Abstract
Introduction
This study explores the association between perioperative hypoglycaemia and surgical outcomes in subjects with diabetes, undergoing colorectal surgery.
Methods
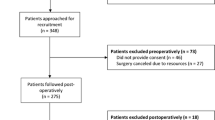
A retrospective review of 149 subjects with Type 2 Diabetes Mellitus (DM) who underwent colorectal surgery between 2010 and 2015 was performed. Perioperative glucose levels, glycated haemoglobin (HbA1c) measurements within 3 months of surgery and surgical complications based on Clavien-Dindo classification were analysed.
Results
The mean age was 67 years (67 ± 11.2). Perioperative hypoglycaemia was found in 7.4% of subjects. The mean HbA1c of subjects with Clavien 2 and above surgical complications were higher than patients with Clavien 1 or no complications, Hba1c 7.6% (7.6 ± 2.5%) and 7.0% (7.0 ± 1.1%, p = 0.008), respectively. Similar findings in subjects with Clavien 3 and above complications, HbA1c of 8.2% (8.2 ± 3.9%) as compared to those with Clavien 2 and below complications, 7.2% (7.2 ± 1.5%, p = 0.001). Adjusted multivariate analysis showed that hypoglycaemia was significantly associated with Clavien 2 and above surgical complications, OR of 19.0 (CI 2.23–162, p = 0.007). Preoperative hypoglycaemia was associated with Clavien 2 and above surgical complications, OR 10.7 (CI 1.22–94.1, p = 0.032). Suboptimal glycaemic control (Hba1c >8.0%) was significantly associated with Clavien 2 and above complications, OR 2.48 (CI 1.04–5.91, p = 0.04), but not with Clavien 3 and above complications, OR 1.50 (CI 0.450–4.98, p = 0.511).
Conclusion
Perioperative hypoglycaemia is associated with adverse surgical outcomes in diabetic patients undergoing colorectal surgery. Prevention of hypoglycaemia may improve surgical outcomes. HbA1c is an independent predictor for adverse surgical outcomes.
Similar content being viewed by others
References
Hu FB (2011) Globalization of diabetes. Diabetes Care 34(6):1249–1257. doi:10.2337/dc11-0442
Kwon S, Thompson R, Dellinger P, Yanez D, Farrohki E, Flum D (2013) Importance of perioperative glycemic control in general surgery: a report from the surgical care and outcomes assessment program. Ann Surg 257:8–14. doi:10.1097/SLA.0b013e31827b6bbc
Kansagara D, Fu R, Freeman M, Wolf F, Helfand M (2011) Intensive insulin therapy in hospitalized patients: a systematic review. Ann Intern Med 154(4):268–282. doi:10.7326/0003-4819-154-4-201102150-00008
Preiser JC, Devos P, Ruiz-Santana S, et al. (2009) A prospective randomised multi-centre controlled trial on tight glucose control by intensive insulin therapy in adult intensive care units: the Glucontrol study. Intensive Care Med 2009 Oct;35(10):1738–1748. doi: 10.1007/s00134-009-1585-2
Bagshaw SM, Bellomo R, Jacka MJ, Egi M, Hart GK, George C (2009) The impact of early hypoglycemia and blood glucose variability on outcome in critical illness. Crit Care 2009;13(3):R91. doi: 10.1186/cc7921.
Van den Berghe G, Wilmer A, Hermans G et al (2006) Intensive insulin therapy in the medical ICU. New Eng J Med 354(5):449–461
Engoren M, Schwann TA, Habib RH (2014) Hyperglycemia, hypoglycemia, and glycemic complexity are associated with worse outcomes after surgery. J Crit Care 29(4):611–617. doi:10.1016/j.jcrc.2014.03.014
Park S, Kim D, Suh GY et al (2012) Mild hypoglycemia is independently associated with increased risk of mortality in patients with sepsis: a 3-year retrospective observational study. Crit Care 16(5):R189. doi:10.1186/cc11674
Dindo D, Demartines N, Clavien P (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213. doi:10.1097/01.sla.0000133083.54934.ae
Clayton D, Woo V, Yale J (2003) Canadian Diabetes Association 2013 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada: hypoglycemia. Can J Diabetes 37:S69–S71. doi:10.1016/j.jcjd.2013.01.022
Teo BW, Koh YY, Toh QC et al (2014) Performance of the CKD-EPI creatinine-cystatin C glomerular filtration rate estimation equations in a multiethnic Asian population. Singap Med J 55(12):656–659. doi:10.11622/smedj.2014181
Ata A, Valerian BT, Lee EC, Bestle SL, Elmendorf SL, Stain SC (2010) The effect of diabetes mellitus on surgical site infections after colorectal and noncolorectal general surgical operations. Am Surg 76(7):697–702
McAnulty GR, Robertshaw HJ, Hall GM (2000) Anaesthetic management of patients with diabetes mellitus. Br J Anaesth 85(1):80–90. doi:10.1093/bja/85.1.80
Health and Social Care Information Centre (2013) National diabetes inpatient audit 2012. Leeds, West Yorkshire, England
Hypoglycemia and Clinical Outcomes in Patients with Diabetes Hospitalized in General Ward. Diabetes Care. 2009; 32(7): 1153–1157.
Mulla I, Schmidt K, Cashy J et al (2014) Comparison of glycemic and surgical outcomes after change in glycemic targets in cardiac surgery patients. Diabetes Care 37(11):2960–2965. doi:10.2337/dc14-1199
Alsahli M, Gerich JE, Navarro-González JF (2015) Hypoglycemia in patients with diabetes and renal disease. J Clin Med 4(5):948–964. doi:10.3390/jcm4050948
Aldam P, Levy N, Hall GM (2014) Perioperative management of diabetic patients: new controversies. Br J Anaesth. doi:10.1093/bja/aeu259
Halkos ME, Lattouf OM, Puskas JD et al (2008) Elevated preoperative hemoglobin A1c level is associated with reduced long-term survival after coronary artery bypass surgery. Ann Thorac Surg 86(5):1431–1437. doi:10.1016/j.athoracsur.2008.06.078
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human rights
For this type of study, formal consent is not required.
Statement on the welfare of animals
This article does not contain any studies with animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Goh, S.N.S., Yeoh, E. & Tan, K.Y. Impact of perioperative hypoglycaemia in subjects with diabetes undergoing colorectal surgery. Int J Colorectal Dis 32, 209–214 (2017). https://doi.org/10.1007/s00384-016-2680-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-016-2680-9