Abstract
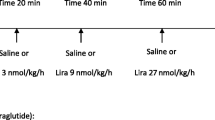
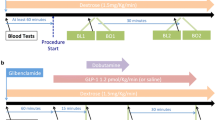
This study examined the cardiovascular effects of GLP-1 (7–36) or (9–36) on myocardial oxygen consumption, function and systemic hemodynamics in vivo during normal perfusion and during acute, regional myocardial ischemia. Lean Ossabaw swine received systemic infusions of saline vehicle or GLP-1 (7–36 or 9–36) at 1.5, 3.0, and 10.0 pmol/kg/min in sequence for 30 min at each dose, followed by ligation of the left circumflex artery during continued infusion at 10.0 pmol/kg/min. Systemic GLP-1 (9–36) had no effect on coronary flow, blood pressure, heart rate or indices of cardiac function before or during regional myocardial ischemia. Systemic GLP-1 (7–36) exerted no cardiometabolic or hemodynamic effects prior to ischemia. During ischemia, GLP-1 (7–36) increased cardiac output by approximately 2 L/min relative to vehicle-controls (p = 0.003). This response was not diminished by treatment with the non-depolarizing ganglionic blocker hexamethonium. Left ventricular pressure–volume loops measured during steady-state conditions with graded occlusion of the inferior vena cava to assess load-independent contractility revealed that GLP-1 (7–36) produced marked increases in end-diastolic volume (74 ± 1 to 92 ± 5 ml; p = 0.03) and volume axis intercept (8 ± 2 to 26 ± 8; p = 0.05), without any change in the slope of the end-systolic pressure–volume relationship vs. vehicle during regional ischemia. GLP-1 (9–36) produced no changes in any of these parameters compared to vehicle. These findings indicate that short-term systemic treatment with GLP-1 (7–36) but not GLP-1 (9–36) significantly augments cardiac output during regional myocardial ischemia, via increases in ventricular preload without changes in cardiac inotropy.





Similar content being viewed by others
References
Allen DG, Kurihara S (1982) The effects of muscle length on intracellular calcium transients in mammalian cardiac muscle. J Physiol 327:79–94
Aroor AR, Sowers JR, Bender SB, Nistala R, Garro M, Mugerfeld I, Hayden MR, Johnson MS, Salam M, Whaley-Connell A, Demarco VG (2013) Dipeptidylpeptidase inhibition is associated with improvement in blood pressure and diastolic function in insulin-resistant male Zucker obese rats. Endocrinology 154:2501–2513. doi:10.1210/en.2013-1096
Ban K, Noyan-Ashraf MH, Hoefer J, Bolz SS, Drucker DJ, Husain M (2008) Cardioprotective and vasodilatory actions of glucagon-like peptide 1 receptor are mediated through both glucagon-like peptide 1 receptor-dependent and -independent pathways. Circulation 117:2340–2350. doi:10.1161/CIRCULATIONAHA.107.739938
Barragan JM, Eng J, Rodriguez R, Blazquez E (1999) Neural contribution to the effect of glucagon-like peptide-1-(7–36) amide on arterial blood pressure in rats. Am J Physiol 277:E784–E791
Barragan JM, Rodriguez RE, Blazquez E (1994) Changes in arterial blood pressure and heart rate induced by glucagon-like peptide-1-(7–36) amide in rats. Am J Physiol 266:E459–E466
Barragan JM, Rodriguez RE, Eng J, Blazquez E (1996) Interactions of exendin-(9–39) with the effects of glucagon-like peptide-1-(7–36) amide and of exendin-4 on arterial blood pressure and heart rate in rats. Regul Pept 67:63–68
Bharucha AE, Charkoudian N, Andrews CN, Camilleri M, Sletten D, Zinsmeister AR, Low PA (2008) Effects of glucagon-like peptide-1, yohimbine, and nitrergic modulation on sympathetic and parasympathetic activity in humans. Am J Physiol Regul Integr Comp Physiol 295:R874–R880. doi:10.1152/ajpregu.00153.2008
Bojanowska E, Stempniak B (2000) Effects of centrally or systemically injected glucagon-like peptide-1 (7–36) amide on release of neurohypophysial hormones and blood pressure in the rat. Regul Pept 91:75–81
Burkhoff D, Mirsky I, Suga H (2005) Assessment of systolic and diastolic ventricular properties via pressure–volume analysis: a guide for clinical, translational, and basic researchers. Am J Physiol Heart Circ Physiol 289:H501–H512. doi:10.1152/ajpheart.00138.2005
Calaghan S, White E (2004) Activation of Na+–H+ exchange and stretch-activated channels underlies the slow inotropic response to stretch in myocytes and muscle from the rat heart. J Physiol 559:205–214. doi:10.113/jphysiol.2004.069021
Deacon CF (2004) Therapeutic strategies based on glucagon-like peptide 1. Diabetes 53:2181–2189. doi:10.2337/diabetes.53.9.2181
Feigl EO, Neat GW, Huang AH (1990) Interrelations between coronary artery pressure, myocardial metabolism and coronary blood flow. J Mol Cell Cardiol 22:375–390
Ford ES, DeStefano F (1991) Risk factors for mortality from all causes and from coronary heart disease among persons with diabetes. Findings from the National Health and Nutrition Examination Survey I Epidemiologic Follow-up Study. Am J Epidemiol 133:1220–1230
Fuchs F, Wang YP (1996) Sarcomere length versus interfilament spacing as determinants of cardiac myofilament Ca2+ sensitivity and Ca2+ binding. J Mol Cell Cardiol 28:1375–1383. doi:10.1006/jmcc.1996.0129
Gardiner SM, March JE, Kemp PA, Bennett T (2006) Mesenteric vasoconstriction and hindquarters vasodilatation accompany the pressor actions of exendin-4 in conscious rats. J Pharmacol Exp Ther 316:852–859. doi:10.1124/jpet.105.093104
Gordon AM, Huxley AF, Julian FJ (1966) The variation in isometric tension with sarcomere length in vertebrate muscle fibres. J Physiol 184:170–192
Gordon AM, Ridgway EB (1993) Cross-bridges affect both TnC structure and calcium affinity in muscle fibers. Adv Exp Med Biol 332:183–192
Heusch G, Libby P, Gersh B, Yellon D, Bohm M, Lopaschuk G, Opie L (2014) Cardiovascular remodelling in coronary artery disease and heart failure. Lancet 383:1933–1943
Isbil-Buyukcoskun N, Gulec G (2004) Effects of intracerebroventricularly injected glucagon-like peptide-1 on cardiovascular parameters; role of central cholinergic system and vasopressin. Regul Pept 118:33–38. doi:10.1016/j.regpep.2003.10.025
Katz AM (2002) Ernest Henry Starling, his predecessors, and the “Law of the Heart”. Circulation 106:2986–2992. doi:10.1161/01.CIR.0000040594.96123.55
Kieffer TJ, McIntosh CH, Pederson RA (1995) Degradation of glucose-dependent insulinotropic polypeptide and truncated glucagon-like peptide 1 in vitro and in vivo by dipeptidyl peptidase IV. Endocrinology 136:3585–3596. doi:10.1210/endo.136.8.7628397
Knaapen P, Germans T, Knuuti J, Paulus WJ, Dijkmans PA, Allaart CP, Lammertsma AA, Visser FC (2007) Myocardial energetics and efficiency: current status of the noninvasive approach. Circulation 115:918–927. doi:10.1161/CIRCULATIONAHA.106.660639
Moberly SP, Berwick ZC, Kohr M, Svendsen M, Mather KJ, Tune JD (2012) Intracoronary glucagon-like peptide 1 preferentially augments glucose uptake in ischemic myocardium independent of changes in coronary flow. Exp Biol Med (Maywood) 237:334–342. doi:10.1258/ebm.2011.011288
Moberly SP, Mather KJ, Berwick ZC, Owen MK, Goodwill AG, Casalini ED, Hutchins GD, Green MA, Ng Y, Considine RV, Perry KM, Chisholm RL, Tune JD (2013) Impaired cardiometabolic responses to glucagon-like peptide 1 in obesity and type 2 diabetes mellitus. Basic Res Cardiol 108:365. doi:10.1007/s00395-013-0365-x
Morrow DA, Givertz MM (2005) Modulation of myocardial energetics: emerging evidence for a therapeutic target in cardiovascular disease. Circulation 112:3218–3221. doi:10.1161/CIRCULATIONAHA.105.581819
Nguyen TD, Shingu Y, Amorim PA, Schwarzer M, Doenst T (2013) Glucagon-like peptide-1 reduces contractile function and fails to boost glucose utilization in normal hearts in the presence of fatty acids. Int J Cardiol 168:4085–4092. doi:10.1016/j.ijcard.2013.07.018
Nikolaidis LA, Elahi D, Hentosz T, Doverspike A, Huerbin R, Zourelias L, Stolarski C, Shen YT, Shannon RP (2004) Recombinant glucagon-like peptide-1 increases myocardial glucose uptake and improves left ventricular performance in conscious dogs with pacing-induced dilated cardiomyopathy. Circulation 110:955–961. doi:10.1124/jpet.104.073890
Nikolaidis LA, Elahi D, Shen YT, Shannon RP (2005) Active metabolite of GLP-1 mediates myocardial glucose uptake and improves left ventricular performance in conscious dogs with dilated cardiomyopathy. Am J Physiol Heart Circ Physiol 289:H2401–H2408. doi:10.1161/01.CIR.0000139339.85840.DD
Nikolaidis LA, Mankad S, Sokos GG, Miske G, Shah A, Elahi D, Shannon RP (2004) Effects of glucagon-like peptide-1 in patients with acute myocardial infarction and left ventricular dysfunction after successful reperfusion. Circulation 109:962–965. doi:10.1152/ajpheart.00347.2005
Ossum A, van Deurs U, Engstrom T, Jensen JS, Treiman M (2009) The cardioprotective and inotropic components of the postconditioning effects of GLP-1 and GLP-1(9-36)a in an isolated rat heart. Pharmacol Res 60:411–417. doi:10.1016/j.phrs.2009.06.004
Penna C, Pasqua T, Perrelli MG, Pagliaro P, Cerra MC, Angelone T (2012) Postconditioning with glucagon like peptide-2 reduces ischemia/reperfusion injury in isolated rat hearts: role of survival kinases and mitochondrial KATP channels. Basic Res Cardiol 107:272. doi:10.1007/s00395-012-0272-6
Sokos GG, Bolukoglu H, German J, Hentosz T, Magovern GJ Jr, Maher TD, Dean DA, Bailey SH, Marrone G, Benckart DH, Elahi D, Shannon RP (2007) Effect of glucagon-like peptide-1 (GLP-1) on glycemic control and left ventricular function in patients undergoing coronary artery bypass grafting. Am J Cardiol 100:824–829. doi:10.1016/j.amjcard.2007.05.022
Sokos GG, Nikolaidis LA, Mankad S, Elahi D, Shannon RP (2006) Glucagon-like peptide-1 infusion improves left ventricular ejection fraction and functional status in patients with chronic heart failure. J Card Fail 12:694–699. doi:10.1016/j.cardfail.2006.08.211
Suga H (1990) Ventricular energetics. Physiol Rev 70:247–277
Thrainsdottir I, Malmberg K, Olsson A, Gutniak M, Ryden L (2004) Initial experience with GLP-1 treatment on metabolic control and myocardial function in patients with type 2 diabetes mellitus and heart failure. Diab Vasc Dis Res 1:40–43. doi:10.3132/dvdr.2004.005
Timmers L, Henriques JP, de Kleijn DP, Devries JH, Kemperman H, Steendijk P, Verlaan CW, Kerver M, Piek JJ, Doevendans PA, Pasterkamp G, Hoefer IE (2009) Exenatide reduces infarct size and improves cardiac function in a porcine model of ischemia and reperfusion injury. J Am Coll Cardiol 53:501–510. doi:10.1016/j.jacc.2008.10.033
Tune JD, Mallet RT, Downey HF (1998) Insulin improves cardiac contractile function and oxygen utilization efficiency during moderate ischemia without compromising myocardial energetics. J Mol Cell Cardiol 30:2025–2035. doi:10.1006/jmcc.1998.0763
Vila Petroff MG, Egan JM, Wang X, Sollott SJ (2001) Glucagon-like peptide-1 increases cAMP but fails to augment contraction in adult rat cardiac myocytes. Circ Res 89:445–452. doi:10.1161/hh1701.095716
Yamamoto H, Lee CE, Marcus JN, Williams TD, Overton JM, Lopez ME, Hollenberg AN, Baggio L, Saper CB, Drucker DJ, Elmquist JK (2002) Glucagon-like peptide-1 receptor stimulation increases blood pressure and heart rate and activates autonomic regulatory neurons. J Clin Invest 110:43–52. doi:10.1172/JCI200215595
Zander M, Madsbad S, Deacon CF, Holst JJ (2006) The metabolite generated by dipeptidyl-peptidase 4 metabolism of glucagon-like peptide-1 has no influence on plasma glucose levels in patients with type 2 diabetes. Diabetologia 49:369–374. doi:10.1007/s00125-005-0098-y
Zhao T, Parikh P, Bhashyam S, Bolukoglu H, Poornima I, Shen YT, Shannon RP (2006) Direct effects of glucagon-like peptide-1 on myocardial contractility and glucose uptake in normal and postischemic isolated rat hearts. J Pharmacol Exp Ther 317:1106–1113. doi:10.1124/jpet.106.100982
Acknowledgments
The authors gratefully acknowledge financial support from multiple agencies. This work was supported by a National Institutes of Health grant, HL117620 (J. Tune and K. Mather, PI). Dr. Goodwill was supported by National Institutes of Health T32HL079995 (K. March, PI) and American Heart Association 13POST1681001813 (A. Goodwill, PI). Mr. Conteh was supported by National Institutes of Health HL117620-S1 (J. Tune and K. Mather, PI). Mr. Sassoon was supported by grant number TL1 TR000162 (A. Shekhar, PI) from the National Institutes of Health, National Center for Advancing Translational Sciences, Clinical and Translational Sciences Award.
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goodwill, A.G., Tune, J.D., Noblet, J.N. et al. Glucagon-like peptide-1 (7–36) but not (9–36) augments cardiac output during myocardial ischemia via a Frank–Starling mechanism. Basic Res Cardiol 109, 426 (2014). https://doi.org/10.1007/s00395-014-0426-9
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-014-0426-9