Abstract
Purpose
To identify 5-year survival prognostic variables in patients with colorectal cancer (CRC) and to propose a survival prognostic score that also takes into account changes over time in the patient’s health-related quality of life (HRQoL) status.
Methods
Prospective observational cohort study of CRC patients. We collected data from their diagnosis, intervention, and at 1, 2, 3, and 5 years following the index intervention, also collecting HRQoL data using the EuroQol-5D-5L (EQ-5D-5L), European Organization for Research and Treatment of Cancer’s Quality of Life Questionnaire-Core 30 (EORTC-QLQ-C30), and Hospital Anxiety and Depression Scale (HADS) questionnaires. Multivariate Cox proportional models were used.
Results
We found predictors of mortality over the 5-year follow-up to be being older; being male; having a higher TNM stage; having a higher lymph node ratio; having a result of CRC surgery classified as R1 or R2; invasion of neighboring organs; having a higher score on the Charlson comorbidity index; having an ASA IV; and having worse scores, worse quality of life, on the EORTC and EQ-5D questionnaires, as compared to those with higher scores in each of those questionnaires respectively.
Conclusions
These results allow preventive and controlling measures to be established on long-term follow-up of these patients, based on a few easily measurable variables.
Implications for cancer survivors
Patients with colorectal cancer should be monitored more closely depending on the severity of their disease and comorbidities as well as the perceived health-related quality of life, and preventive measures should be established to prevent adverse outcomes and therefore to ensure that better treatment is received.
Trial registration
ClinicalTrials.gov identifier: NCT02488161.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Colorectal cancer (CRC) continues to be a major health burden, with high mortality rates throughout the world [1]. It ranks as the second most common cancer cause of death worldwide, leading to more than 881,000 deaths in 2018 [1, 2]. It is therefore important to identify factors that help predict the prognosis in CRC patients [3]. As recently stated by Vogelsang et al. [4], individualized risk assessment provides opportunities for tailoring treatment strategies, optimizing healthcare resources, and improving outcomes [4]. Ideally, these would be factors that can be measured quickly, easily, and non-invasively in an ordinary clinical setting [3].
Several scoring systems have been developed to predict operative risk [5], such as the estimation of physiologic ability and surgical stress (E-PASS) score [6], the colorectal physiologic and operative severity score for the enumeration of mortality (CR-POSSUM) [7], and the prognostic nutritional index (PNI) [8]. Models also exist that target early stages in the postoperative period, such as 30-day and 90-day mortality predictions after CCR surgery [4]. However, these scoring systems and models evaluate patients’ physiological condition and outcomes in the short term, and none of them takes into account patient-reported outcomes.
Health-related quality of life (HRQoL) is emerging not only as an important outcome in survivorship care, but also as a factor that influences mortality [6, 9]. Better HRQoL has been found to be associated with a lower risk of dying [6, 10]. Many articles deal with this subject, but as Mosher et al. mention in a review [11], gaps remain, especially during long-term CCR. Apart from this, those prior studies primarily assessed HRQoL in patients with advanced stage of the disease [12,13,14,15,16], or they did not monitor tumor stage, recurrence, or patients’ comorbidities [17]. In our previous study [10], we observed that non-survivors had poorer anxiety, depression, and HRQoL scores than survivors during the 5-year follow-up, and the baseline scores were worse in those closest to death and worsened as death approached. Longitudinal assessment of patients is therefore important for management of such patients, as supported by the literature, specifically Sepehrvand et al. [18]. On the other hand, the overall 5-year relative survival rate for colorectal cancer is 65% [19].
For the above reasons, it can be concluded that there is still a need for a simple instrument that will enable evaluation of the risk of mortality for colorectal cancer in the years following surgery and that includes an update of the patients’ HRQoL over time in a survival analysis. The aims of this research were twofold: first, to identify significant mortality prognostic variables in patients with CRC among time-dependent patient-reported outcomes as well as basal clinical and sociodemographic variables; and second, to propose a survival prognostic score which considers changes over time in patient’s quality of life status. The use of the prognostic score will provide an estimate of the risk of mortality at a given time (within 5 years of the intervention) which could aid clinicians in the management of CRC patients, thus improving their outcomes.
Material and methods
Patients
This was a longitudinal prospective observational analytic cohort study that includes patients from nineteen public hospitals representing nine provinces in Spain, all of which operate under the Spanish National Health Service (SNHS), which is responsible for most of the country’s population, with a planned patient follow-up period of 5 years. Patients with colon or rectal cancer scheduled to undergo surgery between June 2010 and December 2012 were informed of the aims of the study and invited to participate. Only patients who provided written informed consent were allowed to enroll in the study. The study was approved by the Basque Ethics Committee (Approval Number: 11/23/2010 and PI2014084) and all study data were kept confidential. Patients were deemed eligible for this study if they were on the surgical waiting list of one of the participating hospitals and had a diagnosis of surgically resectable colon or rectal cancer. Exclusion criteria were in situ cancer, an unresectable tumor, terminal disease, inability to respond to questionnaires for any reason, and any severe mental or physical conditions that might prevent the patient from responding to questionnaires, as well as failure to consent to participate. Detailed information of the protocol has been published elsewhere [20].
Data collection
Clinical data and patient-reported outcome measures (PROMs) were collected at basal time (before surgery), and at 1, 2, 3 and 5 years after surgery. Data collected at hospital admission included sociodemographic data, clinical data (including information about comorbidities based on the Charlson comorbidity index), [21, 22] preoperative data, outpatient anesthesia data related to the surgical intervention, American Society of Anesthesiologists (ASA) class [23] pathology data including TNM stage and infiltrated lymph nodes, and data related to the period of admission after surgery (including the presence of complications, need for reoperation, readmission, and death). Clinical data were gathered from medical records and databases by qualified reviewers. In order to ensure consistency among centers and reviewers, instruction manuals were prepared to guide the data collection process.
Patients completed Spanish versions of the following patient-reported outcome measures (PROMs) before surgery and at 1, 2, 3, and 5 years after surgery:
Symptoms of anxiety and depression: The Hospital Anxiety and Depression Scale (HADS) [24, 25] was used, a specific questionnaire to measure symptoms of anxiety and depression in individuals with a physical illness. This is a 14-item measure: 7 items for depressive symptoms and 7 items for anxiety. A subscale score of 0 to 7 indicates absence of anxiety or depression; 8 to 10 a possible case of anxiety or depression; and 11 or higher a probable case of anxiety or depression.
Health-related quality of life: The European Organisation for Research and Treatment of Cancer’s Quality of Life Questionnaire Core 30 (EORTC-QLQ-C30) [26, 27] is a specific health-related quality of life questionnaire widely used in cancer research. It consists of 30 items that assess five functioning domains, eight cancer symptom domains, financial difficulties, and global quality of life. Scores are transformed to a 0-to-100 scale, with a high score on the Functional scale and on Global Quality of Life scale indicating better functioning and HRQoL. In this study, we considered The Global Quality of Life scale. The EuroQol-5D-5L (EQ-5D-5L) [28, 29] is a generic HRQoL measure which consists of two parts: (a) the descriptive system comprises 5-level Likert-type dimensions (mobility, self-care, usual activities, pain/discomfort, and anxiety/depression) with 5 answer options defining different levels of severity; and (b) the visual analogue scale (VAS) records the respondent’s self-rated health on a vertical, 20-mm visual analogue scale, ranging from 0 (worst imaginable state of health) to 100 (best imaginable state of health). For this study, only the descriptive system has been taken into account.
Statistical analysis
The primary outcome of this study was the time between surgery and death. Those patients for whom the event of interest (death) was not observed during the 5-year study period were censored. All variables were measured at baseline, while PROMs were measured at baseline and at four points in time (1, 2, 3, and 5 years) after the intervention, all being assessed at each measurement point as a continuous variable. For exploratory analysis, the Kaplan–Meier survival curves were estimated for baseline patient characteristics [30]. Univariate Cox proportional hazard regression models were adjusted and variables with a p-value < 0.2 were included in the multivariate Cox proportional model. PROMs were introduced as time-dependent predictor variables, whose value was updated throughout the different measurements. The final multivariate model considered was the one whose variables had a significance level of alpha = 0.05 and greater discriminative ability measured by the c-index [31, 32], and the proportional hazard assumption was verified by means of the Schoenfeld global residuals test [33]. Due to the existing correlation between variables, not all the variables significant individually were significant in the multivariate model. We developed a time-dependent risk score by assigning a weight to each predictor variable in relation to the estimated β parameters based on the multivariate cox regression model. We then added up the risk weights of all the patient’s predictor variables, with higher scores indicating a greater probability of event at time t. The score was categorized into four risk groups by maximizing the c-index for the categorized variable using the catpredi package in R [34].The predictive accuracy of the risk score was assessed using the c-index.
Both the model and the score were validated. For the former, a tenfold cross-validation with 100 replicates was used to validate the stability of the estimated parameters as well as the c-index obtained. For the latter, a bootstrap validation was performed with 100 repetitions.
Statistical significance was assumed when p < 0.05. All statistical analyses were performed using R v.4.0.3.
Results
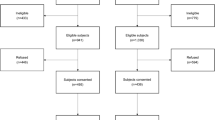
In this study, 2531 patients were recruited who were followed up at 1, 2, 3, and 5 years, collecting sociodemogaphic and clinical information, mortality, and health-related quality of life. A flowchart describing the cohort evolution during the 5 years of follow-up is including in Supplementary Fig. 1. A description of baseline clinical characteristics of the sample is shown in Table 1. Changes in health-related quality of life over the 5 years of follow-up, as measured using the HADS, EORTC-Global Quality of Life Scale, and EQ-5D questionnaires, are shown in Table 2.
The results of the univariate analysis with the variables found to be predictors of mortality at different times of the 5-year follow-up of the cohort of patients with CRC are presented in Table 3. Based on these results, we selected the variables to be included in the multivariate model.
In the multivariable analysis, we identified predictors of mortality over the 5-year follow-up to be being older; being male; having a higher TNM stage; having a higher lymph node ratio; a result of CRC surgery classified as R1 or R2; invasion of neighboring organs; higher score on the Charlson comorbidity index; an ASA IV; and worse scores on the EORTC and EQ-5D health-related quality of life questionnaires, as compared to those with higher scores in each of those questionnaires (Table 4). Given the strong relationship between HADS and EORTC (chi-squared test p-value < 0.0001) and HADS and EQ-5D (chi-squared test p-value < 0.0001), HADs did not appear to be statistically significant in the multivariate model. The c-index of this model was 0.800 (0.796–0.806 95% bootstrap based confidence interval), for which the tenfold cross-validation provided a c-index of 0.801.
Based on the variables identified in this multivariable model, and the weights assigned to each of the categories of their variables, a time-dependent mortality risk score was obtained for the 5 years of follow-up, which was categorized into four categories from lower to higher risk of death with 3, 6, and 10 as the cut-off points. A c-index of 0.794 and 0.779 was obtained for the continuous and categorized scores, respectively. The bootstrap validation provided bootstrap 95% confidence intervals for the c-index of (0.789–0.799) and (0.774–0.785) for the continuous and categorical scores, respectively (see Table 4). Figure 1 shows the Kaplan–Meier curves for the categorized score together with the hazard ratio for each category, where statistically significant differences between all risk categories were obtained.
Discussion
In the current study, we demonstrated that HRQoL measurement was significantly associated with prognosis in CRC patients in a long-term follow-up. We likewise developed and validated a prognostic index for which higher index values were associated with a significantly higher risk of mortality at a given time during a 5-year follow-up. This score can be used in the clinical setting to stratify patients with CRC who underwent surgery into very high-, high-, intermediate-, and low-risk mortality groups in a 5-year follow-up time, combining clinical variables with HRQoL time-dependent measures. Our index showed good discrimination ability and was validated by bootstrap validation. It had a c-index of 0.794 and 0.779, for the continuous and categorized scores, respectively, indicating that it is a reliable tool for estimating prognosis in CRC patients. In addition, the proportional hazards assumption holds for both the model and the score.
Several international societies currently recommend the use of all-cause mortality risk prediction tools when making decisions regarding screening and treatment in geriatric oncology [35]. This recommendation extends to patients with CRC [3], which, despite an improved diagnosis due to greater availability of diagnostic techniques and advances in intraoperative postoperative care and medical care, still ranks as the second most common cancer cause of death worldwide. Therefore, identifying postoperative factors that help predict the prognosis in CRC patients is important—ideally, these would be factors that can be measured quickly, easily, and non-invasively in an ordinary clinical setting [3].
The sociodemographic and clinical characteristics of patients with CRC have been studied more frequently in relation to short- and medium-term mortality. In our study, among the patients’ sociodemographic characteristics, being older [2, 4, 36] and male [36] were related to higher mortality. Within the patients’ clinical parameter at baseline or after surgery, those related to the severity of the CRC, such as having a higher TNM stage [2], a higher lymph node ratio [37, 38], a result of CRC surgery classified as R1 or R2 [39], invasion of neighboring organs [17], or those related to comorbidities or life expectancy, such as a higher score on the Charlson four index [4, 40], or an ASA IV [5, 40,41,42], have been shown to be significant prognostic indicators in CRC patients.
HRQoL has been considered a potential predictor of survival for the general population [12] and also for cancer patients [43]. As recent publication state, [9, 44] HRQoL is a concept that has gained increasing importance as prognostic tool, having done more research in recent years regarding this topics. However, these are not sufficient, as most of them have just a short-medium-term follow-up [13, 14, 16, 44, 45], or taking into account only advanced stage of disease [13,14,15,16]. To our knowledge, only two studies have so far examined the association between HRQoL and mortality in long-term CRC survivors, with providing initial evidence for an inverse relation between better HRQoL and mortality [12, 17]. In those studies, patients were only contacted once after baseline, with HRQoL not being considered a time-dependent covariate in the survival analysis. However, HRQoL may vary over time. At the same time, they used a short and not widely used Veterans RAND 12-item Health Survey to assess HRQoL [12] or did not have information on comorbidities or on tumor stage [17].
In our study, we have collected information on patients’ perceived HRQoL during follow-up at different points in time, using a variety of tools, including a questionnaire, the EQ-5D, that captures general HRQoL, the EORTC, a more specific HRQoL tool for cancer patients, and a questionnaire, the HADS, which focuses on measuring levels of anxiety and depression. We found that having worse scores on the EORTC, and EQ-5D HRQoL questionnaires—i.e., worse quality of life measured by each of these questionnaires, compared to patients with better scores in each of those questionnaires—was related to a greater likelihood of dying in all periods of the follow-up. Our results therefore indicate that poorer scores on the EORTC, and EQ-5D, are also useful predictors of the CRC prognosis when used in addition to the previously described clinical and sociodemographic parameters. This is consistent with the previous studies mentioned above [12, 17].
Regarding the underlying mechanisms of the association between HRQoL and survival in cancer patients, we expanded Ratjen’s analysis [17], adjusting our analyses for tumor stage, recurrence, and comorbidities—variables that might influence worse HRQoL. Our results thus showed that HRQoL is an independent predictor of a prognosis of survival. Moreover, in our index, a low HRQoL score ranked higher (3 points) than variables such as having 5 or more comorbidities (2 points) or invasion (1 point).
Regarding HADS, in our sample, in the univariable analysis, greater anxiety and depression were associated with a greater risk of dying, but they do not appear as independent predictors in the multivariate analysis. The strong association we found in our cohort between HADS and the EORTC and EQ-5D HRQoL scores may be an explanation. An alternative explanation could be that those with worse HADS scores have more severe CRC or more comorbid conditions, which at the same time affect the patients’ survival. Consistent with this observation, Adams et al. [12], who evaluated physical and mental component scores with the Veterans RAND 12-item Health Survey, observed a stronger association between mortality and physical component than with mental component. This contrasts with the potential explications of Ratjen et al. [17] for the observed association between HRQOL and survival; they suggested that it might be psychological distress (stress and depression) that influenced HRQoL. A key factor behind effective coping with cancer-related problems is resilience and it has been considered a protective factor against different health problems, including colon cancer. The higher the resilience, the lower the vulnerability and risk of illness and the better the quality of life [46, 47]. A feasible option for future studies would be to investigate in greater depth the relationship between resilience, HRQoL, and mortality in CRC patients.
To date, no prognostic index has been created considering PROMs variables. Lee et al. [48] stated that function status is particularly useful in prognostic systems because it reflects the severity and consequences of disease, since it is a marker at different points throughout the patients’ trajectories. We believe that this could be extended to HRQoL measurements. The prognostic model of Tanio et al. [3], which combines lymphocyte, monocyte, and neutrophil with clinical characteristics, has an AUC of 0.642. The inclusion of HRQoL measures might perhaps be the reason that our discrimination index compares favorably with Tanio’s model.
Strengths of our study include a large cohort with a variety of clinical information collected through a 5-year follow-up, including patients’ perception of their HRQoL. In developing the model, we followed the TRIPOP guidelines [49], using robust statistical techniques that took into account the various assessments of the HRQoL of patients throughout the 5-year follow-up period. Finally, another strength was the use of valid, reliable, and widely used HRQoL questionnaires. The EORTC-QLQ-C30 is one of the most widely used cancer-specific instrument and EQ-5D-5L is one of the most widely used general instruments.
Several limitations of this study must also be acknowledged. First, as with all prospective cohort studies, loss of patients and information at follow-up is inevitable. Although we have tried to reduce it to a minimum, with such a long follow-up, some loss of data is inevitable. Secondly, all predictive indices tend to optimize the fit of the data to a captive population and, although our score fitted the data well in both the development and validation sets, it is important to cross-validate the scoring system externally by applying the model to a different population in order to assess its predictive power [7]. Finally, some other possible predictors such as molecular data, or the WHO performance status, were not included in the study.
In summary, we identified certain pre-surgery clinical and sociodemographic factors in CCR patients which, combined with the patients’ HRQoL perception in a long-term follow-up, can be used in a prognostic index that has several potential uses in clinical and research fields. It is an accurate tool, indicating that it could be routinely used for better treatment. It may be useful in follow-up, distinguishing both high- and low-risk patients and thus identifying patients with whom it is especially important to discuss advance directives and to provide help in the treatment strategy and in the prevention of adverse outcomes.
Availability of data and material
Data available upon request.
Change history
24 June 2023
A Correction to this paper has been published: https://doi.org/10.1007/s00384-023-04472-z
References
Kanth P, Inadomi JM (2021) Screening and prevention of colorectal cancer. BMJ n1855
Guan X, Ma C, Quan J, Zhao Z, Chen H, Sun P et al (2020) A prognostic index model to individually predict clinical outcomes for colorectal cancer with synchronous bone metastasis. J Cancer 11:4366–4372
Tanio A, Saito H, Uejima C, Takaya S, Yamamoto M, Tokuyasu N et al (2019) A prognostic index for colorectal cancer based on preoperative absolute lymphocyte, monocyte, and neutrophil counts. Surg Today 49:245–253
Vogelsang RP, Bojesen RD, Hoelmich ER, Orhan A, Buzquurz F, Cai L et al (2021) Prediction of 90-day mortality after surgery for colorectal cancer using standardized nationwide quality-assurance data. BJS Open 5:zrab023
Tominaga T, Takeshita H, Takagi K, Kunizaki M, To K, Abo T et al (2016) E-PASS score as a useful predictor of postoperative complications and mortality after colorectal surgery in elderly patients. Int J Colorectal Dis 31:217–225
Haga Y, Ikei S, Owaga M (1999) Estimation of Physiologic Ability and Surgical Stress (E-PASS) as a new prediction scoring system for postoperative morbidity and mortality following elective gastrointestinal surgery. Jpn J Surg 219–25
Tekkis PP, Prytherch DR, Kocher HM, Senapati A, Poloniecki JD, Stamatakis JD et al (2004) Development of a dedicated risk-adjustment scoring system for colorectal surgery (colorectal POSSUM). Br J Surg 91:1174–1182
Onodera T, Goseki N (1984) Kosaki G [Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients]. Nihon Geka Gakkai Zasshi 85:1001–1005
Frank F, Hecht M, Loy F, Rutzner S, Fietkau R, Distel L (2020) Differences in and prognostic value of quality of life data in rectal cancer patients with and without distant metastases. Healthcare 9:1
Orive M, Anton-Ladislao A, Lázaro S, Gonzalez N, Bare M, Fernandez de Larrea N et al (2022) Anxiety, depression, health-related quality of life, and mortality among colorectal patients: 5-year follow-up. Support Care Cancer [Internet]. [cited 23 Jun 2022]; Available from: https://doi.org/10.1007/s00520-022-07177-1
Mosher CE, Winger JG, Given BA, Helft PR, O’Neil BH (2016) Mental health outcomes during colorectal cancer survivorship: a review of the literature: mental health in colorectal cancer survivorship. Psychooncology 25:1261–1270
Adams SV, Ceballos R, Newcomb PA (2016) Quality of life and mortality of long-term colorectal cancer survivors in the seattle colorectal cancer family registry. Montazeri A, editor. PLoS ONE 11:e0156534
Maisey NR, Norman A, Watson M, Allen MJ, Hill ME, Cunningham D (2002) Baseline quality of life predicts survival in patients with advanced colorectal cancer. Eur J Cancer 38:1351–1357
Efficace F, Bottomley A, Coens C, Van Steen K, Conroy T, Schöffski P et al (2006) Does a patient’s self-reported health-related quality of life predict survival beyond key biomedical data in advanced colorectal cancer? Eur J Cancer 42:42–49
Grande GE, Farquhar MC, Barclay SIG, Todd CJ (2009) Quality of life measures (EORTC QLQ-C30 and SF-36) as predictors of survival in palliative colorectal and lung cancer patients. Pall Supp Care 7:289–297
Wong CK, Law W-L, Wan Y-F, Poon JT-C, Lam CL-K (2014) Health-related quality of life and risk of colorectal cancer recurrence and All-cause death among advanced stages of colorectal cancer 1-year after diagnosis. BMC Cancer 14:337
Ratjen I, Schafmayer C, Enderle J, di Giuseppe R, Waniek S, Koch M et al (2018) Health-related quality of life in long-term survivors of colorectal cancer and its association with all-cause mortality: a German cohort study. BMC Cancer 18 [cited 24 Dec 2019]. Available from: https://doi.org/10.1186/s12885-018-5075-1
Sepehrvand N, Savu A, Spertus JA, Dyck JRB, Anderson T, Howlett J et al (2020) Change of health-related quality of life over time and its association with patient outcomes in patients with heart failure. JAHA 9:e017278
American Cancer Society (2022) Cancer facts & figures. Available from: https://www.cancer.org/research/cancer-facts-statistics/all-cancer-facts-figures/cancer-facts-figures-2022.html
Quintana JM, Gonzalez N, Anton-Ladislao A, Redondo M, Bare M, Fernandez de Larrea N et al (2016) Colorectal cancer health services research study protocol: the CCR-CARESS observational prospective cohort project. BMC Cancer 16:435
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Ouellette JR, Small DG, Termuhlen PM (2004) Evaluation of Charlson-Age Comorbidity Index as predictor of morbidity and mortality in patients with colorectal carcinoma. J Gastrointest Surg 8:1061–1067
Owens WD, Felts JA, Spitznagel EL (1978) ASA physical status classifications: a study of consistency of ratings. Anesthesiology 49:239–243
Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67:361–370
Quintana JM, Padierna A, Esteban C, Arostegui I, Bilbao A, Ruiz I (2003) Evaluation of the psychometric characteristics of the Spanish version of the Hospital Anxiety and Depression Scale. Acta Psychiatr Scand 107:216–221
Aaronson NK, Ahmedzai S, Bergman B, Bullinger M, Cull A, Duez NJ et al (1993) The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. J Natl Cancer Inst 85:365–376
Arraras JI, Arias F, Tejedor M, Pruja E, Marcos M, Martínez E et al (2002) The eortc QLQ-C30 (version 3.0) quality of life questionnaire: validation study for Spain with head and neck cancer patients: Validation study of head and neck cancer patients. Psycho-Oncology 11:249–56
Herdman M, Gudex C, Lloyd A, Janssen M, Kind P, Parkin D et al (2011) Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res 20:1727–1736
Hernandez G, Garin O, Pardo Y, Vilagut G, Pont À, Suárez M et al (2018) Validity of the EQ–5D–5L and reference norms for the Spanish population. Qual Life Res 27:2337–2348
Kaplan EL, Meier P (1958) Nonparametric estimation from incomplete observations. J Am Stat Assoc 53:457–481
Harrell FE, Califf RM, Pryor DB, Lee KL, Rosati RA (1982) Evaluating the yield of medical tests. JAMA 247:2543–2546
Therneau TM, Watson DA (2017) The concordance statistic and the Cox model. Department of Health Science Research 85:1–18
Grambsch PM, Therneau TM (1994) Proportional hazards tests and diagnostics based on weighted residuals. Biometrika 81:515–526
Barrio I, Rodríguez-álvarez MX, Meira-Machado L, Esteban C, Arostegui I (2017) Comparison of two discrimination indexes in the categorisation of continuous predictors in time-to-event studies. SORT 1:73–92
Perez-de-Acha A, Pilleron S, Soto-Perez-de-Celis E (2022) All-cause mortality risk prediction in older adults with cancer: practical approaches and limitations. Curr Oncol Rep
Ma C, Teriaky A, Sheh S, Forbes N, Heitman SJ, Jue TL et al (2019) Morbidity and mortality after surgery for nonmalignant colorectal polyps: a 10-year nationwide analysis. Am J Gastroenterol 114:1802–1810
Moccia F, Tolone S, Allaria A, Napolitano V, Rosa D, Ilaria F et al (2019) Lymph node ratio versus TNM system as prognostic factor in colorectal cancer staging. A single Center experience Open Medicine 14:523–531
Rausei S, Iovino D, Tenconi S, Mangano A, Inversini D, Boni L et al (2013) Impact of lymph node ratio on survival of colorectal cancer patients. Int J Surg 11(Suppl 1):S95-99
Staib MDL, Link MDKH, Blatz A, Beger MDHG (2002) Surgery of colorectal cancer: surgical morbidity and five- and ten-year results in 2400 patients—monoinstitutional experience. World J Surg 26:59–66
van den Bosch T, Warps A-LK, de Nerée Tot Babberich MPM, Stamm C, Geerts BF, Vermeulen L et al (2021) Predictors of 30-day mortality among Dutch patients undergoing colorectal cancer surgery, 2011–2016. JAMA Netw Open 4:e217737
Baré M, Mora L, Torà N, Gil MJ, Barrio I, Collera P et al (2018) CCR-CARESS score for predicting operative mortality in patients with colorectal cancer. Br J Surg 105:1853–1861
Novello M, Mandarino FV, Di Saverio S, Gori D, Lugaresi M, Duchi A et al (2019) Post-operative outcomes and predictors of mortality after colorectal cancer surgery in the very elderly patients. Heliyon 5:e02363
Liao K-C, Chuang H-C, Chien C-Y, Lin Y-T, Tsai M-H, Su Y-Y et al (2021) Quality of life as a mediator between cancer stage and long-term mortality in nasopharyngeal cancer patients treated with intensity-modulated radiotherapy. Cancers 13:5063
Jörling M, Rutzner S, Hecht M, Fietkau R, Distel LV (2020) Deterioration of health-related quality of life scores under treatment predicts longer survival. Biomed Res Int 2020:1–10
Fournier E, Jooste V, Woronoff A-S, Quipourt V, Bouvier A-M, Mercier M (2016) Health-related quality of life is a prognostic factor for survival in older patients after colorectal cancer diagnosis: a population-based study. Dig Liver Dis 48:87–93
Babić R, Babić M, Rastović P, Ćurlin M, Šimić J, Mandić K et al (2020) Resilience in health and illness. Psychiatr Danub 32:226–232
Habibpour Z, Mahmoudi H, Nir MS, Areshtanab HN (2019) Resilience and its predictors among the parents of children with cancer: a descriptive-correlational study. Indian J Palliat Care 25:79–83
Lee SJ (2006) Development and validation of a prognostic index for 4-year mortality in older adults. JAMA 295:801
Collins GS, Reitsma JB, Altman DG, Moons KGM (2015) Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. Br J Cancer 112:251–259
Acknowledgements
We are grateful for the support of the nineteen participating hospitals, to the patients who participated in the study, and to Tim Nicholson for English language editing. Open access funding provided by the University of the Basque Country.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature. This work was supported in part by grants from the Instituto de Salud Carlos III and the European Regional Development Fund (PS09/00314, PS09/00910, PS09/00746, PS09/00805, PI09/90460, PI09/90490, PI09/90453, PI09/90441, PI09/90397); the Spanish Ministry of the Economy (PID2020-115738 GB-I00); the Departments of Health (2010111098) and Education, Language Policy and Culture (IT1456-22; IT1598-22; IT-1187–19) of the Basque Government; the Research Committee of Galdakao Hospital; the REDISSEC (Red de Investigación en Servicios de Salud en Enfermedades Crónicas) thematic network of the Instituto de Salud Carlos III; and the Department of Education of the Basque Government through the Consolidated Research Group MATHMODE (IT1456-22) and the Basque Government through BMTF “Mathematical Modeling Applied to Health” Project. This study has been funded by Instituto de Salud Carlos III (ISCIII) through the projects "RD16/0001/0001" and RD21CIII/0003/0017 and co-funded by the European Union.
Author information
Authors and Affiliations
Consortia
Contributions
As a multicenter study, all authors contributed to the conception and design of the study. The material was prepared by Miren Orive, José M. Quintana, and Irantzu Barrio; data collection was performed by all authors; and analyses were performed by Irantzu Barrio and Sarai Cortajarena. The first draft of the manuscript was written by Miren Orive, José M. Quintana, and Irantzu Barrio and all authors submitted comments on preliminary versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Basque Ethics Committee (Approval Number: 11/23/2010).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Patients signed informed consent with regard to publication of their data and all personal information was kept anonymous.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised due to additional funding note.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Orive, M., Barrio, I., Lázaro, S. et al. Five-year follow-up mortality prognostic index for colorectal patients. Int J Colorectal Dis 38, 64 (2023). https://doi.org/10.1007/s00384-023-04358-0
Accepted:
Published:
DOI: https://doi.org/10.1007/s00384-023-04358-0