Abstract
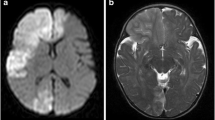
Moyamoya disease is a chronic cerebral vascular disease characterized by progressive occlusion of the cerebral arteries and resulting in the development of abnormal collateral circulation. We report a case of moyamoya disease in a 3-year-old Chinese girl with partly reversible white matter lesions. This case indicates that, in pediatric moyamoya disease, white matter lesions may be associated with cerebral ischemia, and they may be reversible after treatment.




Similar content being viewed by others
Abbreviations
- MMD:
-
Moyamoya disease
- MRA:
-
magnetic resonance angiography
- DSA:
-
digital substraction angiography
- DWI:
-
diffusion-weighted imaging
- MRI:
-
magnetic resonance imaging
- FLAIR:
-
fluid attenuated inversion recovery
- SWI:
-
susceptibility-weighted imaging
- MRS:
-
magnetic resonance spectroscopy
- CBF:
-
cerebral blood flow
References
Takeuchi K, Shimizu K (1957) Hypoplasia of the bilateral internal carotid arteries. Brain Nerve 9:37–43
Piao J, Wu W, Yang Z (2015) Research progress of moyamoya disease in children. Int J Med Sci 12:566–575
Fujimura M, Tominaga T (2015) Diagnosis of moyamoya disease: international standard and regional differences. Neurol Med Chir (Tokyo) 55:189–193
Liao X, Deng J, Dai W, Zhang T, Yan J (2017) Rare variants of RNF213 and moyamoya/non-moyamoya intracranial artery stenosis/occlusion disease risk: a meta-analysis and systematic review. Environ Health Prev Med 22:75
Morimoto T, Enmi JI, Hattori Y, Iguchi S, Saito S, Harada KH, Okuda H, Mineharu Y, Takagi Y, Youssefian S, Iida H, Miyamoto S, Ihara M, Kobayashi H, Koizumi A (2018) Dysregulation of RNF213 promotes cerebral hypoperfusion. Sci Rep 8:3607
Kim WH, Kim SD, Nam MH, Jung JM, Jin SW, Ha SK, Lim DJ, Lee HB (2019) Posterior circulation involvement and collateral flow pattern in moyamoya disease with the RNF213 polymorphism. Childs Nerv Syst 35:309–314
Matsuda Y, Mineharu Y, Kimura M, Takagi Y, Kobayashi H, Hitomi T, Harada KH, Uchihashi Y, Funaki T, Miyamoto S, Koizumi A (2017) RNF213 p.R4810K variant and intracranial arterial stenosis or occlusion in relatives of patients with moyamoya disease. J Stroke Cerebrovasc Dis 26:1841–1847
Zhang Q, Liu Y, Zhang D, Wang R, Zhang Y, Wang S, Yu L, Lu C, Liu F, Zhou J, Zhang X, Zhao J (2017) RNF213 as the major susceptibility gene for Chinese patients with moyamoya disease and its clinical relevance. J Neurosurg 126:1106–1113
Kim EH, Yum MS, Ra YS, Park JB, Ahn JS, Kim GH, Goo HW, Ko TS, Yoo HW (2016) Importance of RNF213 polymorphism on clinical features and long-term outcome in moyamoya disease. J Neurosurg 124:1221–1227
Liu W, Morito D, Takashima S, Mineharu Y, Kobayashi H, Hitomi T, Hashikata H, Matsuura N, Yamazaki S, Toyoda A, Kikuta K, Takagi Y, Harada KH, Fujiyama A, Herzig R, Krischek B, Zou L, Kim JE, Kitakaze M, Miyamoto S, Nagata K, Hashimoto N, Koizumi A (2011) Identifcation of RNF213 as a susceptibility gene for moyamoya disease and its possible role in vascular development. PLoS One 6:e22542
Ernst M, Boers AMM, Forkert ND, Berkhemer OA, Roos YB, Dippel DWJ, Van der Lugt A, Van Oostenbrugge RJ, Van Zwam WH, Vettorazzi E, Fiehler J, Marquering HA, Majoie CBLM, Gellissen S (2018) Impact of ischemic lesion location on the mRS score in patients with ischemic stroke: a voxel-based approach. AJNR Am J Neuroradiol 39:1989–1994
Von Rennenberg R, Siegerink B, Ganeshan R, Villringer K, Doehner W, Audebert HJ, Endres M, Nolte CH, Scheitz JF (2019) High-sensitivity cardiac troponin T and severity of cerebral white matter lesions in patients with acute ischemic stroke. J Neurol 266:37–45
Haussen DC, Lima A, Frankel M, Anderson A, Belagaje S, Nahab F, Rangaraju S, Nogueira RG (2015) Sulcal effacement with preserved gray-white junction: a sign of reversible ischemia. Stroke 46:1704–1706
Holmegaard L, Jensen C, Redfors P, Blomstrand C, Jern C, Jood K (2018) Long-term progression of white matter hyperintensities in ischemic stroke. Acta Neurol Scand 138:548–556
Tamura G, Ihara S, Morota N (2016) Reversible diffusion weighted imaging hyperintensities during the acute phase of ischemic stroke in pediatric moyamoya disease: a case report. Childs Nerv Syst 32:1531–1535
Hara S, Hori M, Inaji M, Maehara T, Aoki S, Nariai T (2018) Regression of white matter hyperintensity after indirect bypass surgery in a patient with moyamoya disease. Magnetic Resonance in Medical Sciences. https://doi.org/10.2463/mrms.ci.2018-0088
Kim TK, Eun BL, Cha SH, Chung KB, Kim JH, Kim BH, Chung HH (2003) Moyamoya disease in a child with previous acute necrotizing encephalopathy. Pediatr Radiol 33:644–647
Sasannejad P, Rezaei F, Bidaki R, Zarepur E (2018) Rare presentation of moyamoya disease with subacute presentation in Iran. Iran J Child Neurol 12:89–93
Li Y, Gor D, Walicki D, Jenny D, Jones D, Barbour P, Castaldo J (2012) Spectrum and potential pathogenesis of reversible posterior leukoencephalopathy syndrome. J Stroke Cerebrovasc Dis 21:873–882
Tashiro R, Fujimura M, Mugikura S, Niizuma K, Endo H, Endo T, Tominaga T (2018) Paradoxical association of symptomatic local vasogenic edema with global cerebral hypoperfusion after direct revascularization surgery for adult moyamoya disease. J Stroke Cerebrovasc Dis 27:e172–e176
Komori A, Mizu D, Ariyoshi K (2018) Posterior reversible encephalopathy syndrome: a rare childhood case with unconsciousness. J Emerg Med 54:540–543
Chen HA, Lin YJ, Chen PC, Chen TY, Lin KC, Cheng HH (2010) Systemic lupus erythematosus complicated with posterior reversible encephalopathy syndrome and intracranial vasculopathy. Int J Rheum Dis 13:e79–e82
Guggenberger K, Urbach H (2018) MRI alterations in immunomodulation. Nervenarzt 89:945–957
Hamano E, Kataoka H, Morita N, Maruyama D, Satow T, Iihara K, Takahashi JC (2017) Clinical implication of the cortical hyper intensity belt sign in fluid-attenuated inversion recovery images after bypass surgery for moyamoya disease. J MNeurosurg 126:1–7
Takanashi J (2011) Moyamoya disease in children. Brain and Development 33:229–234
Bedini G, Blecharz KG, Nava S, Vajkoczy P, Alessandri G, Ranieri M, Acerbi F, Ferroli P, Riva D, Esposito S, Pantaleoni C, Nardocci N, Zibordi F, Ciceri E, Parati EA, Bersano A (2016) Vasculogenic and angiogenic pathways in moyamoya disease. Curr Med Chem 23:315–345
Research committee on the pathology and treatment of spontaneous occlusion of the circle of Willis (2012) Guidelines for diagnosis and treatment of moyamoya disease (spontaneous occlusion of the circle of Willis). Neuro Med Chir (Tokyo) 52:245–266
Smith ER, Scott M (2012) Spontaneous occlusion of the circle of Willis in children:pediatric moyamoya summary with proposed evidence-based practice guidelines. J Neurosurg Pediatrics 9:353–360
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Th authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, SJ., Xiong, J., He, Y. et al. A rare case of pediatric moyamoya disease with reversible white matter lesions in a 3-year-old Chinese girl. Childs Nerv Syst 36, 197–201 (2020). https://doi.org/10.1007/s00381-019-04391-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04391-x