Abstract
Background
There is growing evidence for beneficial prognostic and economic effects of FFR-guided treatment of stable coronary artery disease. We sought to evaluate the real-world use of FFR measurements in patients undergoing elective coronary angiography.
Methods and results
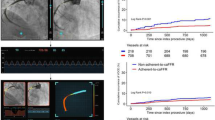
We analyzed the data of the prospective ALKK coronary angiography and PCI registry including data of 38 hospitals from January 2010 to December 2013. A total of 100,977 patients undergoing coronary angiography were included. In 3240 patients (3.2 %) intracoronary pressure measurement was performed. There was a wide range of use of FFR measurement in the different analyzed ALKK hospitals from 0.1 to 8.8 % in elective patients with suspected or known coronary artery disease (median 2.7 %, quartiles 0.9 and 5.3 %), with a successive increase of use over time during the study period. Overall, it was performed in 3.2 % of coronary angiographies. Use in patients with three-vessel disease (2.5 %) and recommendation for bypass surgery (1.6 %) was less frequent. In procedures without PCI, dose area product was higher in the FFR group (2641 cGy × cm2 vs. 2368 cGy × cm2, p < 0.001), while it was lower in procedures with ad hoc PCI (4676 cGy × cm2 vs. 5143 cGy × cm2, p < 0.001). The performing center turned out to be the strongest predictor.
Conclusions
The use of FFR measurement was very heterogeneous between different hospitals and in general relatively low, in particular in patients with multivessel disease or recommendation for bypass surgery, but there was a positive trend during the study period. Technically, FFR measurement was not associated with an increased periprocedural complication rate.




Similar content being viewed by others
References
Tonino PA, Fearon WF, De Bruyne B, Oldroyd KG, Leesar MA, Ver Lee PN, Maccarthy PA, Van’t Veer M, Pijls NH (2010) Angiographic versus functional severity of coronary artery stenoses in the FAME study fractional flow reserve versus angiography in multivessel evaluation. J Am Coll Cardiol 55:2816–2821
Van Belle E, Rioufol G, Pouillot C, Cuisset T, Bougrini K, Teiger E, Champagne S, Belle L, Barreau D, Hanssen M, Besnard C, Dauphin R, Dallongeville J, El Hahi Y, Sideris G, Bretelle C, Lhoest N, Barnay P, Leborgne L, Dupouy P (2014) Outcome impact of coronary revascularization strategy reclassification with fractional flow reserve at time of diagnostic angiography: insights from a large French multicenter fractional flow reserve registry. Circulation 129:173–185
Fearon WF, Bornschein B, Tonino PA, Gothe RM, Bruyne BD, Pijls NH, Siebert U (2010) Economic evaluation of fractional flow reserve-guided percutaneous coronary intervention in patients with multivessel disease. Circulation 122:2545–2550
Pijls NH, van Schaardenburgh P, Manoharan G, Boersma E, Bech JW, van’t Veer M, Bar F, Hoorntje J, Koolen J, Wijns W, de Bruyne B (2007) Percutaneous coronary intervention of functionally nonsignificant stenosis: 5-year follow-up of the DEFER Study. J Am Coll Cardiol 49:2105–2111
Pijls NH, van Son JA, Kirkeeide RL, De Bruyne B, Gould KL (1993) Experimental basis of determining maximum coronary, myocardial, and collateral blood flow by pressure measurements for assessing functional stenosis severity before and after percutaneous transluminal coronary angioplasty. Circulation 87:1354–1367
Tonino PA, De Bruyne B, Pijls NH, Siebert U, Ikeno F, van’t Veer M, Klauss V, Manoharan G, Engstrom T, Oldroyd KG, Ver Lee PN, MacCarthy PA, Fearon WF (2009) Fractional flow reserve versus angiography for guiding percutaneous coronary intervention. N Engl J Med 360:213–224
Wijns W, Kolh P, Danchin N, Di Mario C, Falk V, Folliguet T, Garg S, Huber K, James S, Knuuti J, Lopez-Sendon J, Marco J, Menicanti L, Ostojic M, Piepoli MF, Pirlet C, Pomar JL, Reifart N, Ribichini FL, Schalij MJ, Sergeant P, Serruys PW, Silber S, Sousa Uva M, Taggart D (2010) Guidelines on myocardial revascularization. Eur Heart J 31:2501–2555
Botman KJ, Pijls NH, Bech JW, Aarnoudse W, Peels K, van Straten B, Penn O, Michels HR, Bonnier H, Koolen JJ (2004) Percutaneous coronary intervention or bypass surgery in multivessel disease? A tailored approach based on coronary pressure measurement. Catheter Cardiovasc Interv 63:184–191
Vogt A, Bonzel T, Harmjanz D, von Leitner ER, Pfafferott C, Engel HJ, Niederer W, Schuster PR, Glunz HG, Neuhaus KL (1997) PTCA registry of German community hospitals. Arbeitsgemeinschaft Leitender Kardiologischer Krankenhausarzte (ALKK) Study Group. Eur Heart J 18:1110–1114
Tebbe U, Hochadel M, Bramlage P, Kerber S, Hambrecht R, Grube E, Hauptmann KE, Gottwik M, Elsässer A, Glunz HG, Bonzel T, Carlsson J, Zeymer U, Zahn R, Senges J (2009) In-hospital outcomes after elective and non-elective percutaneous coronary interventions in hospitals with and without on-site cardiac surgery backup. Clin Res Cardiol 98:701–707
Zeymer U, Vogt A, Zahn R, Weber MA, Tebbe U, Gottwik M, Bonzel T, Senges J, Neuhaus KL (2004) Predictors of in-hospital mortality in 1333 patients with acute myocardial infarction complicated by cardiogenic shock treated with primary percutaneous coronary intervention (PCI); Results of the primary PCI registry of the Arbeitsgemeinschaft Leitende Kardiologische Krankenhausarzte (ALKK). Eur Heart J 25:322–328
Zeymer U, Zahn R, Hochadel M, Bonzel T, Weber M, Gottwik M, Tebbe U, Senges J (2005) Incications and complications of invasive diagnostic procedures and percutaneous coronary interventions in the year 2003. Results of the quality control registry of the Arbeitsgemeinschaft Leitende Kardiologische Krankenhausarzte (ALKK). Z Kardiol 94:392–398
Pijls NH, Fearon WF, Tonino PA, Siebert U, Ikeno F, Bornschein B, van’t Veer M, Klauss V, Manoharan G, Engstrom T, Oldroyd KG, Ver Lee PN, MacCarthy PA, De Bruyne B (2010) Fractional flow reserve versus angiography for guiding percutaneous coronary intervention in patients with multivessel coronary artery disease: 2-year follow-up of the FAME (Fractional Flow Reserve Versus Angiography for Multivessel Evaluation) study. J Am Coll Cardiol 56:177–184
Härle T, Zeymer U, Hochadel M, Schmidt K, Zahn R, Darius H, Behrens S, Lauer B, Mudra H, Schächinger V, Elsässer A (2015) Use and impact of thrombectomy in primary percutaneous coronary intervention for acute myocardial infarction with persistent ST-segment elevation: results of the prospective ALKK PCI-registry. Clin Res Cardiol 104:803–811
Härle T, Zeymer U, Schwarz AK, Luers C, Hochadel M, Darius H, Kasper W, Hauptmann KE, Andresen D, Elsässer A (2014) Use of drug-eluting stents in acute myocardial infarction with persistent ST-segment elevation: results of the ALKK PCI-registry. Clin Res Cardiol 103:373–380
De Bruyne B, Pijls NH, Kalesan B, Barbato E, Tonino PA, Piroth Z, Jagic N, Mobius-Winkler S, Rioufol G, Witt N, Kala P, MacCarthy P, Engstrom T, Oldroyd KG, Mavromatis K, Manoharan G, Verlee P, Frobert O, Curzen N, Johnson JB, Juni P, Fearon WF (2012) Fractional flow reserve-guided PCI versus medical therapy in stable coronary disease. N Engl J Med 367:991–1001
Davies RF, Goldberg AD, Forman S, Pepine CJ, Knatterud GL, Geller N, Sopko G, Pratt C, Deanfield J, Conti CR (1997) Asymptomatic Cardiac Ischemia Pilot (ACIP) study two-year follow-up: outcomes of patients randomized to initial strategies of medical therapy versus revascularization. Circulation 95:2037–2043
Hachamovitch R, Hayes SW, Friedman JD, Cohen I, Berman DS (2003) Comparison of the short-term survival benefit associated with revascularization compared with medical therapy in patients with no prior coronary artery disease undergoing stress myocardial perfusion single photon emission computed tomography. Circulation 107:2900–2907
Berger A, Botman KJ, MacCarthy PA, Wijns W, Bartunek J, Heyndrickx GR, Pijls NH, De Bruyne B (2005) Long-term clinical outcome after fractional flow reserve-guided percutaneous coronary intervention in patients with multivessel disease. J Am Coll Cardiol 46:438–442
Nudi F, Schillaci O, Neri G, Pinto A, Procaccini E, Vetere M, Frati G, Tomai F, Biondi-Zoccai G (2016) Prognostic impact of location and extent of vessel-related ischemia at myocardial perfusion scintigraphy in patients with or at risk for coronary artery disease. J Nucl Cardiol 66:274–284
Härle T, Meyer S, Bojara W, Vahldiek F, Elsässer A (2016) Intracoronary pressure measurement differences between anterior and posterior coronary territories. Herz 1–8. doi:10.1007/s00059-016-4471-z
Härle T, Bojara W, Meyer S, Elsässer A (2015) Comparison of instantaneous wave-free ratio (iFR) and fractional flow reserve (FFR)—first real world experience. Int J Cardiol 199:1–7
van de Hoef TP, Nolte F, Rolandi MC, Piek JJ, van den Wijngaard JP, Spaan JA, Siebes M (2012) Coronary pressure-flow relations as basis for the understanding of coronary physiology. J Mol Cell Cardiol 52:786–793
Leone AM, De Caterina AR, Basile E, Gardi A, Laezza D, Mazzari MA, Mongiardo R, Kharbanda R, Cuculi F, Porto I, Niccoli G, Burzotta F, Trani C, Banning AP, Rebuzzi AG, Crea F (2013) Influence of the amount of myocardium subtended by a stenosis on fractional flow reserve. Circ Cardiovasc Interv 6:29–36
Ofili EO, Kern MJ, St Vrain JA, Donohue TJ, Bach R, al-Joundi B, Aguirre FV, Castello R, Labovitz AJ (1995) Differential characterization of blood flow, velocity, and vascular resistance between proximal and distal normal epicardial human coronary arteries: analysis by intracoronary Doppler spectral flow velocity. Am Heart J 130:37–46
Härle T, Meyer S, Vahldiek F, Elsässer A (2016) Differences between automatically detected and steady-state fractional flow reserve. Clin Res Cardiol 105:127–134
Little MP, Wakeford R, Tawn EJ, Bouffler SD, Berrington de Gonzalez A (2009) Risks associated with low doses and low dose rates of ionizing radiation: why linearity may be (almost) the best we can do. Radiology 251:6–12
Seiffert M, Ojeda F, Mullerleile K, Zengin E, Sinning C, Waldeyer C, Lubos E, Schafer U, Sydow K, Blankenberg S, Westermann D (2015) Reducing radiation exposure during invasive coronary angiography and percutaneous coronary interventions implementing a simple four-step protocol. Clin Res Cardiol 104:500–506
Kodama T, Kondo T, Oida A, Fujimoto S, Narula J (2012) Computed tomographic angiography-verified plaque characteristics and slow-flow phenomenon during percutaneous coronary intervention. JACC Cardiovasc Interv 5:636–643
Assali AR, Sdringola S, Ghani M, Denkats AE, Yepes A, Hanna GP, Schroth G, Fujise K, Anderson HV, Smalling RW, Rosales OR (2000) Intracoronary adenosine administered during percutaneous intervention in acute myocardial infarction and reduction in the incidence of “no reflow” phenomenon. Catheter Cardiovasc Interv 51:27–31 (discussion 32)
Marzilli M, Orsini E, Marraccini P, Testa R (2000) Beneficial effects of intracoronary adenosine as an adjunct to primary angioplasty in acute myocardial infarction. Circulation 101:2154–2159
Kapoor N, Yalamanchili V, Siddiqui T, Raza S, Leesar MA (2014) Cardioprotective effect of high-dose intragraft adenosine infusion on microvascular function and prevention of no-reflow during saphenous vein grafts intervention. Catheter Cardiovasc Interv 83:1045–1054
Sen S, Escaned J, Malik IS, Mikhail GW, Foale RA, Mila R, Tarkin J, Petraco R, Broyd C, Jabbour R, Sethi A, Baker CS, Bellamy M, Al-Bustami M, Hackett D, Khan M, Lefroy D, Parker KH, Hughes AD, Francis DP, Di Mario C, Mayet J, Davies JE (2012) Development and validation of a new adenosine-independent index of stenosis severity from coronary wave-intensity analysis: results of the ADVISE (ADenosine Vasodilator Independent Stenosis Evaluation) study. J Am Coll Cardiol 59:1392–1402
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Härle, T., Zeymer, U., Hochadel, M. et al. Real-world use of fractional flow reserve in Germany: results of the prospective ALKK coronary angiography and PCI registry. Clin Res Cardiol 106, 140–150 (2017). https://doi.org/10.1007/s00392-016-1034-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-016-1034-5