Abstract
Purpose
Laparoscopic ventral rectopexy (LVR) is an established surgical technique for the treatment of both rectal prolapse and symptomatic rectoceles. It is, however, not known whether LVR influences sexual function (SF). The aim of this study was, therefore, to determine the impact of this procedure on the SF of patients.
Methods
All female patients after LVR procedure in a single institution were identified and were sent a questionnaire concerning SF. This addressed sexual activity, satisfaction, preoperative SF, and the impact of surgery on SF. Furthermore, the PISQ-12 validated sexual functioning questionnaire was sent to all female patients.
Results
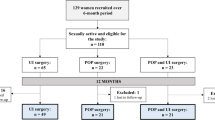
A total of 217 patients were sent a questionnaire. These patients underwent LVR for rectal prolapse, symptomatic rectocele, or enterocele between 2004 and 2011. Mean age was 62 years (range 22–89). Mean follow-up was 30 months (range 5–83). Response rate was 64 % (139 patients). The number of sexual active patients dropped from 71 to 54 % after surgery. The number of patients being satisfied with their SF remained relatively equal; 91 % of patients before and 85 % of patients after surgery. Forty-three percent of patients stated that the LVR procedure did not influence their sexual function, in 16 % of patients, the procedure positively influenced their SF, and in 13 % of respondents, SF decreased after surgery. The mean PISQ-12 score postoperatively was 34 out of 48.
Conclusions
The impact of LVR on SF of patients seems limited in this cross-sectional study in a large cohort of patients.
Similar content being viewed by others
References
D’Hoore A, Cadoni R, Penninckx F (2004) Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg 91(11):1500–1505
D’Hoore A, Penninckx F (2006) Laparoscopic ventral recto(colpo)pexy for rectal prolapse: surgical technique and outcome for 109 patients. Surg Endosc 20(12):1919–1923
Collinson R, Wijffels N, Cunningham C, Lindsey I (2010) Laparoscopic ventral rectopexy for internal rectal prolapse: short-term functional results. Colorectal Dis 12((2):97–104
van den Esschert JW, van Geloven AA, Vermulst N et al (2008) Laparoscopic ventral rectopexy for obstructed defecation syndrome. Surg Endosc 22(12):2728–2732
Wong MT, Abet E, Rigaud J et al (2011) Minimally invasive ventral mesh rectopexy for complex rectocele: impact on anorectal and sexual function. Colorectal Dis 13(10):e320–e326
Wijffels N, Cunningham C, Dixon A, Greenslade G, Lindsey I (2011) Laparoscopic ventral rectopexy for external rectal prolapse is safe and effective in the elderly. Does this make perineal procedures obsolete? Colorectal Dis 13(5):561–566
Paraiso MF, Barber MD, Muir TW, Walters MD (2006) Rectocele repair: a randomized trial of three surgical techniques including graft augmentation. Am J Obstet Gynecol 195(6):1762–1771
Klinge U, Klosterhalfen B, Muller M, Ottinger AP, Schumpelick V (1998) Shrinking of polypropylene mesh in vivo: an experimental study in dogs. Eur J Surg 164(12):965–969
Feiner B, Maher C (2010) Vaginal mesh contraction: definition, clinical presentation, and management. Obstet Gynecol 115(2 Pt 1):325–330
Rogers RG (2011) To mesh or not to mesh: current debates in prolapse repair fueled by the US Food and Drug Administration Safety Notification. Obstet Gynecol 118(4):771–773
Steinberg AC (2011) Use of vaginal mesh in the face of the recent FDA warnings and litigation. Am J Obstet Gynecol 204(6):e10–e11
Rogers RG, Coates KW, Kammerer-Doak D, Khalsa S, Qualls C (2003) A short form of the Pelvic Organ Prolapse/Urinary Incontinence Sexual Questionnaire (PISQ-12). Int Urogynecol J Pelvic Floor Dysfunct 14(3):164–168
Milani AL, Withagen MI (2011) The HS, Nedelcu-van dW, I, Vierhout ME. Sexual function following trocar-guided mesh or vaginal native tissue repair in recurrent prolapse: a randomized controlled trial. J Sex Med 8(10):2944–2953
Wild D, Grove A, Martin M et al (2005) Principles of good practice for the translation and cultural adaptation process for patient-reported outcomes (PRO) measures: report of the ISPOR task force for translation and cultural adaptation. Value Health 8(2):94–104
Geller EJ, Parnell BA, Dunivan GC (2011) Pelvic floor function before and after robotic sacrocolpopexy: one-year outcomes. J Minim Invasive Gynecol 18(3):322–327
Rogers RG, Kammerer-Doak D, Villarreal A, Coates K, Qualls C (2001) A new instrument to measure sexual function in women with urinary incontinence or pelvic organ prolapse. Am J Obstet Gynecol 184(4):552–558
Conflict of interest
Drs. Formijne Jonkers, Draaisma, Consten and Broeders, and Ms. Poierrié have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Formijne Jonkers, H.A., Poierrié, N., Draaisma, W.A. et al. Impact of rectopexy on sexual function: a cohort analysis. Int J Colorectal Dis 28, 1579–1582 (2013). https://doi.org/10.1007/s00384-013-1736-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-013-1736-3