Abstract
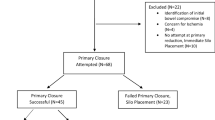
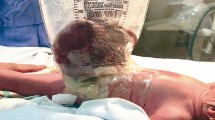
Non-operative management of gastroschisis also known as plastic closure (PC) has been described as an alternative to conventional primary operative closure (POC) or staged silo closure (SSC). The aim of this study was to compare these techniques in neonates with gastroschisis. A retrospective review of neonates with gastroschisis who underwent PC was undertaken. The minimum follow-up was 1 year. Premature neonates (<35 weeks) and those with intestinal atresia or multiple congenital anomalies were excluded. Frequency matching of PC cases with two control groups with either POC or SSC was performed on 1:1 ratio, based on gestational age and birth weight. Statistical analysis using univariate analysis was performed. Three groups were assembled: PC, POC and SSC (n = 33). Median follow-up was 1,198 days. Groups were comparable with regard to: time to first feed, time to full enteral feeding, frequency of vascular access related infections, ventilation time, NICU LOS (length of stay) and hospital LOS. There was no difference observed in surgical complications. Almost all neonates in the PC group developed an umbilical hernia (83.8%). Umbilical hernias were highly associated with PC compared to the other two groups P = 0.001. To date only one patient has had to have an operative repair of the umbilical hernia in the PC group. Plastic closure is safe and comparable to conventional closure techniques. However, PC is associated with the development of more umbilical hernias. The natural history of these hernias remains to be defined.
Similar content being viewed by others
References
Sandler A, Lawrence J, Meehan J et al (2004) A “plastic” sutureless abdominal wall closure in gastroschisis. J Pediatr Surg 39:738–741
Brown AL 2nd, Roty AR Jr, Kilway JB (1978) Increased survival with new techniques in treatment of gastroschisis. Am Surg 44:417–420
Schwartz MZ, Tyson KR, Milliorn K et al (1983) Staged reduction using a silastic sac is the treatment of choice for large congenital abdominal wall defects. J Pediatr Surg 18:713–719
Kidd JN Jr, Jackson RJ, Smith SD et al (2003) Evolution of staged versus primary closure of gastroschisis. Ann Surg 237:759–764
Shermeta DW, Haller JA Jr (1975) A new preformed transparent silo for the management of gastroschisis. J Pediatr Surg 10:973–975
Schlatter M (2003) Preformed silos in the management of gastroschisis: new progress with an old idea. Curr Opin Pediatr 15:239–242
Schlatter M, Norris K, Uitvlugt N et al (2003) Improved outcomes in the treatment of gastroschisis using a preformed silo and delayed repair approach. J Pediatr Surg 38:459–464
Owen A, Marven S, Jackson L et al (2006) Experience of bedside preformed silo staged reduction and closure for gastroschisis. J Pediatr Surg 41:1830–1835
Davies MW, Kimble RM, Cartwright DW (2005) Gastroschisis: ward reduction compared with traditional reduction under general anesthesia. J Pediatr Surg 40:523–527
Chiu B, Lopoo J, Hoover JD et al (2006) Closing arguments for gastroschisis: management with silo reduction. J Perinat Med 34:243–245
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bonnard, A., Zamakhshary, M., de Silva, N. et al. Non-operative management of gastroschisis: a case-matched study. Pediatr Surg Int 24, 767–771 (2008). https://doi.org/10.1007/s00383-008-2153-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-008-2153-5