Abstract
Introduction
Intraventricular haemorrhage (IVH) is a common complication of preterm birth, and optimal treatment remains uncertain. Neuroendoscopic lavage (NEL) has gained interest as a method for removal of intraventricular haematoma, with outcomes suggesting it to be safe and potentially effective.
Methods
A retrospective review was carried identifying infants who underwent NEL for post-IVH hydrocephalus at our institution. Data was extracted on patient baseline demographics, comorbidities, complications, re-operation requirement, and neurodevelopmental outcomes.
Results
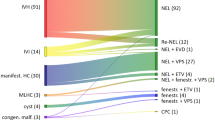
Twenty-six patients (17 male) were identified, who underwent NEL at a mean age of 39 weeks and 4 days. Eighteen patients underwent simultaneous endoscopic third ventriculostomy (ETV). Mean patient follow-up was 57.7 months ± 11.8 months. A total of 17/26 patients went on to require a ventriculoperitoneal shunt (VPS). Nine patients did not require further surgical management of hydrocephalus; all had been managed with NEL + ETV. The relative risk of requiring VPS with NEL + ETV compared with NEL alone was 0.500 (CI: 0.315–0.794; p = 0.0033). The 24-month survival rate of VPS inserted following NEL was 64.7%. Exactly 5/26 (19.2%) had post-procedure complications: 2 CSF leaks (7.7%), 2 infections (7.7%), and 1 rebleed within 72 h of NEL (3.8%). On long-term follow-up, 22/25 patients achieved good motor outcome, either walking independently or with mobility aids. A total of 8/15 children attended mainstream schooling with adaption.
Discussion
NEL is safe and potentially efficacious treatment for neonatal IVH. The procedure may reduce shunt dependence and, for those who require CSF diversion, improve shunt survival. Neurodevelopmentally, good motor and cognitive outcome can be achieved.


Similar content being viewed by others
References
Badhiwala JH, Hong CJ, Nassiri F, Hong BY, Riva-Cambrin J, Kulkarni AV (2015) Treatment of posthemorrhagic ventricular dilation in preterm infants: a systematic review and meta-analysis of outcomes and complications. J Neurosurg Pediatr 28:1–11
Mukerji A, Shah V, Shah PS (2015) Periventricular/intraventricular hemorrhage and neurodevelopmental outcomes: a meta-analysis. Pediatrics 136(6):1132–1143
Christian EA, Melamed EF, Peck E et al (2016) Surgical management of hydrocephalus secondary to intraventricular hemorrhage in the preterm infant. J Neurosurg Pediatr 17(3):278–284
Robinson S (2012) Neonatal posthemorrhagic hydrocephalus from prematurity: pathophysiology and current treatment concepts. J Neurosurg Pediatr 9(3):242–258
Brydon HL, Bayston R, Hayward R et al (1996) The effect of protein and blood cells on the flow-pressure characteristics of shunts. Neurosurgery 38:498–504
Kamat AS, Gretschel A, Vlok AJ, Solomons R (2018) CSF protein concentration associated with ventriculoperitoneal shunt obstruction in tuberculous meningitis. Int J Tuberc Lung Dis 22(7):788–792
Kaestner S, Sani R, Graf K et al (2021) CSF shunt valve occlusion—does CSF protein and cell count matter? Acta Neurochir 163:1991–1996
Ellenbogen JR, Waqar M, Pettorini B (2016) Management of post-haemorrhagic hydrocephalus in premature infants. J Clin Neurosci 31:30–34
Whitelaw A, Evans D, Carter M, Thoresen M, Wroblewska J, Mandera M et al (2007) Randomized clinical trial of prevention of hydrocephalus after intraventricular hemorrhage in preterm infants: brain-washing versus tapping fluid. Pediatrics 119:e1071-1078
Whitelaw A, Jary S, Kmita G, Wroblewska J, Musialik-Swietlinska E, Mandera M et al (2010) Randomized trial of drainage, irrigation and fibrinolytic therapy for premature infants with posthemorrhagic ventricular dilatation: developmental outcome at 2 years. Pediatrics 125:e852-858
Luyt K, Jary SL, Lea CL et al (2020) Drainage, irrigation and fibrinolytic therapy (DRIFT) for posthaemorrhagic ventricular dilatation: 10-year follow-up of a randomised controlled trial. Archives of Disease in Childhood - Fetal and Neonatal Edition 105:466–473
Schulz M, Buhrer C, Pohl-Schickinger A, Haberl H, Thomale UW (2014) Neuroendoscopic lavage for the treatment of intraventricular hemorrhage and hydrocephalus in neonates. J Neurosurg Pediatr 13:626–635
d’Arcangues C, Schulz M, Bührer C, Thome U, Krause M, Thomale UW (2018) Extended experience with neuroendoscopic lavage for posthemorrhagic hydrocephalus in neonates. World Neurosurg 116:e217–e224
Tirado-Caballero J, Rivero-Garvia M, Arteaga-Romero F, Herreria-Franco J, Lozano-Gonzalez Á, Marquez-Rivas J (2020) Neuroendoscopic lavage for the management of posthemorrhagic hydrocephalus in preterm infants: safety, effectivity, and lessons learned. J Neurosurg Pediatr 15:1–10
Riva-Cambrin J, Kestle JRW, Holubkov R, Butler J, Kulkarni AV, Drake J et al (2016) Risk factors for shunt malfunction in pediatric hydrocephalus: a multicenter prospective cohort study. J Neurosurg Pediatr 17(4):382–390
Papile LA, Burstein J, Burstein R, Koffler H (1978) Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 92:529–534
Ballabh P (2010) Intraventricular Hemorrhage in Premature Infants: Mechanism of Disease. Pediatr Res 67(1):1–8
Mazzola CA, Choudhri AF, Auguste KI, Limbrick DD Jr, Rogido M, Mitchell L, et al (2014) Pe- diatric hydrocephalus: systematic literature review and evidence-based guidelines. Part 2: Management of posthemorrhagic hydrocephalus in premature infants. J Neurosurg Pediatr 14(suppl 1):8–23
Kuo MF (2020) Surgical management of intraventricular hemorrhage and posthemorrhagic hydrocephalus in premature infants. Biomed J 43:268e76
García-Méndez A, Álvarez-Vázquez L, Agustín-Aguilar F et al (2014) Ventriculo subgaleal shunt in hydrocephalus secondary to intraventricular hemorrhage in prematures. Gac Med Mex 150(suppl 3):279–281
Wang JY, Amin AG, Jallo GI, Ahn ES (2014) Ventricular reservoir versus ventriculosubgaleal shunt for posthemorrhagic hydrocephalus in preterm infants: infection risks and ventriculo- peritoneal shunt rate. J Neurosurg Pediatr 14(5):447–454
Luyt K, Jary S, Lea C et al (2019) Ten-year follow-up of a randomised trial of drainage, irrigation and fibrinolytic therapy (DRIFT) in infants with post-haemorrhagic ventricular dila- tation. Health Technol Assess 23(4):1–116
Wellons JC, Shannon CN, Kulkarni AV, Simon TD, Riva-Cambrin J, Whitehead WE et al (2009) A multicenter retrospective comparison of conversion from temporary to permanent cerebrospinal fluid diversion in very low birth weight infants with posthemorrhagic hydrocephalus. J Neurosurg Pediatr 4:50–55
Wellons JC 3rd, Shannon CN, Holubkov R, Riva-Cambrin J, Kulkarni AV, Limbrick DD Jr et al (2017) Hydrocephalus Clinical Research Network. Shunting outcomes in post- hemorrhagic hydrocephalus: results of a Hydrocephalus Clinical Research Network prospective cohort study. J Neurosurg Pediatr 20:19–29
Bu Y, Chen M, Gao T et al (2016) Mechanisms of hydrocephalus after intraventricular haemorrhage in adults. Stroke Vasc Neurol 1
Krishnamurthy S, Li J, Schultz L et al (2009) Intraventricular infusion of hyperosmolar dextran induces hydrocephalus: a novel animal model of hydrocephalus. Cerebrospinal Fluid Res 6:16
Strahle J, Garton HJ, Maher CO et al (2012) Mechanisms of hydrocephalus after neonatal and adult intraventricular hemorrhage. Transl Stroke Res 3(Suppl 1):25–38
Simon TD, Whitlock KB, Riva-Cambrin J, Kestle JR, Rosenfeld M, Dean JM et al (2012) Association of intraventricular hemorrhage secondary to prematurity with cerebrospinal fluid shunt surgery in the first year following initial shunt placement. J Neurosurg Pediatr 9:54–63
Behrens P, Tietze A, Walch E, Bittigau P, Bührer C, Schulz M et al (2020) Neurodevelopmental outcome at 2 years after neuroendoscopic lavage in neonates with posthemorrhagic hydrocephalus. J Neurosurg Pediatr 26(5):495–503
Thomale UW, Cinalli G, Kulkarni AV et al (2019) TROPHY registry study design: a prospective, international multicenter study for the surgical treatment of posthemorrhagic hydrocephalus in neonates. Childs Nerv Syst 35(4):613–619
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
No conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Honeyman, S.I., Boukas, A., Jayamohan, J. et al. Neuroendoscopic lavage for the management of neonatal post-haemorrhagic hydrocephalus: a retrospective series. Childs Nerv Syst 38, 115–121 (2022). https://doi.org/10.1007/s00381-021-05373-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-021-05373-8