Abstract
Objective
Patients with non-communicating hydrocephalus due to aqueductal stenosis are often successfully treated with endoscopic third ventriculocisternostomy (ETV). In hydrocephalus, due to other locations of obstruction of the major CSF pathways, endoscopic treatment may also be a good option. We investigated our cohort of patients treated by ETV with patent ventricular outflow but pressure gradient signs at the third ventricle in a single-center retrospective study.
Methods
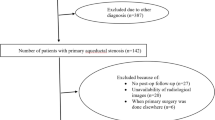
We retrospectively reviewed records and imaging studies of 137 patients who underwent an ETV in our department in the time period of June 2010 to March 2018. We included patients who showed the following findings in MRI: 1st: open Sylvian aqueduct, 2nd: open outlets of the 4th ventricle, 3rd: open spinal canal, 4th: intra-/extraventricular pressure gradient seen at the 3rd ventricle and excluded patients with history of CSF infection or hemorrhage. Perioperative clinical state and possible complications or reoperations were recorded. Shunt dependency and changes in ventricular dilatation were measured as frontal and occipital horn ratio (FOHR) before surgery and during follow-up.
Results
A total of 21 patients met the defined criteria. During the mean follow-up time of 40.7 ± 30 months (range; 5–102 months), two children had to undergo a re-ETV, and six children (all < 1 year of age) received a VP shunt. ETV shunt-free survival was 100% for children > 1 year of age. The ventricular width measured as FOHR was significantly reduced after ETV 0.5 ± 0.08 (range 0.42–0.69; p < 0.05). FOHR was significantly reduced at last follow-up shunt independent patients (0.47 ± 0.05; range 0.41–0.55; p < 0.001)
Conclusion
We conclude that ETV seems to be a successful treatment option for patients with MRI signs of intra-/extraventricular pressure gradient at the 3rd ventricle and patent aqueduct and fourth ventricular outlets in children older than 1 year of age. This condition is observed only rarely and warrants further research on a multicenter basis in order to get more solid data of its pathophysiology.




Similar content being viewed by others
References
Baird LC, Mazzola CA, Auguste KI, Klimo P Jr, Flannery AM (2014) Pediatric hydrocephalus: systematic literature review and evidence-based guidelines. Part 5: Effect of valve type on cerebrospinal fluid shunt efficacy. Journal of neurosurgery Pediatrics 14(Suppl 1):35–43
Limbrick DD Jr, Baird LC, Klimo P Jr, Riva-Cambrin J, Flannery AM (2014) Pediatric hydrocephalus: systematic literature review and evidence-based guidelines. Part 4: cerebrospinal fluid shunt or endoscopic third ventriculostomy for the treatment of hydrocephalus in children. Journal of neurosurgery Pediatrics 14(Suppl 1):30–34
Flannery AM, Mazzola CA, Klimo P Jr, Duhaime AC, Baird LC, Tamber MS et al (2014) Foreword: pediatric hydrocephalus: systematic literature review and evidence-based guidelines. J Neurosurg Pediatr 14(Suppl 1):1–2
Kulkarni AV, Sgouros S, Constantini S (2016) International Infant Hydrocephalus Study: initial results of a prospective, multicenter comparison of endoscopic third ventriculostomy (ETV) and shunt for infant hydrocephalus. Childs Nerv Syst: ChNS: Off J Int Soc Pediatr Neurosurg 32(6):1039–1048
Kulkarni AV, Riva-Cambrin J, Holubkov R, Browd SR, Cochrane DD, Drake JM, Limbrick DD, Rozzelle CJ, Simon TD, Tamber MS, Wellons JC 3rd, Whitehead WE, Kestle JR, Hydrocephalus Clinical Research Network (2016) Endoscopic third ventriculostomy in children: prospective, multicenter results from the Hydrocephalus Clinical Research Network. J Neurosurg Pediatr 18(4):423–429
Benzel EC, Reeves JP, Nguyen PK, Hadden TA (1993) The treatment of hydrocephalus in preterm infants with intraventricular haemorrhage. Acta Neurochir 122(3-4):200–203
Wakhlu A, Ansari NA (2004) The prediction of postoperative hydrocephalus in patients with spina bifida. Childs Nerv Syst 20(2):104–106
Di Rocco C, Massimi L, Tamburrini G (2006) Shunts vs endoscopic third ventriculostomy in infants: are there different types and/or rates of complications?A review. Childs Nerv Syst 22(12):1573–1589
Iantosca MR, Hader WJ, Drake JM (2004) Results of endoscopic third ventriculostomy. Neurosurg Clin N Am 15(1):67–75
Kulkarni AV, Sgouros S, Constantini S, Investigators I (2016) International Infant Hydrocephalus Study: initial results of a prospective, multicenter comparison of endoscopic third ventriculostomy (ETV) and shunt for infant hydrocephalus. Childs Nerv Syst 32(6):1039–1048
Drake JM, Kestle JR, Milner R, Cinalli G, Boop F, Piatt J Jr et al (1998) Randomized trial of cerebrospinal fluid shunt valve design in pediatric hydrocephalus. Neurosurgery 43(2):294–303 discussion -5
Gebert AF, Schulz M, Schwarz K, Thomale UW (2016) Long-term survival rates of gravity-assisted, adjustable differential pressure valves in infants with hydrocephalus. J Neurosurg Pediatr 17(5):544–551
Albright AL, Haines SJ, Taylor FH (1988) Function of parietal and frontal shunts in childhood hydrocephalus. J Neurosurg 69(6):883–886
Haberl EJ, Messing-Juenger M, Schuhmann M, Eymann R, Cedzich C, Fritsch MJ, Kiefer M, van Lindert E, Geyer C, Lehner M, Rohde V, Stroux A, von Berenberg P (2009) Experiences with a gravity-assisted valve in hydrocephalic children. Clinical article. J Neurosurg Pediatr 4(3):289–294
McGirt MJ, Leveque JC, Wellons JC 3rd, Villavicencio AT, Hopkins JS, Fuchs HE et al (2002) Cerebrospinal fluid shunt survival and etiology of failures: a seven-year institutional experience. Pediatr Neurosurg 36(5):248–255
Riva-Cambrin J, Kestle JR, Holubkov R, Butler J, Kulkarni AV, Drake J, Whitehead WE, Wellons JC 3rd, Shannon CN, Tamber MS, Limbrick DD Jr, Rozzelle C, Browd SR, Simon TD, Hydrocephalus Clinical Research Network (2016) Risk factors for shunt malfunction in pediatric hydrocephalus: a multicenter prospective cohort study. J Neurosurg Pediatr 17(4):382–390
Shah SS, Hall M, Slonim AD, Hornig GW, Berry JG, Sharma V (2008) A multicenter study of factors influencing cerebrospinal fluid shunt survival in infants and children. Neurosurgery. 62(5):1095–1102 discussion 102-3
Dupepe EB, Hopson B, Johnston JM, Rozzelle CJ, Jerry Oakes W, Blount JP et al (2016) Rate of shunt revision as a function of age in patients with shunted hydrocephalus due to myelomeningocele. Neurosurg Focus 41(5):E6
Kehler U, Gliemroth J (2003) Extraventricular intracisternal obstructive hydrocephalus--a hypothesis to explain successful 3rd ventriculostomy in communicating hydrocephalus. Pediatr Neurosurg 38(2):98–101
Kageyama H, Miyajima M, Ogino I, Nakajima M, Shimoji K, Fukai R, Miyake N, Nishiyama K, Matsumoto N, Arai H (2016) Panventriculomegaly with a wide foramen of Magendie and large cisterna magna. J Neurosurg 124(6):1858–1866
Schulte-Altedorneburg G, Linn J, Kunz M, Bruckmann H, Zausinger S, Morhard D (2016) Visualization of Liliequist’s membrane prior to endoscopic third ventriculostomy. La Radiologia medica 121(3):200–205
Dias DA (2014) Liliequist membrane: radiological evaluation. Clinical 47(3):182–185
Knaus H, Abbushi A, Hoffmann KT, Schwarz K, Haberl H, Thomale UW (2009) Measurements of burr-hole localization for endoscopic procedures in the third ventricle in children. Childs Nerv Syst 25(3):293–299
Thomale UW, Schaumann A, Stockhammer F, Giese H, Schuster D, Kastner S et al (2018) GAVCA Study: randomized, multicenter trial to evaluate the quality of ventricular catheter placement with a mobile health assisted guidance technique. Neurosurgery. 83(2):252–262
O'Hayon BB, Drake JM, Ossip MG, Tuli S, Clarke M (1998) Frontal and occipital horn ratio: a linear estimate of ventricular size for multiple imaging modalities in pediatric hydrocephalus. Pediatr Neurosurg 29(5):245–249
Vinchon M, Dhellemmes P (2006) Cerebrospinal fluid shunt infection: risk factors and long-term follow-up. Childs Nerv Syst 22(7):692–697
Thomale UW, Gebert AF, Haberl H, Schulz M (2013) Shunt survival rates by using the adjustable differential pressure valve combined with a gravitational unit (proGAV) in pediatric neurosurgery. Childs Nerv Syst 29(3):425–431
Kehler U, Regelsberger J, Gliemroth J, Westphal M (2006) Outcome prediction of third ventriculostomy: a proposed hydrocephalus grading system. Minimally invasive neurosurgery : MIN 49(4):238–243
Adeeb N, Deep A, Griessenauer CJ, Mortazavi MM, Watanabe K, Loukas M, Tubbs RS, Cohen-Gadol AA (2013) The intracranial arachnoid mater : a comprehensive review of its history, anatomy, imaging, and pathology. Childs Nerv Syst 29(1):17–33
Fushimi Y, Miki Y, Takahashi JA, Kikuta K, Hashimoto N, Hanakawa T et al (2006) MR imaging of Liliequist’s membrane. Radiat Med 24(2):85–90
Anik I, Ceylan S, Koc K, Tugasaygi M, Sirin G, Gazioglu N, Sam B (2011) Microsurgical and endoscopic anatomy of Liliequist’s membrane and the prepontine membranes: cadaveric study and clinical implications. Acta Neurochir 153(8):1701–1711
Mortazavi MM, Rizq F, Harmon O, Adeeb N, Gorjian M, Hose N, Modammadirad E, Taghavi P, Rocque BG, Tubbs RS (2015) Anatomical variations and neurosurgical significance of Liliequist’s membrane. Childs Nerv Syst 31(1):15–28
Brasil AV, Schneider FL (1993) Anatomy of Liliequist’s membrane. Neurosurgery. 32(6):956–960 discussion 60-1
Fox JL, Al-Mefty O (1980) Suprasellar arachnoid cysts: an extension of the membrane of Liliequist. Neurosurgery. 7(6):615–618
Andre A, Zerah M, Roujeau T, Brunelle F, Blauwblomme T, Puget S et al (2016) Suprasellar arachnoid cysts: toward a new simple classification based on prognosis and treatment modality. Neurosurgery. 78(3):370–379 discussion 9-80
Ozek MM, Urgun K (2013) Neuroendoscopic management of suprasellar arachnoid cysts. World Neurosurg 79(2 Suppl):S19 e3-8
Paraskevopoulos D, Roth J, Beni-Adani L, Constantini S (2011) Interpeduncular arachnoid cysts in infants and children: insight into the entity based on a case series with long-term follow-up. Childs Nerv Syst 27(3):429–438
Lyu J (2014) Possible origins of suprasellar arachnoid cysts based on anatomical considerations. World neurosurgery 82(3-4):e570–e573
Zhang M, An PC (2000) Liliequist’s membrane is a fold of the arachnoid mater: study using sheet plastination and scanning electron microscopy. Neurosurgery. 47(4):902–908 discussion 8-9
Gui SB, Wang XS, Zong XY, Zhang YZ, Li CZ (2011) Suprasellar cysts: clinical presentation, surgical indications, and optimal surgical treatment. BMC Neurol 11:52
Miyajima M, Arai H, Okuda O, Hishii M, Nakanishi H, Sato K (2000) Possible origin of suprasellar arachnoid cysts: neuroimaging and neurosurgical observations in nine cases. J Neurosurg 93(1):62–67
Froelich SC, Abdel Aziz KM, Cohen PD, van Loveren HR, Keller JT (2008) Microsurgical and endoscopic anatomy of Liliequist’s membrane: a complex and variable structure of the basal cisterns. Neurosurgery 63(1 Suppl 1):ONS1–ONS8 discussion ONS-9
Drake JM (2007) Endoscopic third ventriculostomy in pediatric patients: the Canadian experience. Neurosurgery 60(5):881–886 discussion -6
Kulkarni AV, Drake JM, Mallucci CL, Sgouros S, Roth J, Constantini S (2009) Endoscopic third ventriculostomy in the treatment of childhood hydrocephalus. The Journal of pediatrics 155(2):254–9.e1
Beems T, Grotenhuis JA (2002) Is the success rate of endoscopic third ventriculostomy age-dependent? An analysis of the results of endoscopic third ventriculostomy in young children. Childs Nerv Syst 18(11):605–608
Kulkarni AV, Drake JM, Kestle JR, Mallucci CL, Sgouros S, Constantini S, Canadian Pediatric Neurosurgery Study Group (2010) Predicting who will benefit from endoscopic third ventriculostomy compared with shunt insertion in childhood hydrocephalus using the ETV Success Score. J Neurosurg Pediatr 6(4):310–315
Kulkarni AV, Riva-Cambrin J, Rozzelle CJ, Naftel RP, Alvey JS, Reeder RW et al (2018) Endoscopic third ventriculostomy and choroid plexus cauterization in infant hydrocephalus: a prospective study by the Hydrocephalus Clinical Research Network. J Neurosurg Pediatr 21(3):214–223
Kulkarni AV, Schiff SJ, Mbabazi-Kabachelor E, Mugamba J, Ssenyonga P, Donnelly R, Levenbach J, Monga V, Peterson M, MacDonald M, Cherukuri V, Warf BC (2017) Endoscopic treatment versus shunting for infant hydrocephalus in Uganda. N Engl J Med 377(25):2456–2464
Conflict of interest
The authors have no conflict of interest to declare in relation to the presented content of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study received approval from the institutional ethics committee (EA2/132/17).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Al-Hakim, S., Schaumann, A., Tietze, A. et al. Endoscopic third ventriculostomy in children with third ventricular pressure gradient and open ventricular outlets on MRI. Childs Nerv Syst 35, 2319–2326 (2019). https://doi.org/10.1007/s00381-019-04383-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04383-x