Abstract
Aim of the study
The use of autologous bio-engineered dermo-epidermal skin substitutes (DESS) yields a pivotal opportunity to cover large skin defects in human patients. These skin grafts consist of both epidermal and dermal compartments necessary for robust and permanent functional wound closure. In this study, we investigated the impact of mesenchymal cells derived from different body site origins on the expression pattern of diverse markers within DESS.
Methods
Human keratinocytes were obtained from interfollicular epidermis, and mesenchymal cells were isolated from foreskin, palmar skin, fat tissue, and tonsils. After expansion, epidermal cells were seeded on collagen I hydrogels containing stromal cells. These human DESS were transplanted on the back of immune-incompetent rats. After 3 weeks, transplants were excised and analyzed using immunohistology techniques.
Main results
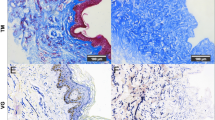
The macroscopic appearance of skin grafts containing tonsil, fat tissue, or palmar derived mesenchymal cells, was similar to substitutes with foreskin derived dermal fibroblasts. All skin grafts had a strong membrane-localized expression of Lingo-1 in the epidermis. Additionally, we observed an intense expression of transglutaminase 5 in upper epidermal cell layers of the skin grafts confirming a proper keratinocyte differentiation. Tropoelastin was localized throughout the dermal compartments and tightly in contact with the dermo-epidermal junction suggesting an advanced maturation of all skin grafts.
Conclusions
Our data implicate that stromal cells derived from tonsil, fat tissue, and palmar skin can assume fibroblast functions supporting keratinocyte proliferation and differentiation. These findings indicate that distinct types of mesenchymal cells can be clinically used for skin engineering purposes.



Similar content being viewed by others
References
Chua AW, Khoo YC, Tan BK, Tan KC, Foo CL, Chong SJ (2016) Skin tissue engineering advances in severe burns: review and therapeutic applications. Burns Trauma 4:3
Schiestl C, Stiefel D, Meuli M (2010) Giant naevus, giant excision, eleg(i)ant closure? Reconstructive surgery with Integra artificial skin to treat giant congenital melanocytic naevi in children. J Plast Reconstr Aesthet Surg 63:610–615
Meyer U (2009) Fundamentals of tissue engineering and regenerative medicine. Springer, Berlin, p 333
Oconnor NE, Mulliken JB, Banksschlegel S, Kehinde O, Green H (1981) Grafting of burns with cultured epithelium prepared from autologous epidermal-cells. Lancet 1:75–78
Gallico GG 3rd, O’Connor NE, Compton CC, Kehinde O, Green H (1984) Permanent coverage of large burn wounds with autologous cultured human epithelium. N Engl J Med 311:448–451
Ter Horst B, Chouhan G, Moiemen NS, Grover LM (2018) Advances in keratinocyte delivery in burn wound care. Adv Drug Deliv Rev 123:18–32
Bottcher-Haberzeth S, Biedermann T, Reichmann E (2010) Tissue engineering of skin. Burns 36:450–460
Bottcher-Haberzeth S, Biedermann T, Klar AS, Pontiggia L, Rac J, Nadal D et al (2014) Tissue engineering of skin: human tonsil-derived mesenchymal cells can function as dermal fibroblasts. Pediatr Surg Int 30:213–222
Hartmann-Fritsch F, Biedermann T, Braziulis E, Meuli M, Reichmann E (2013) A new model for preclinical testing of dermal substitutes for human skin reconstruction. Pediatr Surg Int 29:479–488
Pontiggia L, Klar A, Bottcher-Haberzeth S, Biedermann T, Meuli M, Reichmann E (2013) Optimizing in vitro culture conditions leads to a significantly shorter production time of human dermo-epidermal skin substitutes. Pediatr Surg Int 29:249–256
Bottcher-Haberzeth S, Klar AS, Biedermann T, Schiestl C, Meuli-Simmen C, Reichmann E et al (2013) “Trooping the color”: restoring the original donor skin color by addition of melanocytes to bioengineered skin analogs. Pediatr Surg Int 29:239–247
Candi E, Oddi S, Paradisi A, Terrinoni A, Ranalli M, Teofoli P et al (2002) Expression of transglutaminase 5 in normal and pathologic human epidermis. J Invest Dermatol 119:670–677
Bottcher-Haberzeth S, Biedermann T, Klar AS, Widmer DS, Neuhaus K, Schiestl C et al (2015) Characterization of pigmented dermo-epidermal skin substitutes in a long-term in vivo assay. Exp Dermatol 24:16–21
Pontiggia L, Biedermann T, Meuli M, Widmer D, Bottcher-Haberzeth S, Schiestl C et al (2009) Markers to evaluate the quality and self-renewing potential of engineered human skin substitutes in vitro and after transplantation. J Invest Dermatol 129:480–490
Klar AS, Guven S, Biedermann T, Luginbuhl J, Bottcher-Haberzeth S, Meuli-Simmen C et al (2014) Tissue-engineered dermo-epidermal skin grafts prevascularized with adipose-derived cells. Biomaterials 35:5065–5078
Eoh JH, Shen N, Burke JA, Hinderer S, Xia Z, Schenke-Layland K et al (2017) Enhanced elastin synthesis and maturation in human vascular smooth muscle tissue derived from induced-pluripotent stem cells. Acta Biomater 52:49–59
Kim WS, Park SH, Ahn SJ, Kim HK, Park JS, Lee GY et al (2008) Whitening effect of adipose-derived stem cells: a critical role of TGF-beta 1. Biol Pharm Bull 31:606–610
Klar AS, Biedermann T, Michalak K, Michalczyk T, Meuli-Simmen C, Scherberich A et al (2017) Human adipose mesenchymal cells inhibit melanocyte differentiation and the pigmentation of human skin via increased expression of TGF-beta1. J Invest Dermatol 137:2560–2569
Hinz B (2015) The extracellular matrix and transforming growth factor-beta1: tale of a strained relationship. Matrix Biol 47:54–65
Eckert RL, Sturniolo MT, Broome AM, Ruse M, Rorke EA (2005) Transglutaminase function in epidermis. J Invest Dermatol 124:481–492
Wang CJ, Qu CQ, Zhang J, Fu PC, Guo SG, Tang RH (2014) Lingo-1 inhibited by RNA interference promotes functional recovery of experimental autoimmune encephalomyelitis. Anat Rec (Hoboken) 297:2356–2363
Satoh J, Tabunoki H, Yamamura T, Arima K, Konno H (2007) TROY and LINGO-1 expression in astrocytes and macrophages/microglia in multiple sclerosis lesions. Neuropathol Appl Neurobiol 33:99–107
Jain A, Zhang J, Rabbitts T (2017) LINGO-1 is a new therapy target and biomarker for Ewing sarcoma. Clin Oncol 2:1183
Choi W, Miyamura Y, Wolber R, Smuda C, Reinhold W, Liu H et al (2010) Regulation of human skin pigmentation in situ by repetitive UV exposure: molecular characterization of responses to UVA and/or UVB. J Invest Dermatol 130:1685–1696
Biedermann T, Bottcher-Haberzeth S, Klar AS, Widmer DS, Pontiggia L, Weber AD et al (2015) The influence of stromal cells on the pigmentation of tissue-engineered dermo-epidermal skin grafts. Tissue Eng Part A 21:960–969
Yamaguchi Y, Itami S, Watabe H, Yasumoto K, Abdel-Malek ZA, Kubo T et al (2004) Mesenchymal-epithelial interactions in the skin: increased expression of dickkopf1 by palmoplantar fibroblasts inhibits melanocyte growth and differentiation. J Cell Biol 165:275–285
Yamaguchi Y, Passeron T, Hoashi T, Watabe H, Rouzaud F, Yasumoto K et al (2008) Dickkopf 1 (DKK1) regulates skin pigmentation and thickness by affecting Wnt/beta-catenin signaling in keratinocytes. Faseb J 22:1009–1020
Knapp AC, Franke WW, Heid H, Hatzfeld M, Jorcano JL, Moll R (1986) Cytokeratin No. 9, an epidermal type I keratin characteristic of a special program of keratinocyte differentiation displaying body site specificity. J Cell Biol 103:657–667
Acknowledgements
This work was financially supported by the Clinical Research Priority Programs (CRPP) of the Faculty of Medicine of the University of Zurich. We are particularly grateful to the Gaydoul Foundation and the sponsors of “DonaTissue” (Thérèse Meier and Robert Zingg) for their generous financial support and interest in our work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
ER and MM are co-founding members and shareholders of “Cutiss AG”, a company to fund the further development of the tissue-engineered skin substitutes. All other authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Michalak-Micka, K., Klar, A.S., Böttcher-Haberzeth, S. et al. Impact of human mesenchymal cells of different body site origins on the maturation of dermo-epidermal skin substitutes. Pediatr Surg Int 35, 121–127 (2019). https://doi.org/10.1007/s00383-018-4383-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-018-4383-5