Abstract
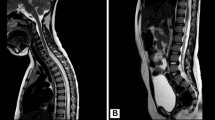
Diffuse leptomeningeal glioneuronal tumors (DLGNTs) are newly recognized as an entity in the 2016 revision of the WHO Classification of tumors of the central nervous system. They typically present as diffuse leptomeningeal infiltrates along the neuraxis with focal and superficial involvement of the parenchyma. Here, we report a DLGNT with unusual radiological and histological features. A 13-year-old girl presented with scoliosis and back pain. Magnetic resonance imaging demonstrated a syrinx from C2 to T11 and an intramedullary mass from T6 to T9–10. No leptomeningeal involvement was recognized. Histological examination of the gross total resection specimen revealed a low-grade neuroepithelial neoplasm predominantly infiltrating the spinal cord and only focally involving the leptomeninges. Chromosome microarray identified co-deletion of the short arm of chromosome 1 and the long arm of chromosome 19 as well as fusion of the KIAA1549 and BRAF genes. Next-generation sequencing demonstrated wild-type alleles at the mutational hotspots of IDH1 (R132) and IDH2 (R140 and R172). In contrast to most reported DLGNTs, the tumor described in this manuscript was characterized by a predominant parenchymal component and only minor leptomeningeal involvement both radiographically and histologically. Our case, therefore, expands the spectrum of radiological and histopathological features of this new entity. It also highlights the critical role of molecular genetic testing in establishing the diagnosis of DLGNT in unusual cases.



Similar content being viewed by others
References
Reifenberger G, Rodriguez F, Burger PC, Perry A, Capper D (2016) In: Louis DN, Ohgaki H, Wiestler OD, Cavenee WK (eds) Diffuse leptomeningeal glioneuronal tumour. World Health Organization histological classification of tumours of the central nervous system, 4th edn. International Agency for Research on Cancer, Lyon, pp 152–155
Rodriguez FJ, Perry A, Rosenblum MK, Krawitz S, Cohen KJ, Lin D, Mosier S, Lin MT, Eberhart CG, Burger PC (2012) Disseminated oligodendroglial-like leptomeningeal tumor of childhood: a distinctive clinicopathologic entity. Acta Neuropathol 124(5):627–641
Johnson DR, Guerin JB, Giannini C, Morris JM, Eckel LJ, Kaufmann TJ (2017) 2016 updates to the WHO brain tumor classification system: what the radiologist needs to know. Radiographics 37(7):2164–2180
Rodriguez FJ, Schniederjan MJ, Nicolaides T, Tihan T, Burger PC, Perry A (2015) High rate of concurrent BRAF-KIAA1549 gene fusion and 1p deletion in disseminated oligodendroglioma-like leptomeningeal neoplasms (DOLN). Acta Neuropathol 129(4):609–610
Kessler BA, Bookhout C, Jaikumar S, Hipps J, Lee YZ (2015) Disseminated oligodendroglial-like leptomeningeal tumor with anaplastic progression and presumed extraneural disease: case report. Clin Imaging 39(2):300–304
Schwetye KE, Kansagra AP, McEachern J, Schmidt RE, Gauvain K, Dahiya S (2017) Unusual high-grade features in pediatric diffuse leptomeningeal glioneuronal tumor: comparison with a typical low-grade example. Hum Pathol 70:105–112
Beck DJK, Russel DS (1942) Oligodendrogliomatosis of the cerebrospinal pathway. Brain 65:352–372
Best PV (1963) Intracranial oligodendrogliomatosis. J Neurol Neurosurg Psychiatry 26:249–256
Wober G, Jellinger K (1976) Intramedullary oligodendroglioma with meningocerebral dissemination (author’s transl). Acta Neurochir 35(4):261–269
Armao DM, Stone J, Castillo M, Mitchell KM, Bouldin TW, Suzuki K (2000) Diffuse leptomeningeal oligodendrogliomatosis: radiologic/pathologic correlation. AJNR Am J Neuroradiol 21(6):1122–1126
Ozkul A, Meteoglu I, Tataroglu C, Akyol A (2007) Primary diffuse leptomeningeal oligodendrogliomatosis causing sudden death. J Neuro-Oncol 81(1):75–79
Gardiman MP, Fassan M, Orvieto E, D'Avella D, Denaro L, Calderone M, Severino M, Scarsello G, Viscardi E, Perilongo G (2010) Diffuse leptomeningeal glioneuronal tumors: a new entity? Brain Pathol 20(2):361–366
Gardiman MP, Fassan M, Nozza P, Orvieto E, Garre ML, Milanaccio C, Severino M, Perilongo G, Giangaspero F (2012) Diffuse leptomeningeal glioneuronal tumours: clinico-pathological follow-up. Pathologica 104(6):428–431
Karlowee V, Kolakshyapati M, Amatya VJ, Takayasu T, Nosaka R, Sugiyama K, Kurisu K, Yamasaki F (2017) Diffuse leptomeningeal glioneuronal tumor (DLGNT) mimicking Whipple’s disease: a case report and literature review. Childs Nerv Syst 33(8):1411–1414
Pellerino A, Ruda R, Bertero L, Magistrello M, Franchino F, Cassoni P, Pasqualetti F, Pinessi L, Giangaspero F, Soffietti R (2018) Successful use of bevacizumab in an adult primary diffuse leptomeningeal glioneuronal tumor. J Neurosurg Sci 62(2):229–232
Fiaschi P, Badaloni F, Cagetti B, Bruzzone L, Marucci G, Dellacha A, Pavanello M, Ganci G, Padolecchia R, Valsania V (2018) Disseminated oligodendroglial-like leptomeningeal tumor in the adult: case report and review of the literature. World Neurosurg 114:53–57
Cho HJ, Myung JK, Kim H, Park CK, Kim SK, Chung CK, Choi SH, Park SH (2015) Primary diffuse leptomeningeal glioneuronal tumors. Brain Tumor Pathol 32(1):49–55
Dodgshun AJ, SantaCruz N, Hwang J, Ramkissoon SH, Malkin H, Bergthold G, Manley P, Chi S, MacGregor D, Goumnerova L, Sullivan M, Ligon K, Beroukhim R, Herrington B, Kieran MW, Hansford JR, Bandopadhayay P (2016) Disseminated glioneuronal tumors occurring in childhood: treatment outcomes and BRAF alterations including V600E mutation. J Neuro-Oncol 128(2):293–302
Acknowledgements
We would like to sincerely thank the patient and her family members for allowing us to report this case.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tiwari, N., Tamrazi, B., Robison, N. et al. Unusual radiological and histological presentation of a diffuse leptomeningeal glioneuronal tumor (DLGNT) in a 13-year-old girl. Childs Nerv Syst 35, 1609–1614 (2019). https://doi.org/10.1007/s00381-019-04074-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04074-7