Abstract
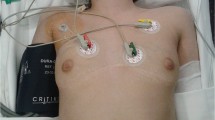
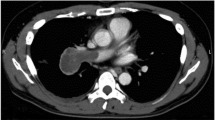
Median sternotomy (M-S) provides excellent exposure and allows dissection of the medial side of an anterior mediastinal tumor (AMT) with minimal risk. We report our experience of resecting AMT using M-S. Five children with AMT were treated using M-S between 1997 and 2004 at our institute. Ages at M-S ranged from 8 months (case 2) to 9 years (case 1) and AMT ranged in size from 5×6×7 cm3 (case 2) to large enough to occupy nearly the entire right thoracic cavity (cases 4 and 5). AMT were resected completely in all cases through M-S with the patient in the supine position. M-S alone was used in cases 1, 2, and 3, and cases 4 and 5 required additional incisions. There were dense adhesions between AMT and important mediastinal structures such as the anterior part of the pericardium (cases 1 and 2), left phrenic nerve (case 3), and pulmonary vessels (case 4, 5), but all were dissected safely under direct vision. There was no respiratory or cardiovascular compromise during M-S due to compression of the healthy lung and mediastinum. Histopathologic findings were mature teratoma in cases 1, 3, and 5, immature teratoma in case 2, and pleuropulmonary blastoma in case 4. Postoperative recovery was unremarkable. After mean follow-up of 3.4 years, cases 1, 2, 3, and 5 are currently well with no signs of recurrence, but case 4 died from disseminated intravascular coagulation during postoperative chemotherapy for massive local tumor recurrence 6 months after surgery. Based on our experience, M-S allows access to all aspects of AMT under direct vision, and provides excellent exposure, thus facilitating complete resection.


Similar content being viewed by others
References
Ito T, Nagaya M (1983) New operative approach for large mediastinal teratoma in children—complete median sternotomy with lateral incision. Z Kinderchir 38:425–428
Lakhoo K, Boyle M, Drake DP (1993) Mediastinal teratomas: review of 15 pediatric cases. J Pediatr Surg 28:1161–1164
Larson EL, Pearson ML (1999) CDC: guideline for the prevention of surgical site infection. Infect cont Hosp Epidemiol 20:247–278
Gross RE (1953) The surgery of infancy and childhood. WB Saunders, Phiadelphia London, pp 775–779
Rickham PP, Kloti J (1980) Mediastinal teratomas in neonates and very infants. Z Kinderchir 29:1–8
Wychulis AR, Payne WS, Clagett OT, Woolner LB (1971) Surgical treatment of mediastinal tumors: a 40 year experience J Thorac Cardiovasc Surg 62:379–392
Seibert JJ, Marvin WT, Rose EF, Schieken RW (1976) Mediastinal teratoma: a rare cause of severe respiratory distress in the newborn. J Pediatr Surg 11:253–255
Chetcuti P, Myers NA, Phelan PD, Beasley SW, Dicker DR (1989) Chest wall deformity in patients with repaired esophageal atresia. J Pediatr Surg 24:244–247
Cherup LL, Siewers RD, Futrell JW (1986) Breast and pectoral muscle maldevelopment after anterolateral and posterolateral thoracotomies in children. Ann Thorac Surg 41:492–497
De Oliveria-Filho AG, Neto LS, Epelman S (1998) Median sternotomy for the resection of bilateral pulmonary metastases in children. Pediatr Surg Int 13:560–563
Partrick DA, Rothenberg SS (2001) Thoracoscopic resection of mediastinal mass in infants and children an evaluation of technique and results. J Pediatr Surg 36:1165–1167
Silomom M, Claus T, Huweer H, Biedler A, Larsen R, Molter G (2000) Interpleural analgesia dose not influence postthoracotomy pain. Anesth Analg 91:44–50
Edwards MS, Baker CJ (1983) Median sternotomy wound infections in children. Pediatr Infect Dis 2:105–109
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Koga, H., Yamataka, A., Kobayashi, H. et al. Median sternotomy provides excellent exposure for excising anterior mediastinal tumors in children. Ped Surgery Int 21, 864–867 (2005). https://doi.org/10.1007/s00383-005-1504-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-005-1504-8