Abstract
Purpose
Recurrent diverticulitis has been reported in 30–50% of patients who recover from an episode of diverticular-associated abscess. Our aim was to review the outcomes of patients who underwent non-operative management after percutaneous drainage (PD) of colonic diverticular abscess.
Methods
All patients with a diverticular-associated abscess were identified between 2001 and 2012. Individual charts were queried for peri-procedural data and follow-up. The most recent follow-up data were acquired via the electronic medical record or telephone call.
Results
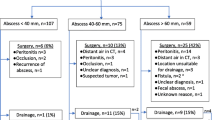
A total of 165 patients underwent PD of diverticular-associated abscesses. Abscess locations were pelvic (n = 122), abdominal (n = 36), and both (n = 7), while median abscess size was 6.1 ± 2.2 cm. One hundred eighteen patients clinically improved following non-operative management, and 81 of these patients did not undergo subsequent colonic resection within 4 months of PD. Of these, 8 died within 12 months. Among the remaining 73 patients, there were no significant differences in demographics or abscess variables compared to those who underwent elective surgery within 4 months. Only 7 of 73 patients had documented episodes of recurrences, while 22 patients later had elective surgery (1.1 ± 1.2 years from the index case). Five-year colectomy-free survival was 55% (95%CI 42–66%), while the recurrence-free survival at 5 years was 77% (95%CI 65–86%). All recurrences were managed non-operatively initially and one patient went on to have elective resection.
Conclusion
A sizable number of patients successfully recover from complicated diverticulitis following PD. Subsequent non-operative management carries an acceptable risk for recurrent episodes and may be considered as a reasonable management option.



Similar content being viewed by others
References
Bogardus ST Jr (2006) What do we know about diverticular disease? A brief overview. J Clin Gastroenterol 40(Suppl 3):S 108–S 111
Parks TG (1975) Natural history of diverticular disease of the colon. Clin Gastroenterol 4:53–69
Chapman J, Davies M, Wolff B et al (2005) Complicated diverticulitis: it is not yet time to rethink the rules! Ann Surg 242:576–581
Brandt D, Gervaz P, Durmishi Y et al (2006) Percutaneous CT scan-guided drainage vs. antibiotherapy alone for Hinchey II diverticulitis: a case-control study. Dis Colon rectum 49(10):1533–1538
Cinat ME, Wilson SE, Din AM (2002) Determinant for successful percutaneous image-guided drainage of intra-abdominal abscess. Arch Surg 137:845–849
Kaiser AM, Jiang JK, Lake JP et al (2005) The management of complicated diverticulitis and the role of computed tomography. Am J Gastroenterol 100:910–917
Myers E, Hurley M, O’Sullivan GC et al (2008) Laparoscopic peritoneal lavage for generalized peritonitis due to perforated diverticulitis. Br J Surg 95:97–101
Dharmarajan S, Hunt SR, Birnbaum EH, Fleshman JW, Mutch MG (2011) The efficacy of nonoperative management of acute complicated diverticulitis. Dis Colon rectum 54(6):663–671
Mueller MH, Glatzle J, Kasparek MS et al (2005) Long-term outcome of conservative treatment in patients with diverticulitis of the sigmoid colon. Eur J Gastroenterol Hepatol 17:649–654
Jeyarajah S, Faiz O, Bottle A et al (2009) Diverticular disease hospital admissions are increasing, with poor outcomes in the elderly and emergency admissions. Aliment Pharmacol Ther 30:1171–1182
Oomen JL, Engel AF, Cuesta MA et al (2006) Outcome of elective primary surgery for diverticular disease of the sigmoid colon: a risk analysis based on the POSSUM scoring system. Color Dis 8:91–97
Binda GA, Arezzo A, Serventi A et al (2012) Multicentre observational study of the natural history of left-sided acute diverticulitis. Br J Surg 99:276–285
Thaler K, Baig MK, Berho M et al (2013) Determinants of recurrence after sigmoid resection for uncomplicated diverticulitis. Dis Colon rectum 46(3):385–388
Thörn M, Graf W, Stefànsson T, Påhlman L (2002) Clinical and functional results after elective colonic resection in 75 consec-utive patients with diverticular disease. Am J Surg 183:7–11
Levack MM, Savitt LR, Berger DL et al (2012) Sigmoidectomy syndrome? Patients’ perspectives on the functional outcomes following surgery for diverticulitis. Dis Colon rectum 55(1):10–17
Egger B, Peter MK, Candinas D (2008) Persistent symptoms after elective sigmoid resection for diverticulitis. Dis Colon rectum 51(7):1044–1048
Devaraj B, Liu W, Tatum J, Cologne K, Kaiser A (2016) Medically treated diverticular abscess associated with high Ris k of recurrence and disease complications. Dis Colon rectum 59(3):208–215
Christian J, Bundgaard L (2011) Danish national guidelines for treatment of diverticular disease. Dan Med J 2012((59) (5)):C4453
Gaertner W, Willis D, Madoff R et al (2013) Percutaneous drainage of colonic diverticular abscess: is colon resection necessary? Dis Colon rectum 56(5):622–626
Elagili F, Stocchi L, Ozuner G, Dietz D, Kiran R (2014) Outcomes of percutaneous drainage without surgery for patients with diverticular abscess. Dis Colon rectum 57(3):331–336
Buchwald P, Diaxon L (2016) Henchey 1 and 2 diverticular abscesses: long-term outcome of conservative management. ANZ J Surj. doi:10.1111/anc. 13501
Lamb N, Kaiser A (2014) Elective resection versus observation after nonoperative management of complicated diverticulitis with abscess: a systemic review and meta-analysis. Disease of the colon and rectum volum 57:12
Gregersen R, Mortensen L (2016) Treatment of patients with acute diverticulitis complicated by abscess formation: a systematic review. Int J Surg 35(2016):201–208
Author information
Authors and Affiliations
Corresponding author
Additional information
Presented previously at the American College of Surgeons Clinical Conference 2014, San Francisco, CA, USA
Source of support: Ferguson Blodgett Foundation for Digestive Diseases
Rights and permissions
About this article
Cite this article
Jalouta, T., Jrebi, N., Luchtefeld, M. et al. Diverticulitis recurrence after percutaneous abscess drainage. Int J Colorectal Dis 32, 1367–1373 (2017). https://doi.org/10.1007/s00384-017-2825-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-017-2825-5