Abstract
Purpose
The use of selective leukocytapheresis for the treatment of ulcerative colitis (UC) has been evaluated in several open and controlled trials, with varying outcomes. A meta-analysis was performed to better assess the efficacy and safety of selective leukocytapheresis as supplemental therapy compared with conventional pharmacotherapy in patients with UC.
Methods
All randomized trials comparing selective leukocytapheresis supplementation with conventional pharmacotherapy were included from electronic databases and reference lists. A meta-analysis that pooled the outcome effects of leukocytapheresis and pharmacotherapy was performed. A fixed effect model or random effect model was selected depending on the heterogeneity test of the trials.
Results
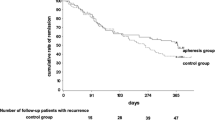
Nine randomized controlled trials met the inclusion criteria contributing a total of 686 participants. Compared with conventional pharmacotherapy, leukocytapheresis supplementation presented a significant benefit in promoting a response rate (OR, 2.88, 95% CI: 1.60–5.18) and remission rate (OR, 2.04; 95% CI, 1.36–3.07) together with significant higher steroid-sparing effects (OR, 10.49; 95% CI, 3.44–31.93) in patients with active moderate-to-severe UC by intention-to-treat analysis. Leukocytapheresis was more effective in maintaining clinical remission for asymptomatic UC patients than conventional therapy (OR, 8.14; 95% CI, 2.22–29.90). The incidence of mild–moderate adverse effects was much less frequent in the leukocytapheresis groups than conventional pharmacotherapy groups (OR, 0.16; 95% CI, 0.04–0.60). Few severe adverse events were observed.
Conclusions
Current data indicate that leukocytapheresis supplementation may be more efficacious on improving response and remission rates and tapering corticosteroid dosage with excellent tolerability and safety than conventional pharmacotherapy in patients with UC. In addition, more high-quality randomized controlled trials are required to confirm the higher efficacy of leukocytapheresis in patients with UC.





Similar content being viewed by others
References
Rugtveit J, Brandtzaeg P, Halstensen TS (1994) Increased macrophage subsets in inflammatory bowel disease: apparent recruitment from peripheral blood monocytes. Gut 35:669–674
Meuret G, Bitzi A, Hammer B (1978) Macrophage turnover in Crohn's disease and ulcerative colitis. Gastroenterol 74:501–503
Mahida YR (1997) Monocytes and macrophages in inflammatory bowel disease. In: Allan RN, Rhodes JM, Hanauer SB, Keighley MRB, Alexander-Williams J, Fazio VW (eds) Inflamatory bowel diseases, 3rd edn. Churchill Livingstone, New York, pp 81–85
Sharon P, Stenson WF (1984) Enhanced synthesis of leukotriene B4 by colonic mucosa in inflammatory bowel disease. Gastroenterol 86:453–460
Balfour S (1994) Cytokines in inflammatory bowel disease: pathophysiology and clinical considerations. Gastroenterol 106:533–539
Nikolaus S, Bauditz J, Gionchetti P (1998) Increased secretion of proinflammatory cytokines by circulating polymorphonuclear neutrophils and regulation by interleukin-10 during intestinal inflammation. Gut 42:470–476
Kaplanski G, Marin V, Montero-Julian F (2003) IL-6: a regulator of the transition from neutrophil to monocyte recruitment during inflammation. Trends Immunol 24:25–29
Hanai H, Watanabe F, Takeuchi K et al (2003) Leukocyte adsorptive apheresis for the treatment of active ulcerative colitis: a prospective, uncontrolled, pilot study. Clin Gastroenterol Hepatol 1:28–35
Rembacken BJ, Newbould HE, Richards SJ et al (1998) Granulocyte apheresis in inflammatory bowel disease: possible mechanisms of effect. Ther Apher 2:93–96
Ayabe T, Ashida T, Taniguchi M et al (1997) A pilot study of centrifugal leukocyte apheresis for corticosteroid-resistant active ulcerative colitis. Intern Med 36:322–326
Saniabadi AR, Hanai H, Takeuchi K et al (2003) Adacolumn, an adsorptive carrier based granulocyte and monocyte apheresis device for the treatment of inflammatory and refractory diseases associated with leukocytes. Ther Apher Dial 7:48–59
Hiraishi K, Takeda Y, Shiobara N et al (2003) Studies on the mechanisms of leukocyte adhesion to cellulose acetate beads: an in vitro model to assess the efficacy of cellulose acetate carrier-based granulocyte and monocyte adsorptive apheresis. Ther Apher Dial 7:334–340
Sawada K, Ohnishi K, Kosaka T et al (1997) Leukocytapheresis with leukocyte removal filter as new therapy for ulcerative colitis. Ther Apher 1:207–211
Bresci G, Parisi G, Mazzoni A, Scatena F, Capria A (2007) Treatment of patients with acute ulcerative colitis: conventional corticosteroid therapy (MP) versus granulocytapheresis (GMA): a pilot study. Dig Liver Dis 39:430–434
Domènech E, Hinojosa J, Esteve-Comas M et al (2004) Granulocyteaphaeresis in steroid-dependent inflammatory bowel disease: a prospective, open, pilot study. Aliment Pharmacol Ther 20:1347–1352
Shimoyama T, Sawada K, Tanaka T et al (1999) Granulocyte and monocyte apheresis with the G-1 column in the treatment of patients with active ulcerative colitis. Jpn J Apher 18:117–131
Sawada K, Muto T, Shimoyama T et al (2003) Multicenter randomized controlled trial for the treatment of ulcerative colitis with a leukocytapheresis column. Curr Pharm Des 9:307–321
Kjaergard LL, Villumsen J, Gluud C (2001) Reported methodologic quality and discrepancies between large and small randomized trials in meta-analyses. Ann Intern Med 135:982–989
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–634
Hanai H, Watanabe F, Yamada M et al (2004) Adsorptive granulocyte and monocyte apheresis versus prednisolone in patients with corticosteroid-dependent moderately severe ulcerative colitis. Digestion 70:36–44
Nakamura T, Kawagoe Y, Matsuda T et al (2004) Effect of granulocyte and monocyte adsorption apheresis on urinary albumin excretion and plasma endothelin-1 concentration in patients with active ulcerative colitis. Blood Purif 22:499–504
Bresci G, Parisi G, Mazzoni A, Scatena F, Capria A (2008) Granulocytapheresis versus methylprednisolone in patients with acute ulcerative colitis: 12-month follow up. J Gastroenterol Hepatol 23:1678–1682
Hanai H, Iida T, Takeuchi K et al (2008) Intensive granulocyte and monocyte adsorption versus intravenous prednisolone in patients with severe ulcerative colitis: an unblinded randomised multi-centre controlled study. Dig Liver Dis 40:433–440
Sands BE, Sandborn WJ, Feagan B et al (2008) A randomized, double-blind, sham-controlled study of granulocyte/monocyte apheresis for active ulcerative colitis. Gastroenterol 135:400–409
Maiden L, Takeuchi K, Baur R et al (2008) Selective white cell apheresis reduces relapse rates in patients with IBD at significant risk of clinical relapse. Inflamm Bowel Dis 14:1413–1418
Emmrich J, Petermann S, Nowak D et al (2007) Leukocytapheresis (LCAP) in the management of chronic active ulcerative colitis–results of a randomized pilot trial. Dig Dis Sci 52:2044–2053
Sakuraba A, Motoya S, Watanabe K et al (2009) An open-label prospective randomized multicenter study shows very rapid remission of ulcerative colitis by intensive granulocyte and monocyte adsorptive apheresis as compared with routine weekly treatment. Am J Gastroenterol 104:2990–2995
Sakata Y, Iwakiri R, Amemori S et al (2008) Comparison of the efficacy of granulocyte and monocyte/macrophage adsorptive apheresis and leukocytapheresis in active ulcerative colitis patients: a prospective randomized study. Eur J Gastroenterol Hepatol 20:629–633
Hidaka T, Suzuki K, Kawakami M et al (2001) Dynamic changes in cytokine levels in serum and synovial fluid following filtration leukocytapheresis therapy in patients with rheumatoid arthritis. J Clin Apher 16:74–81
Shimoyama T, Sawada K, Hiwatashi N et al (2001) Safety and efficacy of granulocyte and monocyte adsorption apheresis in patients with active ulcerative colitis: a multicenter study. J Clin Apher 16:1–9
Sawada K, Kusugami K, Suzuki Y et al (2005) Leukocytapheresis in ulcerative colitis: results of a multicenter double-blind prospective case-control study with sham apheresis as placebo treatment. Am J Gastroenterol 100:1362–1369
Hibi T, Sakuraba A (2005) Is there a role for apheresis in gastrointestinal disorders? Nat Clin Pract Gastroenterol Hepatol 2:200–201
Acknowledgments
This study was supported by the outstanding academic leader's project, Science and Technology Commission of Shanghai (10XD1402600).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhu, M., Xu, X., Nie, F. et al. The efficacy and safety of selective leukocytapheresis in the treatment of ulcerative colitis: a meta-analysis. Int J Colorectal Dis 26, 999–1007 (2011). https://doi.org/10.1007/s00384-011-1193-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-011-1193-9