Abstract
Objectives
Poor sleep quality is common in patients with chronic heart failure (CHF). This study tested the hypothesis that adaptive servo-ventilation (ASV) therapy in CHF patients whose central sleep apnoea (CSA) was not suppressed by continuous positive airway pressure (CPAP) (CPAP-non-responders) would improve sleep quality compared to CPAP-responders receiving ongoing CPAP therapy.
Methods
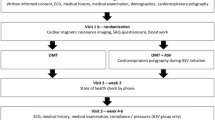
Eighty-two patients with CHF (65 ± 9 years, left ventricular ejection fraction 35 ± 16 %) and CSA [apnoea–hypopnoea index (AHI) ≥15/h] were retrospectively studied. Within an average of 47 days, patients were reevaluated on CPAP therapy and stratified according to their suppression of CSA: 34 were CPAP-non-responders switched to ASV therapy the following day and 48 were CPAP-responders who continued on CPAP therapy. Polysomnographic parameters were assessed in the diagnostic night and on the last night of PAP therapy (CPAP or ASV) before the patient was discharged with the final pressure settings.
Results
Compared with the CPAP group, the ASV group had significantly greater reductions from baseline in AHI (−37 ± 15/h vs −28 ± 18/h, p = 0.02), arousal index (−12.7 ± 13.6/h vs −6.8 ± 12.5/h, p = 0.04) and sleep stage N1 (−9 ± 14 % vs −2 ± 12 %, p = 0.03). In addition, the ASV group gained significantly more rapid eye movement (REM) sleep compared with the CPAP group (+5 ± 9 % vs +1 ± 9 %, p = 0.02).
Conclusions
CPAP therapy is effective in reducing AHI in a significant proportion of CHF patients with reduced ejection fraction and CSA. Treatment of CSA with ASV in CHF patients reduces sleep fragmentation and improves sleep structure to a significantly greater extent than changes seen in responders to CPAP therapy.


Similar content being viewed by others
References
Ferrier K, Campbell A, Yee B, Richards M, O’Meeghan T, Weatherall M, Neill A (2005) Sleep-disordered breathing occurs frequently in stable outpatients with congestive heart failure. Chest 128:2116–2122
Sin DD, Fitzgerald F, Parker JD, Newton G, Floras JS, Bradley TD (1999) Risk factors for central and obstructive sleep apnea in 450 men and women with congestive heart failure. Am J Respir Crit Care Med 160:1101–1106
Jilek C, Krenn M, Sebah D, Obermeier R, Braune A, Kehl V, Schroll S, Montalvan S, Riegger GA, Pfeifer M, Arzt M (2011) Prognostic impact of sleep disordered breathing and its treatment in heart failure: an observational study. Eur J Heart Fail 13:68–75
Reinhard W, Plappert N, Hengstenberg C, Riegger GA, Novack V, Maimon N, Pfeifer M, Arzt M (2013) Prognostic impact of sleep duration and sleep efficiency on mortality in patients with chronic heart failure. Sleep Med 14:502–509
Loredo JS, Ancoli-Israel S, Kim E, Lim WJ, Dimsdale JE (2006) Effect of continuous positive airway pressure versus supplemental oxygen on sleep quality in obstructive sleep apnea: a placebo-CPAP-controlled study. Sleep 29:564–571
McArdle N, Douglas NJ (2001) Effect of continuous positive airway pressure on sleep architecture in the sleep apnea–hypopnea syndrome: a randomized controlled trial. Am J Respir Crit Care Med 164:1459–1463
Bradley TD, Logan AG, Kimoff RJ, Series F, Morrison D, Ferguson K, Belenkie I, Pfeifer M, Fleetham J, Hanly P, Smilovitch M, Tomlinson G, Floras JS (2005) Continuous positive airway pressure for central sleep apnea and heart failure. N Engl J Med 353:2025–2033
Arzt M, Floras JS, Logan AG, Kimoff RJ, Series F, Morrison D, Ferguson K, Belenkie I, Pfeifer M, Fleetham J, Hanly P, Smilovitch M, Ryan C, Tomlinson G, Bradley TD (2007) Suppression of central sleep apnea by continuous positive airway pressure and transplant-free survival in heart failure: a post hoc analysis of the Canadian Continuous Positive Airway Pressure for Patients with Central Sleep Apnea and Heart Failure Trial (CANPAP). Circulation 115:3173–3180
Ruttanaumpawan P, Logan AG, Floras JS, Bradley TD (2009) Effect of continuous positive airway pressure on sleep structure in heart failure patients with central sleep apnea. Sleep 32:91–98
Teschler H, Döhring J, Wang YM, Berthon-Jones M (2001) Adaptive pressure support servo-ventilation: a novel treatment for Cheyne-Stokes respiration in heart failure. Am J Respir Crit Care Med 164:614–619
Arzt M, Schroll S, Series F, Lewis K, Benjamin A, Escourrou P, Luigart R, Kehl V, Pfeifer M (2013) Auto-servo ventilation in heart failure with sleep apnea—a randomized controlled trial. Eur Respir J 42:1244–1254
Aurora RN, Chowdhuri S, Ramar K, Bista SR, Casey KR, Lamm CI, Kristo DA, Mallea JM, Rowley JA, Zak RS, Tracy SL (2012) The treatment of central sleep apnea syndromes in adults: practice parameters with an evidence-based literature review and meta-analyses. Sleep 35:17–40
Arzt M, Wensel R, Montalvan S, Schichtl T, Schroll S, Budweiser S, Blumberg FC, Riegger GA, Pfeifer M (2008) Effects of dynamic bilevel positive airway pressure support on central sleep apnea in men with heart failure. Chest 134:61–66
Patruno V, Aiolfi S, Costantino G, Murgia R, Selmi C, Malliani A, Montano N (2007) Fixed and autoadjusting continuous positive airway pressure treatments are not similar in reducing cardio-vascular risk factors in patients with obstructive sleep apnea. Chest 131:1395–1399
Marrone O, Insalaco G, Bonsignore MR, Romano S, Salvaggio A, Bonsignore G (2002) Sleep structure correlates of CPAP variations during application of an autotitration CPAP machine in obstructive sleep apnea syndrome. Chest 121:759–767
Iber C, Ancoli-Israel S, Chesson A, Quan SF; for the American Academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications, 1st edn. American Academy of Sleep Medicine, Westchester, IL
Cowie MR, Woehrle H, Wegscheider K, Angermann C, d’Ortho MP, Erdmann E, Levy P, Simonds A, Somers VK, Zannad F, Teschler H (2013) Rationale and design of the SERVE-HF study: treatment of sleep-disordered breathing with predominant central sleep apnoea with adaptive servo-ventilation in patients with chronic heart failure. Eur J Heart Fail 15(8):937–943. doi:10.1093/eurjhf/hft051
American College of Cardiology (2015) Preliminary results of SERVE-HF Trial reveal increased CV mortality from ASV therapy. http://www.acc.org/latest-in-cardiology/articles/2015/05/15/11/38/preliminary-results-of-serve-hf-trial-reveal-increased-cv-mortality-from-asv-therapy. Accessed 15 May 2015
Federal Institute for Drugs and Medical Devices (BfArM). Urgent field safety notification/increased risk of cardiovascular death with adaptive servo-ventilation (ASV) therapy for patients with symptomatic chronic heart failure with reduced ejection fraction, ResMed Ltd. http://www.bfarm.de/SharedDocs/Kundeninfos/EN/12/2015/2968-15_Kundeninfo_en.pdf?__blob=publicationFile&v=2. Accessed 15 May 2015
Malhotra A, Patil S, Sands S, Ayas N (2015) Central sleep apnoea in congestive heart failure. Lancet Respir Med. doi:10.1016/S2213-2600(15)00235-0
Randerath WJ, Nothofer G, Priegnitz C, Anduleit N, Treml M, Kehl V, Galetke W (2012) Long-term auto servo-ventilation or constant positive pressure in heart failure and co-existing central with obstructive sleep apnea. Chest 142:440–447
Allam JS, Olson EJ, Gay PC, Morgenthaler TI (2007) Efficacy of adaptive servoventilation in treatment of complex and central sleep apnea syndromes. Chest 132:1839–1846
Campbell AJ, Ferrier K, Neill AM (2012) Effect of oxygen versus adaptive pressure support servo-ventilation in patients with central sleep apnoea-Cheyne Stokes respiration and congestive heart failure. Intern Med J 42:1130–1136
Zhang X, Yin K, Li X, Jia E, Su M (2006) Efficacy of adaptive servoventilation in patients with congestive heart failure and Cheyne-Stokes respiration. Chin Med J 119:622–627
Koyama T, Watanabe H, Tamura Y, Oguma Y, Kosaka T, Ito H (2013) Adaptive servo-ventilation therapy improves cardiac sympathetic nerve activity in patients with heart failure. Eur J Heart Fail 15(8):902–909
Calvin AD, Somers VK, van der Walt C, Scott CG, Olson LJ (2011) Relation of natriuretic peptide concentrations to central sleep apnea in patients with heart failure. Chest 140(6):1517–1523
Acknowledgments
Medical editing assistance was provided by Nicola Ryan, independent medical writer, funded by ResMed.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Michael Arzt has received unrestricted grant support from Philips Home Healthcare Solutions (Murrysville, PA, USA), ResMed (Martinsried, Germany) and the German Foundation for Cardiac Research (Deutsche Stiftung für Herzforschung). Michael Arzt is the holder of an endowed professorship from the Free State of Bavaria at the University of Regensburg that was donated by Philips Home Healthcare Solutions (Murrysville, PA, USA) and ResMed (Martinsried, Germany). Tatjana Roth, Andrea Hetzenecker, Christoph Birner, Lars S. Maier and Michael Pfeifer have reported that they have no potential conflicts of interest with any companies/organizations whose products or services may be discussed in this article. The content is entirely the responsibility of the authors, and sponsors had no role in the design or conduct of the study.
Additional information
A. Hetzenecker and T. Roth were contributed equally to this work.
Rights and permissions
About this article
Cite this article
Hetzenecker, A., Roth, T., Birner, C. et al. Adaptive servo-ventilation therapy of central sleep apnoea and its effect on sleep quality. Clin Res Cardiol 105, 189–195 (2016). https://doi.org/10.1007/s00392-015-0904-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-015-0904-6