Abstract
Purpose
Variation in management characterizes treatment of infants with a congenital pulmonary airway malformation (CPAM). This review addresses six clinically applicable questions using available evidence to provide recommendations for the treatment of these patients.
Methods
Questions regarding the management of a pediatric patient with a CPAM were generated. English language articles published between 1960 and 2014 were compiled after searching Medline and OvidSP. The articles were divided by subject area and by the question asked, then reviewed and included if they specifically addressed the proposed question.
Results
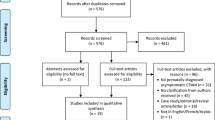
1040 articles were identified on initial search. After screening abstracts per eligibility criteria, 130 articles were used to answer the proposed questions. Based on the available literature, resection of an asymptomatic CPAM is controversial, and when performed is usually completed within the first six months of life. Lobectomy remains the standard resection method for CPAM, and can be performed thoracoscopically or via thoracotomy. There is no consensus regarding a monitoring protocol for observing asymptomatic lesions, although at least one chest computerized tomogram (CT) should be performed postnatally for lesion characterization. An antenatally identified CPAM can be evaluated with MRI if fetal intervention is being considered, but is not required for the fetus with a lesion not at risk for hydrops. Prenatal consultation should be offered for infants with CPAM and encouraged for those infants in whom characteristics indicate risk of hydrops.
Conclusions
Very few articles provided definitive recommendations for care of the patient with a CPAM and none reported Level I or II evidence. Based on available information, CPAMs are usually resected early in life if at all. A prenatally diagnosed congenital lung lesion should be evaluated postnatally with CT, and prenatal counseling should be undertaken in patients at risk for hydrops.

Similar content being viewed by others
References
Peters RT, Burge DM, Marven SS (2013) Congenital lung malformations: an ongoing controversy. Ann R Coll Surg Engl 95(2):144–147
Baird R, Puligandla PS, Laberge JM (2014) Congenital lung malformations: informing best practice. Semin Pediatr Surg 23(5):270–277. doi:10.1053/j.sempedsurg.2014.09.007
Kapralik J, Wayne C, Chan E, Nasr A (2016) Surgical versus conservative management of congenital pulmonary airway malformation in children: a systematic review and meta-analysis. J Pediatr Surg 51(3):508–512. doi:10.1016/j.jpedsurg.2015.11.022
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6(7):e1000100. doi:10.1371/journal.pmed.1000100
Stanton M, Njere I, Ade-Ajayi N, Patel S, Davenport M (2009) Systematic review and meta-analysis of the postnatal management of congenital cystic lung lesions. J Pediatr Surg 44(5):1027–1033
Ng C, Stanwell J, Burge DM, Stanton MP (2014) Conservative management of antenatally diagnosed cystic lung malformations. Arch Dis Child 99(5):432–437
Wong A, Vieten D, Singh S, Harvey JG, Holland AJ (2009) Long-term outcome of asymptomatic patients with congenital cystic adenomatoid malformation. Pediatr Surg Int 25(6):479–485
Wang A, D’Amico TA, Berry MF (2014) Surgical management of congenital pulmonary malformations after the first decade of life. Ann Thorac Surg 97(6):1933–1938
Kamata S, Usui N, Kamiyama M, Nose K, Sawai T, Fukuzawa M (2006) Long-term outcome in patients with prenatally diagnosed cystic lung disease: special reference to ventilation and perfusion scan in the affected lung. J Pediatr Surg 41(12):2023–2027
Khosa JK, Leong SL, Borzi PA (2004) Congenital cystic adenomatoid malformation of the lung: indications and timing of surgery. Pediatr Surg Int 20(7):505–508
Laberge JM, Puligandla P, Flageole H (2005) Asymptomatic congenital lung malformations. Semin Pediatr Surg 14(1):16–33
Priest JR, Williams GM, Hill DA, Dehner LP, Jaffe A (2009) Pulmonary cysts in early childhood and the risk of malignancy. Pediatr Pulmonol 44(1):14–30. doi:10.1002/ppul.20917
Nasr A, Himidan S, Pastor AC, Taylor G, Kim PC (2010) Is congenital cystic adenomatoid malformation a premalignant lesion for pleuropulmonary blastoma? J Pediatr Surg 45(6):1086–1089
Aziz D, Langer JC, Tuuha SE, Ryan G, Ein SH, Kim PC (2004) Perinatally diagnosed asymptomatic congenital cystic adenomatoid malformation: to resect or not? J Pediatr Surg 39(3):329–334 (discussion 329–334)
Feinberg A, Hall NJ, Williams GM, Schultz KA, Miniati D, Hill DA, Dehner LP, Messinger YH, Langer JC (2016) Can congenital pulmonary airway malformation be distinguished from Type I pleuropulmonary blastoma based on clinical and radiological features? J Pediatr Surg 51(1):33–37. doi:10.1016/j.jpedsurg.2015.10.019
Hammond PJ, Devdas JM, Ray B, Ward-Platt M, Barrett AM, McKean M (2010) The outcome of expectant management of congenital cystic adenomatoid malformations (CCAM) of the lung. Eur J Pediatr Surg 20(3):145–149
Hsieh CC, Chao AS, Chang YL, Kuo DM, Hsieh TT, Hung HT (2005) Outcome of congenital cystic adenomatoid malformation of the lung after antenatal diagnosis. Int J Gynaecol Obstet 89(2):99–102
Kongstad T, Buchvald F, Brenoe J, Petersen BL, Tabor A, Nielsen KG (2012) Radiology, histology and short-term outcome of asymptomatic congenital thoracic malformations. Acta Paediatr 101(2):155–158
Lo AY, Jones S (2008) Lack of consensus among Canadian pediatric surgeons regarding the management of congenital cystic adenomatoid malformation of the lung. J Pediatr Surg 43(5):797–799
Mentzer SJ, Filler RM, Phillips J (1992) Limited pulmonary resections for congenital cystic adenomatoid malformation of the lung. J Pediatr Surg 27(11):1410–1413
Revillon Y, Jan D, Plattner V, Sonigo P, Dommergues M, Mandelbrot L, Dumez Y, Nihoul-Fekete C (1993) Congenital cystic adenomatoid malformation of the lung: prenatal management and prognosis. J Pediatr Surg 28(8):1009–1011
Roggin KK, Breuer CK, Carr SR, Hansen K, Kurkchubasche AG, Wesselhoeft CW Jr, Tracy TF Jr, Luks FI (2000) The unpredictable character of congenital cystic lung lesions. J Pediatr Surg 35(5):801–805
Sauvat F, Michel JL, Benachi A, Emond S, Revillon Y (2003) Management of asymptomatic neonatal cystic adenomatoid malformations. J Pediatr Surg 38(4):548–552
Sueyoshi R, Okazaki T, Urushihara N, Fujiwara T, Tobayama S, Fukumoto K, Horigome F, Tei E, Lane GJ, Hasegawa S, Yamataka A (2008) Managing prenatally diagnosed asymptomatic congenital cystic adenomatoid malformation. Pediatr Surg Int 24(10):1111–1115
Takeda S, Miyoshi S, Inoue M, Omori K, Okumura M, Yoon HE, Minami M, Matsuda H (1999) Clinical spectrum of congenital cystic disease of the lung in children. Eur J Cardiothorac Surg 15(1):11–17
Abecasis F, Gomes Ferreira M, Oliveira A, Vaz Velho H (2008) Bronchioloalveolar carcinoma associated with congenital pulmonary airway malformation in an asymptomatic adolescent. Revista Portuguesa de Pneumologia 14(2):285–290
Valfre L, Conforti A, Nahom A, Bagolan P (2010) The outcome of expectant management of congenital cystic adenomatoid malformation of the lung. European Journal of Pediatric Surgery 20(6):412 (author reply 412)
van Leeuwen K, Teitelbaum DH, Hirschl RB, Austin E, Adelman SH, Polley TZ, Marshall KW, Coran AG, Nugent C (1999) Prenatal diagnosis of congenital cystic adenomatoid malformation and its postnatal presentation, surgical indications, and natural history. Journal of Pediatric Surgery 34(5):794–798 (discussion 798–799)
Tran H, Fink MA, Crameri J, Cullinane F (2008) Congenital cystic adenomatoid malformation: monitoring the antenatal and short-term neonatal outcome. Aust N Z J Obstet Gynaecol 48(5):462–466
Doros L, Schultz KA, Stewart DR, Bauer AJ, Williams G, Rossi CT, Carr A, Yang J, Dehner LP, Messinger Y, Hill DA (1993) DICER1-related disorders. In: Pagon RA, Adam MP, Ardinger HH et al (eds) GeneReviews(R). University of Washington, Seattle
Nishibayashi SW, Andrassy RJ, Woolley MM (1981) Congenital cystic adenomatoid malformation: 1 30-year experience. J Pediatr Surg 16(5):704–706
Browdie D, Todd D, Agnew R, Rosen W, Beardmore H (1993) The use of “nonanatomic” pulmonary resection in infants with extensive congenital adenomatoid malformation of the lung. J Thorac Cardiovasc Surg 105(4):732–736
Sapin E, Lejeune V, Barbet JP, Carricaburu E, Lewin F, Baron JM, Barbotin-Larrieu F, Helardot PG (1997) Congenital adenomatoid disease of the lung: prenatal diagnosis and perinatal management. Pediatr Surg Int 12(2–3):126–129
Waszak P, Claris O, Lapillonne A, Picaud JC, Basson E, Chappuis JP, Salle BL (1999) Cystic adenomatoid malformation of the lung: neonatal management of 21 cases. Pediatr Surg Int 15(5–6):326–331
Kim HK, Choi YS, Kim K, Shim YM, Ku GW, Ahn KM, Lee SI, Kim J (2008) Treatment of congenital cystic adenomatoid malformation: should lobectomy always be performed? Ann Thorac Surg 86(1):249–253
Johnson SM, Grace N, Edwards MJ, Woo R, Puapong D (2011) Thoracoscopic segmentectomy for treatment of congenital lung malformations. J Pediatr Surg 46(12):2265–2269
Fascetti-Leon F, Gobbi D, Pavia SV, Aquino A, Ruggeri G, Gregori G, Lima M (2013) Sparing-lung surgery for the treatment of congenital lung malformations. J Pediatr Surg 48(7):1476–1480
Bagrodia N, Cassel S, Liao J, Pitcher G, Shilyansky J (2014) Segmental resection for the treatment of congenital pulmonary malformations. J Pediatr Surg 49(6):905–909. doi:10.1016/j.jpedsurg.2014.01.021
Cagle PT, Thurlbeck WM (1988) Postpneumonectomy compensatory lung growth. Am Rev Respir Dis 138(5):1314–1326. doi:10.1164/ajrccm/138.5.1314
Nakajima C, Kijimoto C, Yokoyama Y, Miyakawa T, Tsuchiya Y, Kuroda T, Nakano M, Saeki M (1998) Longitudinal follow-up of pulmonary function after lobectomy in childhood-factors affecting lung growth. Pediatr Surg Int 13(5–6):341–345
Komori K, Kamagata S, Hirobe S, Toma M, Okumura K, Muto M, Kasai S, Hayashi A, Suenaga M, Miyakawa T (2009) Radionuclide imaging study of long-term pulmonary function after lobectomy in children with congenital cystic lung disease. J Pediatr Surg 44(11):2096–2100
Keijzer R, Chiu PP, Ratjen F, Langer JC (2009) Pulmonary function after early vs late lobectomy during childhood: a preliminary study. J Pediatr Surg 44(5):893–895
Naito Y, Beres A, Lapidus-Krol E, Ratjen F, Langer JC (2012) Does earlier lobectomy result in better long-term pulmonary function in children with congenital lung anomalies? A prospective study. J Pediatr Surg 47(5):852–856
Calvert JK, Lakhoo K (2007) Antenatally suspected congenital cystic adenomatoid malformation of the lung: postnatal investigation and timing of surgery. J Pediatr Surg 42(2):411–414
Pelizzo G, Barbi E, Codrich D, Lembo MA, Zennaro F, Bussani R, Schleef J (2009) Chronic inflammation in congenital cystic adenomatoid malformations. An underestimated risk factor? J Pediatr Surg 44(3):616–619
Conforti A, Aloi I, Trucchi A, Morini F, Nahom A, Inserra A, Bagolan P (2009) Asymptomatic congenital cystic adenomatoid malformation of the lung: is it time to operate? J Thorac Cardiovasc Surg 138(4):826–830
Kim YT, Kim JS, Park JD, Kang CH, Sung SW, Kim JH (2005) Treatment of congenital cystic adenomatoid malformation-does resection in the early postnatal period increase surgical risk? Eur J Cardiothorac Surg 27(4):658–661
Marshall KW, Blane CE, Teitelbaum DH, van Leeuwen K (2000) Congenital cystic adenomatoid malformation: impact of prenatal diagnosis and changing strategies in the treatment of the asymptomatic patient. AJR 175(6):1551–1554
Tsai AY, Liechty KW, Hedrick HL, Bebbington M, Wilson RD, Johnson MP, Howell LJ, Flake AW, Adzick NS (2008) Outcomes after postnatal resection of prenatally diagnosed asymptomatic cystic lung lesions. J Pediatr Surg 43(3):513–517
Rothenberg SS, Kuenzler KA, Middlesworth W, Kay S, Yoder S, Shipman K, Rodriguez R, Stolar CJ (2011) Thoracoscopic lobectomy in infants less than 10 kg with prenatally diagnosed cystic lung disease. J Laparoendosc Adv Surg Tech Part A 21(2):181–184
Albanese CT, Sydorak RM, Tsao K, Lee H (2003) Thoracoscopic lobectomy for prenatally diagnosed lung lesions. J Pediatr Surg 38(4):553–555
Kaneko K, Ono Y, Tainaka T, Sumida W, Kawai Y, Ando H (2010) Thoracoscopic lobectomy for congenital cystic lung diseases in neonates and small infants. Pediatr Surg Int 26(4):361–365
Garrett-Cox R, MacKinlay G, Munro F, Aslam A (2008) Early experience of pediatric thoracoscopic lobectomy in the UK. J Laparoendosc Adv Surg Tech A 18(3):457–459. doi:10.1089/lap.2007.0038
Crombleholme TM, Coleman B, Hedrick H, Liechty K, Howell L, Flake AW, Johnson M, Adzick NS (2002) Cystic adenomatoid malformation volume ratio predicts outcome in prenatally diagnosed cystic adenomatoid malformation of the lung. J Pediatr Surg 37(3):331–338
Yong PJ, Von Dadelszen P, Carpara D, Lim K, Kent N, Tessier F, Delisle MF, Wong T, Blair G, Skarsgard ED (2012) Prediction of pediatric outcome after prenatal diagnosis and expectant antenatal management of congenital cystic adenomatoid malformation. Fetal Diagn Ther 31(2):94–102
Cass DL, Olutoye OO, Cassady CI, Moise KJ, Johnson A, Papanna R, Lazar DA, Ayres NA, Belleza-Bascon B (2011) Prenatal diagnosis and outcome of fetal lung masses. J Pediatr Surg 46(2):292–298
Alamo L, Reinberg O, Vial Y, Gudinchet F, Meuli R (2013) Comparison of foetal US and MRI in the characterisation of congenital lung anomalies. Eur J Radiol 82(12):e860–866
Beydon N, Larroquet M, Coulomb A, Jouannic JM, Ducou le Pointe H, Clement A, Garel C (2013) Comparison between US and MRI in the prenatal assessment of lung malformations. Pediatr Radiol 43(6):685–696
Hubbard AM, Crombleholme TM, Adzick NS, Coleman BG, Howell LJ, Meyer JS, Flake AW (1999) Prenatal MRI evaluation of congenital diaphragmatic hernia. Am J Perinatol 16(8):407–413
Matsuoka S, Takeuchi K, Yamanaka Y, Kaji Y, Sugimura K, Maruo T (2003) Comparison of magnetic resonance imaging and ultrasonography in the prenatal diagnosis of congenital thoracic abnormalities. Fetal Diagn Ther 18(6):447–453
Liu YP, Chen CP, Shih SL, Chen YF, Yang FS, Chen SC (2010) Fetal cystic lung lesions: evaluation with magnetic resonance imaging. Pediatr Pulmonol 45(6):592–600
Winters WD, Effmann EL (2001) Congenital masses of the lung: prenatal and postnatal imaging evaluation. J Thorac Imaging 16(4):196–206
Epelman M, Kreiger PA, Servaes S, Victoria T, Hellinger JC (2010) Current imaging of prenatally diagnosed congenital lung lesions. Semin Ultrasound CT MR 31(2):141–157
Loh KC, Jelin E, Hirose S, Feldstein V, Goldstein R, Lee H (2012) Microcystic congenital pulmonary airway malformation with hydrops fetalis: steroids vs open fetal resection. J Pediatr Surg 47(1):36–39
Curran PF, Jelin EB, Rand L, Hirose S, Feldstein VA, Goldstein RB, Lee H (2010) Prenatal steroids for microcystic congenital cystic adenomatoid malformations. J Pediatr Surg 45(1):145–150
Peranteau WH, Wilson RD, Liechty KW, Johnson MP, Bebbington MW, Hedrick HL, Flake AW, Adzick NS (2007) Effect of maternal betamethasone administration on prenatal congenital cystic adenomatoid malformation growth and fetal survival. Fetal Diagn Ther 22(5):365–371
Morris LM, Lim FY, Livingston JC, Polzin WJ, Crombleholme TM (2009) High-risk fetal congenital pulmonary airway malformations have a variable response to steroids. J Pediatr Surg 44(1):60–65
Knox EM, Kilby MD, Martin WL, Khan KS (2006) In-utero pulmonary drainage in the management of primary hydrothorax and congenital cystic lung lesion: a systematic review. Ultrasound Obstet Gynecol 28(5):726–734
Harrison MR, Adzick NS, Jennings RW, Duncan BW, Rosen MA, Filly RA, Goldberg JD, deLorimier AA, Golbus MS (1990) Antenatal intervention for congenital cystic adenomatoid malformation. Lancet 336(8721):965–967
Adzick NS, Harrison MR, Crombleholme TM, Flake AW, Howell LJ (1998) Fetal lung lesions: management and outcome. Am J Obstet Gynecol 179(4):884–889
Hedrick HL, Flake AW, Crombleholme TM, Howell LJ, Johnson MP, Wilson RD, Adzick NS (2005) The ex utero intrapartum therapy procedure for high-risk fetal lung lesions. J Pediatr Surg 40(6):1038–1043 (discussion 1044)
Cass DL, Olutoye OO, Cassady CI, Zamora IJ, Ivey RT, Ayres NA, Olutoye OA, Lee TC (2013) EXIT-to-resection for fetuses with large lung masses and persistent mediastinal compression near birth. J Pediatr Surg 48(1):138–144
Acknowledgement
The authors would like to thank Michel Atlas, Reference and Acquisitions Librarian, Kornhauser Health Sciences Library, University of Louisville, for her assistance with the literature search and citation management. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Downard, C.D., Calkins, C.M., Williams, R.F. et al. Treatment of congenital pulmonary airway malformations: a systematic review from the APSA outcomes and evidence based practice committee. Pediatr Surg Int 33, 939–953 (2017). https://doi.org/10.1007/s00383-017-4098-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-017-4098-z