Abstract
Background
Epidemiological studies have suggested that adipsin and visfatin are associated with the development of type 2 diabetes. This is the first study to investigate the effects of supplementation with purified anthocyanins on serum adipsin and visfatin in patients with prediabetes or newly diagnosed diabetes.
Methods
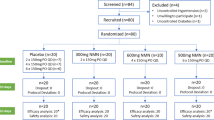
A total of 160 participants with prediabetes or newly diagnosed diabetes (40–75 years old) were given 320 mg anthocyanins or placebo daily for 12 weeks in a randomized trial. Serum adipsin, serum visfatin, lipids and glycated hemoglobin A1c (HbA1c) were measured. The areas under the curve (AUCs) for glucose, insulin and C-peptide were determined before-and after-treatment by a standard 3-h 75 g oral glucose tolerance test (OGTT).
Results
Relatively significant increases in serum adipsin (net change 0.15 µg/mL [0.03, 0.27], p = 0.018) and decreases in visfatin (−3.5 ng/mL [−6.69, −0.31], p = 0.032) were observed between the anthocyanins and placebo groups. We also observed significant improvements in HbA1c (−0.11% [−0.22, −0.11], p = 0.033), apolipoprotein A-1 (apo A-1) (0.12 g/L [0.03, 0.21], p = 0.012) and apolipoprotein B (apo B) (−0.07 g/L [−0.14, −0.01], p = 0.033) in response to the anthocyanins intervention.
Conclusion
Purified anthocyanins supplementation for 12 weeks increased serum adipsin and decreased serum visfatin in patients with prediabetes or newly diagnosed diabetes.
Trial registration ClinicalTrials.gov, identifier: NCT02689765.

Similar content being viewed by others
References
Saeedi P, Petersohn I, Salpea P, Malanda B, Karuranga S, Unwin N, Colagiuri S, Guariguata L, Motala AA, Ogurtsova K, Shaw JE, Bright D, Williams R, Committee IDFDA (2019) Global and regional diabetes prevalence estimates for 2019 and projections for 2030 and 2045: Results from the International Diabetes Federation Diabetes Atlas, 9(th) edition. Diabetes Res Clin Pract 157:107843. https://doi.org/10.1016/j.diabres.2019.107843
Leal Vde O, Mafra D (2013) Adipokines in obesity. Clin Chim Acta 419:87–94. https://doi.org/10.1016/j.cca.2013.02.003
Kim WK, Bae KH, Lee SC, Oh KJ (2019) The latest insights into adipokines in diabetes. J Clin Med 8(11):1874. https://doi.org/10.3390/jcm8111874
Lo JC, Ljubicic S, Leibiger B, Kern M, Leibiger IB, Moede T, Kelly ME, Chatterjee Bhowmick D, Murano I, Cohen P, Banks AS, Khandekar MJ, Dietrich A, Flier JS, Cinti S, Bluher M, Danial NN, Berggren PO, Spiegelman BM (2014) Adipsin is an adipokine that improves beta cell function in diabetes. Cell 158(1):41–53. https://doi.org/10.1016/j.cell.2014.06.005
Wang JS, Lee WJ, Lee IT, Lin SY, Lee WL, Liang KW, Sheu WH (2019) Association between serum adipsin levels and insulin resistance in subjects with various degrees of glucose intolerance. J Endoc Soc 3(2):403–410. https://doi.org/10.1210/js.2018-00359
Zhou Q, Ge Q, Ding Y, Qu H, Wei H, Wu R, Yao L, Wei Q, Feng Z, Long J, Deng H (2018) Relationship between serum adipsin and the first phase of glucose-stimulated insulin secretion in individuals with different glucose tolerance. J Diabetes Invest 9(5):1128–1134. https://doi.org/10.1111/jdi.12819
Chen MP, Chung FM, Chang DM, Tsai JC, Huang HF, Shin SJ, Lee YJ (2006) Elevated plasma level of visfatin/pre-B cell colony-enhancing factor in patients with type 2 diabetes mellitus. J Clin Endocrinol Metab 91(1):295–299. https://doi.org/10.1210/jc.2005-1475
Catalina MO, Redondo PC, Granados MP, Cantonero C, Sanchez-Collado J, Albarran L, Lopez JJ (2019) New insights into adipokines as potential biomarkers for type-2 diabetes mellitus. Curr Med Chem 26(22):4119–4144. https://doi.org/10.2174/0929867325666171205162248
Wedick NM, Pan A, Cassidy A, Rimm EB, Sampson L, Rosner B, Willett W, Hu FB, Sun Q, van Dam RM (2012) Dietary flavonoid intakes and risk of type 2 diabetes in US men and women. Am J Clin Nutr 95(4):925–933. https://doi.org/10.3945/ajcn.111.028894
Mursu J, Virtanen JK, Tuomainen TP, Nurmi T, Voutilainen S (2014) Intake of fruit, berries, and vegetables and risk of type 2 diabetes in Finnish men: the Kuopio Ischaemic Heart Disease Risk Factor Study. Am J Clin Nutr 99(2):328–333. https://doi.org/10.3945/ajcn.113.069641
Sasaki R, Nishimura N, Hoshino H, Isa Y, Kadowaki M, Ichi T, Tanaka A, Nishiumi S, Fukuda I, Ashida H, Horio F, Tsuda T (2007) Cyanidin 3-glucoside ameliorates hyperglycemia and insulin sensitivity due to downregulation of retinol binding protein 4 expression in diabetic mice. Biochem Pharmacol 74(11):1619–1627. https://doi.org/10.1016/j.bcp.2007.08.008
Tsuda T, Ueno Y, Aoki H, Koda T, Horio F, Takahashi N, Kawada T, Osawa T (2004) Anthocyanin enhances adipocytokine secretion and adipocyte-specific gene expression in isolated rat adipocytes. Biochem Biophys Res Commun 316(1):149–157. https://doi.org/10.1016/j.bbrc.2004.02.031
Matsukawa T, Inaguma T, Han J, Villareal MO, Isoda H (2015) Cyanidin-3-glucoside derived from black soybeans ameliorate type 2 diabetes through the induction of differentiation of preadipocytes into smaller and insulin-sensitive adipocytes. J Nutr Biochem 26(8):860–867. https://doi.org/10.1016/j.jnutbio.2015.03.006
American Diabetes A (2013) Standards of medical care in diabetes–2013. Diabetes Care 36(Suppl 1):S11–66. https://doi.org/10.2337/dc13-S011
Moher D (2011) CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. Brit Med J 340:869
Cooke DN, Thomasset S, Boocock DJ, Schwarz M, Winterhalter P, Steward WP, Gescher AJ, Marczylo TH (2006) Development of analyses by high-performance liquid chromatography and liquid chromatography/tandem mass spectrometry of bilberry (Vaccinium myrtilus) anthocyanins in human plasma and urine. J Agric Food Chem 54(19):7009–7013. https://doi.org/10.1021/jf061562q
Nakamura Y, Matsumoto H, Morifuji M, Iida H, Takeuchi Y (2010) Development and validation of a liquid chromatography tandem mass spectrometry method for simultaneous determination of four anthocyanins in human plasma after black currant anthocyanins ingestion. J Agric Food Chem 58(2):1174–1179. https://doi.org/10.1021/jf9027365
Gomez-Banoy N, Guseh JS, Li G, Rubio-Navarro A, Chen T, Poirier B, Putzel G, Rosselot C, Pabon MA, Camporez JP, Bhambhani V, Hwang SJ, Yao C, Perry RJ, Mukherjee S, Larson MG, Levy D, Dow LE, Shulman GI, Dephoure N, Garcia-Ocana A, Hao M, Spiegelman BM, Ho JE, Lo JC (2019) Adipsin preserves beta cells in diabetic mice and associates with protection from type 2 diabetes in humans. Nat Med 25(11):1739–1747. https://doi.org/10.1038/s41591-019-0610-4
Sayers SR, Beavil RL, Fine NHF, Huang GC, Choudhary P, Pacholarz KJ, Barran PE, Butterworth S, Mills CE, Cruickshank JK, Silvestre MP, Poppitt SD, McGill AT, Lavery GG, Hodson DJ, Caton PW (2020) Structure-functional changes in eNAMPT at high concentrations mediate mouse and human beta cell dysfunction in type 2 diabetes. Diabetologia 63(2):313–323. https://doi.org/10.1007/s00125-019-05029-y
Li D, Zhang Y, Liu Y, Sun R, Xia M (2015) Purified anthocyanin supplementation reduces dyslipidemia, enhances antioxidant capacity, and prevents insulin resistance in diabetic patients. J Nutr 145(4):742–748. https://doi.org/10.3945/jn.114.205674
Zhang PW, Chen FX, Li D, Ling WH, Guo HH (2015) A CONSORT-compliant, randomized, double-blind, placebo-controlled pilot trial of purified anthocyanin in patients with nonalcoholic fatty liver disease. Medicine 94(20):e758. https://doi.org/10.1097/MD.0000000000000758
Anette Karlsen LR, Laake P, Paur I, Kjølsrud-Bøhn S, Sandvik L, Blomhoff AR (2007) Anthocyanins inhibit nuclear factor-kappaB activation in monocytes and reduce plasma concentrations of pro-inflammatory mediators in healthy adults. J Nutr 137:1951
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419
Maturu A, DeWitt P, Kern PA, Rasouli N (2015) The triglyceride to high-density lipoprotein cholesterol (TG/HDL-C) ratio as a predictor of beta-cell function in African American women. Metabolism 64(5):561–565. https://doi.org/10.1016/j.metabol.2015.01.004
Abdul-Ghani MA, Jenkinson CP, Richardson DK, Tripathy D, DeFronzo RA (2006) Insulin secretion and action in subjects with impaired fasting glucose and impaired glucose tolerance: results from the Veterans Administration Genetic Epidemiology Study. Diabetes 55(5):1430–1435. https://doi.org/10.2337/db05-1200
Burattini R, Di Nardoa F, Casagrande F, Boemi M, Morosini P (2009) Insulin action and secretion in hypertension in the absence of metabolic syndrome: model-based assessment from oral glucose tolerance test. Metab Clin Exp 58(1):80–92. https://doi.org/10.1016/j.metabol.2008.08.010
Okuno Y, Komada H, Sakaguchi K, Nakamura T, Hashimoto N, Hirota Y, Ogawa W, Seino S (2013) Postprandial serum C-peptide to plasma glucose concentration ratio correlates with oral glucose tolerance test- and glucose clamp-based disposition indexes. Metabolism 62(10):1470–1476. https://doi.org/10.1016/j.metabol.2013.05.022
Vasilenko MA, Kirienkova EV, Skuratovskaia DA, Zatolokin PA, Mironyuk NI, Litvinova LS (2017) The role of production of adipsin and leptin in the development of insulin resistance in patients with abdominal obesity. Dokl Biochem Biophys 475(1):271–276. https://doi.org/10.1134/S160767291704010X
Martinez-Garcia MA, Moncayo S, Insenser M, Alvarez-Blasco F, Luque-Ramirez M, Escobar-Morreale HF (2019) Metabolic cytokines at fasting and during macronutrient challenges: influence of obesity, female androgen excess and sex. Nutrients 11(11):2566. https://doi.org/10.3390/nu11112566
Saisho Y (2016) Postprandial C-peptide to glucose ratio as a marker of beta cell function: implication for the management of type 2 diabetes. Int J Mol Sci 17(5):744. https://doi.org/10.3390/ijms17050744
Liu Y, Wang Y, Ni Y, Cheung CKY, Lam KSL, Wang Y, Xia Z, Ye D, Guo J, Tse MA, Panagiotou G, Xu A (2020) Gut microbiome fermentation determines the efficacy of exercise for diabetes prevention. Cell Metab 31(1):77–91. https://doi.org/10.1016/j.cmet.2019.11.001
Luc G, Empana JP, Morange P, Juhan-Vague I, Arveiler D, Ferrieres J, Amouyel P, Evans A, Kee F, Bingham A, Machez E, Ducimetiere P (2010) Adipocytokines and the risk of coronary heart disease in healthy middle aged men: the PRIME Study. Int J Obes 34(1):118–126. https://doi.org/10.1038/ijo.2009.204
Prugger C, Luc G, Haas B, Arveiler D, Machez E, Ferrieres J, Ruidavets JB, Bingham A, Montaye M, Amouyel P, Yarnell J, Kee F, Ducimetiere P, Empana JP, PRIME Study Group (2012) Adipocytokines and the risk of ischemic stroke: the PRIME Study. Ann Neurol 71(4):478–486. https://doi.org/10.1002/ana.22669
An JH, Kim DL, Lee TB, Kim KJ, Kim SH, Kim NH, Kim HY, Choi DS, Kim SG (2016) Effect of rubus occidentalis extract on metabolic parameters in subjects with prediabetes: a proof-of-concept, randomized, double-blind, placebo-controlled Clinical Trial. PTR. https://doi.org/10.1002/ptr.5664
Zhu Y, Xia M, Yang Y, Liu F, Li Z, Hao Y, Mi M, Jin T, Ling W (2011) Purified anthocyanin supplementation improves endothelial function via NO-cGMP activation in hypercholesterolemic individuals. Clin Chem 57(11):1524–1533. https://doi.org/10.1373/clinchem.2011.167361
Qin Y, Xia M, Ma J, Hao Y, Liu J, Mou H, Cao L, Ling W (2009) Anthocyanin supplementation improves serum LDL- and HDL-cholesterol concentrations associated with the inhibition of cholesteryl ester transfer protein in dyslipidemic subjects. Am J Clin Nutr 90(3):485–492. https://doi.org/10.3945/ajcn.2009.27814
Yang L, Ling W, Du Z, Chen Y, Li D, Deng S, Liu Z, Yang L (2017) Effects of anthocyanins on cardiometabolic health: a systematic review and meta-analysis of randomized controlled trials. Adv Nutr 8(5):684–693. https://doi.org/10.3945/an.116.014852
Owczarek AJ, Olszanecka-Glinianowicz M, Kocelak P, Bozentowicz-Wikarek M, Brzozowska A, Mossakowska M, Puzianowska-Kuznicka M, Grodzicki T, Wiecek A, Chudek J (2016) The relationship between circulating visfatin/nicotinamide phosphoribosyltransferase, obesity, inflammation and lipids profile in elderly population, determined by structural equation modeling. Scand J Clin Lab Invest 76(8):632–640. https://doi.org/10.1080/00365513.2016.1230884
Chang YH, Chang DM, Lin KC, Shin SJ, Lee YJ (2011) Visfatin in overweight/obesity, type 2 diabetes mellitus, insulin resistance, metabolic syndrome and cardiovascular diseases: a meta-analysis and systemic review. Diabetes Metab Res Rev 27(6):515–527. https://doi.org/10.1002/dmrr.1201
Pagano C, Pilon C, Olivieri M, Mason P, Fabris R, Serra R, Milan G, Rossato M, Federspil G, Vettor R (2006) Reduced plasma visfatin/pre-B cell colony-enhancing factor in obesity is not related to insulin resistance in humans. J Clin Endocrinol Metab 91(8):3165–3170. https://doi.org/10.1210/jc.2006-0361
Hosseinzadeh-Attar MJ, Golpaie A, Foroughi M, Hosseinpanah F, Zahediasl S, Azizi F (2016) The relationship between visfatin and serum concentrations of C-reactive protein, interleukin 6 in patients with metabolic syndrome. J Endocrinol Invest 39(8):917–922. https://doi.org/10.1007/s40618-016-0457-1
Legakis I, Mantzouridis T, Bouboulis G, Chrousos GP (2016) Reciprocal changes of serum adispin and visfatin levels in patients with type 2 diabetes after an overnight fast. Arch Endocrinol Metab 60(1):76–78. https://doi.org/10.1590/2359-3997000000147
Ahmed MB, Ismail MI, Meki AR (2015) Relation of osteoprotegerin, visfatin and ghrelin to metabolic syndrome in type 2 diabetic patients. Int J Health Sci 9(2):127–139
Toan NL, Van Hoan N, Cuong DV, Dung NV, Dung PT, Hang NT, Dieu DTH, Chung DT, Son HA, Phong PX, Lenon GB, Van De D, Van Tong H (2018) Adipose tissue-derived cytokines and their correlations with clinical characteristics in Vietnamese patients with type 2 diabetes mellitus. Diabetol Metab Synd 10:41. https://doi.org/10.1186/s13098-018-0343-4
Hetta HF, Ez-Eldeen ME, Mohamed GA, Gaber MA, ElBadre HM, Ahmed EA, Abdellatief RB, Abd-ElBaky RM, Elkady A, Nafee AM, Zahran AM, Ahmad M (2018) Visfatin serum levels in obese type 2 diabetic patients: relation to proinflammatory cytokines and insulin resistance. Egypt J Immunol 25(2):141–151
Mazaherioun M, Hosseinzadeh-Attar MJ, Janani L, Vasheghani Farahani A, Rezvan N, Karbaschian Z, Hossein-Nezhad A (2012) Elevated serum visfatin levels in patients with acute myocardial infarction. Arch Iran Med 15(11):688–692
Adya R, Tan BK, Chen J, Randeva HS (2008) Nuclear factor-kappaB induction by visfatin in human vascular endothelial cells: its role in MMP-2/9 production and activation. Diabetes Care 31(4):758–760. https://doi.org/10.2337/dc07-1544
Zheng LY, Xu X, Wan RH, Xia S, Lu J, Huang Q (2019) Association between serum visfatin levels and atherosclerotic plaque in patients with type 2 diabetes. Diabetol Metab Synd 11:60. https://doi.org/10.1186/s13098-019-0455-5
Yang W, Li Y, Wang JY, Han R, Wang L (2018) Circulating levels of adipose tissue-derived inflammatory factors in elderly diabetes patients with carotid atherosclerosis: a retrospective study. Cardiovasc Diabetol 17(1):75. https://doi.org/10.1186/s12933-018-0723-y
McQueen MJ, Hawken S, Wang X, Ounpuu S, Sniderman A, Probstfield J, Steyn K, Sanderson JE, Hasani M, Volkova E, Kazmi K, Yusuf S, Investigators Is (2008) Lipids, lipoproteins, and apolipoproteins as risk markers of myocardial infarction in 52 countries (the INTERHEART study): a case-control study. Lancet 372(9634):224–233
Emerging Risk Factors C, Di Angelantonio E, Gao P, Pennells L, Kaptoge S, Caslake M, Thompson A, Butterworth AS, Sarwar N, Wormser D, Saleheen D, Ballantyne CM, Psaty BM, Sundstrom J, Ridker PM, Nagel D, Gillum RF, Ford I, Ducimetiere P, Kiechl S, Koenig W, Dullaart RP, Assmann G, D’Agostino RB Sr, Dagenais GR, Cooper JA, Kromhout D, Onat A, Tipping RW, Gomez-de-la-Camara A, Rosengren A, Sutherland SE, Gallacher J, Fowkes FG, Casiglia E, Hofman A, Salomaa V, Barrett-Connor E, Clarke R, Brunner E, Jukema JW, Simons LA, Sandhu M, Wareham NJ, Khaw KT, Kauhanen J, Salonen JT, Howard WJ, Nordestgaard BG, Wood AM, Thompson SG, Boekholdt SM, Sattar N, Packard C, Gudnason V, Danesh J (2012) Lipid-related markers and cardiovascular disease prediction. JAMA 307(23):2499–2506. https://doi.org/10.1001/jama.2012.6571
Scazzocchio B, Vari R, Filesi C, D'Archivio M, Santangelo C, Giovannini C, Iacovelli A, Silecchia G, Li Volti G, Galvano F, Masella R (2011) Cyanidin-3-O-beta-glucoside and protocatechuic acid exert insulin-like effects by upregulating PPARgamma activity in human omental adipocytes. Diabetes 60(9):2234–2244. https://doi.org/10.2337/db10-1461
Singh S, Netticadan T, Ramdath DD (2016) Expression of cardiac insulin signalling genes and proteins in rats fed a high-sucrose diet: effect of bilberry anthocyanin extract. Genes Nutr 11:8. https://doi.org/10.1186/s12263-016-0516-4
Li Y, Zou W, Brestoff JR, Rohatgi N, Wu X, Atkinson JP, Harris CA, Teitelbaum SL (2019) Fat-produced adipsin regulates inflammatory arthritis. Cell Rep 27(10):2809–2816. https://doi.org/10.1016/j.celrep.2019.05.032
McCullough RL, McMullen MR, Sheehan MM, Poulsen KL, Roychowdhury S, Chiang DJ, Pritchard MT, Caballeria J, Nagy LE (2018) Complement Factor D protects mice from ethanol-induced inflammation and liver injury. Am J Physiol Gastrointest Liver Physiol 315(1):G66–G79. https://doi.org/10.1152/ajpgi.00334.2017
Saleh J, Al-Maqbali M, Abdel-Hadi D (2019) Role of complement and complement-related adipokines in regulation of energy metabolism and fat storage. Compr Physiol 9(4):1411–1429. https://doi.org/10.1002/cphy.c170037
Garten A, Schuster S, Penke M, Gorski T, de Giorgis T, Kiess W (2015) Physiological and pathophysiological roles of NAMPT and NAD metabolism. Nat Rev Endocrinol 11(9):535–546. https://doi.org/10.1038/nrendo.2015.117
Fukuhara A, Matsuda M, Nishizawa M, Segawa K, Tanaka M, Kishimoto K, Matsuki Y, Murakami M, Ichisaka T, Murakami H, Watanabe E, Takagi T, Akiyoshi M, Ohtsubo T, Kihara S, Yamashita S, Makishima M, Funahashi T, Yamanaka S, Hiramatsu R, Matsuzawa Y, Shimomura I (2005) Visfatin: a protein secreted by visceral fat that mimics the effects of insulin. Science 307(5708):426–430. https://doi.org/10.1126/science.1097243
Kieswich J, Sayers SR, Silvestre MF, Harwood SM, Yaqoob MM, Caton PW (2016) Monomeric eNAMPT in the development of experimental diabetes in mice: a potential target for type 2 diabetes treatment. Diabetologia 59(11):2477–2486. https://doi.org/10.1007/s00125-016-4076-3
Pei L, Wan T, Wang S, Ye M, Qiu Y, Jiang R, Pang N, Huang Y, Zhou Y, Jiang X, Ling W, Zhang Z, Yang L (2018) Cyanidin-3-O-beta-glucoside regulates the activation and the secretion of adipokines from brown adipose tissue and alleviates diet induced fatty liver. Biomed Pharmacother 105:625–632. https://doi.org/10.1016/j.biopha.2018.06.018
Acknowledgments
The authors are grateful to the participants as well as the medical staff involved in this study.
Funding
This study was supported by the Key Project of National Natural Science Foundation of China (grant number 81730090) and the Health Technology Project of NanShan, ShenZhen (grant number 2019034).
Author information
Authors and Affiliations
Contributions
Liping Yang carried out the trial and wrote the manuscript; Yun Qiu collected the raw data; Jianying Chen contributed to participant recruitment; Changyi Wang and Xiaolin Peng managed the project; Li Wang conducted the statistical analysis; Zhaomin Liu contributed to manuscript revision; Wenhua Ling and Lili Yang designed and supervised the study.
Corresponding author
Ethics declarations
Disclosure Summary
None of the authors have a potential conflict of interest related to the submitted work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yang, L., Qiu, Y., Ling, W. et al. Anthocyanins regulate serum adipsin and visfatin in patients with prediabetes or newly diagnosed diabetes: a randomized controlled trial. Eur J Nutr 60, 1935–1944 (2021). https://doi.org/10.1007/s00394-020-02379-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-020-02379-x