Abstract
Purpose
Antibiotic treatment is the treatment of choice for uncomplicated diverticulitis (uD) and can be performed for mild complicated diverticulitis (mcD). In several cases, outpatient treatment (OT) can be undertaken. This study assessed the 1-month failure rate of OT for uD/mcD compared to inpatient treatment (IT), and identified predictive factors for treatment failure.
Methods
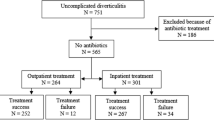
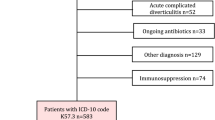
All consecutive patients (2006–2012) diagnosed with uD/mcD by CT scan were retrospectively analyzed. Acute uD was defined as absence of the following: abscess, fistula, extraluminal contrast, pneumoperitoneum, and need for immediate percutaneous drainage/surgery. Acute mcD was defined as complicated diverticulitis with abscess <4 cm or pneumoperitoneum <2 cm. All patients received antibiotherapy. Treatment failure was defined as (re)hospitalization the first month after treatment onset or need of drainage/surgery during hospitalization. All patients were contacted using a standardized questionnaire.
Results
Out of 540 uD/mcD, IT was offered to 369 patients (68%) and OT to 171 patients (32%). The IT group had higher median age, more women, higher median Charlson Index, more severe median Ambrosetti score, longer median time in the emergency room, and higher median CRP. Response rates to the questionnaire were 56% (IT) vs. 62% (OT), p = 0.18. Failure rates were 32% in IT vs. 10% in OT group, p < 0.01. Among the uD/mcD patients, admission/CT time between midnight and 6 AM, Ambrosetti score of 4, and free air around the colon were risk factors for failure.
Conclusions
Outpatient treatment for uncomplicated/mild complicated diverticulitis is feasible and safe. Prognostic factors of failure necessitating closer follow-up were admission/CT time, Ambrosetti score of 4, and free air around the colon.

Similar content being viewed by others
References
Sheth AA, Longo W, Floch MH (2008) Diverticular disease and diverticulitis. Am J Gastroenterol 103:1550–1556
Etzioni DA, Mack TM, Beart RW et al (2009) Diverticulitis in the United States: 1998-2005: changing patterns of disease and treatment. Ann Surg 249:210–217
Jacobs DO (2007) Clinical practice. Diverticulitis. N Engl J Med 57:2057–2066
Stollman N, Raskin JB (2004) Diverticular disease of the colon. Lancet 363:631–639
Chabok A, Påhlman L, Hjern F et al (2012) Randomized clinical trial of antibiotics in acute uncomplicated diverticulitis. Br J Surg 99:532–539
Jones OM, Stevenson ARL, Clark D et al (2008) Laparoscopic resection for diverticular disease: follow-up of 500 consecutive patients. Ann Surg 248:1092–1097
Vennix S, Morton DG, Hahnloser D et al (2014) Systematic review of evidence and consensus on diverticulitis: an analysis of national and international guidelines. Color Dis 16:866–878
Biondo S, Lopez Borao J, Millan M et al (2012) Current status of the treatment of acute colonic diverticulitis: a systematic review. Color Dis 14:e1–11
Etzioni DA, Chiu VY, Cannom RR et al (2010) Outpatient treatment of acute diverticulitis: rates and predictors of failure. Dis Colon Rectum 53:861–865
Biondo S, Golda T, Kreisler E et al (2014) Outpatient versus hospitalization management for uncomplicated diverticulitis: a prospective, multicenter randomized clinical trial (DIVER Trial). Ann Surg 259:38–44
Abbas MA, Cannom RR, Chiu VY et al (2013) Triage of patients with acute diverticulitis: are some inpatients candidates for outpatient treatment? Color Dis 15:451–457
Moya P, Arroyo A, Pérez-Legaz J et al (2012) Applicability, safety and efficiency of outpatient treatment in uncomplicated diverticulitis. Tech Coloproctol 16:301–307
Lorente L, Cots F, Alonso S et al (2013) Outpatient treatment of uncomplicated acute diverticulitis: impact on healthcare costs. Cir Esp 91:504–509
Sallinen VJ, Mentula PJ, Leppäniemi AK (2014) Nonoperative management of perforated diverticulitis with extraluminal air is safe and effective in selected patients. Dis Colon Rectum 57:875–881
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Ambrosetti P, Jenny A, Becker C et al (2000) Acute left colonic diverticulitis—compared performance of computed tomography and water-soluble contrast enema: prospective evaluation of 420 patients. Dis Colon Rectum 43:1363–1367
Jackson JD, Hammond T (2014) Systematic review: outpatient management of acute uncomplicated diverticulitis. Int J Color Dis 29:775–781
Unlü C, de Korte N, Daniels L et al (2010) A multicenter randomized clinical trial investigating the cost-effectiveness of treatment strategies with or without antibiotics for uncomplicated acute diverticulitis (DIABOLO trial). BMC Surg 10:23
Rueda JC, Jimenez A, Caro A et al (2012) Home treatment of uncomplicated acute diverticulitis. Int Surg 97:203–209
Andeweg CS, Mulder IM, Felt-Bersma RJF et al (2013) Guidelines of diagnostics and treatment of acute left-sided colonic diverticulitis. Dig Surg 30:278–292
Rafferty J, Shellito P, Hyman NH et al (2006) Practice parameters for sigmoid diverticulitis. Dis Colon Rectum 49:939–944
Wong WD, Wexner SD, Lowry A et al (2000) Practice parameters for the treatment of sigmoid diverticulitis—supporting documentation. The Standards Task Force. The American Society of Colon and Rectal Surgeons. Dis Colon Rectum 43:290–297
Acknowledgements
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Joliat, GR., Emery, J., Demartines, N. et al. Antibiotic treatment for uncomplicated and mild complicated diverticulitis: outpatient treatment for everyone. Int J Colorectal Dis 32, 1313–1319 (2017). https://doi.org/10.1007/s00384-017-2847-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-017-2847-z