Abstract
Purpose
We aim to evaluate the diagnostic performance and relationship between clinical characteristics, imaging findings, and final diagnosis for the neonatal contrast enema (CE).
Methods
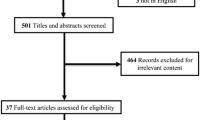
Retrospective 10-year review of all neonatal CEs including imaging findings, clinical information, indication, and final diagnosis from discharge summaries, surgical reports, and pathology (reference standard). Two blinded pediatric radiologists reinterpreted 366 CEs for obstruction, microcolon, rectosigmoid index (RSI), serrations, meconium, ileal cut-off, transition zone, diagnosis, and level of confidence. CE diagnostic performance was calculated versus reference standard.
Results
Diagnoses included Hirschsprung disease (HD) (15.8%), small left colon syndrome (14.8%), small intestinal atresia/colonic atresia (SIA/CA) (12.6%), meconium ileus (MI) (4.4%), and normal (48.9%). CE had a moderate specificity (87.7%) and low sensitivity (65.5%) for HD; abnormal RSI and serrations showed high specificities (90.3%, 97.4%) but low sensitivities (46.6%, 17.2%). CE showed high specificity (97.4%) and low sensitivity (56.3%) for MI blinded to cystic fibrosis status. Microcolon was specific (96.6%) but not sensitive (68.8%) for MI. CE showed highest PPV (73.1%) (specificity 95.6%, sensitivity 82.6%) for SIA/CA. Microcolon with an abrupt cut-off was specific (99.1%) but not sensitive (41.3%) for atresias.
Conclusion
Neonatal CE demonstrates high specificities and low to moderate sensitivities across all diagnoses, with lowest performance in HD.
Clinical trial registration
None.




Similar content being viewed by others
Abbreviations
- CE:
-
Contrast enema
- RSI:
-
Ectosigmoid index
- Z:
-
Transition zone
- HD:
-
Hirschsprung disease
- SLCS:
-
Small left colon syndrome
- SIA:
-
Small intestinal atresia
- CA:
-
Colonic atresia
- MI:
-
Meconium ileus
- CF:
-
Cystic fibrosis
References
Alehossein M, Roohi A, Pourgholami M et al (2015) Diagnostic accuracy of radiologic scoring system for evaluation of suspicious hirschsprung disease in children. Iran J Radiol 12:e12451. https://doi.org/10.5812/iranjradiol.12451
Putnam LR, John SD, Greenfield SA et al (2015) The utility of the contrast enema in neonates with suspected hirschsprung disease. J Pediatr Surg 50:963–966. https://doi.org/10.1016/j.jpedsurg.2015.03.019
Garcia R, Arcement C, Hormaza L et al (2007) Use of the recto-sigmoid index to diagnose hirschsprung’s disease. Clin Pediatr (Phila) 46:59–63. https://doi.org/10.1177/0009922806289328
Hwang TJ, Servaes S, Mattei P, Anupindi SA (2017) Radiologist performance in the interpretation of contrast enemas performed for hirschsprung’s disease in children >1 year of age. Clin Radiol 72:519.e11–519.e19. https://doi.org/10.1016/j.crad.2017.01.007
Burge D, Drewett M (2004) Meconium plug obstruction. Pediatr Surg Int 20:108–110. https://doi.org/10.1007/s00383-003-1098-y
Ellis DG, William Clatworthy H (1966) The meconium plug syndrome revisited. J Pediatr Surg 1:54–61. https://doi.org/10.1016/0022-3468(66)90008-X
Keckler SJ, St Peter SD, Spilde TL et al (2008) Current significance of meconium plug syndrome. J Pediatr Surg 43:896–898. https://doi.org/10.1016/j.jpedsurg.2007.12.035
Cuenca AG, Ali AS, Kays DW, Islam S (2012) “Pulling the plug”—management of meconium plug syndrome in neonates. J Surg Res 175:e43–e46. https://doi.org/10.1016/j.jss.2012.01.029
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174. https://doi.org/10.2307/2529310
Amodio J, Berdon W, Abramson S, Stolar C (1986) Microcolon of prematurity: a form of functional obstruction. AJR Am J Roentgenol 146:239–244. https://doi.org/10.2214/ajr.146.2.239
Berdon WE, Baker DH, Santulli TV et al (1968) Microcolon in newborn infants with intestinal obstruction. Its correlation with the level and time of onset of obstruction. Radiology 90:878–885. https://doi.org/10.1148/90.5.878
Carroll AG, Kavanagh RG, Ni Leidhin C et al (2016) Comparative effectiveness of imaging modalities for the diagnosis of intestinal obstruction in neonates and infants: a critically appraised topic. Acad Radiol 23:559–568. https://doi.org/10.1016/j.acra.2015.12.014
Berrocal T, Lamas M, Gutieérrez J et al (1999) Congenital anomalies of the small intestine, colon, and rectum. Radiographics 19:1219–1236. https://doi.org/10.1148/radiographics.19.5.g99se041219
Escobar MA, Grosfeld JL, Burdick JJ et al (2005) Surgical considerations in cystic fibrosis: a 32-year evaluation of outcomes. Surgery 138:560–571. https://doi.org/10.1016/j.surg.2005.06.049 (discussion 571)
Carlyle BE, Borowitz DS, Glick PL (2012) A review of pathophysiology and management of fetuses and neonates with meconium ileus for the pediatric surgeon. J Pediatr Surg 47:772–781. https://doi.org/10.1016/j.jpedsurg.2012.02.019
Farrell PM, Rosenstein BJ, White TB et al (2008) Guidelines for diagnosis of cystic fibrosis in newborns through older adults: cystic fibrosis foundation consensus report. J Pediatr 153:S4–S14. https://doi.org/10.1016/j.jpeds.2008.05.005
Fakhoury K, Durie PR, Levison H, Canny GJ (1992) Meconium ileus in the absence of cystic fibrosis. Arch Dis Child 67:1204–1206
De Lorijn F, Reitsma JB, Voskuijl WP et al (2005) Diagnosis of hirschsprung’s disease: a prospective, comparative accuracy study of common tests. J Pediatr 146:787–792. https://doi.org/10.1016/j.jpeds.2005.01.044
Hope JW, Borns PF, Berg PK (1965) Roentgenologic manifestations of hirschsprung’s disease in infancy. Am J Roentgenol Radium Ther Nucl Med 95:217–229. https://doi.org/10.2214/ajr.95.1.217
O’Donovan AN, Habra G, Somers S et al (1996) Diagnosis of Hirschsprung’s disease. AJR Am J Roentgenol 167:517–520. https://doi.org/10.2214/ajr.167.2.8686640
Lewis NA, Levitt MA, Zallen GS et al (2003) Diagnosing Hirschsprung’s disease: increasing the odds of a positive rectal biopsy result. J Pediatr Surg 38:412–416. https://doi.org/10.1053/jpsu.2003.50070 (discussion 412)
Diamond IR, Casadiego G, Traubici J et al (2007) The contrast enema for hirschsprung disease: predictors of a false-positive result. J Pediatr Surg 42:792–795. https://doi.org/10.1016/j.jpedsurg.2006.12.031
Taxman TL, Yulish BS, Rothstein FC (1986) How useful is the barium enema in the diagnosis of infantile hirschsprung’s disease? Am J Dis Child 140:881–884
Reid JR (2012) Practical imaging approach to bowel obstruction in neonates: a review and update. Semin Roentgenol 47:21–31. https://doi.org/10.1053/j.ro.2011.07.003
Chandler NW, Zwiren GT (1970) Complete reflux of the small bowel in total colon hirschsprung’s disease. Radiology 94:335–339. https://doi.org/10.1148/94.2.335
De Campo JF, Mayne V, Boldt DW, De Campo M (1984) Radiological findings in total aganglionosis coli. Pediatr Radiol 14:205–209. https://doi.org/10.1007/BF01042242
Stranzinger E, DiPietro MA, Teitelbaum DH, Strouse PJ (2008) Imaging of total colonic hirschsprung disease. Pediatr Radiol 38:1162–1170. https://doi.org/10.1007/s00247-008-0952-4
Funding
The authors have no financial relationships relevant to this article to disclose. This project was completed without a specific funding source.
Author information
Authors and Affiliations
Contributions
Dr. Reid conceptualized and designed the study, supervised data collection, and reviewed and revised the manuscript. Dr. Baad collected data, conducted the initial analysis, drafted the initial manuscript, and reviewed and revised the manuscript. Dr. Delgado conceptualized and designed the study, collected data, conducted statistical data analysis, and reviewed and revised the manuscript. Ms. Dayneka conducted data analysis and reviewed and revised the manuscript. Dr. Anupindi collected data and reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the institutional review board of the Children’s Hospital of Philadelphia and is compliant with the 1964 Helsinki declaration and its later amendments. This retrospective study was approved by the institutional review board of the Children’s Hospital of Philadelphia and compliant with the Health Insurance Portability and Accountability Act.
Informed consent
The requirement to obtain informed consent for this retrospective study was waived by our institutional review board.
Consent to participate
The requirement to obtain informed consent was waived.
Consent to publish
The requirement to obtain informed consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Baad, M., Delgado, J., Dayneka, J.S. et al. Diagnostic performance and role of the contrast enema for low intestinal obstruction in neonates. Pediatr Surg Int 36, 1093–1101 (2020). https://doi.org/10.1007/s00383-020-04701-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-020-04701-4