Abstract
Objective
The objectives of this study were to evaluate the demographic and clinical characteristics, causes, treatment patterns, outcome, and recurrence of childhood peripheral facial palsy.
Methods
We performed a retrospective study of 144 peripheral facial palsy patients, under 18 years old in a tertiary care pediatric hospital. Medical charts were reviewed to analyze the age, gender, side of facial nerve paralysis, family history, cause, grading by the House-Brackmann Facial Nerve Grading Scale (HBS), results of diagnostic tests, therapies, outcomes, and recurrence.
Results
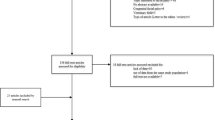
Causes were as follows: 115 idiopathic (Bell’s palsy) facial palsy (79.9%), 17 infections (11.8%) (9 otitis media, 4 varicella zoster virus (VZV) infection, 3 tooth abscess, and 1 group A β-hemolytic streptococcus infection), 7 trauma (4.9%), 4 congenital-syndrome (2.8%), and 1 (0.7%) arterial hypertension. There was no difference in age, sex, family history, grading, or outcome between idiopathic and cause-defined facial palsy. At the end of the first year, our recovery rates were 98.3%. No significant difference in recovery outcome was detected between the patients who were treated with and without steroid treatment. Thirteen (9%) patients had recurrent attacks, and no differences in the outcomes of patients with recurrent facial palsy were observed. Recurrence time ranged from 6 months to 6 years.
Conclusion
The results of this study indicate that both Bell’s palsy and cause-defined facial palsy in children have a very good prognosis. Medical treatment based on corticosteroids is not certainly effective in improving outcomes in children. Recurrent attacks occurred in 6 years from the onset which leads to the conclusion that we should have a long-term follow-up of patients diagnosed with Bell’s palsy.
Similar content being viewed by others
References
Jenke AC, Stoek LM, Zilbauer M, Wirth S, Borusiak P (2011) Facial palsy: etiology, outcome and management in children. Eur J Paediatr Neurol 15(3):209–213. https://doi.org/10.1016/j.ejpn.2010.11.004
Barr JS, Katz KA, Hazen A (2011) Surgical management of facial nerve paralysis in the pediatric population. J Pediatr Surg 46(11):2168–2176. https://doi.org/10.1016/j.jpedsurg.2011.06.036
Rowhani-Rahbar A, Baxter R, Rasgon B, Ray P, Black S, Klein JO, Klein NP (2012) Epidemiologic and clinical features of Bell’s palsy among children in Northern California. Neuroepidemiology 38(4):252–258. https://doi.org/10.1159/000338303
Sullivan FM, Swan IR, Donnan PT, Morrison JM, Smith BH, McKinstry B et al (2007) Early treatment with prednisolone or acyclovir in Bell’s palsy. N Engl J Med 357(16):1598–1607. https://doi.org/10.1056/NEJMoa072006
Engstrom M, Berg T, Stjernquist-Desatnik A, Axelsson S, Pitkaranta A, Hultcrantz M et al (2008) Prednisolone and valaciclovir in Bell’s palsy: a randomised, double-blind, placebo-controlled, multicentre trial. Lancet Neurol 7(11):993–1000. https://doi.org/10.1016/S1474-4422(08)70221-7
Salinas RA, Alvarez G, Daly F, Ferreira J (2010) Corticosteroids for Bell’s palsy (idiopathic facial paralysis). Cochrane Database Syst Rev 3:CD001942
Evans AK, Licameli G, Brietzke S, Whittemore K, Kenna M (2005) Pediatric facial nerve paralysis: patients, management and outcomes. Int J Pediatr Otorhinolaryngol 69(11):1521–1528. https://doi.org/10.1016/j.ijporl.2005.04.025
Yilmaz U, Cubukcu D, Yilmaz TS, Akinci G, Ozcan M, Guzel O (2014) Peripheral facial palsy in children. J Child Neurol 29(11):1473–1478. https://doi.org/10.1177/0883073813503990
Drack FD, Weissert M (2013) Outcome of peripheral facial palsy in children—a catamnestic study. Eur J Paediatr Neurol 17(2):185–191. https://doi.org/10.1016/j.ejpn.2012.09.003
Ismail AQ, Alake O, Kallappa C (2014) Do oral steroids aid recovery in children with Bell’s palsy? J Child Neurol 29(10):NP96–NP97. https://doi.org/10.1177/0883073813504624
May M, Fria TJ, Blumenthal F, Curtin H (1981) Facial paralysis in children: differential diagnosis. Otolaryngol Head Neck Surg 89(5):841–848. https://doi.org/10.1177/019459988108900528
Ozkale Y, Erol I, Saygi S, Yilmaz I (2015) Overview of pediatric peripheral facial nerve paralysis: analysis of 40 patients. J Child Neurol 30(2):193–199. https://doi.org/10.1177/0883073814530497
Abdel-Aziz M, Azab NA, Khalifa B, Rashed M, Naguib N (2015) The association of varicella zoster virus reactivation with Bell’s palsy in children. Int J Pediatr Otorhinolaryngol 79(3):328–331. https://doi.org/10.1016/j.ijporl.2014.12.010
Al-Muharraqi MA, O’Sullivan EC (2010) Unilateral facial nerve paralysis following an infected lower third molar. Int J Oral Maxillofac Surg 39(2):192–195. https://doi.org/10.1016/j.ijom.2009.12.003
Hyden D, Akerlind B, Peebo M (2006) Inner ear and facial nerve complications of acute otitis media with focus on bacteriology and virology. Acta Otolaryngol 126(5):460–466. https://doi.org/10.1080/00016480500401043
Jorg R, Milani GP, Simonetti GD, Bianchetti MG, Simonetti BG (2013) Peripheral facial nerve palsy in severe systemic hypertension: a systematic review. Am J Hypertens 26(3):351–356. https://doi.org/10.1093/ajh/hps045
Siegler RL, Brewer ED, Corneli HM, Thompson JA (1991) Hypertension first seen as facial paralysis: case reports and review of the literature. Pediatrics 87(3):387–389
Harms MM, Rotteveel JJ, Kar NC, Gabreels FJ (2000) Recurrent alternating facial paralysis and malignant hypertension. Neuropediatrics 31(6):318–320. https://doi.org/10.1055/s-2000-12948
Shapiro M, Peters S, Spinelli HM (2003) Melkersson-Rosenthal syndrome in the periocular area: a review of the literature and case report. Ann Plast Surg 50(6):644–648. https://doi.org/10.1097/01.SAP.0000069068.03742.48
Rivera-Serrano CM, Man LX, Klein S, Schaitkin BM (2014) Melkersson-Rosenthal syndrome: a facial nerve center perspective. J Plast Reconstr Aesthet Surg 67(8):1050–1054. https://doi.org/10.1016/j.bjps.2014.04.014
Pavlou E, Gkampeta A, Arampatzi M (2011) Facial nerve palsy in childhood. Brain and Development 33(8):644–650. https://doi.org/10.1016/j.braindev.2010.11.001
Pitaro J, Waissbluth S, Daniel SJ (2012) Do children with Bell’s palsy benefit from steroid treatment? A systematic review. Int J Pediatr Otorhinolaryngol 76(7):921–926. https://doi.org/10.1016/j.ijporl.2012.02.044
Wang CH, Chang YC, Shih HM, Chen CY, Chen JC (2010) Facial palsy in children: emergency department management and outcome. Pediatr Emerg Care 26(2):121–125. https://doi.org/10.1097/PEC.0b013e3181d018d0
Chen WX, Wong V (2005) Prognosis of Bell’s palsy in children—analysis of 29 cases. Brain and Development 27(7):504–508. https://doi.org/10.1016/j.braindev.2005.01.002
Sun B, Zhou C, Han Z (2015) Facial palsy in Melkersson-Rosenthal syndrome and Bell’s palsy: familial history and recurrence tendency. Ann Otol Rhinol Laryngol 124(2):107–109. https://doi.org/10.1177/0003489414546398
Eidlitz-Markus T, Gilai A, Mimouni M, Shuper A (2001) Recurrent facial nerve palsy in paediatric patients. Eur J Pediatr 160(11):659–663. https://doi.org/10.1007/s004310100836
Dhiravibulya K (2002) Outcome of Bell’s palsy in children. J Med Assoc Thail 85(3):334–339
Pitts DB, Adour KK, Hilsinger RL Jr (1988) Recurrent Bell’s palsy: analysis of 140 patients. Laryngoscope 98(5):535–540. https://doi.org/10.1288/00005537-198805000-00012
Crego F, Galindo J, Quesada P, Naches S, Pinas J, Vila J et al (1998) Recurrent peripheral facial paralysis. Our case load from 1995. Acta Otorrinolaringol Esp 49(4):280–282
Salman MS, MacGregor DL (2001) Should children with Bell’s palsy be treated with corticosteroids? A systematic review. J Child Neurol 16(8):565–568. https://doi.org/10.1177/088307380101600805
Acknowledgments
This study was completed at the Department of Pediatric Neurology, Ankara Children’s Hematology-Oncology Training and Research Hospital. The authors thank all colleagues for their help in follow-up of the patients.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
ZSK and ZO were involved in the diagnosis and follow-up of the patients, collected data, and wrote the whole article. TBK performed the data collection. BDT was involved in writing the article. EG was involved in the diagnosis and follow-up of the patients. AG was involved in developing the project and the revision of the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
This study was approved by the Hospital Ethical Committee of Health IRB# 2015/048.
Rights and permissions
About this article
Cite this article
Karalok, Z.S., Taskin, B.D., Ozturk, Z. et al. Childhood peripheral facial palsy. Childs Nerv Syst 34, 911–917 (2018). https://doi.org/10.1007/s00381-018-3742-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-3742-9