-21* in hepatocytes promotes lipid and glucose metabolic disorders associated with high-fat diet consumption. Gut 65:1871–1881. https://doi.org/10.1136/gutjnl-2015-310822
Chen Q, Qiu F, Zhou K, Matlock HG, Takahashi Y, Rajala RVS, Yang Y, Moran E, Ma JX (2017) Pathogenic role of microRNA-21 in diabetic retinopathy through downregulation of PPARα. Diabetes 66:1671–1682. https://doi.org/10.2337/db16-1246
Chin-Dusting JP, Alexander CT, Arnold PJ, Hodgson WC, Lux AS, Jennings GL (1996) Effects of in vivo and in vitro L-arginine supplementation on healthy human vessels. J Cardiovasc Pharmacol 28:158–166. https://doi.org/10.1097/00005344-199607000-00023
Cho SY, Kim SH, Yi MH, Zhang E, Kim E, Park J, Jo EK, Lee YH, Park MS, Kim Y, Park J, Kim DW (2017) Expression of PGC1α in glioblastoma multiforme patients. Oncol Lett 13:4055–4076. https://doi.org/10.3892/ol.2017.5972
Choi M, Lu YW, Zhao J, Wu M, Zhang W, Long X (2020) Transcriptional control of a novel long noncoding RNA Mymsl in smooth muscle cells by a single Cis-element and its initial functional characterization in vessels. J Mol Cell Cardiol 138:147–157. https://doi.org/10.1016/j.yjmcc.2019.11.148
Choi SK, Galan M, Kassan M, Partyka M, Trebak M, Matrougui K (2012) Poly(ADP-ribose) polymerase 1 inhibition improves coronary arteriole function in type 2 diabetes mellitus. Hypertension 59:1060–1068. https://doi.org/10.1161/hypertensionaha.111.190140
Couto GK, Britto LR, Mill JG, Rossoni LV (2015) Enhanced nitric oxide bioavailability in coronary arteries prevents the onset of heart failure in rats with myocardial infarction. J Mol Cell Cardiol 86:110–120. https://doi.org/10.1016/j.yjmcc.2015.07.017
Craige SM, Kroller-Schon S, Li C, Kant S, Cai S, Chen K, Contractor MM, Pei Y, Schulz E, Keaney JF Jr (2016) PGC-1alpha dictates endothelial function through regulation of eNOS expression. Sci Rep 6:38210. https://doi.org/10.1038/srep38210
Dagamajalu S, Rex DAB, Philem PD, Rainey JK, Keshava Prasad TS (2021) A network map of apelin-mediated signaling. J Cell Commun Signal 16(1):137–143 (Netherlands)
Dai B, Li H, Fan J, Zhao Y, Yin Z, Nie X, Wang DW, Chen C (2018) MiR-21 protected against diabetic cardiomyopathy induced diastolic dysfunction by targeting gelsolin. Cardiovasc Diabetol 17:123. https://doi.org/10.1186/s12933-018-0767-z
Dang X, Du G, Hu W, Ma L, Wang P, Li Y (2019) Peroxisome proliferator-activated receptor gamma coactivator-1α/HSF1 axis effectively alleviates lipopolysaccharide-induced acute lung injury via suppressing oxidative stress and inflammatory response. J Cell Biochem 120:544–551. https://doi.org/10.1002/jcb.27409
Ding M, Feng N, Tang D, Feng J, Li Z, Jia M, Liu Z, Gu X, Wang Y, Fu F, Pei J (2018) Melatonin prevents Drp1-mediated mitochondrial fission in diabetic hearts through SIRT1-PGC1alpha pathway. J Pineal Res 65:e12491. https://doi.org/10.1111/jpi.12491
Dissard R, Klein J, Caubet C, Breuil B, Siwy J, Hoffman J, Sicard L, Ducasse L, Rascalou S, Payre B, Buleon M, Mullen W, Mischak H, Tack I, Bascands JL, Buffin-Meyer B, Schanstra JP (2013) Long term metabolic syndrome induced by a high fat high fructose diet leads to minimal renal injury in C57BL/6 mice. PLoS One 8:e76703. https://doi.org/10.1371/journal.pone.0076703
Duling DR (1994) Simulation of multiple isotropic spin-trap EPR spectra. J Magn Reson B 104:105–110. https://doi.org/10.1006/jmrb.1994.1062
Freed JK, Beyer AM, LoGiudice JA, Hockenberry JC, Gutterman DD (2014) Ceramide changes the mediator of flow-induced vasodilation from nitric oxide to hydrogen peroxide in the human microcirculation. Circ Res 115:525–532. https://doi.org/10.1161/CIRCRESAHA.115.303881
Gomez IG, MacKenna DA, Johnson BG, Kaimal V, Roach AM, Ren S, Nakagawa N, Xin C, Newitt R, Pandya S, Xia TH, Liu X, Borza DB, Grafals M, Shankland SJ, Himmelfarb J, Portilla D, Liu S, Chau BN, Duffield JS (2015) Anti-microRNA-21 oligonucleotides prevent Alport nephropathy progression by stimulating metabolic pathways. J Clin Invest 125:141–156. https://doi.org/10.1172/JCI75852
Hutcheson R, Chaplin J, Hutcheson B, Borthwick F, Proctor S, Gebb S, Jadhav R, Smith E, Russell JC, Rocic P (2014) miR-21 normalizes vascular smooth muscle proliferation and improves coronary collateral growth in metabolic syndrome. Faseb J 28:4088–4099. https://doi.org/10.1096/fj.14-251223
Hutcheson R, Terry R, Hutcheson B, Jadhav R, Chaplin J, Smith E, Barrington R, Proctor SD, Rocic P (2015) miR-21-mediated decreased neutrophil apoptosis is a determinant of impaired coronary collateral growth in metabolic syndrome. Am J Physiol Heart Circ Physiol 308:H1323-1335. https://doi.org/10.1152/ajpheart.00654.2014
Jia G, Hill MA, Sowers JR (2018) Diabetic cardiomyopathy: an update of mechanisms contributing to this clinical entity. Circ Res 122:624–638. https://doi.org/10.1161/CIRCRESAHA.117.311586
Kadlec AO, Barnes C, Durand MJ, Gutterman DD (2018) Microvascular adaptations to exercise: protective effect of PGC-1α. Am J Hypertens 31:240–246. https://doi.org/10.1093/ajh/hpx162
Kadlec AO, Chabowski DS, Ait-Aissa K, Hockenberry JC, Otterson MF, Durand MJ, Freed JK, Beyer AM, Gutterman DD (2017) PGC-1α (Peroxisome Proliferator-Activated Receptor gamma Coactivator 1-α) overexpression in coronary artery disease recruits NO and hydrogen peroxide during flow-mediated dilation and protects against increased intraluminal pressure. Hypertension 70:166–173. https://doi.org/10.1161/HYPERTENSIONAHA.117.09289
Kang PT, Chen CL, Ohanyan V, Luther DJ, Meszaros JG, Chilian WM, Chen YR (2015) Overexpressing superoxide dismutase 2 induces a supernormal cardiac function by enhancing redox-dependent mitochondrial function and metabolic dilation. J Mol Cell Cardiol 88:14–28. https://doi.org/10.1016/j.yjmcc.2015.09.001
Kaur R, Kaur M, Singh J (2018) Endothelial dysfunction and platelet hyperactivity in type 2 diabetes mellitus: molecular insights and therapeutic strategies. Cardiovasc Diabetol 17:121. https://doi.org/10.1186/s12933-018-0763-3
Keleher MR, Erickson K, Smith HA, Kechris KJ, Yang IV, Dabelea D, Friedman JE, Boyle KE, Jansson T (2021) Placental insulin/IGF-1 signaling, PGC-1α, and inflammatory pathways are associated with metabolic outcomes at 4–6 years of age: the ECHO healthy start cohort. Diabetes 70:745–751. https://doi.org/10.2337/db20-0902
Labazi H, Trask AJ (2017) Coronary microvascular disease as an early culprit in the pathophysiology of diabetes and metabolic syndrome. Pharmacol Res 123:114–121. https://doi.org/10.1016/j.phrs.2017.07.004
Langbein H, Brunssen C, Hofmann A, Cimalla P, Brux M, Bornstein SR, Deussen A, Koch E, Morawietz H (2016) NADPH oxidase 4 protects against development of endothelial dysfunction and atherosclerosis in LDL receptor deficient mice. Eur Heart J 37:1753–1761. https://doi.org/10.1093/eurheartj/ehv564
Lau P, Nixon SJ, Parton RG, Muscat GE (2004) RORα regulates the expression of genes involved in lipid homeostasis in skeletal muscle cells: caveolin-3 and CPT-1 are direct targets of ROR. J Biol Chem 279:36828–36840. https://doi.org/10.1074/jbc.M404927200
Li X, Wei Y, Wang Z (2018) microRNA-21 and hypertension. Hypertens Res 41:649–661. https://doi.org/10.1038/s41440-018-0071-z
Liu H, Lessieur EM, Saadane A, Lindstrom SI, Taylor PR, Kern TS (2019) Neutrophil elastase contributes to the pathological vascular permeability characteristic of diabetic retinopathy. Diabetologia 62(12):2365–2374
Liu Y, Zhao H, Li H, Kalyanaraman B, Nicolosi AC, Gutterman DD (2003) Mitochondrial sources of H2O2 generation play a key role in flow-mediated dilation in human coronary resistance arteries. Circ Res 93:573–580. https://doi.org/10.1161/01.RES.0000091261.19387.AE
Luo S, Truong AH, Makino A (2016) Isolation of mouse coronary endothelial cells. J Vis Exp. https://doi.org/10.3791/53985
Luther KM, Haar L, McGuinness M, Wang Y, Lynch Iv TL, Phan A, Song Y, Shen Z, Gardner G, Kuffel G, Ren X, Zilliox MJ, Jones WK (2018) Exosomal miR-21a-5p mediates cardioprotection by mesenchymal stem cells. J Mol Cell Cardiol 119:125–137. https://doi.org/10.1016/j.yjmcc.2018.04.012
Majithiya JB, Paramar AN, Balaraman R (2005) Pioglitazone, a PPARγ agonist, restores endothelial function in aorta of streptozotocin-induced diabetic rats. Cardiovasc Res 66:150–161. https://doi.org/10.1016/j.cardiores.2004.12.025
Matoba T, Shimokawa H, Nakashima M, Hirakawa Y, Mukai Y, Hirano K, Kanaide H, Takeshita A (2000) Hydrogen peroxide is an endothelium-derived hyperpolarizing factor in mice. J Clin Invest 106:1521–1530. https://doi.org/10.1172/jci10506
Miura H, Bosnjak JJ, Ning G, Saito T, Miura M, Gutterman DD (2003) Role for hydrogen peroxide in flow-induced dilation of human coronary arterioles. Circ Res 92:e31-40. https://doi.org/10.1161/01.res.0000054200.44505.ab
Miura H, Wachtel RE, Liu Y, Loberiza FR Jr, Saito T, Miura M, Gutterman DD (2001) Flow-induced dilation of human coronary arterioles: important role of Ca(2+)-activated K(+) channels. Circulation 103:1992–1998. https://doi.org/10.1161/01.cir.103.15.1992
Murthy VL, Naya M, Foster CR, Gaber M, Hainer J, Klein J, Dorbala S, Blankstein R, Di Carli MF (2012) Association between coronary vascular dysfunction and cardiac mortality in patients with and without diabetes mellitus. Circulation 126:1858–1868. https://doi.org/10.1161/CIRCULATIONAHA.112.120402
Nishiyama SK, Zhao J, Wray DW, Richardson RS (2017) Vascular function and endothelin-1: tipping the balance between vasodilation and vasoconstriction. J Appl Physiol (1985) 122:354–360. https://doi.org/10.1152/japplphysiol.00772.2016
Ohanyan V, Yin L, Bardakjian R, Kolz C, Enrick M, Hakobyan T, Kmetz J, Bratz I, Luli J, Nagane M, Khan N, Hou H, Kuppusamy P, Graham J, Fu FK, Janota D, Oyewumi MO, Logan S, Lindner JR, Chilian WM (2015) Requisite role of Kv1.5 channels in coronary metabolic dilation. Circ Res 117:612–621. https://doi.org/10.1161/CIRCRESAHA.115.306642
Ohanyan V, Yin L, Bardakjian R, Kolz C, Enrick M, Hakobyan T, Luli J, Graham K, Khayata M, Logan S, Kmetz J, Chilian WM (2017) Kv1.3 channels facilitate the connection between metabolism and blood flow in the heart. Microcirculation. https://doi.org/10.1111/micc.12334
Oishi K, Yamamoto S, Itoh N, Nakao R, Yasumoto Y, Tanaka K, Kikuchi Y, Fukudome S, Okita K, Takano-Ishikawa Y (2015) Wheat alkylresorcinols suppress high-fat, high-sucrose diet-induced obesity and glucose intolerance by increasing insulin sensitivity and cholesterol excretion in male mice. J Nutr 145:199–206. https://doi.org/10.3945/jn.114.202754
Ormazabal V, Nair S, Elfeky O, Aguayo C, Salomon C, Zuniga FA (2018) Association between insulin resistance and the development of cardiovascular disease. Cardiovasc Diabetol 17:122. https://doi.org/10.1186/s12933-018-0762-4
Park Y, Yang J, Zhang H, Chen X, Zhang C (2011) Effect of PAR2 in regulating TNF-α and NAD(P)H oxidase in coronary arterioles in type 2 diabetic mice. Basic Res Cardiol 106:111–123. https://doi.org/10.1007/s00395-010-0129-9
Qiao L, Hu S, Liu S, Zhang H, Ma H, Huang K, Li Z, Su T, Vandergriff A, Tang J, Allen T, Dinh PU, Cores J, Yin Q, Li Y, Cheng K (2019) microRNA-21-5p dysregulation in exosomes derived from heart failure patients impairs regenerative potential. J Clin Invest 129:2237–2250. https://doi.org/10.1172/JCI123135
Ramanujam D, Schon AP, Beck C, Vaccarello P, Felician G, Dueck A, Esfandyari D, Meister G, Meitinger T, Schulz C, Engelhardt S (2021) MicroRNA-21-dependent macrophage-to-fibroblast signaling determines the cardiac response to pressure overload. Circulation 143:1513–1525. https://doi.org/10.1161/CIRCULATIONAHA.120.050682
Ranjan P, Kumari R, Goswami SK, Li J, Pal H, Suleiman Z, Cheng Z, Krishnamurthy P, Kishore R, Verma SK (2021) Myofibroblast-derived exosome induce cardiac endothelial cell dysfunction. Front Cardiovasc Med 8:676267. https://doi.org/10.3389/fcvm.2021.676267
Rughani A, Friedman JE, Tryggestad JB (2020) Type 2 diabetes in youth: the role of early life exposures. Curr Diab Rep 20:45. https://doi.org/10.1007/s11892-020-01328-6
Sato A, Sakuma I, Gutterman DD (2003) Mechanism of dilation to reactive oxygen species in human coronary arterioles. Am J Physiol Heart Circ Physiol 285:H2345-2354. https://doi.org/10.1152/ajpheart.00458.2003
Seeger FH, Sedding D, Langheinrich AC, Haendeler J, Zeiher AM, Dimmeler S (2009) Inhibition of the p38 MAP kinase in vivo improves number and functional activity of vasculogenic cells and reduces atherosclerotic disease progression. Basic Res Cardiol 105:389–397. https://doi.org/10.1007/s00395-009-0072-9
Sekar D, Venugopal B, Sekar P, Ramalingam K (2016) Role of microRNA 21 in diabetes and associated/related diseases. Gene 582:14–18. https://doi.org/10.1016/j.gene.2016.01.039
Sharabi K, Lin H, Tavares CDJ, Dominy JE, Camporez JP, Perry RJ, Schilling R, Rines AK, Lee J, Hickey M, Bennion M, Palmer M, Nag PP, Bittker JA, Perez J, Jedrychowski MP, Ozcan U, Gygi SP, Kamenecka TM, Shulman GI, Schreiber SL, Griffin PR, Puigserver P (2017) Selective chemical inhibition of PGC-1α gluconeogenic activity ameliorates type 2 diabetes. Cell 169:148–160. https://doi.org/10.1016/j.cell.2017.03.001 (e115)
Shimokawa H (2010) Hydrogen peroxide as an endothelium-derived hyperpolarizing factor. Pflugers Arch 459:915–922. https://doi.org/10.1007/s00424-010-0790-8
Simonsen U, Prieto D, Mulvany MJ, Ehrnrooth E, Korsgaard N, Nyborg NC (1992) Effect of induced hypercholesterolemia in rabbits on functional responses of isolated large proximal and small distal coronary arteries. Arterioscler Thromb 12:380–392. https://doi.org/10.1161/01.atv.12.3.380
St-Pierre J, Drori S, Uldry M, Silvaggi JM, Rhee J, Jager S, Handschin C, Zheng K, Lin J, Yang W, Simon DK, Bachoo R, Spiegelman BM (2006) Suppression of reactive oxygen species and neurodegeneration by the PGC-1 transcriptional coactivators. Cell 127:397–408. https://doi.org/10.1016/j.cell.2006.09.024
Surwit RS, Kuhn CM, Cochrane C, McCubbin JA, Feinglos MN (1988) Diet-induced type II diabetes in C57BL/6J mice. Diabetes 37:1163–1167. https://doi.org/10.2337/diab.37.9.1163
Takaki A, Morikawa K, Tsutsui M, Murayama Y, Tekes E, Yamagishi H, Ohashi J, Yada T, Yanagihara N, Shimokawa H (2008) Crucial role of nitric oxide synthases system in endothelium-dependent hyperpolarization in mice. J Exp Med 205:2053–2063. https://doi.org/10.1084/jem.20080106
Tavares CDJ, Aigner S, Sharabi K, Sathe S, Mutlu B, Yeo GW, Puigserver P (2020) Transcriptome-wide analysis of PGC-1α-binding RNAs identifies genes linked to glucagon metabolic action. Proc Natl Acad Sci USA 117:22204–22213. https://doi.org/10.1073/pnas.2000643117
Urbich C, Kuehbacher A, Dimmeler S (2008) Role of microRNAs in vascular diseases, inflammation, and angiogenesis. Cardiovasc Res 79:581–588. https://doi.org/10.1093/cvr/cvn156
van de Wouw J, Sorop O, van Drie RWA, van Duin RWB, Nguyen ITN, Joles JA, Verhaar MC, Merkus D, Duncker DJ (2020) Perturbations in myocardial perfusion and oxygen balance in swine with multiple risk factors: a novel model of ischemia and no obstructive coronary artery disease. Basic Res Cardiol 115:21. https://doi.org/10.1007/s00395-020-0778-2
Wang D, Deuse T, Stubbendorff M, Chernogubova E, Erben RG, Eken SM, Jin H, Li Y, Busch A, Heeger CH, Behnisch B, Reichenspurner H, Robbins RC, Spin JM, Tsao PS, Schrepfer S, Maegdefessel L (2015) Local microRNA modulation using a novel anti-miR-21-eluting stent effectively prevents experimental in-stent restenosis. Arterioscler Thromb Vasc Biol 35:1945–1953. https://doi.org/10.1161/ATVBAHA.115.305597
Wang Z, Wu Y, Zhang S, Zhao Y, Yin X, Wang W, Ma X, Liu H (2019) The role of NO-cGMP pathway inhibition in vascular endothelial-dependent smooth muscle relaxation disorder of AT1-AA positive rats: protective effects of adiponectin. Nitric Oxide 87:10–22. https://doi.org/10.1016/j.niox.2019.02.006
Weber M, Baker MB, Moore JP, Searles CD (2010) MiR-21 is induced in endothelial cells by shear stress and modulates apoptosis and eNOS activity. Biochem Biophys Res Commun 393:643–648. https://doi.org/10.1016/j.bbrc.2010.02.045
Weil BR, Canty JM Jr (2014) Ceramide signaling in the coronary microcirculation: a double-edged sword? Circ Res 115:475–477. https://doi.org/10.1161/circresaha.114.304589
Weitzberg E, Hezel M, Lundberg JO (2010) Nitrate-nitrite-nitric oxide pathway: implications for anesthesiology and intensive care. Anesthesiology 113:1460–1475. https://doi.org/10.1097/ALN.0b013e3181fcf3cc
Xu X, Jiao X, Song N, Luo W, Liang M, Ding X, Teng J (2017) Role of miR21 on vascular endothelial cells in the protective effect of renal delayed ischemic preconditioning. Mol Med Rep 16:2627–2635. https://doi.org/10.3892/mmr.2017.6870
Xu Y, Zalzala M, Xu J, Li Y, Yin L, Zhang Y (2015) A metabolic stress-inducible miR-34a-HNF4alpha pathway regulates lipid and lipoprotein metabolism. Nat Commun 6:7466. https://doi.org/10.1038/ncomms8466
Zhang Z, Peng H, Chen J, Chen X, Han F, Xu X, He X, Yan N (2009) MicroRNA-21 protects from mesangial cell proliferation induced by diabetic nephropathy in db/db mice. FEBS Lett 583:2009–2014. https://doi.org/10.1016/j.febslet.2009.05.021
Acknowledgements
We would like to thank Laura Zhang for illustrating Supplementary Figure 3.
Funding
This research is funded by National Institutes of Health grant 2R01HL103227-05 (YZ, LY), 1R01HL135110-01 (WMC, LY), 1 R01 HL137008-01A1 (LY), and F31HL156726 (CJ).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The corresponding author states that there is no conflict of interest on behalf of all authors.
Additional information
The previous version of this manuscript (R1) was uploaded to bioRxiv (https://doi.org/10.1101/2021.05.18.444667).
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Juguilon, C., Wang, Z., Wang, Y. et al. Mechanism of the switch from NO to H2O2 in endothelium-dependent vasodilation in diabetes. Basic Res Cardiol 117, 2 (2022). https://doi.org/10.1007/s00395-022-00910-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-022-00910-1