Abstract
Background
Hypertensive urgency/emergency occurs frequently, yet no prospective data on common secondary causes, including sleep apnea (SA), renal artery stenosis (RAS), and hyperaldosteronism, are available.
Methods
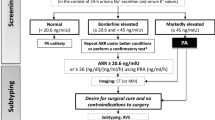
Patients presenting to the emergency room for over 1 year with systolic blood pressure ≥180 mmHg and/or diastolic blood pressure ≥100 mmHg and typical symptoms were included. RAS was diagnosed by direct duplex/Doppler ultrasound of the renal artery, resistance index, and imaging. The aldosterone/renin ratio (ARR) was determined from morning blood samples taken with the patients supine after ≥2 h of rest. A positive ARR (>50) was followed by saline infusion to exclude primary hyperaldosteronism. SA was evaluated by nasal breathing flow screening; when positive [apnea/hypopnea index (AHI) >5/h], complete polysomnography was performed.
Results
Of 161 patients (age, 66.0 ± 13.1 years; BMI, 28.6 ± 5.1 kg), 131 had previously identified hypertension (duration, 12.7 ± 11.5 years; 1.9 ± 1.5 antihypertensive medications). SA was found in 114 (70.8%) patients [18% mild (AHI: 5–15/h), 26.8% moderate (15.1–30/h), and 24.2% severe (>30/h)]. Aldosterone levels exceeded 160 pg/ml in 22 of 23 patients with hyperaldosteronism; 4 had primary and 12 had secondary hyperaldosteronism. Thirteen (8.1%) patients had RAS. Three secondary causes were found in 1 patient (0.6%), ≥2 in 25 (15.5%), and ≥1 in 124 patients (77.0%). Of 150 detected secondary causes, only 5 were recognized previously.
Conclusions
Secondary causes of hypertension are common and predominantly unrecognized in patients with hypertensive urgency/emergency. Co-prevalence of secondary causes occurs in about 15% and should be considered before therapeutic intervention.
Similar content being viewed by others
References
Zampaglione B, Pascale C, Marchisio M, Cavallo-Perin P (1996) Hypertensive urgencies and emergencies. Prevalence and clinical presentation. Hypertension 27(1):144–147
(1997) Practice parameters for the indications for polysomnography and related procedures. Polysomnography Task Force, American Sleep Disorders Association Standards of Practice Committee. Sleep 20(6):406–422
Zeller T, Bonvini RF, Sixt S (2008) Color-coded duplex ultrasound for diagnosis of renal artery stenosis and as follow-up examination after revascularization. Catheter Cardiovasc Interv 71(7):995–999
Seiler L, Rump LC, Schulte-Monting J et al (2004) Diagnosis of primary aldosteronism: value of different screening parameters and influence of antihypertensive medication. Eur J Endocrinol 150(3):329–337
Calhoun DA, Jones D, Textor S et al (2008) Resistant hypertension: diagnosis, evaluation, and treatment: a scientific statement from the American Heart Association Professional Education Committee of the Council for High Blood Pressure Research. Circulation 117(25):e510–e526
(1967) Effects of treatment on morbidity in hypertension. Results in patients with diastolic blood pressures averaging 115 through 129 mm Hg. JAMA 202(11):1028–1034
Krijnen P, van Jaarsveld BC, Deinum J, Steyerberg EW, Habbema JD (2004) Which patients with hypertension and atherosclerotic renal artery stenosis benefit from immediate intervention? J Hum Hypertens 18(2):91–96
van Jaarsveld BC, Krijnen P, Pieterman H et al (2000) The effect of balloon angioplasty on hypertension in atherosclerotic renal-artery stenosis. Dutch Renal Artery Stenosis Intervention Cooperative Study Group. N Engl J Med 342(14):1007–1014
Pratt-Ubunama MN, Nishizaka MK, Boedefeld RL, Cofield SS, Harding SM, Calhoun DA (2007) Plasma aldosterone is related to severity of obstructive sleep apnea in subjects with resistant hypertension. Chest 131(2):453–459
Calhoun DA, Nishizaka MK, Zaman MA, Harding SM (2004) Aldosterone excretion among subjects with resistant hypertension and symptoms of sleep apnea. Chest 125(1):112–117
Eide IK, Torjesen PA, Drolsum A, Babovic A, Lilledahl NP (2004) Low-renin status in therapy-resistant hypertension: a clue to efficient treatment. J Hypertens 22(11):2217–2226
Calhoun DA, Nishizaka MK, Zaman MA, Thakkar RB, Weissmann P (2002) Hyperaldosteronism among black and white subjects with resistant hypertension. Hypertension 40(6):892–896
Anderson GH Jr, Blakeman N, Streeten DH (1994) The effect of age on prevalence of secondary forms of hypertension in 4429 consecutively referred patients. J Hypertens 12(5):609–615
Logan AG, Perlikowski SM, Mente A et al (2001) High prevalence of unrecognized sleep apnoea in drug-resistant hypertension. J Hypertens 19(12):2271–2277
Nieto FJ, Young TB, Lind BK et al (2000) Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. JAMA 283(14):1829–1836
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342(19):1378–1384
Grote L, Hedner J, Peter JH (2000) Sleep-related breathing disorder is an independent risk factor for uncontrolled hypertension. J Hypertens 18(6):679–685
Somers VK, Dyken ME, Clary MP, Abboud FM (1995) Sympathetic neural mechanisms in obstructive sleep apnea. J Clin Invest 96(4):1897–1904
Oldenburg O, Lamp B, Freivogel K, Bitter T, Langer C, Horstkotte D (2008) Low night-to-night variability of sleep disordered breathing in patients with stable congestive heart failure. Clin Res Cardiol 97(11):836–842
Becker HF, Jerrentrup A, Ploch T et al (2003) Effect of nasal continuous positive airway pressure treatment on blood pressure in patients with obstructive sleep apnea. Circulation 107(1):68–73
Sanner BM, Tepel M, Markmann A, Zidek W (2002) Effect of continuous positive airway pressure therapy on 24-hour blood pressure in patients with obstructive sleep apnea syndrome. Am J Hypertens 15(3):251–257
Logan AG, Tkacova R, Perlikowski SM et al (2003) Refractory hypertension and sleep apnoea: effect of CPAP on blood pressure and baroreflex. Eur Respir J 21(2):241–247
Borgel J, Sanner BM, Keskin F et al (2004) Obstructive sleep apnea and blood pressure. Interaction between the blood pressure-lowering effects of positive airway pressure therapy and antihypertensive drugs. Am J Hypertens 17(12 Pt 1):1081–1087
Marin JM, Carrizo SJ, Vicente E, Agusti AG (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365(9464):1046–1053
Buchner NJ, Sanner BM, Borgel J, Rump LC (2007) Continuous positive airway pressure treatment of mild to moderate obstructive sleep apnea reduces cardiovascular risk. Am J Respir Crit Care Med 176(12):1274–1280
Gotsopoulos H, Kelly JJ, Cistulli PA (2004) Oral appliance therapy reduces blood pressure in obstructive sleep apnea: a randomized, controlled trial. Sleep 27(5):934–941
Otsuka R, Ribeiro de Almeida F, Lowe AA, Linden W, Ryan F (2006) The effect of oral appliance therapy on blood pressure in patients with obstructive sleep apnea. Sleep Breath 10(1):29–36
Mosso L, Carvajal C, Gonzalez A et al (2003) Primary aldosteronism and hypertensive disease. Hypertension 42(2):161–165
Douma S, Petidis K, Doumas M et al (2008) Prevalence of primary hyperaldosteronism in resistant hypertension: a retrospective observational study. Lancet 371(9628):1921–1926
Rossi GP, Bernini G, Caliumi C et al (2006) A prospective study of the prevalence of primary aldosteronism in 1,125 hypertensive patients. J Am Coll Cardiol 48(11):2293–2300
Zeller T, Frank U, Spath M, Roskamm H (2001) Color duplex ultrasound imaging of renal arteries and detection of hemodynamically relevant renal artery stenoses. Ultraschall Med 22(3):116–121
Krumme B, Blum U, Schwertfeger E et al (1996) Diagnosis of renovascular disease by intra- and extrarenal Doppler scanning. Kidney Int 50(4):1288–1292
Conflict of interest statement
The authors state that there are no potential conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Börgel, J., Springer, S., Ghafoor, J. et al. Unrecognized secondary causes of hypertension in patients with hypertensive urgency/emergency: prevalence and co-prevalence. Clin Res Cardiol 99, 499–506 (2010). https://doi.org/10.1007/s00392-010-0148-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-010-0148-4